Pandemic of Novel Coronavirus (nCOVID-19): Impact on World
Mihir YP1*, Tribhuvan S2 and Akhlesh V3
1Department of Pharmacology, Principal & Professor, Sanjay College of Pharmacy, Dr. A. P. J. Abdul Kalam Technical University, Lucknow, UP, India
2Department of Pharmacology, Principal & Director, Srajan Institute of Pharmacy, Oel-Dhakwa, Lakhimpur Kheri, Dr. A. P. J. Abdul Kalam Technical University, Lucknow, UP, India
3Department of Surgery, General Surgeon & Chairman, Srajan Institute of Pharmacy, Oel-Dhakwa, Lakhimpur Kheri, Dr. A. P. J. Abdul Kalam Technical University, Lucknow, UP, India
Received Date: 15/06/2020; Published Date: 16/07/2020
*Corresponding author: Mihir Y. Parmar, Department of Pharmacology, Principal and Professor, Sanjay College of Pharmacy, Dr. A. P. J. Abdul Kalam Technical University, Lucknow, UP, India. Tel: +91-7016422726; E-mail: mihirparmar4uonly@yahoo.com
Abstract
Coronaviruses (CoV) belong to the genus Coronavirus with its high mutation rate in the Coronaviridae. The intention of this analysis was to have a preliminary opinion about the epiudemic of viral disease, the ways of treatment, and prevention in this early stage of nCOVID-19 outburst.
Keywords: nCOVID-19; Coronaviruses; Outburst; Pandemic; World
Introduction
Coronaviruses (CoV) belong to the genus Coronavirus in the Coronaviridae. All CoVs are pleomorphic RNA viruses characteristically containing crown-shape peplomers with 80-160 nM in size and 27-32 kb positive polarity (Figure 1). Recombination rates of CoVs are very high because of constantly developing transcription errors and RNA Dependent RNA Polymerase (RdRP) jumps. With its high mutation rate, Coronaviruses are zoonotic pathogens that are present in humans and various animals with a wide range of clinical features from asymptomatic course to requirement of hospitalization in the intensive care unit; causing infections in respiratory, gastrointestinal, hepatic and neurologic systems [1-3]. They were not considered as highly pathogenic for humans until they have been seen with the severe acute respiratory syndrome (SARS) in the Guangdong state of China for the first time in 2002 and 2003. Before these outbreaks, there were the two most known types of CoV as CoV OC43 and CoV 229E that have mostly caused mild infections in people with an adequate immune system [3,4].
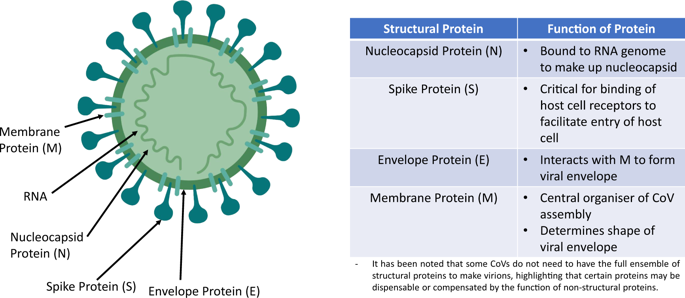
Figure 1: Coronavirus Particle
Approximately ten years after SARS this time, another highly pathogenic nCoV, Middle East Respiratory Syndrome Coronavirus (MERS-CoV) has emerged in the Middle East countries such as suadi arabia [5]. In December 2019, 2019 novel Coronavirus (nCoV), which is another public health problem, has emerged in the Huanan Seafood Market, where livestock animals are also traded, in Wuhan State of Hubei Province in China and has been the focus of global attention due to a pneumonia epidemic of unknown cause [6]. At first, an unknown pneumonia case was detected on December 12, 2019, and possible influenza and other coronaviruses were ruled out by laboratory testing. Chinese authorities announced on January 7, 2020 that a new type of Coronavirus (novel Coronavirus, nCoV) was isolated [7]. This virus was named as nCOVID-19 by WHO on January 12 and COVID-19 on 11 February 2020. As of February 12, 2020, a total of 43.103 confirmed cases and 1.018 deaths have been announced [8]. When given where the first case originated, the infection were transmitted probably as zoonotic agent (from animal to human). The increase in the number of cases in Wuhan city and internationally after closing the market and evacuation of the cases in China, has indicated a second transmission from human-to-human. New cases are identified, primarily in other Asian countries and in many countries such as the trans-oceanic USA and France (Table 1 & 2).
