Patient Satisfaction and Quality of Life Correlation in VMAT Radiation Therapy: a first approach for Head and Neck Cancer under the scope of psycho-oncology
Panagiota Kiafi1,*, Maria Anthi Kouri1,2, Georgios Patatoukas1, Marina Chalkia1, Andromachi Kougioumtzopoulou1, Ourania Nicolatou-Galitis3, Efthimios Kyrodimos4, Vassilis Kouloulias1 and Kalliopi Platoni1,*
12nd Department of Radiology, Medical School, Attikon University Hospital, National and Kapodistrian University of Athens, 11527 Athens, Greece
2 Medical Physics, General Hospital GHA Korgialeneio Mpenakeio-Hellenic Red Cross, Athanasaki 11, 11526 Athens, Greece
3Oral Oncology Unit, Clinic of Hospital Dentistry, Dental School, University of Athens, Bouboulinas 41, N. Psyhico, 154 51, Athens, Greece
42nd Department of Otolaryngology-Head and Neck Surgery, Hippokration General Hospital, University of Athens, Athens, Greece
Received Date: 20/01/2025; Published Date: 07/03/2025
*Corresponding author: Panagiota Kiafi and Kalliopi Platoni, 2nd Department of Radiology, Medical School, Attikon University Hospital, National and Kapodistrian
Abstract
Background: This study explores the complex relationships between patient satisfaction, psychological well-being, and symptom reporting among head and neck cancer patients undergoing Volumetric Modulated Arc Therapy (VMAT) radiation treatment.
Aim of the Study: Building on our previous research that examined correlations between QoL, dosimetric toxicities, and symptoms, this study delves further into the psychological factors influencing symptom reporting. Patient satisfaction, a key metric in modern oncology, was evaluated through a custom-designed survey that assessed interactions with medical, nursing, and radiology staff, communication quality, and the doctor-patient relationship. Psychological well-being was assessed using the emotional functioning category of the EORTC QLQ-C30 questionnaire, capturing levels of anxiety, depression, and emotional distress at three key stages: before treatment, immediately post-treatment, and three months post-treatment.
Materials and Methods: Our analysis employed descriptive statistics, exploratory factor analysis, and repeated measures MANOVA to examine changes in QoL and patient satisfaction over time, alongside correlational analysis to explore relationships between satisfaction scores and emotional well-being. The results revealed consistently high levels of satisfaction with healthcare services, highlighting the critical role of effective communication and emotional support in fostering trust and confidence in treatment. However, the study also identified potential biases in patient-reported outcomes, particularly regarding emotional distress and psychological well-being, suggesting that QoL and patient satisfaction questionnaires alone may not provide a fully accurate reflection of patient experiences.
Results: The findings underscore the limitations of relying solely on self-reported questionnaires for clinical assessments and highlight the need for a more comprehensive approach. By integrating psycho-oncological principles into cancer care, this study emphasizes the importance of a multidimensional approach to patient assessment, capturing not only clinical outcomes but also the psychological and emotional aspects of patient well-being. This holistic perspective ensures a more comprehensive understanding of how patients experience and respond to treatment, ultimately leading to more effective and personalized care strategies.
Conclusion: Ultimately, this research reinforces the critical need for integrating psychological care and emotional support into routine oncology practice. By acknowledging the intricate interplay between psychological factors and treatment outcomes, this study aspires to set a new standard in cancer care that not only enhances patients' quality of life but also significantly improves their overall treatment efficacy and satisfaction.
