Are Prophylactic Antibiotics Still Required for Inguinal Herniotomy in Children?
Fatima Majeed1,*, Ayesha Manzoor2, Smika Shafique3, Muhammad Huzaifa Khalil3, Amna Rafaqat4, Nisha Shan5, Muhammad Saleem6 and Faiza Ashraf6
1Department of Pediatrics Surgery, King Saud Medical City, Riyadh, KSA
2Department of Pediatrics Surgery, The University of Child Health Sciences and the Children's Hospital, Lahore, Pakistan
3Department of Pediatrics, The Fatima Memorial Hospital, Lahore, Pakistan
4Department of Pediatrics, Sir Ganga Raam Hospital, Lahore
5Department of Pediatrics Surgery, Nottingham Children Hospital, UK
6Department of Pediatrics Surgery, Akhtar Saeed Medical and Dental College, Pakistan
Received Date: 23/07/2025; Published Date: 01/09/2025
*Corresponding author: Fatima Majeed, Department of Pediatrics Surgery, King Saud Medical City, Riyadh, KSA
Abstract
Introduction: The inguinal hernia is one of the commonest defects in pediatric population. Herniotomy is performed in children traditionally. Prophylactic antibiotics are usually given for herniotomy but many groups don’t favor this approach. Because in case of clean surgeries the rate of surgical site infection (SSI) is very low and some groups think that antibiotics can be omitted in these cases.
Objective: The objective of the study is to compare the frequency of surgical site infection in children undergoing inguinal herniotomy with vs without antibiotic prophylaxis.
Study Design: Randomized controlled trial.
Material and Methods: A total number of 100 patients undergoing elective inguinal herniotomy for inguinal hernia were included. Patients were divided into two groups group A was given prophylactic antibiotics and group B did not get any antibiotics. Post-operatively patients was examined for surgical site infection(SSI) and recorded on the basis of Southampton wound scoring system.
Results: On the first day after surgery, 6 patients in group A and 5 patients in group B, had normal healing with mild bruising and erythema (grade 1). On day 7th, only 2 patients from group A had pus discharge(grade 4) , while no one from group B had such issue .
Conclusion: There was no statistically significant difference in the proportion of post-operative wound infection cases between the patients who received antibiotics prophylaxis and the patients who did not received antibiotics prophylaxis undergoing inguinal herniotomy.
Keywords: Inguinal herniotomy; Prophylactic Antibiotics
Introduction
The antibiotic overuse has resulted in development of bacterial resistance. Many studies have shown direct relationship between injudicious use of antibiotics and development and propagation of bacterial resistance [1]. Moreover, overuse and misuse of antibiotics are a source of significant burden to hospitals and patients and resistant strains compromise effectiveness of antibiotics [2].
The inguinal hernia is the commonest defect the pediatric surgeon performs surgery on. It is believed that these hernias rarely go away, and therefore, virtually all should be repaired [3]. Traditionally, prophylactic antibiotics are given for herniotomies but many groups don’t favor this approach. On the basis of contamination, surgical procedures are divided into four types; clean, clean contaminated, contaminated and dirty. The prophylactic use of antibiotics is universally accepted for clean contaminated, contaminated and dirty surgeries because of potential risk of infection. [4,11]. However, in case of clean surgeries the rate of surgical site infection (SSI) is very low and some groups think that antibiotics can be omitted in these cases [5,8,9,10,12]
Vaze D and colleagues conducted a trial in children undergoing inguinal herniotomy and they provided one group with prophylactic antibiotic while other group was not given any prophylaxis. Surgical site infection rate was almost similar in both groups; 2.2% in antibiotic group and 3.37% in without antibiotic group [6].
However, some studies have proven efficiency and cost-effectiveness of pre-operative antibiotic prophylaxis in clean surgeries like herniotomy and inguinal orchiopexy. But the meta-analyses of similar studies do not recommend or discard the use of prophylactic pre-operative antibiotics [7]. The problem is further compounded by scarcity of controlled clinical trials in the pediatric population.
