Nivolumab in the First-Line Treatment of Advanced NSCLC
Francesca Casaluce, Cesare Gridelli*
A.O.R.N. San Giuseppe Moscati, Contrada Amoretta, Italy
Received Date: 02/11/2020; Published Date: 04/12/2020
*Corresponding author:Cesare Gridelli, Division of Medical Oncology, A.O.R.N. S.G. Moscati Hospital, Contrada Amoretta, 83100, Avellino, Italy; phone: +39 0825203573; E-mail: cgridelli@libero.it.
Abstract
Nowadays, immunotherapy has changed paradigms for care of newly diagnosed Non-Small Cell Lung Cancer (NSCLC) patients without oncogenic driver mutations, whose treatment choice was crucially driven by Programmed Death-Ligand1 (PD-L1) expression. An immunotherapy-based regimen alone or in combination with chemotherapy is now the preferred option based on high-level evidence obtained from randomized controlled trials and in accordance with all guidelines. But, the list of available fist-line options is getting longer and the improvement of patient selection remain a key interest, considering the expensiveness and some serious side effects of immune drugs. Differing from pembrolizumab and atezolizumab, nivolumab use as single agent is restricted to subsequent-line therapy, while the current nivolumab approval as front-line treatment is limited to use into combination regimens. Specifically, the dual immune combination of nivolumab plus an anti-Cytotoxic T-Lymphocyte Antigen 4 (CTLA-4) agent, ipilimumab, with or without short course of chemotherapy, has opened the new frontier of a chemo-sparing option. Choosing between current upfront therapeutic options can be difficult due to the lack of direct cross-comparison studies, differences in chemotherapies and stratification factors, and differences in study populations resulting from inclusion criteria such as histology, PD-L1 expression. In an attempt to aid the decision-making process, we discuss and summarize the most recent data from clinical trials focused on nivolumab use in patients with previously untreated metastatic NSCLC, outlining its potential impact on current clinical practice.
Keywords: Anti CTLA-4; Anti PD-1 agent; Combination approach; Immunotherapy; Ipilimumab; Nivolumab; Non-small cell lung cancer
Introduction
The field of lung cancer treatment has evolved over past years and continues to race forward. Without targetable oncogenic driver alterations, who consequently defined targeted opportunities as the best upfront choice, the management of metastatic Non-Small Cell Lung Cancer (NSCLC) is focused on immunotherapy-based regimen, as single agent mainly for tumors expressing programmed cell death ligand-1 (PD-L1) at least 50% or more, and as combined to histologic-directed chemotherapy for those with lower PD-L1 expression levels. So, platinum-based chemotherapy is a low bar as the standard, while immunotherapy is now the preferred option based on high-level evidence obtained from randomized controlled trials and in accordance with all guidelines. However, the list of available fist-line options is getting longer and the choice of the best treatments for each patient remain a critical point of discussion. In the era of precision medicine, new predictors of immune clinical benefit to improve patient selection is the current challenge, considering the financial burden and some serious side effects of the immunotherapy treatment.