Table 1: The Number of Cases and Death of COVID-19 outbreak according to John Hopkins University, Times of INDIA on March 30, 2020.
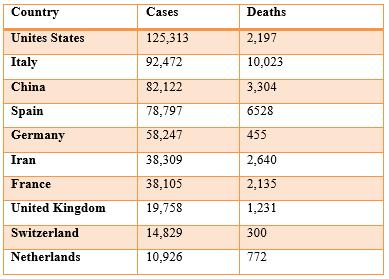
Table 2: The Number of Cases and Death of COVID-19 outbreak according to John Hopkins University, Times of INDIA on May 15, 2020.
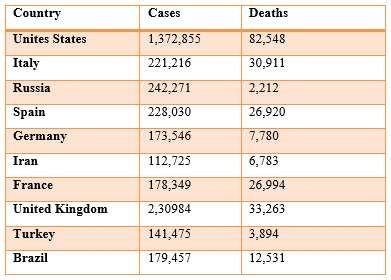
The intention of this article was to have a preliminary opinion about the disease, the ways of treatment, and prevention in this early stage of this outburst.
Epidemiology
In December 2019, many pneumonia cases that were clustered in Wuhan city were reported and searches for the source have shown Huanan Seafood Market as the origin. The first case of the COVID-19 epidemic was discovered with unexplained pneumonia on December 12, 2019, and 27 viral pneumonia cases with seven being severe, were officially announced on December 31, 2019 [7,9]. Etiologic investigations have been performed in patients who applied to the hospital due to similar viral pneumonia findings. The common history of high-risk animal contact in the medical histories of these patients has strengthened the likelihood of an infection transmitted from animals to humans [3,9]. On January 22, 2020, novel CoV has been declared to be originated from wild bats and belonged to Group 2 of beta-coronavirus that contains Severe Acute Respiratory Syndrome Associated Coronavirus (SARS-CoV). Although COVID-19 and SARS-CoV belong to the same beta coronavirus subgroup, similarity at genome level is only 70%, and the novel group has been found to show genetic differences from SARS-CoV (Figure 2) [10].
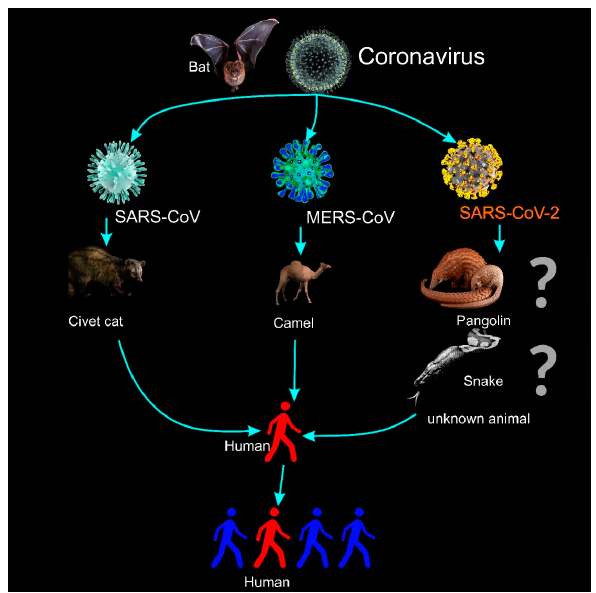
Figure 2: The illustration for the transmission of coronaviruses and the 2019 novel Coronavirus (2019-nCoV or SARS-CoV-2).
Similar to the SARS epidemic, this outbreak has occurred during the Spring Festival in China, which is the most famous traditional festival in China, during which nearly 3 billion people travel countrywide. These conditions caused favorable conditions for the transmission of this highly contagious disease and severe difficulties in prevention and control of the epidemic. The period of the Spring Festival of China was between January 17 and February 23 in 2003, when the SARS epidemic peaked, while the period of the festival was between January 10 and February 18 in 2020. Similarly, there was a rapid increase in COVID-19 cases between January 10 to 22. Wuhan, the center of the epidemic with 10 million populations, is also an important center in the spring festival transportation network. The estimated number of travelers during the 2020 spring festival has raised 1.7 folds when compared with the number traveled in 2003 and reached to 3.11 billion from 1.82 billion. This large-scale travel traffic has also created favorable conditions for the spread of this difficult-to control disease [11].
