A Systematic Review of Fixation Methods for Basicervical Femoral Neck Fractures
Joash Kumar1,*, Tristan Symonds2, Matthew Ludlow3, Jonathan Quinn4, Tom Walsh5 and Simon Platt6
1Lecturer Griffith University, Department of Orthopaedics, Gold Coast Hospital and Health Service, Australia
2Department of Orthopaedics, Ipswich Hospital and Health Service, Australia
3Department of Orthopaedics, The Prince Charles Hospital, Australia
4Department of Orthopaedics, Gold Coast Hospital and Health Service, Australia
5Office for Research Governance and Development, Gold Coast Hospital and Health Service, Australia
6Department of Orthopaedics, Gold Coast Hospital and Health Service, Australia
Received Date: 12/10/2025; Published Date: 22/12/2025
*Corresponding author: Dr. Joash Kumar, MBBS, Lecturer Griffith University, Department of Orthopaedics, Gold Coast Hospital and Health Service, 1 Hospital Blvd, Southport, Queensland, 4216, Australia
Abstract
Background: Basicervical femoral neck fractures (BFNFs), comprising 1.8–7.7% of hip fractures, are biomechanically challenging due to their transitional location. Optimal fixation methods remain debated due to inconsistent classification and limited evidence. This review compared outcomes of sliding hip screw (SHS), cannulated cancellous screws (CCS), and cephalomedullary nails (CMN) for BFNF fixation, with fixation failure as the primary outcome measure.
Methods: A PRISMA-compliant systematic review identified 19 studies comprising (989 patients; mean age 73.7 years, 43% male). Fixation methods included SHS (n=610), CCS (n=69), and CMN (n=310). The Newcastle-Ottawa Scale/RoB2 assessed study quality, and statistical analyses compared failure, revision, and non-union rates. This study was registered with PROSPERO on the 11th of November 2020 (PROSPERO 2020 CRD42020209111).
Results: Prospective/retrospective studies, case series, and one RCT was included. CMN demonstrated the lowest non-union rate (0.32%) compared to 2.3% for SHS and 2.9% for CCS (p=0.072). Revision rates were significantly lower with CMN (3.54%) compared to SHS (6.39%) and CCS (13.04%) (p=0.011). Fixation failure rates were 6.56% for SHS (CI 4.6% - 8.5%), 21.74% for CCS (CI 12% - 31.5%), and 4.52% for CMN (p<0.00001, CI 2.3% - 7.7%). CMN exhibited the longest time to union (3.6 months).
Conclusion: CMN fixation was associated with lower non-union, fixation failure, and revision rates. However, due to limitations in the existing literature, definitive recommendations cannot be made. Randomised controlled trials (RCTs) are needed to validate these results and standardise treatment protocols.
Keywords: Basicervical; Neck of femur; Fracture; Open reduction internal fixation; Method of fixation; Intracapsular; Geriatric fracture, Neck of femur fixation
Background
Annually, over four million individuals worldwide experience hip fractures, with projections that more than 21 million people will live with fracture-related disabilities by 2050 [1,2]. Neck of femur fractures, particularly in the elderly, are associated with high morbidity and mortality. Early surgery and immediate weight-bearing are key to optimising recovery.
Hip fractures are classified as either intracapsular (treated with fixation or arthroplasty) and extracapsular (treated with various fixation methods). Basicervical femoral neck fractures (BFNFs) lie between these classifications, combining biomechanical instability with compromised vascular supply [3].
BFNFs occur at the junction of the femoral neck and intertrochanteric region [4,5], accounting for 1.8-7.7% of all hip fractures [5,6]. Their location subjects them to high shear forces, limited vascularity, and reduced cancellous bone interdigitation, predisposing them to mechanical failure [7,8]. The optimal fixation method for BFNFs remains uncertain, partly due to classification inconsistencies and limited evidence. The two-part fracture is by far the commonest definition, the fracture line located at the base of femoral neck and medial to intertrochanteric line, exiting above the lesser trochanter [9,10].
Treatment strategies include arthroplasty, or internal fixation (cannulated cancellous screws [CCS], fixed angle devices, sliding hip screw +/- anti-rotation screw [SHS], or cephalomedullary nail [CMN]) [11-14]. Fixation approaches have evolved with a better understanding of the fracture morphology and implant biomechanics.
This systematic review evaluates the most effective fixation method for BFNF in adults (≥18) by comparing union, fixation failures, and revision surgeries across CMN, SHS and CCS constructs. Outcomes were assessed at a minimum follow-up of 12 months. The primary outcome registered was fixation failure, defined as metalwork failure or screw cut-out.
We hypothesised that CMNs would demonstrate the lowest fixation failure rates.
Methodology
This systematic review was registered with PROSPERO on the 11th of November 2020 (PROSPERO 2020 CRD42020209111), and conducted in accordance with PRISMA guidelines (Figure 1, 2) [15].
Search strategy and identification of studies (Figure 3)
A comprehensive search of Google Scholar, PubMed, MEDLINE, Cochrane, Web of Science, EMBASE, Scopus, and Ovid was conducted up to July 11, 2021, with an updated search on the 12th of February 2025. MeSH terms included: basicervical, transcervical, hip fracture, femoral neck fracture, femoral neck fractures femur fracture, femur fractures, neck of femur. An experienced librarian assisted in developing the search strategy (Figure 3). The updated search confirmed no new studies that altered conclusions.