Nivolumab as First Line Choice: Phase Iii Clinical Trials
The immunotherapy story back in 2012, when phase I trials firstly demonstrated significant activity of PD-(L)1 inhibitors in unselected patients with NSCLC [1,2]. Subsequently, several programmed cell death-1 (PD-1) and PD-L1 agents were approved as first- and subsequent- lines of treatment. The first of them began in March 2015, consisting in second-line approval of nivolumab. Nivolumab is a human monoclonal antibody that targets the PD-1 receptor, whose expressed on surface of T cells, B cells, and macrophages. Consequently, it blocks the interaction of PD-1 with PD-L1, thereby limiting cancer cell's capacity to conceal itself from immune effector cells. Differing from pembrolizumab and atezolizumab, both approved as upfront monotherapy for metastatic NSCLC with high PD-L1 expression (PD-L1 ≥ 50% for pembrolizumab; PD-L1-stained ≥ 50% of tumor cells [TC ≥ 50%] or PD-L1 stained tumor-infiltrating Immune Cells [IC] covering ≥ 10% of the tumor area [IC ≥ 10%]) and without epidermal growth factor receptor- (EGFR) or Anaplastic Lymphoma Kinase- (ALK) sensitizing alterations, nivolumab use as single agent is restricted to subsequent-line therapy. The phase III CheckMate 026 trial firstly investigated nivolumab efficacy as upfront monotherapy for patients with metastatic NSCLC expressing PD-L1 at least 1% or more, failing to achieve positive results [3]. Compared to platinum-based chemotherapy, frontline nivolumab did not improve Progression-Free Survival (PFS) and Overall Survival (OS) at primary efficacy analysis involving 428 patients with ≥5% PD-L1 positivity (hazard ratio [HR] PFS: 1.19; HR OS: 1.08), with similar negative results in all randomized PD-L1≥1% population. Notably, disappointing results were strikingly reported also for strongly PD-L1 positive subgroup (PD-L1 ≥50%) in the post-hoc analysis (HR PFS: 1.07; HR OS: 0.90) [3]. To justify the unsuccessful of nivolumab with synchronous and opposite practice-changing results of the other anti PD-1 agent pembrolizumab, many critical doubts were suggested, above all on patient selection and trial design. As previously suggested from KEYNOTE trials [4,5], the expression of PD-L1 by the tumor appeared to be predictive of response to immune treatment. Notably, patients enrolled in CheckMate 026 had to have ≥5% PD-L1 tumor expression, while the eligibility to pivotal KEYNOTE-024 trial required PD-L1 levels at least 50% or more. Second, an imbalance between control and nivolumab arms was noted, with an higher percentage of strongly positive in the first one (74.1% vs. 53.2%), as well as an higher proportions of patients with better prognosis disease at baseline randomized to chemotherapy arm (slightly fewer liver metastases, smaller tumor burden, and a higher proportion of women). Although the failure of the trial, in the exploratory analysis nivolumab reported higher response rates (47% vs. 28%) and longer PFS (median PFS: 9.7 vs. 5.8 months; HR PFS: 0.62) than chemotherapy among patients selected by high Tumor Mutational Burden (TMB), defined as cutoff of >10 mutations/megabase (mut/Mb), but with no impact on survival results. Of note, the highest responses to nivolumab were observed in those patients with both high TMB and high PD-L1, accounting an Overall Response Rate (ORR) of 75% rather than 32% and 16% reported for those patients with only one or neither of these two markers, respectively, and suggesting that combining two biomarkers (high PD-L1 expression and high TMB) may identify those patients who obtained the maximum benefit of immunotherapy [3].
To validate prospectively this hypothesis emerged from a not pre-specified analysis, the design of Checkmate 227 trial was subsequently modified, but the trial has not checked results as expected.
For the first time, the CheckMate 227 trial evaluated the dual immuno-combination of an anti PD-1 (nivolumab) with a cytotoxic T-lymphocyte–associated antigen-4–blocking monoclonal antibody (ipilimumab) in metastatic/recurrent NSCLC without sensitizing EGFR/ALK alterations [6]. The study design was quite complicated, with many modifications since the begin. The trial consisted of a PD-L1 positive cohort (1189 patients with PD-L1 ≥1% tumors, part 1a) and a PD-L1 negative cohort (550 patients with PD-L1 <1% tumors, part 1b), each of this randomized 1:1:1 to three different arms: nivolumab plus ipilimumab and histology-directed chemotherapy in both of these populations, while the third arm was nivolumab in part 1a and nivolumab plus chemotherapy in part 1b. Initially, the study was designed with primary endpoint of OS among patient with PD-L1 positive tumors for nivolumab plus ipilimumab versus chemotherapy. Midway to the trial, the study protocol was modified to include a co-primary endpoint of PFS in the subgroup of patients classified as high-TMB, according to CheckMate 026 and CheckMate 568 suggestions [3,7]. Based on TMB analysis, a very impressive improvement in PFS was seen using the immune-doublet (nivolumab plus low dose ipilimumab) over chemotherapy among all patients with tumors carrying high-TMB (HR PFS: 0.58), regardless of PD-L1 expression levels. Of note, this PFS benefit was not associated with a significant improvement of OS over chemotherapy among the same subgroup of patients with high-TMB (HR: 0.79 at minimum follow up of 14.2 months [6,8,9].
