Excessive Gingival Display Due to Altered Passive Eruption: From Diagnosis to Smile Rehabilitation - A Contemporary Literature Review
Chariklia Neophytou1,*, Avra Maria Neofytou2, Eirini Salvanou2, Sotiria Davidopoulou3 and Konstantinos Papadimitriou1
1Department of Preventive Dentistry, Periodontology and Implant Biology, Dental School, Aristotle University of Thessaloniki, 54124 Thessaloniki, Greece
2Dental School, Aristotle University of Thessaloniki, 54124 Thessaloniki, Greece
3Department of Operative Dentistry, Dental School, Aristotle University of Thessaloniki, 54124 Thessaloniki, Greece
Received Date: 23/07/2025; Published Date: 04/09/2025
*Corresponding author: Chariklia Neophytou, Department of Preventive Dentistry, Periodontology and Implant Biology, Dental School, Aristotle University of Thessaloniki, 54124 Thessaloniki, Greece
Abstract
Background: An esthetically pleasing smile is defined by the harmonious interplay of the teeth, lips, and gingival architecture. Excessive gingival display (EGD), often referred to as a "gummy smile," can significantly impact facial esthetics and patient self-esteem. Among its etiologies, Altered Passive Eruption (APE) is a common and frequent condition that disrupts the normal relationship between teeth and gingiva.
Objective: This review provides a comprehensive overview of the diagnosis and management of EGD, with an emphasis on APE as a primary cause. It aims to guide clinicians in differentiating between the various etiologies of EGD and selecting evidence-based, individualized treatment strategies.
Methods: A literature search was performed in PubMed, Scopus, Cochrane, and Embase using the terms “excessive gingival display” and “altered passive eruption”. The review focuses on classification, diagnosis, and treatment options for EGD, with emphasis on APE. Key aspects include clinical and radiographic evaluation, as well as the role of digital planning in modern treatment approaches.
Results: APE is classified into distinct subtypes (Type 1A, 1B, 2A, 2B), each requiring a tailored surgical approach. Procedures range from simple gingivectomy to flap surgery with osseous resection, depending on the relationship between the cemento-enamel junction (CEJ) and alveolar bone crest. The preservation and understanding of biologic width are critical for ensuring periodontal health and preventing relapse. The use of digital workflows and surgical guides, especially the double-guide concept, enhances precision, particularly in cases requiring bone recontouring. Postoperative care, appropriate healing periods, and careful timing of restorative phases are essential for long-term success.
Conclusion: Effective management of APE and EGD necessitates a multidisciplinary, patient-specific approach involving periodontics, prosthodontics, and, when needed, orthodontics. Proper diagnosis, biologic principles, and modern digital planning tools are key to achieving optimal esthetic and functional outcomes. With careful planning and execution, crown-lengthening procedures for APE can significantly improve smile harmony, support restorative success, and promote long-term periodontal stability.
Keywords: Excessive gingival display; Altered passive eruption; Gummy smile; Esthetic crown lengthening; Periodontal diagnosis; Smile design; Digital planning; Double guide concept; Gingivectomy; Ostectomy; Surgical guide
Abbreviations: ABC – Alveolar Bone Crest; APE – Altered Passive Eruption; APF – Apically Positioned Flap; CBCT – Cone Beam Computed Tomography; CEJ – Cementoenamel Junction; DGU – Dentogingival Unit; EGD – Excessive Gingival Display; GS – Gummy Smile; MGJ – Mucogingival Junction; OHI – Oral Hygiene Instruction; VME – Vertical Maxillary Excess
Introduction
Excessive Gingival Display (EGD), commonly referred to as a "Gummy Smile" (GS), is a frequent esthetic concern that can significantly impact a patient’s self-perception and quality of life. While multiple etiological factors may contribute to EGD, including skeletal discrepancies, dentoalveolar extrusion, and soft tissue variations, altered passive eruption (APE) remains an underdiagnosed yet highly treatable cause. With advances in diagnostic imaging, surgical techniques, and digital workflows, clinicians are now better equipped to accurately identify APE and tailor minimally invasive treatments for optimal esthetic outcomes. This review aims to provide a focused update on the classification, diagnostic protocols, and treatment strategies specific to EGD due to APE, emphasizing a modern, evidence-based, and interdisciplinary approach.
Methods and Materials
This narrative review was conducted through an electronic search of four major databases: PubMed, Scopus, Cochrane Library, and Embase. The search strategy employed the keywords: “excessive gingival display” OR “altered passive eruption.” Relevant literature published in English up to July 2025 was considered. Articles were selected based on their focus on the etiology, classification, diagnosis, and treatment of APE-related EGD. Additional manual screening of reference lists was performed to identify key studies. Both clinical and radiographic diagnostic approaches, as well as analog and digital treatment modalities, were reviewed to provide a comprehensive synthesis of current best practices.