The rationale of this study is that there is controversy whether pre-operative antibiotics should be given in herniotomies in pediatric patients and this study will help find out answer to this question. Moreover, misuse of antibiotics will be decreased, that will lessen cost on hospital and patients.
The objective of the study is to compare surgical site infection rate in children undergoing inguinal herniotomy with and without antibiotic prophylaxis.
Material and Method
The study is a randomized control trial, that was done in The Children Hospital and Institute of Child Health sciences, Lahore from May 2019 to October 2021. the sampling was done through lottery method. total 100 patients were included in study.
Inclusion criteria:
- All male and female patients undergoing elective inguinal herniotomy for inguinal hernia (as per operative definition).
- Patients of any age between 6 months -12 years.
Exclusion criteria:
- Patients with any generalized debilitating disease, malnourished or immunocompromised.
- Any infective focus in the body /on the skin.
- Poor quality of the skin or ongoing infection at the incision site.
- Allergy to routinely used antibiotic.
- History of use of antibiotics within past 7 days.
- Any break in anti-septic technique.
- Whose parents refuse to be part of study.
Ethical approval from institute:
The ethical approval letter ref:2021-415-CHICH, was issued from IRB (Institutional Review Board) the Institute of Child Health Sciences, The Children’s Hospital. Lahore on 09-08-2011.
Procedure and Data Collection
Approval from hospital ethical committee was obtained. After approval of the synopsis, 100 patients fulfilling the inclusion and exclusion criteria were included in the study. Patient’s parents/guardian were counseled that includes detailed explanation of the study in progress, possible postoperative complications and management of complications.