The co-primary OS endpoint in PD-L1 positive group was also met (HR OS: 0.79). To note, no consistent correlation between survival outcomes with nivolumab plus ipilimumab over chemotherapy and PD-L1 expression or TMB cut-off were reported, questioning the role of TMB as predictive biomarker. According to PD-L1 levels, survival outcomes with nivolumab plus ipilimumab were not consistently different from chemotherapy alone in the PD-L1 1-49% subgroup, performing the same median OS of 15.1 months (unstratified HR OS: 0.94), while the immune combination upgraded chemotherapy results for PD-L1≥50% patients, achieving the maximum benefit (median 21.2 vs 14 months, unstratified HR OS 0.70) [6]. Without direct comparison of dual immune combination with immune-monotherapy - the current standard of care for strongly positive patients -, the addition of ipilimumab to single agent nivolumab in PD-L1 ≥50% subgroup did not increase PFS (HR 0.80) or OS (HR 0.87) over nivolumab alone, with more toxicity (grade ≥3 adverse events: 33% vs. 19%), as emerged from pre-specified analysis.
Although the trial was not powered to directly compare the OS between nivolumab plus ipilimumab versus nivolumab plus chemotherapy in PD-L1 negative tumors, survival benefit was substantially similar (1-yr OS: 59% vs. 60%; 2-yr OS: 35% vs. 40%), while the dual immune-combination improved PFS outcomes (1-year PFS rates: 45% vs 27%) in PD-L1 negative and high-TMB cohort of patients [8].
Finally, the trial assessed the efficacy of nivolumab monotherapy versus chemotherapy as a pre-specified endpoint, and similarly to CheckMate 026, nivolumab did not improve the OS over chemotherapy neither in the PD-L1 ≥1% nor in the PD-L1 ≥50% subgroup.
On other hand, according to findings from part II of the final analysis, the addition of nivolumab to first-line platinum-based chemotherapy performed better than chemotherapy alone in terms of PFS and ORR, but failing to improve significantly OS in non-squamous disease (HR OS: 0.86), with opposite interesting data in squamous histology (HR OS: 0.69) [10].
An update of Checkmate 227 with 3-years survival data was recently reported. Looking again at initial primary endpoint of OS based on PD-L1 status, the immunotherapy doublet combination significantly improved the 3-years survivals of PD-L1 positive population over chemotherapy (median OS: 17.1 vs. 14.9 months; HR OS: 0.79), with more pronounced benefit in the PD-L1 negative population (HR OS: 0.64). In each PD-L1 subgroup, a third of them were alive at 3 years. Comparing with other treatment arms of each part, the dual immune-combination revealed its superiority over nivolumab alone for patient with PD-L1>1% (median OS: 17.1 vs. 15.7, HR OS: 0.90), and over nivolumab plus chemotherapy for patients with PD-L1 less than 1% (median OS: 17.2 vs. 15.2 months, HR OS: 0.82) [11].