Data extraction and assessment
Twoindependent reviewers screened titles, abstracts, and full texts using Covidence software. Disagreements were resolved via third-party adjudication. Full-text articles were comprehensively assessed, and data on publication year, study type, patient demographics, fixation methods, and clinical outcomes were extracted. A hand search was completed for additional relevant studies. Only studies exclusively reporting BFNF data were included. Studies with mixed fracture types were excluded unless BFNF outcomes were separately reported.
Inclusion criteria
Studies were included if they:
- Included patients with BFNFs.
- Reported outcomes of internal fixation using CCS, SHS +/- anti-rotation screw, CMN.
- Reported at least one of the following: time to union, non-union rate, fixation failure, mortality and/or functional outcome score. Failure was defined as metalwork failure or screw cut-out.
- Were RCTs, non-randomised controlled trials, prospective cohort trials, retrospective comparative studies, or case-series, published in peer reviewed journals.
- Had ≥ 12 months follow-up.
Exclusion criteria
Studies were excluded if they:
- Grouped BFNFs with other proximal femur fractures without separate reporting.
- Were non-English publications
- Were case reports or ongoing/unpublished studies.
Risk of bias (methodological quality) assessment of individual studies
Given that there are no tools to assess the risk of bias (i.e., methodological quality) of case series’, we derived items from the Newcastle-Ottawa scale that were appropriate for this systematic review [16]. We removed the Newcastle-Ottawa scale items that relate to comparability and adjustment and kept items that focused on selection and representativeness of cases, outcome, and exposure. This resulted in five criteria (Table 2) in the form of questions with binary responses to indicate whether the item is suggestive or not of bias. Studies were rated as low risk (5/5 criteria), moderate (4/5), or high risk (<3/5). The sole RCT was assessed using the Cochrane RoB2 tool [17], evaluating randomisation, deviations from the intended interventions, missed outcome data, measurement methods, and reporting bias.
Statistical analysis
Descriptive statistics were used for demographic and outcome data. Meta-analysis was not performed due to clinical and methodological heterogeneity across studies.
From: Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 2021;372:n71. doi: 10.1136/bmj.n71. This work is licensed under CC BY 4.0. To view a copy of this license, visit https://creativecommons.org/licenses/by/4.0/
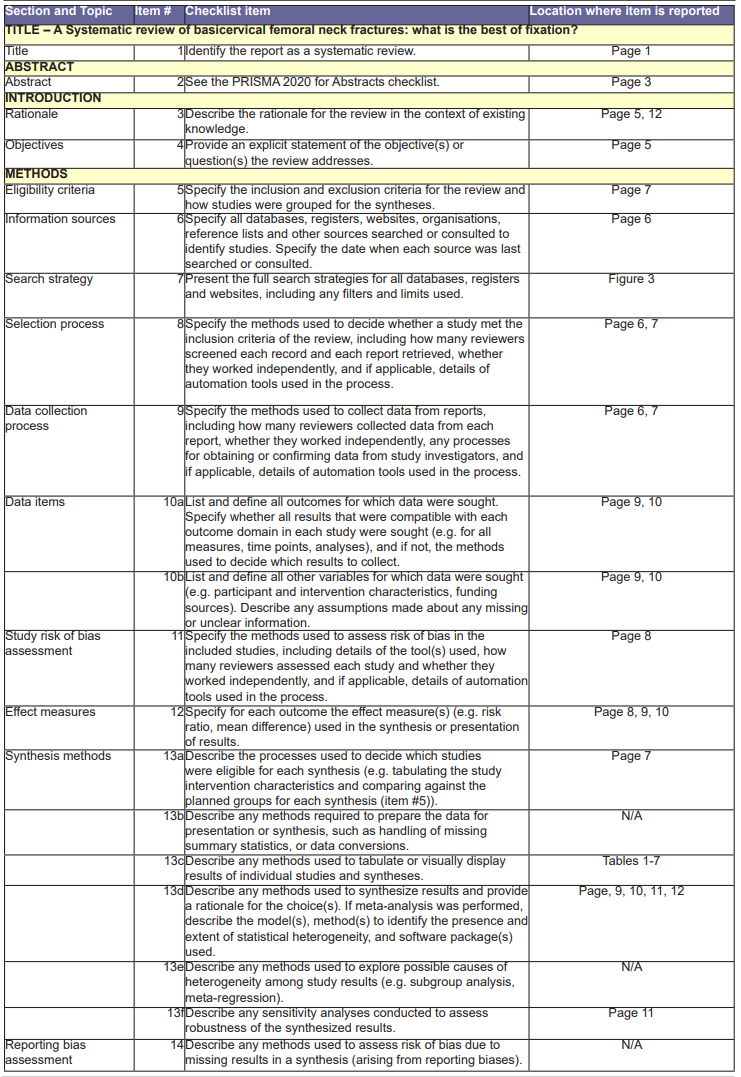
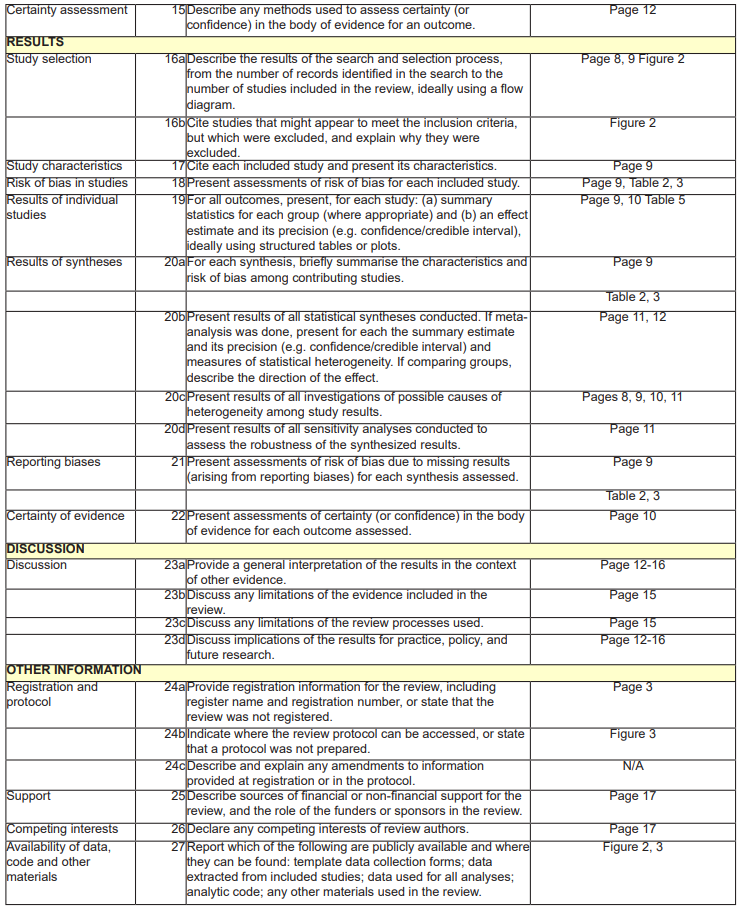
Figure 1: PRISMA 2020 Checklist.
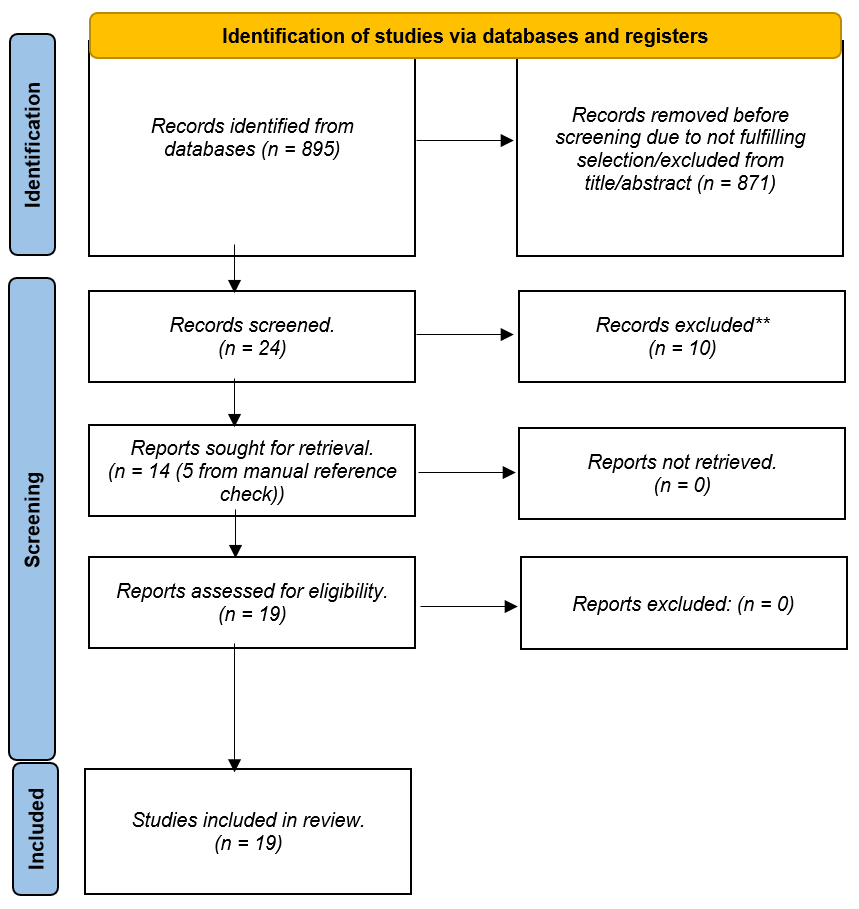
Figure 2: PRISMA Flow Diagram.
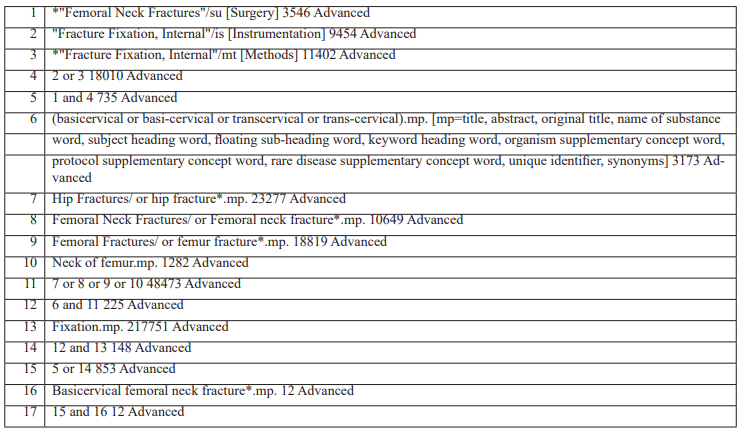
Figure 3: Example of search strategy.