Patients were divided into two groups: Antibiotic group (group A) and no antibiotic group (group B) by lottery method. Written informed consent was taken from all patients. All procedures were done under general anesthesia. Patients in group A was given inj. Amoxicillin and clavulanic acid 30-50mg/kg intravenously as a single dosage at the time of induction of anesthesia and postoperatively they received same antibiotic for three to five days thrice daily per orally. While patients in group B did not receive any antibiotics pre and post-operatively. All the patients in both groups underwent herniotomy in a same manner. Post-operatively patients were examined for surgical site infection at 1st, 7th and 14th post-operative day and wound condition was recorded according to Southampton wound scoring system.
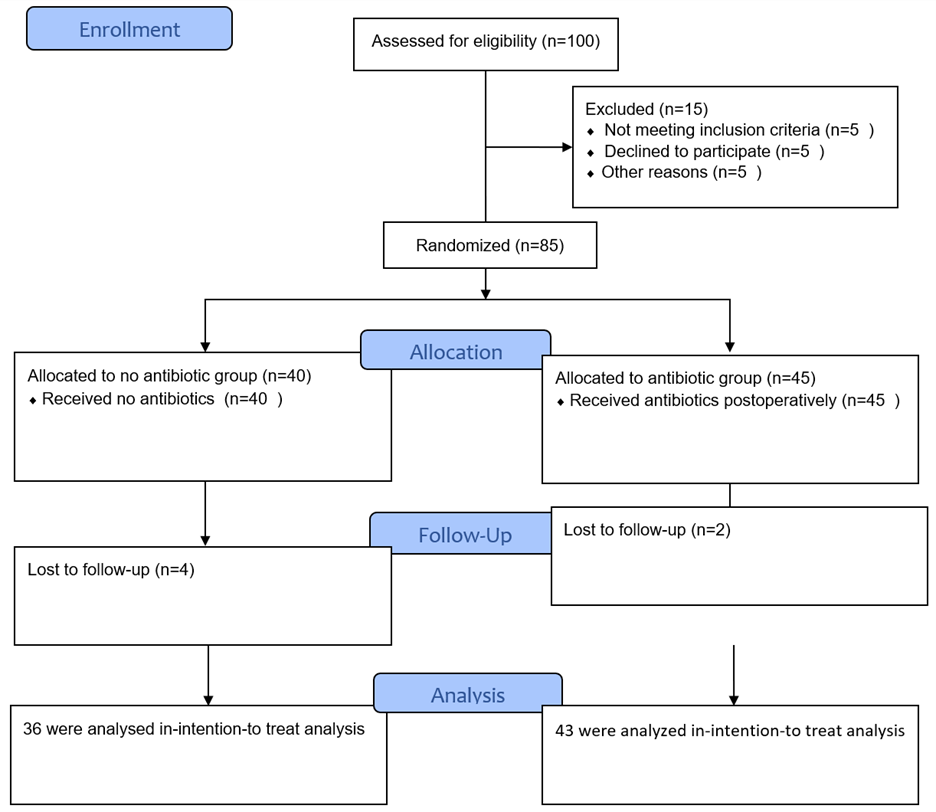
Results
The demographic details of patients in both groups were compared. Mean age of patients at time of surgery in group A was 30.6±22.68 months and in group B was 46.7±36.5 months. in group A 93.3%(n=42) were males and in group B 87.5%(n=35) were males (Table 1). In group A, there were 55.6%(n=25) patietns with right sided hernia, 35.6%(n=16) patients with left sided hernia and 8.9%(n=4) had bilateral hernia. in group B, there were 60%(n=24) with right sided hernia, 37.5%(n=15) with left sided hernia and 2.5%(n=1) had bilateral hernia (Table 2).
Table 1
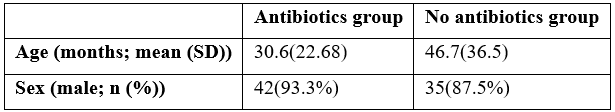
Table 2
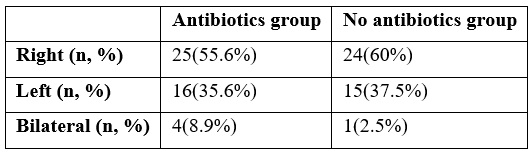
Condition of wound was recorded in both groups on day 1,7 and 14 post-operatively. On day 1, 14% (n=6) patients in group A and 13.9%(n=5) patients in group B had grade 1 of wound according to Southampton wound scoring system. rest of the patients in both groups, had normal healing (grade 0). p-value was non-significant in both groups (Table 3).
Table 3: Condition of wound on day 1.
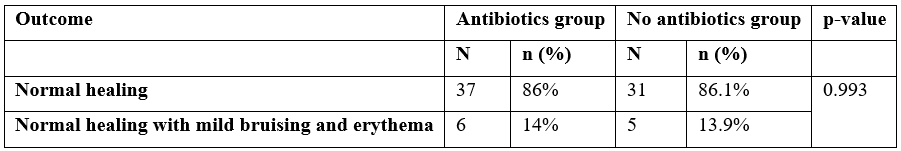
At day 7, 2.3%(n=1) patients in group A and 2.8%(n=1) patients in group B had erythema and other signs of inflammation i.e grade 2. But 4.7%(n=2) patients in group A had major complication like pus i.e., grade 4 according to Southampton wound scoring system and rest of patients in both groups had normal healing (grade 0). p-value was non-significant in bith groups (Table 4).
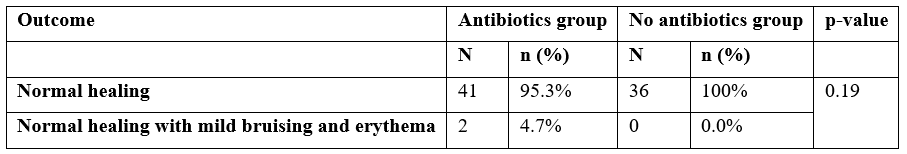
At day 14, 4.7%(n=2) patients from group A had normal healing with mild bruising or erythema (grade 1) and rest of the patients had healthy wounds (grade 0) (Table 5) p-value was non-significant.