Aesthetic Smile Characteristics
The aesthetic perception of a smile is governed by the harmonious interplay between three primary elements: (a) the dentition, (b) the surrounding soft tissue framework, and (c) the gingival architecture [1]. The lips serve as the natural frame of the smile, defining the aesthetic zone and influencing the overall perception of dental and facial harmony. Smile lines are commonly classified as high, average, or low, based on the extent of tooth and gingival exposure during smiling [2].
In Western populations, the average smile line, characterized by complete visibility of the upper anterior teeth and approximately 1–2 mm of gingival exposure, is considered the most aesthetically pleasing. A low smile line conceals up to 75% of the anterior dentition, while a high smile line reveals all anterior teeth along with more than 2 mm of gingival tissue, a condition referred to as EGD or GS [2].
Although gingival display is not intrinsically unaesthetic, disproportionate exposure, particularly when associated with tissue asymmetries or irregularities, can compromise smile harmony. Both clinicians and lay observers have demonstrated sensitivity to such discrepancies, often perceiving EGD or midline asymmetries as unattractive [3,4]. The psychosocial impact may be profound, influencing self-esteem, social interactions, and overall quality of life [5,6].
An esthetically pleasing smile typically features a dental midline aligned with the facial midline, a smile arc that mirrors the curvature of the lower lip, and symmetrical, vertically aligned central incisors. The incisal embrasures should deepen gradually from central to canine teeth, and the upper teeth should ideally display a width-to-length ratio of 75–80% [7]. Visibility of maxillary teeth up to the second premolars, minimal (<3 mm) gingival display, and complete interdental papillae with no signs of recession or overgrowth are also considered optimal [8]. The incisal edge of the upper anterior teeth should trace a line parallel to the lower lip and to an imaginary interproximal contact line, contributing to overall smile symmetry and esthetic balance.
Excessive Gingival Display
As defined, EGD is the exposure of the full maxillary anterior dentition accompanied by more than 2 mm of gingival tissue during smiling [2]. Epidemiologically, it affects approximately 7% of males and 14% of females between the ages of 20 and 30, with prevalence declining with age due to soft tissue sagging and lip elongation [9].
Wu et al. classified EGD into four distinct types [10]:
- Type I: Continuous band of gingival display (most common)
- Type II: Excessive posterior gingival display
- Type III: Unilateral gingival display
- Type IV: Localized anterior gingival display
Diagnosis:
EGD is a multifactorial condition necessitating a systematic diagnostic approach to identify its etiology, which may be soft tissue, dental, skeletal, or a combination of these [11,12]. The most common etiologies include:
- Altered Passive Eruption (APE): Incomplete apical migration of the gingival margin following tooth eruption, resulting in short clinical crowns despite normal anatomic crown length.
- Vertical Maxillary Excess (VME): Vertical overgrowth of the maxilla leading to an increased lower facial height and gingival exposure, despite normal tooth dimensions.
- Hypermobile Upper Lip: Excessive elevation (>8 mm) of the upper lip during smiling due to hyperactivity of elevator muscles such as the levator labii superioris and levator labii superioris alaeque nasi.
- Short Upper Lip: Defined as a vertical lip length <20 mm in females or <22 mm in males (measured from subnasale to stomion), often contributing to gingival visibility even at rest.
- Anterior Dentoalveolar Extrusion: Overeruption of the anterior teeth and associated alveolar bone, commonly observed in deep bite cases. The gingival margin follows the incisal edge, enhancing the gingival display.
- Inflammatory or Drug-Induced Gingival Hyperplasia: Gingival overgrowth secondary to plaque-induced inflammation or pharmacologic agents (e.g., phenytoin, cyclosporine, calcium channel blockers).
In many patients, EGD arises from a combination of these factors, underscoring the importance of accurate diagnosis to inform appropriate treatment planning [13,14].
A comprehensive diagnostic protocol should include:
- Medical and dental history
- Photographic analysis (frontal, lateral, and dynamic smile images)
- Lip analysis (mobility, length, incisor show at rest and during smiling)
- Periodontal evaluation (gingival margin, crown dimensions, probing depth)
- Radiographic assessment (to determine crown-root ratio, bone levels)
- Cephalometric analysis (especially critical in evaluating skeletal components such as VME) (15).