Virology-Pathogenesis
Coronaviruses are viruses whose genome structure is best known among all RNA viruses. Two-thirds of RNA they have encodes viral polymerase (RdRp), RNA synthesis materials, and two large nonstructural polyproteins that are not involved in host response modulation (ORF1a-ORF1b). The other one-third of the genome encodes four structural proteins (spike (S), envelope (E), membrane (M) ve nucleocapsid (N), and the other helper proteins [12,13]. Although the length of the CoV genome shows high variability for ORF1a/ORF1b and four structural proteins, it is mostly associated with the number and size of accessory proteins [12,13].
The first step in virus infection is the interaction of sensitive human cells with Spike Protein. Genome encoding occurs after entering to the cell and facilitates the expression of the genes that encode useful accessory proteins, which advance the adaptation of CoVs to their human host [13]. Genome changes resulting from recombination, gene exchange, gene insertion, or deletion are frequent among CoVs, and this will take place in future outbreaks as in past epidemics. As a result of the studies, the CoV subfamily is rapidly expanding with new generation sequencing appli- cations that improve the detection and definition of novel CoV species. In conclusion, CoV classification is continually changing. According to the most recent classification of The International Committee on Taxonomy of Viruses (ICTV), there are four genera of thirty-eight unique species (Figure 3) [14].
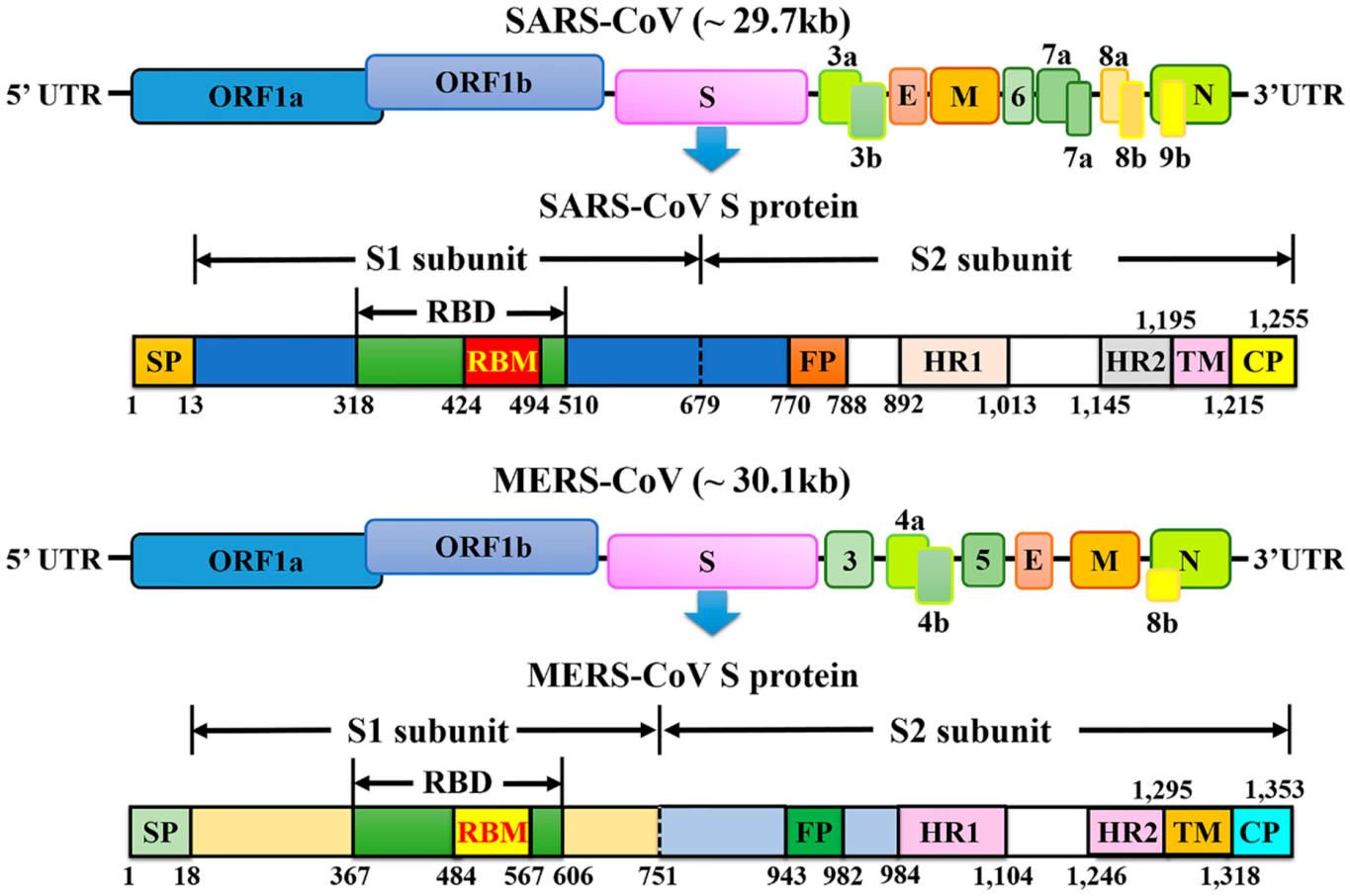
Figure 3: Schematic representation of the genome organization and functional domains of S protein for SARS-CoV and MERS-CoV.