Results
The search yielded 895 articles, 871 were excluded based on titles and abstracts. Of the 24 full texts, 14 met inclusion criteria. An additional five studies were found through hand search, totalling 19 papers (Figure 2).
Study characteristics (Table 1)
The review included seven retrospective cohort studies (from Finland, UK, Sweden, South Korea, and China) [7,11,18-22], three prospective cohort studies (from Egypt, South Korea, and India) [3,13,23], and one RCT conducted over multiple hospitals internationally [24]. The remaining eight were case series from six countries (Finland, China, Turkey, USA, Japan, and South Korea) [6,8-10,14,25-27].
Participant’s characteristics (Table 1)
A total of 989 patients were analysed (43% male, 57% female) with a mean age of 73.7 years. Data from 1982 to 2022 showed 610 (62%) patients received SHS fixation, 69 (7%) underwent CCS fixation, and 310 (31%) were treated with various CMN.
Methodological quality assessment (Table 2, 3)
Risk of bias assessment for the cohort/case series showed 12 papers being at low risk (66.6%), four at moderate risk (22.2%) and two at high risk (11.1%). The single RCT was at a low risk of bias across all five domains of the RoB2 tool.
Definition of basicervical femoral neck fractures (Table 4)
Definitions varied among studies. The two most common definitions were the Arbeitsgemeinschaft fur osteosynthesis classification B2 and Watson et al’s definition; Two-part fracture at the base of the femoral neck that was medial to the intertrochanteric line and exited above the lesser trochanter but was more lateral than a classic transcervical fracture [10].
Definition of union, fixation failure and complications (Table 5)
In total, six papers defined union (four with radiological definitions, two with both radiological and clinical definitions). The most common definitions were ‘evidence/presence of bony trabeculae across the fracture site’ for radiological union, and ‘absence of pain during mobilisation’ for clinical union.
Fixation failure was defined in five papers, the most common of which were screw cut-out (penetration of screw through femoral head) and non-union. The remaining 12 papers did not define fixation failure, but instead defined complications which were non-specific.
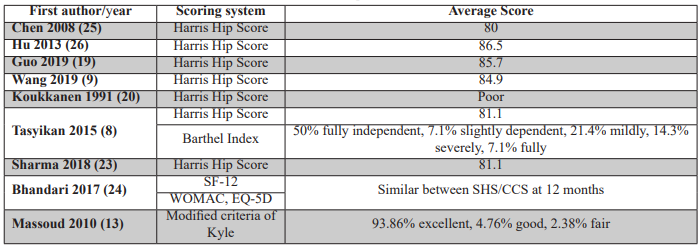
Outcomes by fixation method (Table 6)
For SHS (610 patients in 11 studies), time to union averaged 3.1 months. Non-union rates averaged 2.3%. Revision rates were 6.39%, and failure rates 6.55%.
For CCS (69 patients in four studies), time to union averaged 3.3 months. Revision rates were 13%, and failure rates 21.7%.
For CMN (310 patients in 12 studies), time to union averaged 3.6 months. Non-union rates were 0.3%. Revision rates were 3.54%, and failure rates 4.51%.
The corresponding 95% confidence intervals were: SHS (4.6%–8.5%), CCS (12.0%–31.5%), and CMN (2.3%–7.7%), reflecting greater precision and reliability with CMN and SHS over CCS.
Patient reported outcome measures/functional outcome (Table 7)
Eleven studies reported functional scores. Seven used the Harris Hip Score (mean 83.2, indicating ‘good’ outcomes). Other tools included the Barthel Index, SF-12, SF-36, FRS, Modified criteria of Kyle, WOMAC, and EQ-5D. Heterogeneity limited pool analysis.
Mortality
Mortality was inconsistently reported and thus not analysed.
Table 1: Characteristics of included studies.
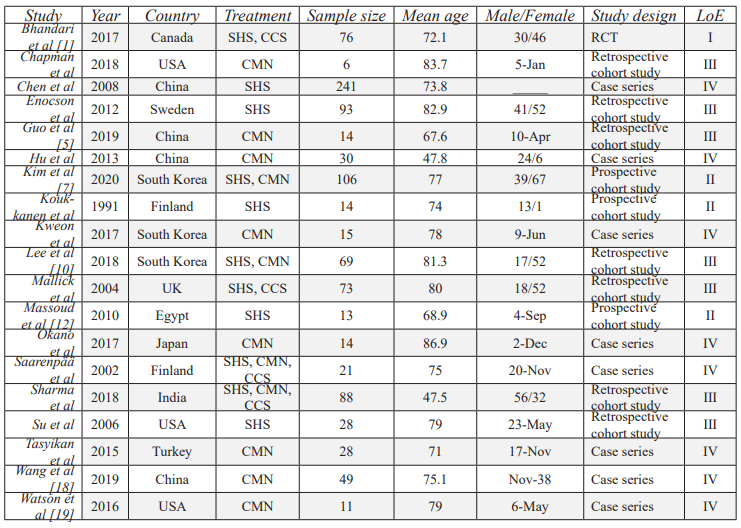

Table 2: Risk of bias assessment of cohort/case studies (Newcastle Ottawa Scale).