Treatment:
Management of EGD should be etiology-driven and individualized. Conservative, minimally invasive therapies such as botulinum toxin or hyaluronic acid injections, are suitable for cases related to lip hyperactivity. Both are minimally invasive. Botox is reversible in 3–6 months; hyaluronic acid offers more volume modulation but requires anatomical precision. More invasive interventions, including lip repositioning, crown lengthening, orthodontic therapy, and orthognathic surgery, are indicated based on the dental or skeletal origin of the condition.
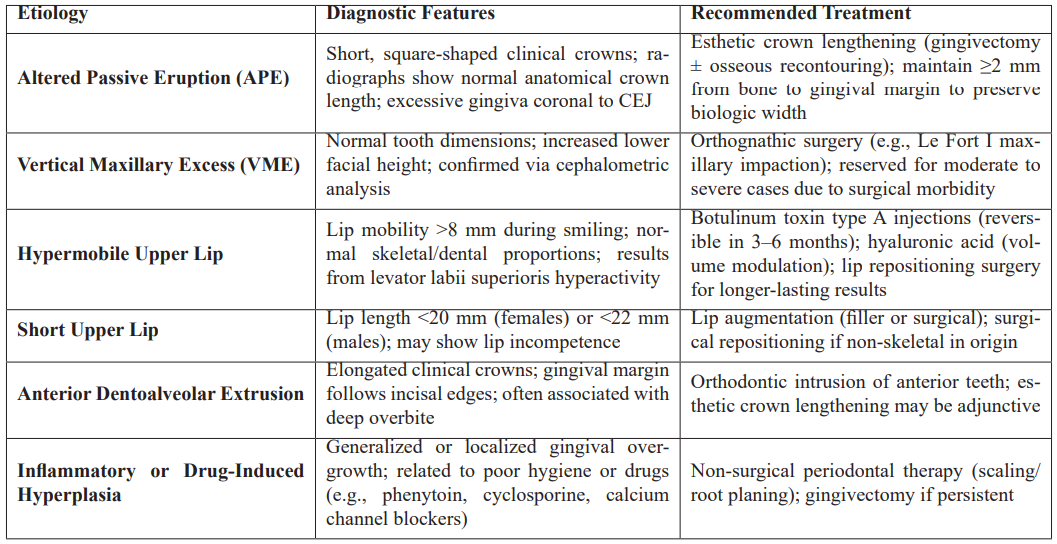
Multifactorial cases often require a multidisciplinary approach, integrating periodontal, orthodontic, and surgical disciplines to achieve long-term esthetic and functional outcomes. The Table 1 summarizes key diagnostic indicators and recommended evidence-based treatments [14,15]:
Table 1: Diagnostic indicators and recommended treatments for Excessive Gingival Display.
Altered Passive Eruption
Tooth eruption is a physiological process comprising two distinct phases: active eruption and passive eruption. Active eruption refers to the vertical emergence of the tooth through the alveolar bone and gingiva until it reaches the occlusal plane. During this phase, the gingiva follows the crown coronally. Subsequently, passive eruption occurs, characterized by the apical migration of the gingival margin, exposing more of the clinical crown until it stabilizes slightly coronal to the Cemento-Enamel Junction (CEJ) (16). Passive eruption proceeds through four histological stages: (1) junctional epithelium located entirely on enamel, (2) partly on enamel and cementum, (3) entirely on cementum with the base of the sulcus at the CEJ, and (4) apical migration beyond the CEJ with partial root exposure [17].
In some individuals, this apical migration does not progress adequately, leaving the gingival margin in a more coronal position. This condition, known as altered or retarded or delayed passive eruption, results in excessive gingival coverage of anatomically normal crowns, giving the appearance of short clinical crowns [18].
APE is generally diagnosed after skeletal growth completion (around 18–20 years), although soft tissue maturation, particularly in posterior segments, may continue into the third decade [19]. Epidemiologic studies report an APE prevalence of approximately 12%, with a significantly higher incidence in patients with a thick gingival biotype compared to those with a thin biotype [20-23].
From a diagnostic perspective, gingival coverage exceeding 19% of the anatomic crown height strongly suggests APE [16,24]. Histologically, APE is marked by a long junctional epithelium firmly attached to the enamel, a normal sulcus depth, and a shortened connective tissue zone. A coronal alveolar crest position compromises the biologic width, disrupting the normal spatial relationship between CEJ and bone crest [25].
Etiology and Contributing Factors:
APE is multifactorial, influenced by anatomical and systemic factors that interfere with normal apical migration of gingival tissues:
- Thick, fibrotic gingival biotype resistant to migration
- Excessive buccal bone thickness, impeding bone remodeling
- Occlusal trauma or soft tissue interference during eruption
- Genetic predisposition affecting eruption patterns
- Orthodontic trauma (e.g., intrusive forces)
- Systemic or endocrine disorders affecting tissue homeostasis [17,26].