SARS-CoV and MERS-CoV that attach to the host cell respectively bind to cellular receptor angiotensin-converting enzyme 2 (SARS-CoV associated) and cellular receptor of dipeptidyl peptidase 4 (MERS-CoV associated) [15]. After entering the cell, the viral RNA manifest itself in the cytoplasm. Genomic RNA is encapsulated and polyadenylated, and encodes various structural and non-structural polypeptide genes. These polyproteins are split by proteases that exhibit chymotrypsin-like activity [13,15]. The resulting complex drives (-) RNA production through both replication and transcription. During replication, full-length (-) RNA copies of the genome are produced and used as a template for full-length (+) RNA genomes [12, 13]. During transcription, a subset of 7-9 sub-genomic RNAs, including those encoding all structural proteins, are produced by discontinuous transcription. Viral nucleocapsids are combined from genomic RNA and R protein in the cytoplasm and then are budded into the lumen of the endoplasmic reticulum. Virions are then released from the infected cell through exocytosis. The released viruses can infect kidney cells, liver cells, intestines, and T lymphocytes, as well as the lower respiratory tract, where they form the main symptoms and signs [15]. Remarkably, CDT lymphocytes were found to be lower than 200 cells/mm3 in three patients with SARS-CoV infection. MERS-CoV is able to affect human dendritic cells and macrophages in-vitro. T lymphocytes are also a target for the pathogen due to the characteristic CD26 rosettes. This virus can make the antiviral T-cell response irregular due to the stimulation of T-cell apoptosis, thus causing a collapse of the immune system [16,].
Sources and Modes of Transmission
CoVs have been defined as a novel respiratory tract virus in the samples collected from the individuals who present symptoms of respiratory tract infection in 1962 [18]. This is a large family of viruses that are common in many different animal species, including camels, cattle, cats, and bats (Figure 2). Rarely, animal CoVs can infect humans and, as a result, may spread among humans during epidemics such as MERS, SARS, and COVID-19 [13-16]. At the onset of major outbreaks caused by CoVs, palm cats have been proposed to be a natural reservoir of Human CoVs for SARS and dromedary camels for MERS [3]. However, more advanced virological and genetic studies have shown that bats are reservoir hosts of both SARS-CoV and MERS-CoV and before these viruses spread to humans, they use the other responsible animals as intermediate hosts. Studies have reported that most of the bat CoVs are the gene source of alpha-CoV and beta-CoVs, while most of the bird CoVs are the gene source of gamma-CoVs and delta-CoVs [3]. In recent studies, it has been observed that the novel virus causing epidemics coincides with the CoV isolated in bats. Presence of wild animal trade in Huanan Seafoods Market where the first cases appeared, supports this finding [6,10].
After the first outbreak, secondary cases began to be reported after approximately ten days. Moreover, while these new patients had no contact with the marketplace, they had a history of contact with humans there. Confirmed recent reports from many infected healthcare workers in Wuhan show that human-to-human transmission can occur. As in SARS and MERS epidemics in the past, human-tohuman transmission has accelerated the spread of the outbreak and case reports have also started from other states of China. The first non-Chinese case of the infection, which spread to the Chinese provinces, and then to the Asian continent, was reported from Thailand on January 13, 2020. The case reported being a Chinese tourist who has traveled to Thailand and had no epidemiologic connection with the marketplace [19]. Other cases from oversea countries such as the USA and France have continued to be reported [20].
