Perioperative Antibiotics Impact for Post Distal Hypospadias Surgical Repair with Stent Placement, A Retrospective Comparison Study
Abdelbasit Elsyed ali A Hamid, Osama Ibrahim A Alquaymi* and Izzat Malkani
Department of Pediateric Surgery, King Suad Medical City, Riyadh, Saudia Arabia
Received Date: 22/07/2025; Published Date: 29/08/2025
*Corresponding author: Osama Ibrahim A Alquaymi, Department of Pediateric Surgery, King Suad Medical City, Riyadh, Saudia Arabia
Abstract
Objective: Hypospadias is a common congenital defect that presents in the early life of male patients. The use of perioperative antibiotics has been controversial among physicians, with no adequate evidence regarding its benefits or effect in minimizing the risk of developing postoperative infections. We aim to both evaluate the risk of developing a urinary tract infection (UTI) or surgical site infection (SSI) postoperatively with or without receiving perioperative antibiotics and assess the incidence.
Methods: We adopted a retrospective study design and collected data from the file records of male patients (1–12 years) admitted between 2020 and 2022 to King Saud Medical City who underwent hypospadias repair. We excluded those who underwent redo repair, had proximal hypospadias or an associated anomaly (e.g., a disorder of sex development), had chordee, or presented with a preexisting UTI or immune deficiency. Statistical analyses were performed using SPSS version 21. Inferential statistical methods included univariate analysis using chi-square tests to determine the association of UTIs/SSIs and a positive culture with pre- and postoperative antibiotic use. Additionally, the Kruskal– Wallis test was used to assess the relationship between patient age and postoperative UTIs/SSIs.
Prevalence rates were calculated as percentages with 95% confidence intervals. A P-value < 0.05 was considered statistically significant.
Results: Most of the included sample belonged to the 1- to 2-year-old group (n = 21, 53.8%), with the least frequency found for infants (4, 10.3%). There was no preoperative culture, and most patients received preoperative antibiotics (35, 89.7%). Postoperative antibiotics were administered to 38 (97.4%) patients. We subdivided participants into two groups, Group A comprised 18 patients who received either a single preoperative antibiotic dose or antibiotics for up to 24 hours post surgery. Group B consisted of 21 patients: 17 received preoperative antibiotics plus extended antibiotics, and 4 patients initially did not receive preoperative antibiotics but were given extended therapy, Postoperatively, only two patients of group B (5.1%) had a febrile illness, and one (2.6%) had a positive culture.
Conclusion: In the surgical management of distal hypospadias, we found no advantage of extended use of antibiotics over prophylaxis. To better understand the incidence of infection and compare prophylactic and extended antibiotic use following distal hypospadias repair, our findings indicate the need for more prospective research.
Keywords: Distal hypospadias; Infections; Urinary tract infection; Surgical site infections
Introduction
Hypospadias is one of the most prevalent congenital defects in male children. Several procedures are currently performed to treat hypospadias (e.g., tubularized incised plate urethroplasty) [1].
Prophylactic antibiotics are used for patients undergoing surgery to avoid infection, although this practice is being investigated due to rising rates of antibiotic resistance [2].
There is conflicting information in the current literature about the use of antibiotics during several pediatric surgeries, including hypospadias [3]. One study provided evidence in favor of prophylaxis, reporting that children who did not receive postoperative antibiotic prophylaxis had higher levels of bacteriuria and clinical urinary tract infections (UTIs). On the other hand, another study indicated no differences in surgical complications or symptomatic UTIs between two retrospective cohorts of patients, one receiving antibiotic prophylaxis and the other not [4]. We aimed to evaluate the incidence of UTIs and surgical site infections (SSIs) after a distal hypospadias repair procedure for patients who did and did not receive antibiotics perioperatively and postoperatively.
Methods
Our study design is a retrospective cohort of patients admitted to King Saud Medical City, Riyadh from 2020 to December 2022 who underwent distal hypospadias repair with stent placement. The study included all boys aged 1–12 years who had isolated distal hypospadias and were otherwise well and not on antibiotics for other reasons. Patients who underwent redo repair, had proximal hypospadias or an associated anomaly (e.g., a disorder of sex development), had chordee, or presented with a preexisting UTI or immune deficiency were excluded. We defined a UTI as an infection that might present anywhere along the urinary system. The presence of >10 white blood cells/mm3 and 50,000 CFU/mL of a single pathogen in a urine sample was considered diagnostic.