Zucchelli et al. [27] emphasized the frequent association of thick buccal bone with APE, highlighting the importance of osseous resection for successful surgical correction. This excess bone may be both a cause and consequence of APE [16].
Two principal morphologic patterns are identified:
- Eruption space deficiency due to reduced maxillo-mandibular vertical dimension, often influenced by facial growth pattern
- Tissue dimension mismatch, where thick gingival or periodontal tissues inhibit apical migration [16].
Classification:
APE is classified based on two anatomical relationships (Figure 1) [28-30]:
- The position of the Mucogingival Junction (MGJ) relative to the Alveolar Bone Crest (ABC)
- The position of the ABC relative to the CEJ
This dual classification helps assess both soft and hard tissue morphology and is essential for guiding appropriate surgical treatment planning.
A. Classification Based on MGJ–ABC Relationship
Type 1 APE: Wide band of attached gingiva with MGJ apical to alveolar crest.
Type 2 APE: Normal width of attached gingiva located entirely on the crown; MGJ near CEJ.
Normal attached gingiva ranges from 3.0–4.2 mm in the maxilla and 2.5–2.6 mm in the mandible [31].
B. Classification Based on ABC–CEJ Relationship
Subgroup A: Bone crest 1–2 mm apical to CEJ (normal).
Subgroup B: Bone crest at or coronal to CEJ, encroaching on biologic width.
These parameters yield four clinical subtypes: Type 1A, 1B, 2A, and 2B, each with distinct surgical implications [7,18,24].
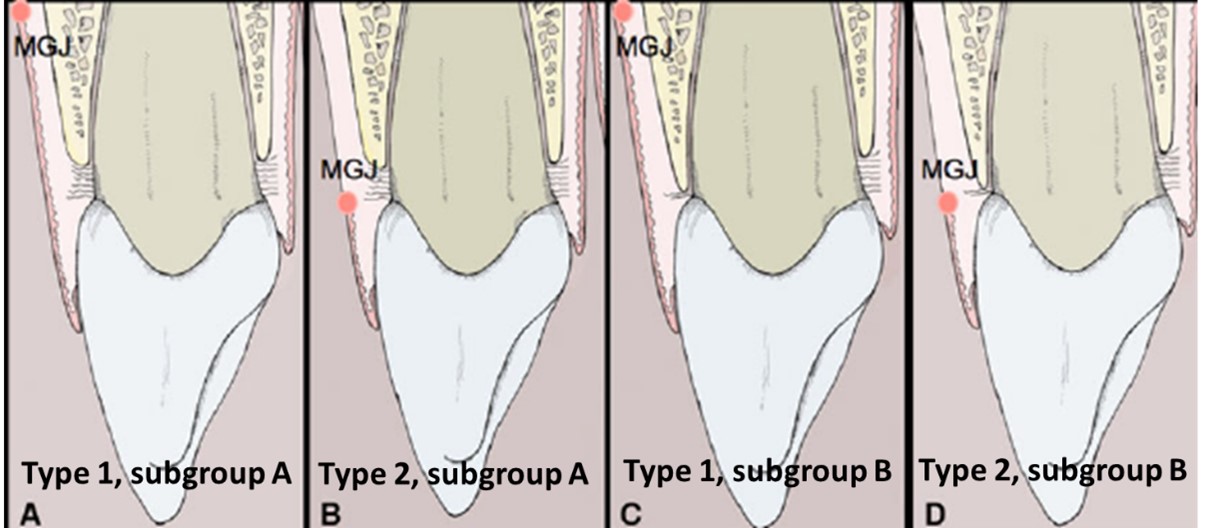
Figure 1: Classification of Altered Passive Eruption based on MGJ–ABC and ABC–CEJ relationship.
Treatment:
Diagnostic Algorithm and Clinical Decision-Making
Accurate diagnosis, guided by a structured algorithm, is essential for precise treatment selection (Figure 2) [32]:
- Incisal edge positioned coronally with deep overbite: Orthodontic intrusion followed by reevaluation for crown lengthening
- Proper incisal edge and intact teeth: Esthetic crown lengthening indicated
- Incisal edge worn: Restorative rehabilitation needed; resistance form assessed to determine surgical extent
Techniques for esthetic crown lengthening treatment planning include:
- Traditional Approach: A method based on clinical experience and periodontal measurements. While simple and accessible, this technique may lack precision and is most suitable for straightforward cases.
- Chu Proportion Gauge: A specialized tool that aids in determining ideal tooth proportions and gingival symmetry, offering greater precision in planning soft tissue recontouring.