Also PFS, ORR and duration of response (DOR) were improved with nivolumab plus ipilimumab compared to chemotherapy, regardless of PD-L1 levels. According to responses, patients receiving nivolumab plus ipilimumab had no significantly differences over chemotherapy in term of ORR, but a very significant durability, with a proportion of patients who still having a response at 3 year overtime after receiving this immune-therapy (38% vs. 4% and 34% vs. 0%, for PD-L1 positive and negative cohorts, respectively). Specifically, the median DOR with chemotherapy was 5-7 months, whereas with immunotherapy was 18 months for PD-L1 negative and nearly 2 years for PD-L1 positive patients. As emerged from an exploratory post-landmark OS analysis, patients who were responders to at 6 months, were more likely to be still alive at 3 years, with very encouraging data regardless of PD-L1 status: among PD-L1 positive patients who had complete/partial responses at 6 months, over 70% were alive 3 years later versus 39% in chemotherapy arm, and similar findings were observed in PD-L1 negative cohort [11]. Assessing the safety as well as the efficacy, focusing on treatment-related adverse events (TRAEs) leading to discontinuation of any component of regimen, this events occurred generally early in timeline, within first 6 months of treatment, and their frequency was doublet when comparing nivolumab/ipilimumab to chemotherapy (18% vs. 9%), most of these consisting in severe grade (grade 3-4 AEs: 12% vs. 5%) (8, 11). Based on these data, the dual immune-combination was approved by U.S. Food and Drug Administration (FDA) in May 2020 as another first-line option to choice for the management of metastatic NSCLC patients, but restricted to PD-L1 positive disease only. Notably, the OS for PD-L1 negative was defined as secondary endpoint, so the approval is not extended to this population, despite the median OS was encouraging. However, if this approach is currently U.S. approved, it will never be used worldwide, considering the Bristol-Meyer Squibb withdrawal of nivolumab plus ipilimumab application in Europe at January 2020.
In May 2020, the CheckMate 9LA regimen - consisting in continuous therapy with nivolumab plus ipilimumab plus 2 cycles of chemotherapy - was also added by U.S. FDA to the copious list of first-line treatment options approved in metastatic NSCLC, but without restriction to PD-L1 status, in contrast to CheckMate 227 regimen. Who maybe ask yourself why so much therapy as upfront, the rational is based on Checkmate 227 suggestions, where PFS curves not separated before 6 months, suggesting that a significant percentage of patients did not benefit from this regimen. A similar trend was observed for OS curves, with probably detrimental outcomes for early progressed patients. Using eligibility criteria quite similar to CheckMate 227, 719 patients enrolled to Checkmate 9LA were randomized 1:1 to receive nivolumab plus ipilimumab plus 2 cycles of platinum-based chemotherapy, while control arm was represented by 4 cycles of chemotherapy according to histology. Notably, over two third of population enrolled have no-squamous type, and patients with PD-L1>50%, liver and bone metastasis at baseline were more represented in chemotherapy arm. The experimental arm improved significantly OS at preplanned interim analysis (HR OS: 0.69), as well as at updated analysis at minimum follow up of 12.7 months (HR OS: 0.66), prolonging median OS of 5 months (median OS: 15.6 vs. 10.9 months) [12]. Importantly, the survival curves started to separate early. Looking at different subgroup of patients with aim to see differential impact between two arms, the triplet was encouraging superior to chemotherapy alone irrespective of histology or PD-L1 levels, including the piece of PD-L1 1-49% (HR OS: 0.61). Despite no availability of PFS data, survival data of PD-L1 1-49% subgroup of CheckMate 9LA are a lot more convincing than those emerged from the same PD-L1 subgroup enrolled in the CheckMate 227.
As mentioned, one of the rational of the trial design was really to improve the early disease progression rate: 84% of patients presented a control of disease, and importantly, as seen in OS, the early separation of PFS curves before 6 months was reported (HR PFS: 0.68). In terms of response, the median DOR was doubled with this approach (11.3 vs 5.6 months), while the improvement of ORR was significant (38% vs 25%) but numerically lower than observed with other immuno-chemotherapy combinations [12].
About toxicities, despite limitation of crossover trial comparisons, the frequency of TRAEs leading to discontinuation of therapy is quite comparable to CheckMate 227 (19% and 18%, respectively), but over doubled than chemotherapy arm (any grade: 19% vs 7%, grade 3-4: 16% vs 5%). No new safety signals were observed, with side effect profile consistent with other immune-chemotherapy combinations. Particularly focused on immune-related adverse events (irAEs), skin and endocrine toxicities were the most common events, usually as low grade, with gastrointestinal as higher rates of severe grade [12-17]. So, in contrast to immunotherapy monotherapy approaches, the association with just two cycles of chemotherapy - not forward more as we seen with other immuno-chemotherapy combinations - is associated with an improvement of OS regardless of PD-L1 status, with no crossing of curves early on.