Table 4: Condition of wound at day 7.
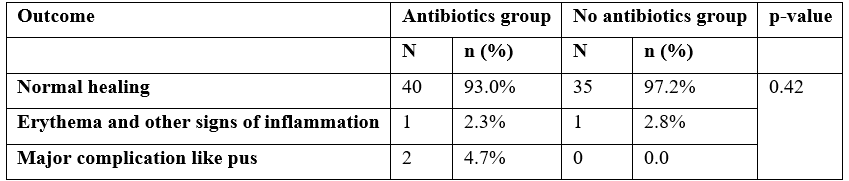
Table 5: Condition of wound at day 14.
Adverse or Harm effects: No adverse or harm effects were recorded.
Discussion
Inguinal hernia repair procedures belong to the group of the most commonly performed procedures in general surgery and are among the first procedures to be carried out by junior surgeons during their professional training. More than one million operations for hernia are performed in Europe and the United States each year [1,2].
Routine use of antibiotic prophylaxis in elective inguinal hernia repair procedures using mesh is still controversial. The rate of surgical site infection (SSI) following hernia repair procedures reported in the international literature ranges between 0% and 14% [3,4].
The European Hernia Society (EHS) does not recommend routine antibiotic prophylaxis for elective inguinal hernia repair procedures using a mesh in low-risk patients but recommends considering prophylaxis where there are patient-related risks (recurrence, old age, immunosuppression) or procedure-related risks (long duration of surgery, drainage). This applies to centres where the SSI rate for elective clean surgery is below 5% [5].
The supplement to the EHS guidelines and the comment of the Polish Working Group for Recommendations state that in the setting of Polish hospitals, the use of antibiotic prophylaxis reduces the risk of surgical wound infection in open hernia repair procedures [6].
Inappropriate antibiotic use is associated with significant risk of adverse drug reactions and emergence of bacterial resistance [7]. According to one study, 92% of surgical patients receive antibiotics, of which 79% receive antibiotics purely for prophylactic purposes [8]. In another study, up to 40% of paediatric surgical patients received antibiotics when not indicated. Use of antibiotics when not indicated was also found to be associated with a higher risk for adverse reactions [9]. In fact, of all perioperative anaphylactic reactions, of which 6% are fatal, 8% to 27.3% have been found to be cause by antibiotics [10].
The rate of surgical site infection in case group of 2.30% and that in control group of 4.60%. The rate of surgical site infections in both the groups was comparable. This observation of ours is in line with the observations of Cochrane meta-analysis, which stated that antibiotic prophylaxis (especially in clean surgeries) cannot be firmly recommended or discarded.
Usang and colleagues conducted a trial in children undergoing inguinal herniotomy and they provided one group with prophylactic antibiotic while other group was not given any prophylaxis. All wounds of patients who received prophylactic antibiotics healed without complication. But infection rate was 4.8 percent in group given no prophylactic antibiotics [6].
In a study population of 269 patients, Yerdel et al. demonstrated that the frequency of perioperative infections in the control (placebo) group was 9%. The study did not reach sufficient power (334 patients were required) and had to be terminated early due to the large number of infections in the placebo group. The rate of SSI in the antibiotic-treated group reached the value of 0.7% (1 in 136 patients). Such a considerable difference between the groups and such a high rate of infections in the control group generated discussion in the medical community [11].
In 2003, a Cochrane meta-analysis showed that antibiotic prophylaxis in inguinal hernia repair procedures could neither be unequivocally recommended nor rejected. It was concluded that the problem remained unsolved. Further studies were postulated [12].