- Digitally Designed 3D-Printed Surgical Guides: The most advanced and accurate approach, utilizing CBCT and intraoral scanning for preoperative planning of both soft and hard tissue modifications. This technique enhances precision, reduces chair time, and supports optimal esthetic outcomes.
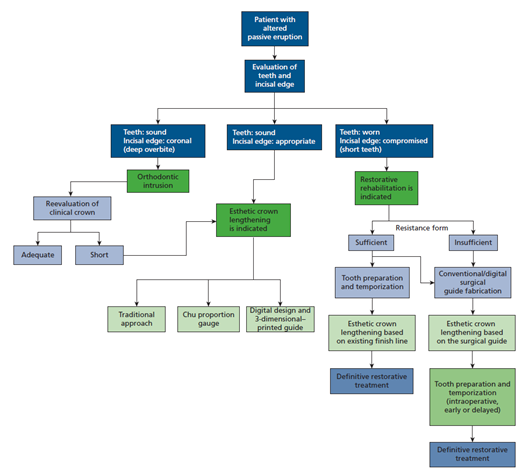
Figure 2: Diagnostic algorithm and clinical decision-making for altered passive eruption.
Surgical Management:
Treatment begins with a presurgical phase focused on plaque control and inflammation reduction (e.g., scaling and root planing), enabling accurate gingival margin assessment [12,33,34].
Once periodontal health is achieved, crown-lengthening surgery proceeds.
Surgical Guide Selection:
Table 2 summarizes the available surgical guides for the crown-lengthening surgery.
Table 2: Surgical guides for esthetic crown-lengthening.
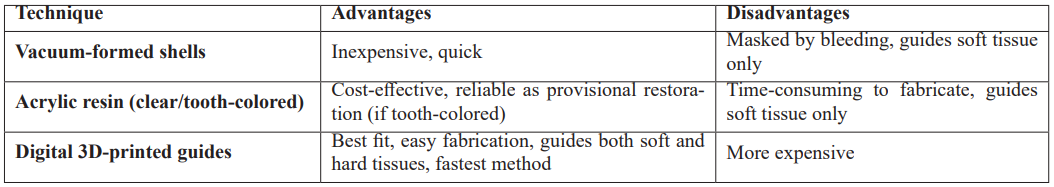

The digital approach offers the highest level of precision in esthetic crown lengthening procedures, providing guidance for both soft and hard tissue modifications, a critical advantage when osseous resection is required [35]. By superimposing CBCT data with intraoral scans, clinicians can accurately identify the CEJ and plan the desired final bone level. This digital workflow enables the fabrication of a custom 3D-printed surgical guide, ensuring precise execution of both gingivectomy and ostectomy. This double-guide concept represents the most advanced and predictable method for managing cases of APE, offering superior esthetic outcomes, surgical efficiency, and long-term stability [36-39].
Type of surgical intervention in esthetic crown lengthening:
Planning surgical intervention for esthetic crown lengthening requires careful evaluation of several anatomical parameters, including the width and height of keratinized gingiva, the position of the MGJ, the location of the buccal ABC relative to the CEJ, and the anticipated restorative requirements [7,40,41]. These factors determine whether a case is amenable to a simple gingivectomy or requires a full-thickness flap with osseous resection.
When the alveolar bone crest lies at a normal apical distance from the CEJ (≥1 mm) and at least 3 mm of soft tissue is present between the gingival margin and bone crest, as seen in Type 1A APE, a gingivectomy alone may be sufficient. In these cases, both the attached gingiva and biologic width are preserved. Removal of excess gingival tissue can effectively expose more of the clinical crown without compromising the Dentogingival Unit (DGU), resulting in improved gingival contours and esthetic outcomes. In some Type 1A cases, where preservation of the entire band of keratinized tissue is desired, an Apically Positioned Flap (APF) may be used instead. This technique repositions the gingival margin apically while maintaining soft tissue integrity.
In Type 2A APE, a conventional gingivectomy risks removing the entire zone of keratinized gingiva, potentially leading to an unfavorable mucogingival relationship. In such scenarios, an apically repositioned flap is the preferred surgical approach. This technique re-establishes the band of keratinized tissue closer to the CEJ, thereby preserving both esthetic and functional soft tissue dimensions.
In Type 1B and 2B APE, the alveolar bone crest is located at or coronal to the CEJ. Performing a gingivectomy alone in these cases will violate the biologic width and result in chronic inflammation, gingival recession, or alveolar bone loss. Therefore, a full-thickness mucoperiosteal flap must be raised, followed by osseous resection (ostectomy) to apically reposition the bone crest and reestablish the proper biologic width.