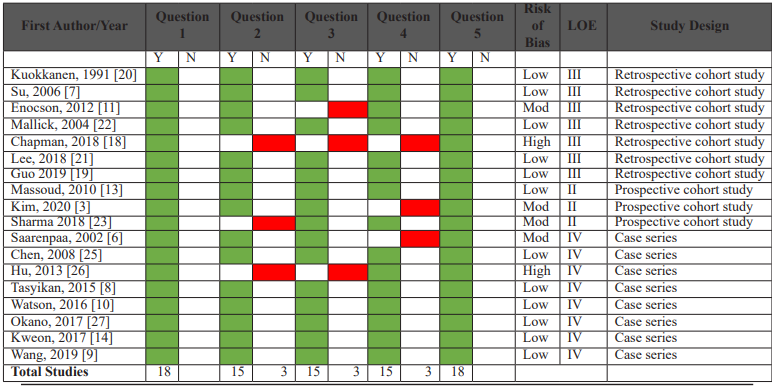
Table 3: Risk of bias assessment of RCT (Risk of Bias 2 Tool).
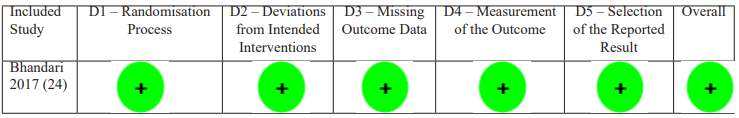
Table 4: Definition of basicervical fractures.
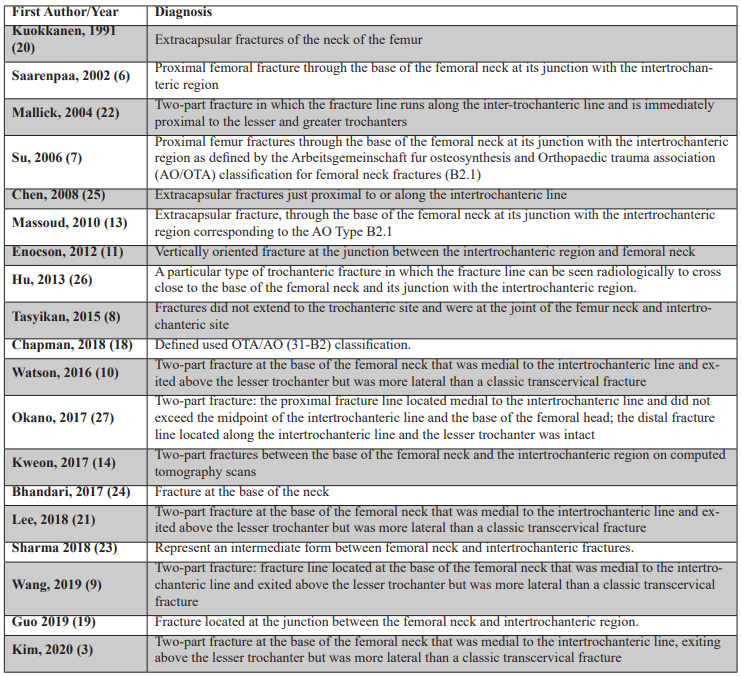
Table 5: Union/Failure/Complication definitions.
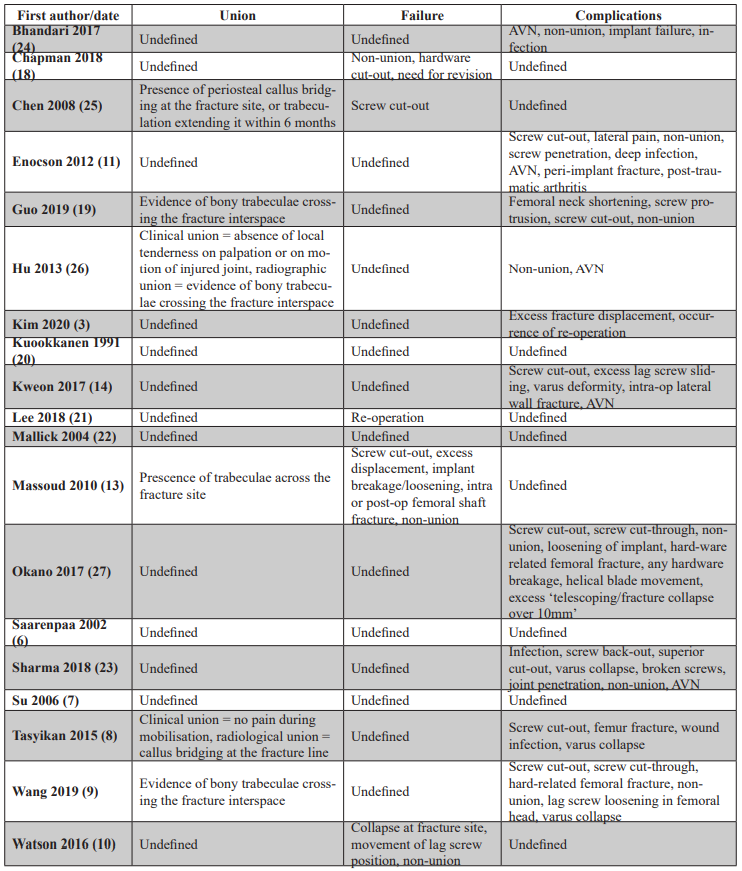
Table 6: Outcomes.