Keywords: Patient Satisfaction; Quality of Life; Head and Neck cancer; Radiation Therapy, Volumetric Modulated Arc Therapy (VMAT); Psycho-oncology
Introduction
Patient satisfaction and quality of life (QoL) have become increasingly important metrics in evaluating the impact of modern cancer treatments, particularly in complex modalities such as those used in Radiation Therapy [1,2]. These metrics offer insights not only into the clinical effectiveness of treatment but also into the holistic well-being of patients, encompassing their physical, emotional, and social functioning. However, traditional assessments of patient satisfaction and QoL may not fully capture the psychological complexities experienced by patients undergoing intensive therapies [3]. This remark has prompted a shift towards integrating psycho-oncology into clinical practice, which emphasizes the psychological and emotional dimensions of cancer care [4,5]. Understanding the correlation between patient satisfaction, QoL, and psychological support is essential to enhancing patient-centered care, aiming to improve not only survival outcomes but also the overall patient experience throughout their cancer journey [6].
Head and neck cancers, in particular, present unique challenges due to their impact on essential functions such as speech, swallowing, and facial appearance [7]. The physical and functional impairments resulting from these cancers and their treatments often lead to significant emotional distress, including anxiety, depression, and diminished self-esteem [8,9]. Psycho-oncology offers targeted psychological support to address these issues, thereby enhancing patients' quality of life [10]. Interventions such as cognitive-behavioral therapy and emotional counseling help patients cope with the psychological effects of their illness and treatment, improving their overall well-being and adjustment to physical changes [11,12].
The field of psycho-oncology has thus emerged as a critical component of comprehensive cancer care, especially for patients with head and neck cancers [13,14]. This interdisciplinary approach addresses the psychological and emotional challenges associated with cancer diagnosis, treatment, and survivorship [15]. Integrating psycho-oncology into clinical practice can significantly improve patient quality of life and satisfaction, underscoring its value in modern oncology [16].
In a previous study, we investigated the relationship between QoL, dosimetric toxicities, and symptoms in head and neck cancer patients [17]. Our findings revealed varying degrees of correlation between dosimetric data at organs at risk (OARs) and patient-reported symptoms, highlighting the potential limitations of using QoL questionnaires alone as indicators of treatment efficacy. While the study indicated that patients were generally compliant in reporting their symptoms and QoL, it also raised concerns about the biases inherent in self-reported questionnaires. Patients may underestimate their symptoms or present their condition more favorably, either to appear polite to healthcare professionals or to convince themselves that they are experiencing fewer or less severe symptoms than they actually are [18,19]. This phenomenon raises questions about the reliability of relying solely on patient-reported outcomes (PROs) for clinical assessments. The tendency to refine or underreport symptoms can be influenced by factors such as a desire to please medical staff, fear of disappointing caregivers, or psychological coping mechanisms that minimize discomfort [20,21]. These biases underscore the need for a more comprehensive approach to symptom assessment that integrates objective measures with patient-reported data,
providing a more accurate picture of treatment efficacy and patient well-being [22].
Aims
Building on our previous research, this work aims into investigating the relationship among patient satisfaction and the accuracy of symptom reporting. Unlike existing studies that often focus solely on clinical outcomes or QoL metrics, our research takes a more integrated approach by examining how patient satisfaction, psychological well-being, and symptom reporting interact. A comprehensive survey was conducted to explore the nuances of patient satisfaction and its correlation with the perceived severity of symptoms and overall QoL. The survey delved deeper into patients' subjective experiences and how these experiences might influence their reporting behavior. By incorporating questions related to their satisfaction with various aspects of care—including communication with healthcare providers, the clarity of information received, and their overall treatment experience—as well as assessing their psychological status using the emotional functioning category (questions 21-24) of the QLQ-C30 questionnaire, we sought to identify any patterns or discrepancies that could shed light on the reliability of QoL questionnaires.
This study focuses on the combination of patient satisfaction, psychological well-being, and symptom reporting within the framework of psycho-oncology. By incorporating psycho-oncological principles into our analysis, we aim to study the psychological factors that may affect patients' perceptions and influence their reporting of symptoms. This comprehensive approach seeks to enhance the accuracy of QoL assessments while providing new insights into the psychological and emotional determinants that affect patient-reported outcomes in head and neck cancer treatment.