In patients with a thick periodontal phenotype, additional osteoplasty is often required to reduce buccal bone thickness and minimize the risk of soft tissue rebound—a frequent cause of surgical relapse if the bone is not adequately thinned [42-44]. After hard tissue recontouring, the flap is repositioned and sutured at a more apical level, supporting long-term periodontal health and stable gingival margins.
In Type 1B cases, a preliminary gingivectomy may be performed to establish the ideal gingival margin before osseous resection, especially when an adequate band of keratinized tissue is present.
Figure 3 illustrates the treatment options, which should be selected based on the specific APE Type and Subgroup of the case.
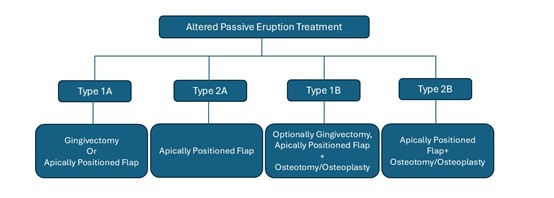
Figure 3: Treatment approaches based on the specific APE Type and Subgroup.
Biologic Width Considerations:
The concept of biologic width is fundamental to crown-lengthening procedures. Initially defined by Gargiulo et al., the biologic width encompasses the junctional epithelium (approximately 0.97 mm) and connective tissue attachment (approximately 1.07 mm), with an average total of 2.04 mm (45). More recent investigations report similar average values ranging from 2.15 to 2.30 mm, but highlight considerable individual variation, with biologic widths ranging from 0.2 mm to 6.7 mm. These findings underscore that no universal biologic width exists, and a personalized approach is essential.
Postoperative Management:
Effective postoperative care is critical to surgical success. Patients should be prescribed analgesics and instructed to rinse with 0.12% chlorhexidine gluconate twice daily for the first two weeks. Sutures are typically removed within 7–14 days, at which point supragingival prophylaxis and oral hygiene instruction (OHI) are reinforced. Patients are advised to begin gentle brushing with a surgical extra-soft toothbrush once sutures are removed.
Frequent recall visits are scheduled initially, followed by three-month maintenance intervals to assess healing, reinforce OHI, and perform routine prophylaxis. Regular monitoring is essential to detect early signs of relapse or inflammation.
The successful treatment of Altered Passive Eruption (APE) relies on a systematic, multidisciplinary approach integrating periodontology, prosthodontics, and, in some cases, orthodontics. Critical elements of success include:
- Accurate diagnosis and presurgical planning
- Comprehensive understanding of biologic width and anatomic variation
- Selection of the appropriate surgical technique tailored to the APE classification
- Adequate healing time before restorative procedures
- Careful postoperative care and long-term follow-up
When performed with attention to biologic principles, individual anatomy, and patient-specific goals, crown-lengthening procedures can deliver significant improvements in smile esthetics, restorative outcomes, and periodontal health. Long-term success is highly dependent on patient compliance, interdisciplinary coordination, and regular maintenance.
Post-Surgical Restorative Phase:
Following a healing period, the restorative phase may begin [46]. At this stage, veneers or fixed dental prostheses can be fabricated to address esthetic concerns and restore function. Allowing sufficient healing time is essential to avoid gingival rebound or relapse. Bibliography is not conclusive- it shows valiable time as adequate for the healing time: 6 weeks until >6 months [47,48]. Final restorations should respect the newly established gingival architecture and biologic width [49].
Conclusion
The successful treatment of APE relies on a systematic, multidisciplinary approach integrating periodontology, prosthodontics, and, in some cases, orthodontics. Critical elements of success include:
- Accurate diagnosis and presurgical planning
- Comprehensive understanding of biologic width and anatomic variation
- Selection of the appropriate surgical technique tailored to the APE classification
- Adequate healing time before restorative procedures
- Careful postoperative care and long-term follow-up
When performed with attention to biologic principles, individual anatomy, and patient-specific goals, crown-lengthening procedures can deliver significant improvements in smile esthetics, restorative outcomes, and periodontal health. Long-term success is highly dependent on patient compliance, interdisciplinary coordination, and regular maintenance.
References
- Garber DA, Salama MA. The aesthetic smile: Diagnosis and treatment. Periodontol 2000; 1996; 11(1): 18–28.
- Peck S, Peck L, Kataja M. The gingival smile lines. Angle Orthodontist, 1992; 62(2): 91–100; discussion 101.
- Kokich VO, Asuman Kiyak H, Shapiro PA. Comparing the perception of dentists and lay people to altered dental esthetics. Journal of Esthetic and Restorative Dentistry, 1999; 11(6): 311–324.
- Kokich VO, Kokich VG, Kiyak HA. Perceptions of dental professionals and laypersons to altered dental esthetics: Asymmetric and symmetric situations. American Journal of Orthodontics and Dentofacial Orthopedics, 2006; 130(2): 141–151.