In response to the above meta-analysis, a prospective, multicentre, double-blind, randomised, placebo-controlled trial was conducted. It was hypothesised that antibiotic prophylaxis would reduce the rate of SSI from 4% to 1% in hernia repair procedures. A total of 1008 patients were included in the study (against the initially planned sample size of 978), but no significant difference in the rate of SSI was demonstrated between the patients receiving antibiotic prophylaxis and those receiving placebo (1.6% vs. 1.8%) [13].
This study highlights that the rate of surgical site infections for clean surgeries is very low. With this observation we are hopeful that the results in our preliminary study (i.e., antibiotic prophylaxis is not warranted in clean surgeries) shall reflect in a study with a bigger sample size.
The limitations of our study include small number of patients. In future the study should be carried out with large number of patients to get better results.
Conclusion
There was no statistically significant difference in the proportion of early post-operative wound infection cases between the patients who received antibiotics prophylaxis and the patients who did not received antibiotics prophylaxis undergoing inguinal herniotomy.
Registry of trial: This study was registered in austrailian New Zealand Clinical Trial Registry with registration number ACTRN12620000400965
Universal trail number: U1111-1245-1948
References
- Lishman H, Aylin P, Alividza V, Castro-Sanchez E, Chatterjee A, Mariano V, et al. Investigating the burden of antibiotic resistance in ethnic minority groups in high-income countries: protocol for a systematic review and meta-analysis. Syst. Rev, 2017; 6(1): 251.
- S Lee, CS Park, SH Jo, SD Lee. Is Postoperative Prophylactic Antibiotics Necessary for Pediatric Scrotal and Inguinal Outpatient Surgeries? Korean J Urogenit Tract Infect Inflamm, 2014; 9: 111-114.
- Ein SH, Njere I, Ein A. Six thousand three hundred sixty-one pediatric inguinal hernias: a 35-year review. J. Pediatr. Surg, 2006; 41(5): 980-986.
- Merkow RP, Ju MH, Chung JW, Hall BL, Cohen ME, Williams MV, et al. Underlying reasons associated with hospital readmission following surgery in the United States. JAMA, 2015; 313: 483-495.
- Hasan GZ, Saleh FM, Hossain MZ, Amin MR, Siddiqui TH, Islam MD, Chakraborty S. Antibiotic prophylaxis is unnecessary in clean surgery. MMJ, 2013; 22(2): 342-344.
- Vaze D, Samujh R, Narasimha Rao KL. Risk of surgical site infection in paediatric herniotomies without any prophylactic antibiotics: A preliminary experience. Afr J Paediatr Surg, 2014; 11: 158-161.
- Sanchez-Manuel FJ, Lozano-García J, Seco-Gil JL. Antibiotic prophylaxis for hernia Cochrane Database Syst Rev, 2012; 2: CD003769.
- Rensing AJ, Whittam BM, Chan KH, Cain MP, Carroll AE, Bennett Jr WE. Is surgical antibiotic prophylaxis necessary for pediatric orchiopexy? J Pediatr Urol, 2018; 14(3): 261-e1.
- Kremer KM, Foster RT, Drobnis EZ, Hyde KJ, Brennaman LM. Non-indicated use of prophylactic antibiotics in gynaecological surgery at an academic tertiary medical centre. Am J Obstet Gynecol MFM, 2018; 38(4): 543-547.
- Lee KB, Kim SY, Kim SM, Chang HJ, Kim BW, Lee Y, et al. Perioperative Antibiotic Prophylaxis May Not Be Required Routinely in Thyroid Surgery. J Endocr Surg, 2017; 17(4): 160-167.
- Shivakumar CR, Shoeb MF, Pinate AR. Study of efficacy of short course peri-operative antibiotics in clean contaminated surgeries. Int Surg J, 2017; 4(8): 2455-2459.
- Kekre G, Dikshit V, Kothari P, Mudkhedkar K, Gupta A, Patil P. Incidence of wound infection in common paediatric day care surgeries following a no-antibiotic protocol: a viable recommendation for a public hospital in India. Int Surg J, 2018; 5(5): 1729-1732.