Materials and Methods
Study Design
This complementary study aimed to evaluate patient satisfaction among 75 patients undergoing VMAT radiation treatment for head and neck cancer and to correlate these findings with the QoL outcomes from our previously published research. The study was conducted at Attikon General University Hospital in Athens, Greece, following the ethical standards outlined in the Declaration of Helsinki. Approval was obtained from the Bioethics and Ethics Committee of the Scientific Council of the Attikon General University Hospital. All participants provided informed consent before inclusion in the study.
Participants
Eligible participants were patients diagnosed with head and neck cancer scheduled for VMAT radiation therapy. A total of 82 patients were initially recruited. After applying exclusion criteria—including changes in prescribed therapy, patient withdrawal, and mortality during treatment—the final sample comprised of 75 patients. All participants were informed about the study’s purpose, and written consent was obtained. Inclusion criteria ensured a representative sample of the total head and neck cancer patient population undergoing VMAT.
Patient Satisfaction Survey
To assess patient satisfaction with VMAT radiation therapy, a custom developed survey was conducted. It included questions in four main categories:
- Demographics and Lifestyle: Collected data such as gender, age, diagnosis, smoking and alcohol consumption habits, and comorbidities.
- Satisfaction with Medical Services: Assessed interactions with doctors, nurses, and radiation technicians, focusing on politeness, respect, clarity of information, treatment instructions, lifestyle modifications, and time spent during consultations.
- Satisfaction with Healthcare Staff: Evaluated professionalism, communication, and supportiveness from medical personnel throughout the treatment.
- Doctor-Patient Relationship: Measured trust, overall satisfaction with medical visits, comfort level, empathy, understanding, and willingness to continue with medical care.
The survey questionnaire was designed to promote unbiased responses, with patients completing it anonymously and without any external guidance. Completed questionnaires were deposited in a secure box at the hospital's reception to maintain confidentiality.
Integration of Psycho-Oncology
To enhance the study's depth, an additional layer of psycho-oncological assessment was integrated. We assessed the psychological status of patients using the emotional functioning category (questions 21-24) of the EORTC QLQ-C30 questionnaire, which evaluates anxiety, depression, and overall emotional well-being. This component aimed to identify any patterns or discrepancies that could illuminate the psychological factors affecting patient satisfaction and QoL reports. Psychological assessments were conducted at three key time points: before VMAT treatment, immediately post-treatment, and three months after treatment. This allowed us to capture both immediate and longer-term emotional responses, providing insights into the reliability of QoL questionnaires in reflecting true patient experiences.
Data Collection and Statistical Analysis
QoL data were collected at three time points: before VMAT treatment, immediately after the end of treatment, and three months post-treatment, while patient satisfaction data were collected three months post-treatment to ensure that patients had a comprehensive perspective on their treatment experience.
Statistical analysis was performed using SPSS version 26.0 (IBM Corporation, Somers, NY, USA). Descriptive statistics summarized quantitative data, including the number of participants (N), mean values, and standard deviations. Categorical variables were presented as frequencies (N) and percentages (%). Normality was assessed using the Kolmogorov-Smirnov test and normal probability plots. Reliability of the satisfaction survey was evaluated with Cronbach's alpha, while Exploratory Factor Analysis (EFA) using maximum likelihood extraction and Varimax rotation identified underlying factors within the satisfaction survey, with factors selected based on eigenvalues greater than 1 and factor loadings exceeding 0.4.
To assess changes in QoL, a one-way repeated measures MANOVA was conducted to examine differences over time (baseline, end of treatment, and 3 months post-treatment). Assumptions for MANOVA, such as correlations among dependent variables, normality, and homogeneity of variances, were verified. Pearson's or Spearman's correlation coefficients were used to explore relationships between patient satisfaction scores and QoL outcomes from the EORTC questionnaires. A p-value of <0.05 was considered statistically significant.