Often, the human-to-human transmission occurs with close contact. The transmission primarily occurs when an infected person sneezes and through the respiratory droplets produced just as the spread of influenza and other respiratory pathogens. These droplets can settle in the mouth or nasal mucosa and lungs of people with inhaled air. Currently, it remains unclear whether a person can be infected by COVID- 19 by touching an infected surface or object and then touching their mouth, nose, or possibly eyes [21].
Typically, like most respiratory viruses, it is considered to be the most contagious when people are most symptomatic. However, cases, who were infected from an asymptomatic person in the prodrome period of COVID-19, were also reported. Sufficient data are not available on infectiousness of the disease and research is ongoing [22].
Clinical Progression-Diagnosis
Before SARS-CoV cases, it was thought that human CoVs leads to cold-like upper respiratory infection and self-limiting lower respiratory infection. The first death due to coronaviruses has reported by the isolation of SARS-CoV from a patient with pneumonia in China. As in other respiratoryinfected viruses and previous beta-CoV, similarities present in the clinical aspects of COVID-19 infections, it is known that clinical picture varies from simple respiratory infection findings to septic shock. Similar to SARS CoV and MERS CoVthat caused epidemics in the past years, the first symptoms are commonly defined as fever, cough, and shortness of breath [19]. Although diarrhea was presentin about 20-25% of patients with MERS-CoV or SARS-CoV infection, intestinal symptoms were rarely reported in patients with COVID-19. In another study of 99 patients, chest pain, confusion, and nausea-vomiting were noted in addition to previous findings [23]. On X-rays or thorax CT imaging of the examined patients, unilateral or bilateral involvement compatible with viral pneumonia was found, and bilateral multiple lobular and subsegmental consolidation areas were observed in patients hospitalized in the intensive care unit [24,25].
In a cohort study of 41 hospitalized patients, fever, dry cough, myalgia and fatigue symptoms were reported in most patients, and less often, symptoms of expectoration, headache, hemoptysis and diarrhea were also observed [24]. According to that study, comorbidities such as underlying diabetes mellitus, hypertension, and cardiovascular disease were found in about half of these patients. Besides, patients developed dyspnea accompanied by abnormal thorax CT compatible with pneumonia mean eight days after the admission. Complications include ARDS, acute heart damage, secondary infections, and pneumothorax. Similarly to the previous data, X-rays or thorax CT images of the patients revealed unilateral or bilateral lung involvement, compatible with viral pneumonia. Bilateral multiple lobular and subsegmental consolidation areas were present in patients in the intensive care unit [24]. The patients with underlying comorbidity exhibited a more severe clinical course, as expected by the experience gained from the previous epidemics [26].
As in SARS and MERS, the diagnosis of 2019 n-CoV infection is based on a history of detailed contact and travel, and precise laboratory testing. The diagnostic tools are molecular methods, serology and viral culture. The most common diagnostic methods are molecular methods as RT-PCR (reverse transcription) or real-time PCR, which are made using RNA from respiratory samples such as oropharyngeal swabs, sputum, nasopharyngeal aspirate, deep tracheal aspirate, or bronchoalveolar lavage. In particular, lower respiratory tract samples can offer significantly higher viral load and genome fraction than upper respiratory tract samples. These techniques are beneficial in terms of evaluating the results quickly, showing the genome structure and viral load [25].
The sensitivity of antibody detection is generally lower than molecular methods and is mostly used in retrospective diagnosis. Viral culture is a more time consuming method compared to the other methods. Culture is much more useful in the first stage of outbreaks before other diagnostic methods become clinically available. In addition, viral cultures can be used in the in-vitro and in-vivo antiviral treatment and vaccine evaluation trials [3].