- Malkinson S, Waldrop TC, Gunsolley JC, Lanning SK, Sabatini R. The Effect of Esthetic Crown Lengthening on Perceptions of a Patient’s Attractiveness, Friendliness, Trustworthiness, Intelligence, and Self‐Confidence. J Periodontol, 2013; 84(8): 1126–1133.
- Kerosuo H, Hausen H, Laine T, Shaw WC. The influence of incisal malocclusion on the social attractiveness of young adults in finland. Eur J Orthod, 1995; 17(6): 505–512.
- Mele M, Felice P, Sharma P, Mazzotti C, Bellone P, Zucchelli G. Esthetic treatment of altered passive eruption. Periodontol 2000, 2018; 77(1): 65–83.
- Assessment of the “golden proportion” in agreeable smiles – PubMed, 2025.
- Vig RG, Brundo GC. The kinetics of anterior tooth display. J Prosthet Dent, 1978; 39(5): 502–504.
- Wu H, Lin J, Zhou L, Bai D. Classification and craniofacial features of gummy smile in adolescents. Journal of Craniofacial Surgery, 2010; 21(5): 1474–1479.
- Levine RA, McGuire M. The diagnosis and treatment of the gummy smile. Compend Contin Educ Dent, 1997; 18(8).
- Robbins JW. Differential diagnosis and treatment of excess gingival display. Pract Periodontics Aesthet Dent, 1999; 11(2): 265–72; quiz 273.
- Castro LT de, Sementille MCC, Ragghianti Zangrando MS, Greghi SLA, Damante CA, Sant’Ana E, et al. Facial, dental, periodontal, and tomographic characteristics of the etiology of excessive gingival display: a cross-sectional clinical study. J Periodontal Implant Sci, 2024; 54(6).
- Mohamed Ali J, Ines D. Excessive Gingival Display. StatPearls, 2023.
- Excessive gingival display--etiology, diagnosis, and treatment modalities – PubMed, 2025.
- Alpiste-Illueca F. Morphology and dimensions of the dentogingival unit in the altered passive eruption. Med Oral Patol Oral Cir Bucal, 2012; 17(5): e814.
- Mele M, Felice P, Sharma P, Mazzotti C, Bellone P, Zucchelli G. Esthetic treatment of altered passive eruption. Periodontol 2000, 2018; 77(1): 65–83.
- Henry M Goldman, Walter Cohen D, Henry M Goldman. Periodontal therapy. Open Library, 2025.
- Volchansky A, Cleaton-jones P. Delayed passive eruption - A predisposing factor to Vincent’s Infection? 1974.
- Volchansky A, Cleaton-Jones PE. Delayed passive eruption. A predisposing factor to Vincent’s infection? J Dent Assoc S Afr, 1974: 29: 291–294.
- Nart J, Carrió N, Valles C, Solís‐Moreno C, Nart M, Reñé R, et al. Prevalence of Altered Passive Eruption in Orthodontically Treated and Untreated Patients. J Periodontol, 2014; 85(11).
- Lamichhane S, Humagain M, Thapa S, Bhusal S, Rijal AH, Rupakhety P, et al. Altered Passive Eruption among Patients Visiting Dental Outpatient Department in a Tertiary Care Center: A Descriptive Cross-sectional Study. Journal of the Nepal Medical Association. 2024; 62(273): 284–287.
- Rakmanee T, Phromngam Y, Thipraksa R, Janaphan K. Clinical and radiographic assessment of gummy smile patients with altered passive eruption: a cross-sectional study in a Thai population. Clin Oral Investig, 2024; 28(10): 530.
- Coslet JG, Vanarsdall R, Weisgold A. Diagnosis and classification of delayed passive eruption of the dentogingival junction in the adult. Alpha Omegan, 1977; 70(3): 24–28.
- Pilloni A, Marini L, Zeza B, Ferlosio A, Aghazada R. Histologic Analysis of Clinically Healthy Human Gingiva in Patients with Altered Passive Eruption. Dent J (Basel), 2021; 9(3): 29.
- Moshrefi A. book ch 19- periodontal-Altered passive eruption. J West Soc Periodontol Periodontal Abstr, 2000; 48: 5–8.
- Giovanni Zucchelli. Mucogingival Esthetic Surgery. Quintessence Publishing Company, Ltd, 2025.
- Coslet JG, Vanarsdall R, Weisgold A. Diagnosis and classification of delayed passive eruption of the dentogingival junction in the adult. Alpha Omegan, 1977; 70(3): 24–28.