We divided our cohort into two groups based on their antibiotic exposure to determine any resulting impact on postoperative infection rates. Group A represented patients who received a single preoperative antibiotic dose and those who received antibiotics for up to 24 hours. Group B comprised patients who received preoperative antibiotics plus extended antibiotics until the catheter was removed (3–7 days) and those who did not receive a preoperative dose but received extended antibiotics. Statistical analyses were performed using SPSS version 21. For descriptive statistics, categorical variables were summarized as frequencies and percentages. Inferential statistical methods included univariate analysis using chi-square tests to determine the association of UTIs/SSIs and a positive culture with pre- and postoperative antibiotic use. Additionally, the Kruskal–Wallis test was used to assess the relationship between age and postoperative UTIs/SSIs. Prevalence rates were calculated as percentages with 95% confidence intervals. A P-value < 0.05 was considered statistically significant.
Results
Descriptive data
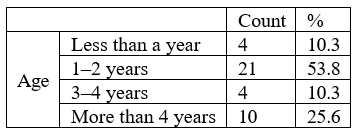
An evaluation of the demographic features of the study sample revealed that most of the patients were 1–2 years old (n = 21, 53.8%), followed by those who were more than 4 years old. Patients aged 3– 4 years (4, 10.3%) and less than a year old (4, 10.3%) had the least frequency (Table 1).
Table 1: Descriptive statistics of the included sample.
Regarding preoperative antibiotic administration, no patient had a preoperative culture taken, but most received preoperative antibiotics (35, 89.7%), of which they were no UTI or SSI cases. Similarly, postoperative antibiotics were administered to 38 (97.4%) cases. Postoperatively, two patients (5.1%) out of the total sample (39) had a febrile illness. Their cultures were taken, and one (2.6%) had a positive result. No patient had an SSI. In terms of antibiotic timing, most participants (21, 53.8%) took postoperative antibiotics until urinary catheter removal, while 17 (43.6%) patients received preoperative and postoperative antibiotics up to 24 hours.
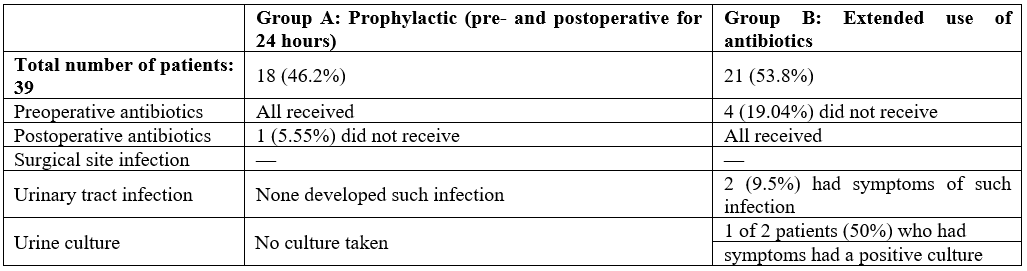
Group A comprised 18 patients who received either a single preoperative antibiotic dose or antibiotics for up to 24 hours postsurgery, with just one patient in the former category. Group B consisted of 21 patients: 17 received preoperative antibiotics plus extended antibiotics, and 4 initially did not receive preoperative antibiotics but were given extended therapy (Table 2).
Table 2: Comparison of Groups A and B.
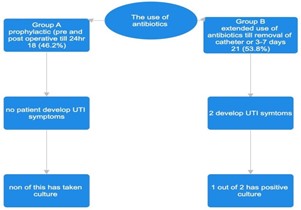
Flow chart 1: comparison groups.
Analysis of postoperative UTI and SSI according to antibiotic timing
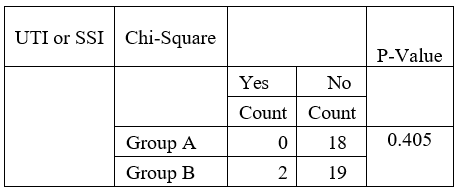
Of the patients treated with pre- and postoperative antibiotics within 24 hours, there were no observed complications. Furthermore, no infections were recorded for the patient who received only a preoperative dose. Of the 21 patients who received antibiotics postoperatively until urinary catheter removal, two developed infections. Nevertheless, this difference was statistically insignificant, as represented by the chi-square P-value of 0.405. These findings, therefore, indicate that timing is not particularly important in altering the rate of postoperative infection possibilities (Table 3).