Coronavirus from SARS to MERS
SARS-CoV, which originated from China and then was spread to other parts of the world with hospital-acquired infectious cases, had a mortality rate of 10%, and was transmitted to 8000 people during an 8-month outbreak in 2002-2003 [21]. In 2012, MERS-CoV, when it emerged in Arabian Peninsula MERS-CoV, spread to 27 countries with 35.6% mortality rate in 2220 cases. It is known that both of them are zoonotic viruses showing hospital-acquired and human-to-human transmission [21,22]. Similar dynamics apply for COVID-19 that was originated from Wuhan and the current the rate of mortality from this infection is about 2%. CoVs can use different receptors and pathways when entering the cell. SARS-CoV usually infects young people, MERS-CoV people aged above 50 years and COVID-19 infects middle age and above. Comparing non-respiratory complications, MERS-CoV involve the cardiovascular system more frequently than SARS-CoV and frequently require vasopressor treatment [3,19,20]. Case series have reported that COVID-19 affects the cardiovascular system [23]. Acute kidney failure was more commonly seen in SARS-CoV and MERS-CoV epidemics compared to COVID-19 [3,26]. Whereas radiological findings are present in all three pathogens, airspace opacifications are seen in SARS-CoV and groundglass appearance in MERS-CoV and COVID-19 [3,26]. Hospital- acquired secondary infections have been defined in all three pathogens.[3,23] There are no studies that report a definitely successful drug for their treatment [24]. In terms of epidemic periods, SARS-CoV ended in less than a year, and the MERS-CoV epidemic lasted for seven years despite its spread to more restricted areas and. The question of how long the novel COVID-19 outbreak will last is a question that everyone is curious about.
Treatment and Protection
In general, there are few or no treatment options for viral diseases that occur suddenly [24]. In parallel with this knowledge, today there is no vaccine or effective treatment to prevent COVID-19 infection. Molecules are being tested for COVID-19 in in-vitro and human-based SARS-CoV and MERS-Cov trials. Studies evaluating the antiviral activity of types I and II interferons have reported, interferon-beta (IFNb), as the most potent interferon, was reducing in- vitro MERS-CoV replication [19]. According to a human MERSCoV case report from South Korea, the use of the combination of Lopinavir/Ritonavir (LPV/RTV) (Anti-HIV drugs), pegylated interferon and ribavirin provided a successful viral clearance [23]. For this purpose, a randomized control trial (MIRACLE Trial), that aimed to determine whether LPV/RTV-IFNb improved clinical results in MERS-CoV patients, was initiated in 2016 and 76 patients were enrolled [27]. Although another antiviral drug, remdesivir was used in the first case reported from the United States of America, seemed successful, controlled studies with more cases are needed [21]. In-vitro studies have shown that viral RNA transcription was terminated with remdesivir in early stage [28,29]. There are publications demonstrating that remdesivir has a strong antiviral activity in epithelial cell cultures against SARS-CoV, MERS-CoV and related zoonotic bat CoVs [30, 31].
Many measures should be taken, such as timely publication of epidemic information for elimination of the source of infection, early diagnosis, reporting, isolation, supportive treatments and for avoiding unnecessary panic. CDC reminds basic measures such as hand washing, using disinfectant solutions, avoiding contact with patients in order to prevent the spread of viruses by droplets. Precautionary actions including the provision of medicines supply chains, personal protective equipment, and hospital supplies should be made in a short time for the protection of the Chinese people and global health, especially in the places with close travel ports to major Chinese ports [32].
Based on the 2003 SARS-CoV epidemic experience, the Chinese government takes many effective measures including closing public transport, reducing migration and promoting personal protection with masks in Wuhan and other provinces. Hence, there are reported cases of infected hospital personnel, healthcare staff should be informed about taking personal protective measures such as the use of gloves, eye masks and N95 masks during the examination of patients with a suspected history of COVID-19 contact or travel to China [11,33].
Future Projections
Near future course of COVID-19, which as of 12 Şubat 2020 has spread to 25 countries in total on 4 continents with 43.103 confirmed cases and 1.018 deaths, 1.017 being in mainland China and 1 in the Philippines, arouses public interest [9]. Since COVID-19 is very similar to SARS-CoV, some important features of SARS epidemic are guiding the predictions on current epidemic. According to the logistical modelling studies performed by combining daily numbers from COVID-19 cases with data obtained in SARS epidemics; timely diagnosis is essential for quarantine and integrated interventions to control the outbreak.