- Alpiste-Illueca F. Altered passive eruption (APE): a little-known clinical situation. Med Oral Patol Oral Cir Bucal, 2011; 16(1): e100-4.
- Evian CI, Cutler SA, Rosenberg ES, Shah RK. Altered passive eruption: the undiagnosed entity. J Am Dent Assoc, 1993; 124(10): 107–110.
- Wang IC, Chan HL, Johnson GK, Elangovan S. Assessment of Negative Gingival Recession: A Critical Component of Periodontal Diagnosis. Applied Sciences (Switzerland). 2022; 12(14): 7015.
- Kao RT, Dault S, Frangadakis K, Salehieh JJ. Esthetic crown lengthening: appropriate diagnosis for achieving gingival balance. J Calif Dent Assoc, 2008; 36(3): 187–191.
- Rossi R, Benedetti R, Santos-Morales RI. Treatment of altered passive eruption: periodontal plastic surgery of the dentogingival junction. Eur J Esthet Dent, 2008; 3(3): 212–223.
- Majzoub ZAK, Romanos A, Cordioli G. Crown lengthening procedures: A literature review. Semin Orthod, 2014; 20(3): 188–207.
- Alhumaidan A, al-Qarni F, AlSharief M, AlShammasi B, Albasry Z. Surgical guides for esthetic crown lengthening procedures. The Journal of the American Dental Association, 2022; 153(1): 31–38.
- Carrera TMI, Freire AEN, de Oliveira GJPL, dos Reis Nicolau S, Pichotano EC, Junior NVR, et al. Digital planning and guided dual technique in esthetic crown lengthening: a randomized controlled clinical trial. Clin Oral Investig, 2023; 27(4): 1589–1603.
- Borham E, Abuel-Ela HA, Mohamed IS, Fouad YA. Treatment of excessive gingival display using conventional esthetic crown lengthening versus computer guided esthetic crown lengthening: (a randomized clinical trial). BMC Oral Health, 2024; 24(1).
- Longo E, de Giovanni F, Napolitano F, Rossi R. Double guide concept: A new digital paradigm for the treatment of altered passive eruption in patients with high esthetic expectations. International Journal of Esthetic Dentistry, 2022; 17(3): 254–265.
- Rossi R, Longo E, Cozzani M. Diagnosis and inter-disciplinary treatment of altered passive eruption, the digital evolution. Semin Orthod, 2024; 30(2): 190–205.
- Sonick M. Esthetic crown lengthening for maxillary anterior teeth. Compend Contin Educ Dent, 1997; 18(8).
- Foley TF, Sandhu HS, Athanasopoulos C. Esthetic periodontal considerations in orthodontic treatment--the management of excessive gingival display. J Can Dent Assoc, 2003; 69(6): 368–372.
- Al-Sowygh ZH. Does Surgical Crown Lengthening Procedure Produce Stable Clinical Outcomes for Restorative Treatment? A Meta-Analysis. Journal of Prosthodontics. Blackwell Publishing Inc, 2019; 28: p. e103–109.
- Arora R, Narula SC, Sharma RK, Tewari S. Evaluation of Supracrestal Gingival Tissue After Surgical Crown Lengthening: A 6‐Month Clinical Study. J Periodontol, 2013; 84(7): 934–940.
- Pontoriero R, Carnevale G. Surgical Crown Lengthening: A 12-Month Clinical Wound Healing Study. J Periodontol, 2001.
- Gargiulo A, Wentz F, of BOTJ, 1961 undefined. Dimensions and relations of the dentogingival junction in humans. Wiley Online LibraryAW Gargiulo, FM Wentz, B OrbanThe Journal of Periodontology, 1961•Wiley Online Library, 1961; 32(3): 261–267.
- Marzadori M, Stefanini M, Sangiorgi M, Mounssif I, Monaco C, Zucchelli G. Crown lengthening and restorative procedures in the esthetic zone. Periodontol 2000, 2018; 77(1): 84–92.
- Malamoudi GA, Tsachouridou I, Menexes G, Mikrogeorgis G, Tortopidis D, Tsalikis L. Pre-restorative crown lengthening surgery: influence of restorative treatment timing on clinical outcomes—a pilot study. Oral Maxillofac Surg, 2024; 28(1): 253–267.
- Abou‐Arraj RV, Majzoub ZAK, Holmes CM, Geisinger ML, Geurs NC. Healing Time for Final Restorative Therapy After Surgical Crown Lengthening Procedures: A Review of Related Evidence. Clin Adv Periodontics, 2015; 5(2): 131–139.
- Schä M, Lang NP, Ånerud Å, Boysen H, Bü W, Lö H. The influence of margins of. J Clin Periodontol, 2001; 28: 57–64.