Table 3: Analysis of urinary tract and surgical site infections in patients according to antibiotic timing.
Analysis of postoperative UTI and SSI according to patient age
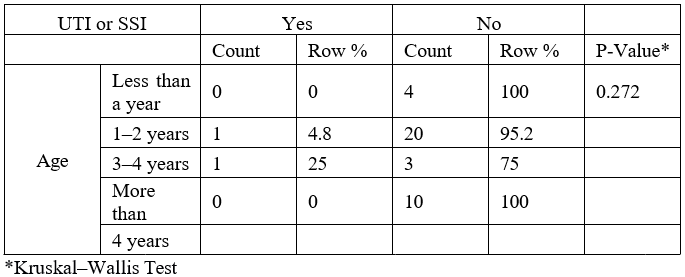
Our analysis of the association between age and incidence of UTIs and SSIs, using the Kruskal– Wallis test, did not indicate a significant difference across the age groups of the study. Of the 39 patients, none of the infants developed infections. Correspondingly, the infection rate increased slightly—4.8% (1 of 21) in the 1- to 2-year-old group and 25% (1 of 4) in the 3- to 4-year-old group—while no child older than 4 years developed an infection. For the Kruskal–Wallis test, the P-value was 0.272, confirming that there is no significant relationship between age and the development of postoperative infections. These findings thus suggest that age is not a vital factor in the development of UTIs or SSIs among these patients (Table 4).
Table 4: Analysis of postoperative urinary tract and surgical site infections according to patient age.
Discussion
In recent years, the medical community has faced an escalating crisis: the growing resistance to antibiotics. It is imperative that every possible effort be made to promote adequate and reasonable use of antimicrobial therapy. One specific strategy to promote responsible antibiotic use is the implementation of single-dose perioperative antibiotic prophylaxis, an approach currently recommended for all patients undergoing open urological surgery [6]. The rationale behind this recommendation is to minimize the risk of postoperative infections while reducing overall antibiotic use.
Periprocedural prophylaxis refers to the administration of antibiotics immediately before, during, or after a surgical procedure to prevent infection. In the context of urological surgery, the goal is to protect the patient from potential infections that could be introduced during the operation. Traditionally, various antibiotic regimens have been employed to mitigate infection risks following hypospadias repair, yet the necessity and duration of antibiotic prophylaxis remain widely debated.
Due to a lack of specific guidelines, most surgeons recommend prolonged antibiotic prophylaxis during hospital stays and recovery at home for patients undergoing urethral reconstruction [7]. This is because infections are common complications in these surgeries, and the aim is to use extended antibiotics to reduce them.
The administration of postoperative antibiotic prophylaxis following pediatric hypospadias repair has been the subject of extensive research and debate. This study aimed to assess the role of antibiotics in distal hypospadias repair, addressing the controversy surrounding the necessity for extended antibiotic regimens. Our retrospective study included 41 candidates for distal hypospadias repair over three years— with two exclusions due to incomplete data, resulting in a final sample of 39 patients. Group A comprised 18 patients who received either a single preoperative antibiotic dose or antibiotics for up to 24 hours postsurgery. Out of 18 patients, one received only a preoperative stat dose. Group B consisted of 21 patients, of which 17 received preoperative antibiotics plus extended antibiotics and 4 patients initially did not receive preoperative antibiotics but were given extended therapy. Within Group B, two patients experienced febrile illness accompanied by dysuria. Subsequent urine cultures identified one case of Proteus mirabilis infection, while the other showed no bacterial growth. Conversely, Group A demonstrated no clinical indicators of UTIs or SSIs.
Although the number of patients in this study is limited, there was no major difference between the two groups in terms of developing UTIs or SSIs. Patients who were not exposed to extended antibiotic use did not develop any such infections. This highlights the key findings of this study and implies that extended antibiotic use may not be necessary to prevent infections in distal hypospadias repair.
Recent studies have suggested that such prophylaxis may not provide additional benefits in reducing postoperative complications. A randomized, double-blind, placebo-controlled trial evaluated the effect of postoperative prophylactic antibiotics on infection rates and urethroplasty complications after stented midshaft-to-distal hypospadias repair. The study found no significant difference in the incidence of symptomatic UTIs, SSIs, or urethroplasty complications between the antibiotic and placebo groups.
Specifically, 22% of boys receiving antibiotics experienced complications compared to 10% in the placebo group, a difference that was not statistically significant (P = 0.16) [5].