Currently growth factor (New cases of everyday/cases of previous day) of COVID-19 started to fall below 1 threshold. If the current trend continues, the number of infected people is expected to reach peak at the beginning of March 2020 (80 days from the onset). The duration between onset of symptoms and isolation is about 6 days, and it’s expected that each one day reduction in this period will decrease the size of peak population by 72-84% and cumulative infected cases and deaths by 68-80%. It is estimated that with the effects of integrated interventions such as promoting the use of face masks and reduced traveling, each 10% reduction in transmission rate, the size of peak population will decrease by 20-47% and cumulative infected cases and deaths will decrease by 23-49% [34].
Owing to the measures by Chinese government, including passing laws for effective infection management, supports accelerating the diagnosis and treatment such as distribution of more than 30.000 PCR- fluorescent probe kits to determined diagnosis centers in Wuhan, and closing Wuhan and nearby Huang Guang provinces, the number of Cases are expected to be below the estimates. Rapid diagnosis with quarantine and integrated interventions will have a great effect on future trends of the outbreak. Although COVID- 19 has a similar spread with SARS and MERS, it exhibits lower mortality rates. However, variables such as traveler flow due to the Spring Festival and cross-border spread of infection require further research about advanced intervention strategies in order to make more precise predictions. As imposition of globalization, coronaviruses will cause spreads and outbreaks with different-mutant strains similarly in the coming years. With increased scientific collaboration, which is a result of globalization, we may have more powerful means of fighting against coronaviruses, in which we know the genome structure very well in the future [34].
References
-
-
- Woo PC, Huang Y, Lau SK, Yuen KY. Coronavirus genomics and bioinformatics analysis. Viruses. 2010;2:1804-20.
- Drexler JF, Gloza-Rausch F, Glende J, Corman VM, Muth D, Goettsche M, et al. Genomic characterization of severe acute respiratory syndrome-related coronavirus in European bats and classification of coronaviruses based on partial RNA-dependent RNA polymerase gene sequences. J Virol. 2010;84:11336-49.
- Yin Y, Wunderink RG. MERS, SARS and other coronaviruses as causes of pneumonia. Respirology. 2018;23:130-7.
- Peiris JSM, Lai ST, Poon L, et al. Coronavirus as a possible cause of severe acute respiratory syndrome. The Lancet. 2003;361:1319-25.
- Zaki AM, van Boheemen S, Bestebroer TM, Osterhaus AD, Fouchier RA. Isolation of a novel coronavirus from a man with pneumonia in Saudi Arabia. N Engl J Med. 2012;367:1814-20.
- Seven days in medicine: 8-14 Jan 2020. BMJ. 2020;368:m132.31948945.
- Imperial College London. Report 2: estimating the potential total number of novel coronavirus cases in Wuhan City, China. 2020. https://www.imperial.ac.uk/mrc-globalinfectiousdisease- analysis/news--wuhan-coronavirus.
- European Centre for Disease Prevention and Control data. Geographical distribution of 2019- nCov cases. (https://www.ecdc.europa.eu/en/geographical-distribution- 2019-ncov-cases) (accessed on 05 February 2020).
- World Helath Organization, 2019- nCoV Situation Report-22 2020. https://www.who.int/docs/defaultsource/ coronaviruse/situation-reports/.
- Gralinski L, Menachery V. Return of the Coronavirus: 2019- nCoV, Viruses. 2020;12:135.
- Chen Z, Zhang W, Lu Y, et al. From SARS-CoV to Wuhan 2019- nCoV Outbreak: Similarity of Early Epidemic and Prediction of Future Trends: Cell Press 2020.
- Luk HK, Li X, Fung J, Lau SK, Woo PC. Molecular epidemiology, evolution and phylogeny of SARS coronavirus. Infection, Genetics and Evolution. 2019;71:21-30.
- Coronavirinae in ViralZone. Available online: https://viralzone. expasy.org/785 (accessed on 05 February 2019).
- Subissi L, Posthuma CC, Collet A, Zevenhoven-Dobbe JC, Gorbalenya AE, Decroly E, et al. One severe acute respiratory syndrome coronavirus protein complex integrates processive RNA polymerase and exonuclease activities. Proc Natl Acad Sci USA. 2014;111:E3900-E3909.
- Lambeir AM, Durinx C, Scharpe S, De Meester I. Dipeptidylpeptidase IV from bench to bedside: An update on structural properties, functions, and clinical aspects of the enzyme DPPIV. Crit Rev Clin Lab Sci. 2003;40:209-94.