Discussion
Both trials has established themselves as an available and acceptable chemo-free option and may have inevitably a role in future clinical trials, but are these results practice changing? Is there a benefit to nivolumab/ipilimumab combinations over chemotherapy plus PD-(L)1 approach? Available data are not sufficient to suggest that nivolumab plus ipilimumab alone or combined to chemotherapy will displace the KEYNOTE-189 and KEYNOTE-024 regimens. On other hand, the CheckMate 227 and 9LA regimens could be considered, despite it’s still unclear who benefits most, and the incorporation of CTLA-4 agent brings toxicity, yet manageable but not minor.
In term of duration of responses, curves of Checkmate 227 and 9LA clearly revealed that some patients strongly benefit from the incorporation of a CTLA-4 inhibition, with more superior and impressive results than previously seen with PD-L1 blockade.
Analyzing OS curves of checkmate 227 and 9LA for PD-L1 positive subgroup, two interesting points need to further clarifications. Focusing on first three months of therapy, the triplet nivolumab/ipilimumab/chemotherapy performed similarly well to chemotherapy alone in checkmate 9LA, then curves separated and the experimental regimen continues to have advantage. In the first couple of months of CheckMate 227 trial, patients treated with chemotherapy alone seemed to have more benefit in terms of survival over immunotherapy alone (nivolumab alone or combined to ipilimumab). The second point of interest concerns survival rates at first year: more than 60% of patients in immunotherapy containing regimens were alive in both CheckMate trials, while chemotherapy arm performed different, with better survival rates in CheckMate 227 rather than 9LA (56% vs 47%). About PD-L1 negative cohort, survival benefit with immune-arms compared to chemotherapy in both trials were similarly, reporting an HR of 0.64 and of 0.62 in Checkmate 9LA and Checkmate 227, respectively.
The main questions about two studies consisted firstly, in the choice of chemotherapy alone as competitor arm, not yet the current standard of care, representing by chemotherapy plus PD-1 approach; secondly, the real benefit with nivolumab/ipilimumab combinations over chemotherapy plus PD-1 approach is not yet clear, paying the hole of longer follow up data, and the unavoidable increased risk of irAEs. Clearly, long term survival might be key for elucidating any potential benefit of CTLA4 inhibition addition.
Based on data available and comparing indirectly phase III clinical trials (Table 1), focusing on the CheckMate 227, CheckMate 9LA and KEYNOTE 189, the different length of median follow up must be evaluated, with 12.7 months of CheckmateM9LA as the shortest. Looking at first year, the survival rates ranged of 60-70% across all trials, downing to 40-46% at two years in CheckMate 227 and KEYNOTE 189, with immature data for CheckMate 9LA.The 3 year updated OS analysis from CheckMate 227 looks promising, assessing survival rates to 33%, but the trial design not provide direct comparison with nivolumab plus chemotherapy.
Anyway, the CheckMate9LA regimen might be potentially used in patients with large tumor burden, PDL-1 negative and symptomatic disease, where the goal of treatment is to establish a durable disease control, providing the ability of those patients to support toxicities (younger patients without extensive comorbidities). To note, this regimen seems to be promising mainly for the “unlucky” category of PD-L1 negative patients, where other immuno-chemo combinations performed not so well (marginal PFS benefit in KEYNOTE 189; few data from IMpower130; more pronounced benefit for patients with liver metastases at baseline or high-TMB from IMpower150 or CheckMate 227 regimens, respectively).
On opposite, the CheckMate 227 regimen could be possibly administered to patients with PD-L1 less than 50% (the approval is not for the PDL1 negative patients, despite the benefit seen in this population, as well as data are not so robust to displace pembrolizumab monotherapy in high PD-L1 ≥ 50% patients), and a contraindication/aversion to chemotherapy or those who develop metastatic disease on or soon after adjuvant chemotherapy.