Similarly, a retrospective cohort study investigated whether perioperative parenteral antibiotic prophylaxis reduces infectious complications in stented distal hypospadias repair. The results indicated no significant difference in infection rates between those who received antibiotics and those who did not.
Notably, all subjects who developed infectious complications received postoperative oral antibiotic prophylaxis, and there was an instance of Clostridioides difficile infection in a patient who received perioperative antibiotics [8].
A systematic review and meta-analysis assessed the utility of postoperative prophylactic antibiotics in preventing complications after stented distal hypospadias repair. The analysis, which included seven studies with 986 cases, found no significant difference in overall postoperative complications between those who received antibiotics and those who did not. However, asymptomatic bacteriuria was more prevalent in the nonantibiotic group [2]. Another prospective randomized study compared postoperative antibiotic prophylaxis using trimethoprim-sulfamethoxazole to no treatment after mid-to-distal hypospadias repair. While the antibiotic group showed reduced bacteriuria and inflammation markers, there was no significant difference in clinical UTIs or surgical complications between the groups. Additionally, higher trimethoprim-sulfamethoxazole resistance was observed in the antibiotic group [4]. Collectively, these studies indicate that routine postoperative antibiotic prophylaxis may not significantly reduce the risk of infections or other complications following pediatric hypospadias repair.
Our study also underscores that extended antibiotic therapy does not conclusively enhance infection control in distal hypospadias repair compared to prophylactic regimens. Further large-scale studies could fortify these findings and assist in evolving surgical and postoperative care
practices. Studies focusing on stratifying patients based on risk factors, such as preexisting conditions and surgical complexity, could provide more tailored recommendations. By refining the current approach to antibiotic use, physicians can enhance patient care quality, reduce the risk of antibiotic resistance, and hence, contribute to sustainable healthcare practices.
Conclusion
We found no advantage of extended use of antibiotics over prophylactic use in the perioperative treatment of distal hypospadias. Our study revealed the need for further prospective studies to clarify the incidence of infection in post-hypospadias repair and elaborate the comparison between prophylactic and extended antibiotic use post-distal hypospadias repair.
Funding: No funding was obtained from a second or third party.
Ethical Considerations: This is a retrospective record-based study that does not reveal patients’ identities. Data and information were obtained from medical records, with no need for patients’ consent.
References
- Almusafer M, Abduljabbar OH, Buchholz Stented versus non-stented snodgrass urethroplasty for distal hypospadia repair. Urol Int, 2020; 104(1–2): 156–159.
- Chua ME, Kim JK, Rivera KC, Ming JM, Flores F, Farhat WA. The use of postoperative prophylactic antibiotics in stented distal hypospadias repair: A systematic review and meta- analysis. J Pediatr Urol, 2019; 15(2): 138–148.
- Canon SJ, Smith JC, Sullivan E, Patel A, Zamilpa I. Comparative analysis of perioperative prophylactic antibiotics in prevention of surgical site infections in stented, distal hypospadias repair. J Pediatr Urol, 2021; 17(2): 256.e1–256.e5. doi:10.1016/j.jpurol.2020.11.033.
- Roth EB, Kryger JV, Durkee CT, Lingongo MA, Swedler RM, Groth Antibiotic prophylaxis with trimethoprim-sulfamethoxazole versus no treatment after mid-to-distal hypospadias repair: A prospective, randomized study. Adv Urol, 2018; 2018: 7031906. doi:10.1155/2018/7031906.
- Faasse MA, Farhat WA, Rosoklija I, Shannon R, Odeh RI, Yoshiba GM, et Randomized trial of prophylactic antibiotics vs. placebo after midshaft-to-distal hypospadias repair: The PROPHY Study. J Pediatr Urol, 2022; 18(2): 171–177.
- Lightner DJ, Wymer K, Sanchez J, Kavoussi Best practice statement on urologic procedures and antimicrobial prophylaxis. J Urol, 2020; 203: 351–356.
- McDonald ML, Buckley Antimicrobial practice patterns for urethroplasty: Opportunity for improved stewardship. Urology, 2016; 94: 237–245.
- Doersch KM, Logvinenko T, Nelson CP, Yetistirici O, Venna AM, Masoom SN, et al. Is parenteral antibiotic prophylaxis associated with fewer infectious complications in stented, distal hypospadias repair? J Pediatr Urol, 2022; 18(6): 759–763. doi:10.1016/j.jpurol.2022.05.003.