- Chu H, Zhou J, Wong BH, Li C, Cheng ZS, Lin X, et al. Productive replication of Middle East respiratory syndrome coronavirus in monocyte-derived dendritic cells modulates innate immune response. Virology. 2014;454-455:197-205.
- Zhou J, Chu H, Li C, Wong BH, Cheng ZS, Poon VK. Active replication of Middle East respiratory syndrome coronavirus and aberrant induction of inflammatory cytokines. chemokines in human macrophages: Implications for pathogenesis. J Infect Dis. 2014;209:1331-42.
- Hamre D, Procknow JJ. A new virus isolated from the human respiratory tract. Proceedings of the Society for Experimental Biology and Medicine. 1966;121:190-3.
- Hui DS, Azhar EI, Madani TA, Ntoumi F, Kock R, Dar O, et al. The continuing 2019-nCoV epidemic threat of novel coronaviruses to global health -The latest 2019 novel coronavirus outbreak in Wuhan, China. Int J Infect Dis. 2020;264-6.
- Holshue ML, DeBolt C, Lindquist S, Lofy KH, Wiesman J, Bruce H, et al. First Case of 2019 Novel Coronavirus in the United States The New England Journal of Medicine 2020.
- WHO. Emergencies preparedness, response. Pneumonia of unknown origin – China. Disease outbreak news. Available online: https:// HYPERLINK "http://www.who.int/csr/don/12- january-2020-novel-coronavirus-china/en/" www.who.int/ csr/don/12-january-2020-novel-coronavirus-china/en/ (accessed on 05 February 2020).
- Rothe C, Schunk M, Sothmann P, Bretzel G, Froeschl G, Wallrauch C, et al. Transmission of 2019-nCoV Infection from an Asymptomatic Contact in Germany. 2020.
- Chen N, Zhou M, Dong X, Qu J, Gong F, Han Y, et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet. 2020. https://doi.org/10.1016/ S0140-6736(20)30211-7.
- Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020.HYPERLINK "https://doi. org/10.1016/S01406736(20)301835" https://doi.org/10.1016/ S0140–6736(20)30183-5.
- Zhu N, Zhang D, Wang W, et al. A novel coronavirus from patients with pneumonia in China. N England J Medicine. 2019. DOI: 10.1056/NEJMoa2001017
- Wang C, Horby PW, Harden FG, Gao GF. A novel coronavirus outbreak of global health concern. Lancet. 2020. https://doi.org/10.1016/S0140-6736(20)30185-9.
- Arabi YM, Alothman A, Balkhy, et al. Treatment of Middle East respiratory syndrome with a combination of lopinavir-ritonavir and interferon-β1b (MIRACLE trial): study protocol for a randomized controlled trial. Trials 2016;19;81.
- Warren TK, et al. Therapeutic efficacy of the small molecule GS-5734 against Ebola virus in rhesus monkeys. Nature. 2016;531:381-5.
- Jordan PC, et al. Initiation, extension, and termination of RNA synthesis by a paramyxovirus polymerase. PLoS Pathog. 2018;14:e1006889.
- Cockrell AS, et al. A mouse model for MERS coronavirusinduced acute respiratory distress syndrome. Nat. Microbiol. 2016;2:16226.
- Brown AJ, et al. Broad spectrum antiviral remdesivir inhibits human endemic and zoonotic deltacoronaviruses with a highly divergent RNA dependent RNA polymerase. Antivir Res. 2019;169:104541.
- Novel Coronavirus.Prevention and Treatment. 2019. Available online: https://www.cdc.gov/coronavirus/2019-ncov/about/ prevention-treatment.html (accessed on 05 February 2020)
- What to do if you are sick with 2019 Novel Coronavirus. https://www.cdc.gov/coronavirus/2019-ncov/ about/steps-when-sick.html (accessed on 05 February 2020)
- Shen M, Peng Z, Xiao, Zhang L. Modelling the epidemic trend of the 2019 novel coronavirus outbreak in China.
- Daily New 2019-nCoV Cases 2020. Available Online: https://www.worldometers. info/coronavirus/coronavirus-cases/ (Accessed on 12 February, 2020)
- Growth Factor Chart of 2019-nCoV outbreak. https://www.worldometers.info/coronavirus/coronavirus- cases/ (Accessed on 12 February, 2020).
-