Table 1: Combination strategies as fist-line treatment of advanced NSCLC.
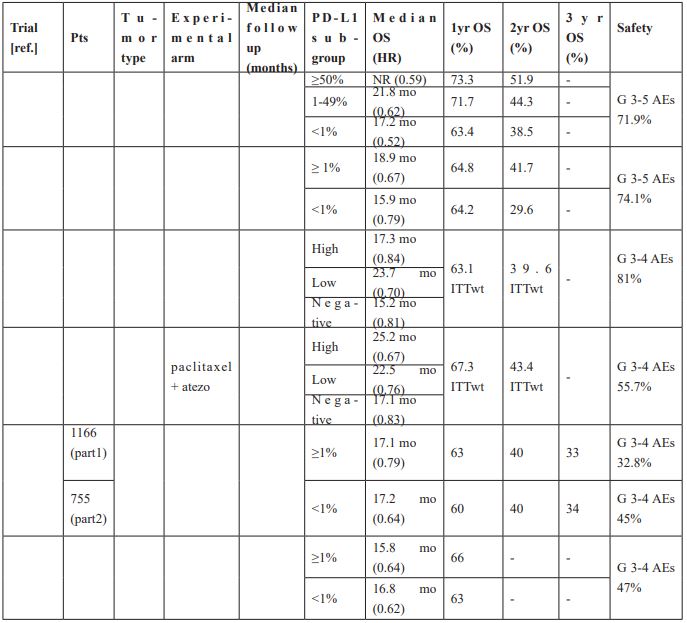
Conclusion
So, chemotherapy alone is no longer standard of care, with three FDA-approved strategies: chemotherapy plus PD-(L)1 agents, chemotherapy for two cycles plus nivolumab/ipilimumab, nivolumab plus ipilimumab alone only in PD-L1 positive. Choosing between current upfront therapeutic options can be difficult due to the lack of direct cross-comparison studies, differences in chemotherapies and stratification factors, and differences in study populations resulting from inclusion criteria such as histology and PD-L1 expression. Nowadays, one of the most common discussions in clinical practice are concerns about whose patients should be candidate to receive immunotherapy alone or in combination with chemotherapy, or to receive “the last-come” dual immune combination with/without chemotherapy. More specific biomarkers are inevitably needed for patient’s selection, considering that not all patients respond and benefit from these treatments, not delaying the financial burden and the toxicities profile of these drugs. From clinical trials, both TMB and PD-L1 clearly emerged as “the biomarker” who may help to identify the subset of patients for whom the use of chemotherapy can be spared. Long-term survival rates and ongoing immunotherapy biomarker research will help us to differentiate all current combination options and more accurately customize first-line immunotherapy strategies for metastatic NSCLC.
Competing Interests
Cesare Gridelli: as speaker bureau and advisory board member for Astra Zeneca, BMS, Menarini, MSD Novartis, Roche; Francesca Casaluce: no conflict of interest to declare.
References
- Topalian SL, Hodi FS, Brahmer JR, et al. Safety, activity, and immune correlates of anti PD-1 antibody in cancer. N Engl J Med 2012; 366:2443-54.
- Brahmer JR, Tykodi SS, Chow LQ, et al. Safety and activity of anti PD-L1 antibody in patients with advanced cancer. N Engl J Med 2012; 366:2455-65.
- Carbone DP, Reck M, Paz-Ares L., et al. First-line nivolumab in stage IV or recurrent non-small-cell lung cancer. N Engl J Med 2017; 376:2415-2426.
- Lopes G, Wu Y-L, Kudaba I, et al. Pembrolizumab (pembro) versus platinum-based chemotherapy (chemo) as first-line therapy for advanced/metastatic NSCLC with a PD-L1 tumor proportion score (TPS) ≥ 1%: open-label, phase 3 KEYNOTE-042 study. J Clin Oncol 2018; 36: Suppl: LBA4-LBA4. Abstract.