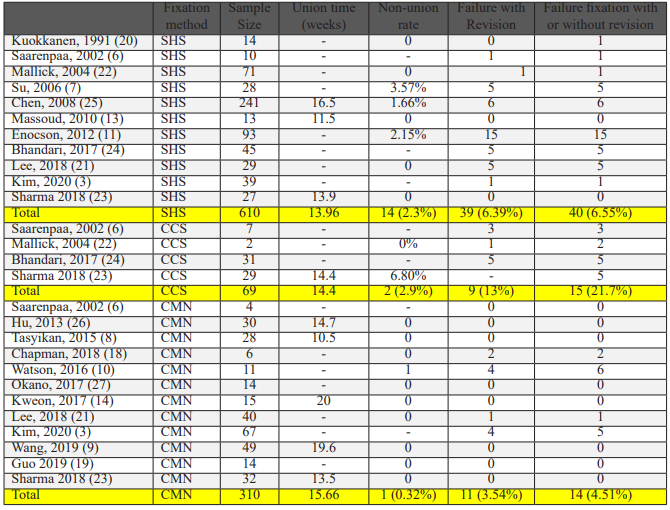
Table 7: Patient reported outcomes.
Analysis
Time to union:
Time to union was similar across fixation methods: SHS (3.1 months), CCS (3.3 months), and CMN (3.6 months). Although CMN had the longest union time, this was not clinically significant, as all patients were permitted to weight-bear as tolerated. This highlights the importance of considering overall recovery and function, not just radiographic union.
Non-Union rates:
Non-union occurred in 2.3% of SHS cases, 2.9% of CCS cases, and 0.32% of CMN cases. Although the differences were not statistically significant (p=0.072), CMN showed a clinically meaningful reduction in non-union rates.
Revision rates:
Revision surgery was required in 6.39% of SHS, 13.04% of CCS, and 3.54% of CMN cases. The difference was statistically significant (p=0.011), suggesting CMN and SHS were more reliable than CCS, with CMN demonstrating the most favourable profile.
Failure rates (with or without revision):
Fixation failure occurred in 6.56% of SHS, 21.74% of CCS, and 4.52% of CMN cases. The differences were highly significant (p<0.00001). Confidence intervals supported this: SHS (CI 4.6%–8.5%), CCS (CI 12.0%–31.5%), and CMN (CI 2.3%–7.7%). These findings highlight the higher mechanical failure rate and uncertainty associated with CCS compared to the more consistent outcomes seen with SHS and CMN.
Sensitivity and Heterogeneity:
Formal sensitivity analyses were not performed due to the descriptive nature of this review and heterogeneity in study design, definitions, and outcomes. Differences in fracture classification, fixation constructs, and follow-up protocols likely contributed to variability in reported outcomes.
Discussion
This review examined fixation strategies for BFNFs. Previous similar reviews [28,29] did not include several pertinent studies considered in this analysis [23,24], and one review included arthroplasty as a treatment option, underscoring the novelty and depth of our review as we focused solely on internal fixation methods to maintain methodological consistency. The FAITH trial is a landmark RCT on femoral neck fractures but did not specifically address basicervical fractures, which have distinct biomechanical characteristics. We incorporated its subset data on basicervical fractures to help address this evidence gap in our focused analysis [24].
Finally, a recent meta-analysis by Yoo et al [30] was found to be in-exhaustive in its literature search and included two articles which did not meet our inclusion criteria (one was reviewing intertrochanteric fractures, one was not yet published in a peer reviewed journal).
Both Yoo et al. and Dekhne et al. highlighted the heterogeneity in defining and managing basicervical fractures, with comparable revision rates reported between CMN and SHS. While Dekhne et al. suggested SHS may have slightly lower reoperation rates, our study found CMN had the lowest failure and revision rates, likely due to stricter inclusion criteria and more consistent definitions. Unlike Yoo et al., who reported variable outcomes with CMNs, our review demonstrated more favourable and reliable results with their use.
BFNFs occupy a transitional anatomical zone between intracapsular and extracapsular fractures, rendering them biomechanically unstable due to high shear forces, reduced cancellous bone interdigitation, and compromised vascularity [13,29-31]. These factors increase the risk of fixation failure, making optimal surgical management critical.
Our findings suggest that CMNs provide the most reliable fixation for BFNFs. CMNs had the lowest fixation failure (4.52%, CI 2.3%–7.7%), revision (3.54%), and non-union rates (0.32%), despite a slightly longer time to union (3.6 months). This extended healing time did not affect post-operative weight-bearing or functional outcomes, supporting CMN's role as a biomechanically superior construct.
Literature purports that the extended union time in CMN could be due to the internal stabilisation mechanisms that allow for controlled load transfer and potentially better adaptation to the mechanical environment of the hip, especially in osteoporotic bones [32,33]. The inherent stability provided by CMN, especially vital in osteoporotic bone [32,33], underscores its suitability for effectively managing these complex fractures.
Historically, SHS with or without anti-rotation screws were favoured; however, CMN have gained preference due to their biomechanical superiority [3,21]. Unlike SHS, which is prone to complications like cut-out and varus collapse, CMN offers a biomechanically advantageous design. Its shorter lever arm and reduced bending moment allow for controlled impaction and stabilisation of the fracture, thus reducing mechanical stress and enhancing healing [11,17,19,21,27], thereby effectively countering the shear forces that may compromise SHS.
Finite analysis in Kwak et al’s paper showed that CMNs distribute stress more effectively across the femoral head, reducing peak stress at the lag screw tip- a major issue of SHS cut-out failures [31].
CMNs also engage the intramedullary canal, reducing axial and cranial migration, whereas SHS relies on lateral fixation, which is more vulnerable to shear forces in BFNFs [31].
CCS limitations include weaker holding capabilities and consequent functional compromise post-operatively, especially in the elderly [34,35]. Comparative studies show that SHS with anti-rotation screws can withstand nearly twice the peak force before failure compared to CCS, and CCS-treated patients exhibit lower ultimate load to failure and lack angular stability leading to higher non-union rates and implant migration [4,5].
Fracture definitions
Fracture classification remains a significant source of heterogeneity across studies [6]. Older studies employed the Arbeitsgemeinschaft für Osteosynthesefragen (AO) classification (B2.1) [7,13,18], while more recent research has adopted the definition by Watson et al.- a two-part fracture at the base of the femoral neck that was medial to the intertrochanteric line and exited above the lesser trochanter but was more lateral than a classic transcervical fracture [3,9,10,21,27]. Consistent use of a standardised definition, such as Watson’s, will improve diagnostic accuracy and facilitate inter-study comparisons.
PROMs
Patient-reported outcome measures (PROMs) varied significantly among studies, hindering direct comparisons. The Harris Hip Score was most reported, but other scoring systems such as SF-12, SF-36, and WOMAC were inconsistently applied. Future studies should prioritise standardised PROMs to enable robust assessment of functional recovery.
Limitations
Limitations of this review include the predominance of retrospective cohort studies and case series, small sample sizes, inconsistent follow-up durations, and moderate-to-high risk of bias in several studies. Additionally, some included studies featured younger patients or high-energy trauma mechanisms, which may not represent typical geriatric hip fracture populations. Publication bias and incomplete reporting of post-operative protocols and complications may also influence findings.
Conclusion
This systematic review provides evidence that CMNs offer a reliable fixation method for BFNFs, with lower failure, revision, and non-union rates compared to SHS and CCS. CMNs demonstrated superior biomechanical stability and resistance to complications such as varus collapse and cut-out. While SHS remains a viable alternative, its biomechanical limitations—particularly in osteoporotic bone—make it less favourable. CCS, associated with the highest failure and revision rates, should be used with caution.
Given the heterogeneity of study designs and the lack of high-quality evidence, definitive recommendations remain limited. Future large, multicentre RCTs are essential to confirm these findings, refine treatment algorithms, and support the development of standardised fracture classifications, fixation protocols, and outcome measures.
Level of Evidence: Level III
Disclosure statement: Each author certifies that there are no funding or commercial associations (consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article related to the author or any immediate family members. AI was used to assist with the general scientific flow of the writing as well as grammar checks.
Location of work: All work was performed at Gold Coast University Hospital, 1 Hospital Blvd, Southport, Qld, 4216.
Funding/Acknowledgements: No fundings were received and there are no acknowledgements to be made.
Contributions:
Joash Kumar – primary author, methodology, data analysis, final manuscript write-up
Tristan Symonds – data collection and literature review, data extraction
Matthew Ludlow - data collection and literature review, data extraction
Jonathan Quinn – data analysis, manuscript review, supervisor
Tom Walsh – manuscript review, supervisor, editor
Simon Platt – conceptualisation, editor, supervisor
References
- Parker M, Johansen A. Hip fracture. Bmj, 2006; 333(7557): 27-30.
- Gullberg B, Johnell O, Kanis JA. World-wide projections for hip fracture. Osteoporos Int, 1997; 7(5): 407-413.
- Kim JT, Ha YC, Park CH, Yoo JI, Kim TY. Single screw type of lag screw results higher reoperation rate in the osteosynthesis of basicervical hip fracture. J Orthop Sci, 2020; 25(1): 152-155.
- Blair B, Koval KJ, Kummer F, Zuckerman JD. Basicervical fractures of the proximal femur. A biomechanical study of 3 internal fixation techniques. Clin Orthop Relat Res, 1994; 306: 256-263.
- Deneka DA, Simonian PT, Stankewich CJ, Eckert D, Chapman JR, Tencer AF. Biomechanical comparison of internal fixation techniques for the treatment of unstable basicervical femoral neck fractures. J Orthop Trauma, 1997; 11(5): 337-343.
- Saarenpää I, Partanen J, Jalovaara P. Basicervical fracture--a rare type of hip fracture. Arch Orthop Trauma Surg, 2002; 122(2): 69-72.
- Su BW, Heyworth BE, Protopsaltis TS, Lipton CB, Sinicropi SM, Chapman CB, et al. Basicervical versus intertrochanteric fractures: an analysis of radiographic and functional outcomes. Orthopedics, 2006; 29(10): 919-925.
- Tasyıkan L, Ugutmen E, Sanel S, Soylemez MS, Ozkan K, Solakoglu C. Short-term results of surgical treatment with cephalomedullary nails for basicervical proximal femoral fractures. Acta Orthop Belg, 2015; 81(3): 427-434.
- Wang Q, Gu XH, Li X, Wu JH, Ju YF, Huang WJ, et al. Management of Low-Energy Basicervical Proximal Femoral Fractures by Proximal Femoral Nail Anti-Rotation. Orthop Surg, 2019; 11(6): 1173-1179.
- Watson ST, Schaller TM, Tanner SL, Adams JD, Jeray KJ. Outcomes of Low-Energy Basicervical Proximal Femoral Fractures Treated with Cephalomedullary Fixation. J Bone Joint Surg Am, 2016; 98(13): 1097-1102.