- Brahmer J, Rodríguez-Abreu D, Robinson A, et al. Updated analysis of KEYNOTE-024: pembrolizumab vs platinum-based chemotherapy for advanced NSCLC with PD-L1 TPS ≥50%. J Thorac Oncol 2017; 12: S1793-4.
- Hellmann MD, Ciuleanu TE, Pluzanski A, et al. Nivolumab plus Ipilimumab in Lung Cancer with a High Tumor Mutational Burden. N Engl J Med. 2018; 378:2093-2104.
- Ramalingam SS, Hellmann MD, Awad MM, et al. Tumor mutational burden (TMB) as a biomarker for clinical benefit from dual immune checkpoint blockade with nivolumab (nivo) + ipilimumab (ipi) in first-line (1L) non-small cell lung cancer (NSCLC): identification of TMB cutoff from CheckMate 568. Cancer Research 2018; 78:CT078-CT078.
- Hellmann M, Paz-Ares L, Bernabe Caro R, et al. Nivolumab plus Ipilimumab in Advanced Non–Small-Cell Lung Cancer. N Eng J Med. 2019; 381:2020-2031.
- Bristol-Myers Squibb Provides Update on the Ongoing Regulatory Review of Opdivo Plus Low-Dose Yervoy in First-Line Lung Cancer Patients with Tumor Mutational Burden ≥10 mut/Mb|https://news.bms.com/press-release/corporatefinancial-news/bristol-myers-squibb-providesupdate-ongoing-regulatory-review (accessed November 10, 2018).
- Paz-Ares L, Ciuleanu TE, Yu X et al. Nivolumab (NIVO) + platinum-doublet chemotherapy (chemo) vs chemo as first-line (1L) treatment (tx) for advanced non-small cell lung cancer (aNSCLC): CheckMate 227 - part 2 final analysis. Ann of Oncol 2019; 30:xi67-xi68.
- Ramalingam SS, Ciuleanu TE, Pluzanski A, et al. Nivolumab + ipilimumab versus platinum-doublet chemotherapy as first-line treatment for advanced non-small cell lung cancer: Three-year update from CheckMate 227 Part 1. J Clin Oncol 2020; 38:9500-9500.
- Reck M, Ciuleanu T-E, Dols M C, et al. Nivolumab (NIVO) + ipilimumab (IPI) + 2 cycles of platinum-doublet chemotherapy (chemo) vs 4 cycles chemo as first-line (1L) treatment (tx) for stage IV/recurrent non-small cell lung cancer (NSCLC): CheckMate 9LA. J Clin Oncol 2020; 38:9501-9501.
- Gandhi L, Rodríguez-Abreu D, Gadgeel S, et al. Pembrolizumab plus Chemotherapy in Metastatic Non–Small-Cell Lung Cancer. N Engl J Med 2018; 378:2078-2092.
- Rodriguez-Abreu D, Powell SF, Hochmair M, et al. Final analysis of KEYNOTE-189: Pemetrexed-platinum chemotherapy (chemo) with or without pembrolizumab (pembro) in patients (pts) with previously untreated metastatic nonsquamous non-small cell lung cancer (NSCLC). J Clin Oncol 38; 15:9582-9582.
- Paz-Ares L, Luft A, Vicente D, et al. Pembrolizumab plus Chemotherapy for Squamous Non–Small-Cell Lung Cancer. N Engl J Med 2018; 379:2040-2051.
- West H, McCleod M, Hussein M, et al. Atezolizumab in combination with carboplatin plus nab-paclitaxel chemotherapy compared with chemotherapy alone as first-line treatment for metastatic non-squamous non-small-cell lung cancer (IMpower130): a multicentre, randomised, open-label, phase 3 trial. The lancet 2019; 20:924-937.
- Socinski MA, Jotte RM, Cappuzzo F, et al. Overall survival (OS) analysis of IMpower150, a randomized Ph 3 study of atezolizumab (atezo) + chemotherapy (chemo) ± bevacizumab (bev) vs chemo + bev in 1L nonsquamous (NSQ) NSCLC. J Clin Oncol; 36:9002-9002.