- Enocson A, Lapidus LJ. The vertical hip fracture - a treatment challenge. A cohort study with an up to 9 year follow-up of 137 consecutive hips treated with sliding hip screw and antirotation screw. BMC Musculoskelet Disord, 2012; 13: 171.
- Sprague S, Bhandari M, Heetveld MJ, Liew S, Scott T, Bzovsky S, et al. Factors associated with health-related quality of life, hip function, and health utility after operative management of femoral neck fractures. Bone Joint J, 2018; 100-b(3): 361-369.
- Massoud EI. Fixation of basicervical and related fractures. Int Orthop, 2010; 34(4): 577-582.
- Kweon SH, Lee SH, Kook SH, Choi YC. Outcomes of Cephalomedullary Nailing in Basicervical Fracture. Hip Pelvis, 2017; 29(4): 270-276.
- Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ, 2021; 372: n71.
- Wells GA, Wells G, Shea B, Shea B, O'Connell D, Peterson J, et al., editors. The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Nonrandomised Studies in Meta-Analyses, 2014.
- Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, et al. RoB 2: a revised tool for assessing risk of bias in randomised trials. Bmj, 2019; 366: l4898.
- Chapman T, Zmistowski B, Krieg J, Stake S, Jones CM, Levicoff E. Helical Blade Versus Screw Fixation in the Treatment of Hip Fractures With Cephalomedullary Devices: Incidence of Failure and Atypical "Medial Cutout". J Orthop Trauma, 2018; 32(8): 397-402.
- Guo J, Dong W, Jin L, Yin Y, Zhang R, Hou Z, et al. Treatment of basicervical femoral neck fractures with proximal femoral nail antirotation. J Int Med Res, 2019; 47(9): 4333-4343.
- Kuokkanen HO. Treatment options for basicervical fractures of the femoral neck. A clinical follow-up. Acta Orthop Belg, 1991; 57(2): 162-168.
- Lee YK, Yoon BH, Hwang JS, Cha YH, Kim KC, Koo KH. Risk factors of fixation failure in basicervical femoral neck fracture: Which device is optimal for fixation? Injury, 2018; 49(3): 691-696.
- Mallick A, Parker MJ. Basal fractures of the femoral neck: intra- or extra-capsular. Injury, 2004; 35(10): 989-993.
- Sharma A, Sethi A, Sharma S. Comparative analysis of treatment of basicervical femur fractures in young adults with CCS, DHS, and PFN. Rev Bras Ortop, 2018; 53(6): 783-787.
- Bhandari M. Fracture fixation in the operative management of hip fractures (FAITH): an international, multicentre, randomised controlled trial. Lancet, 2017; 389(10078): 1519-1527.
- Chen CY, Chiu FY, Chen CM, Huang CK, Chen WM, Chen TH. Surgical treatment of basicervical fractures of femur--a prospective evaluation of 269 patients. J Trauma, 2008; 64(2): 427-429.
- Hu SJ, Yu GR, Zhang SM. Surgical treatment of basicervical intertrochanteric fractures of the proximal femur with cephalomeduallary hip nails. Orthop Surg, 2013; 5(2): 124-129.
- Okano I, Sawada T, Kushima N, Tachibana T, Inagaki K. Treatment With Helical Blade Cephalomedullary Nail for Two-Part Basicervical Proximal Femoral Fracture in Elderly Patients: A Retrospective Observational Study. Geriatr Orthop Surg Rehabil, 2017; 8(4): 244-251.
- Dekhne MS, Thomas HM, Haider T, Mortensen S, Rodriguez EK, Weaver MJ, et al. Treatment and outcomes of basicervical femoral neck fractures: A systematic review. Journal of Orthopaedic Surgery, 2021; 29(1): 23094990211003344.
- Yoo JI, Cha Y, Kwak J, Kim HY, Choy WS. Review on Basicervical Femoral Neck Fracture: Definition, Treatments, and Failures. Hip Pelvis, 2020; 32(4): 170-181.
- Yoon YC, Kim CH, Kim YC, Song HK. Cephalomedullary Nailing versus Dynamic Hip Screw Fixation in Basicervical Femoral Neck Fracture: A Systematic Review and Meta-Analysis. Yonsei Med J, 2022; 63(8): 744-750.
- Kwak DK, Kim WH, Lee SJ, Rhyu SH, Jang CY, Yoo JH. Biomechanical Comparison of Three Different Intramedullary Nails for Fixation of Unstable Basicervical Intertrochanteric Fractures of the Proximal Femur: Experimental Studies. Biomed Res Int, 2018; 2018: 7618079.
- Jones HW, Johnston P, Parker M. Are short femoral nails superior to the sliding hip screw? A meta-analysis of 24 studies involving 3,279 fractures. Int Orthop, 2006; 30(2): 69-78.
- Mahomed N, Harrington I, Kellam J, Maistrelli G, Hearn T, Vroemen J. Biomechanical analysis of the Gamma nail and sliding hip screw. Clin Orthop Relat Res, 1994; 304: 280-288.
- Kumar J, Symonds T, Quinn J, Walsh T, Platt S. What is the best method of fixation for minimally displaced subcapital neck of femur fractures? A systematic review. J Orthop, 2023; 45: 54-60.
- Parker MJ. Results of internal fixation of Pauwels type-3 vertical femoral neck fractures. J Bone Joint Surg Am, 2009; 91(2): 490-491.