Results
Patient Demographics and Clinical Characteristics
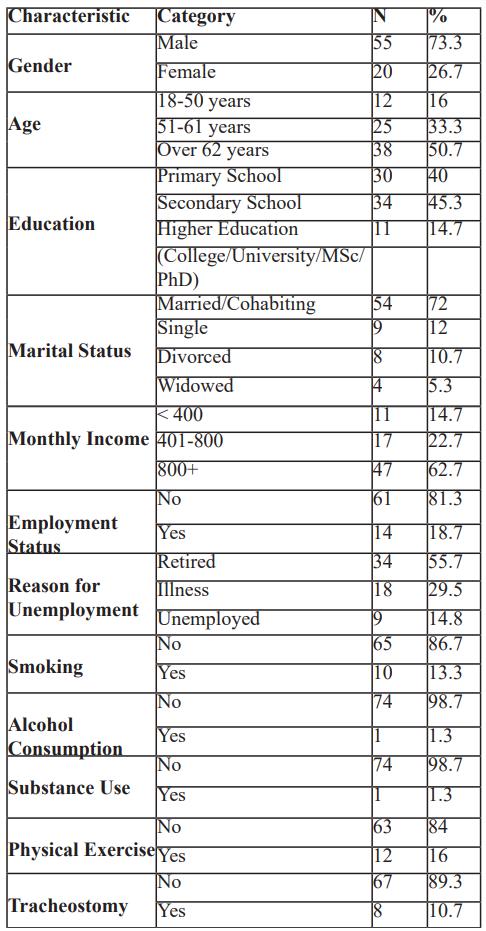
Table 1 provides an analysis of the demographic characteristics of the patient sample, showing percentages and values for each category.
Table 1: Demographic data of the selected sample.
Patient Satisfaction
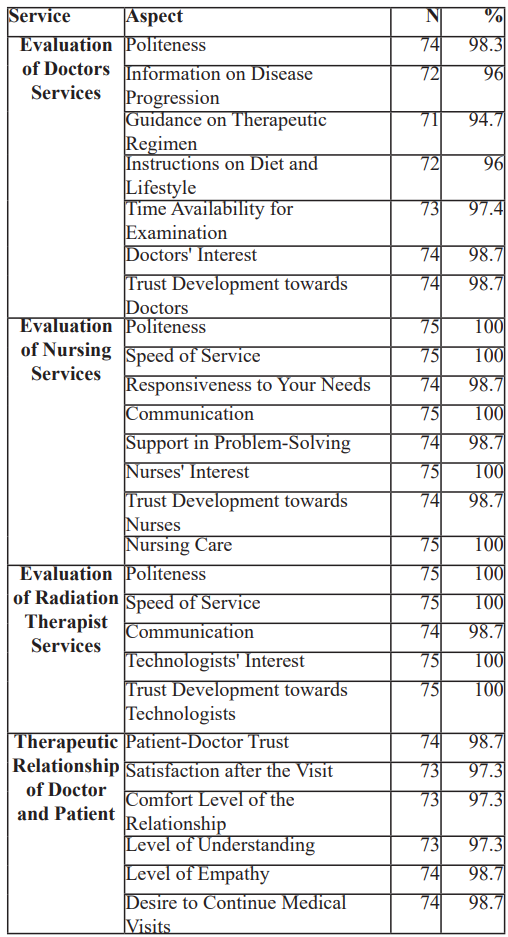
Table 2 provides a comprehensive evaluation of different aspects of medical, nursing, and radiation therapist services, as well as the therapeutic relationship between doctor and patient, showing both the percentages and the values for each assessed category.
Table 2: Assesement of the patient satisfaction on the medical services.
Psycho-Oncology Analysis: Emotional Functioning
The analysis of the emotional functioning (questions 21-24 of the EORTC QLQ-C30) provided insight into patients' psychological status at three distinct time points as can be depicted in Figure 1.
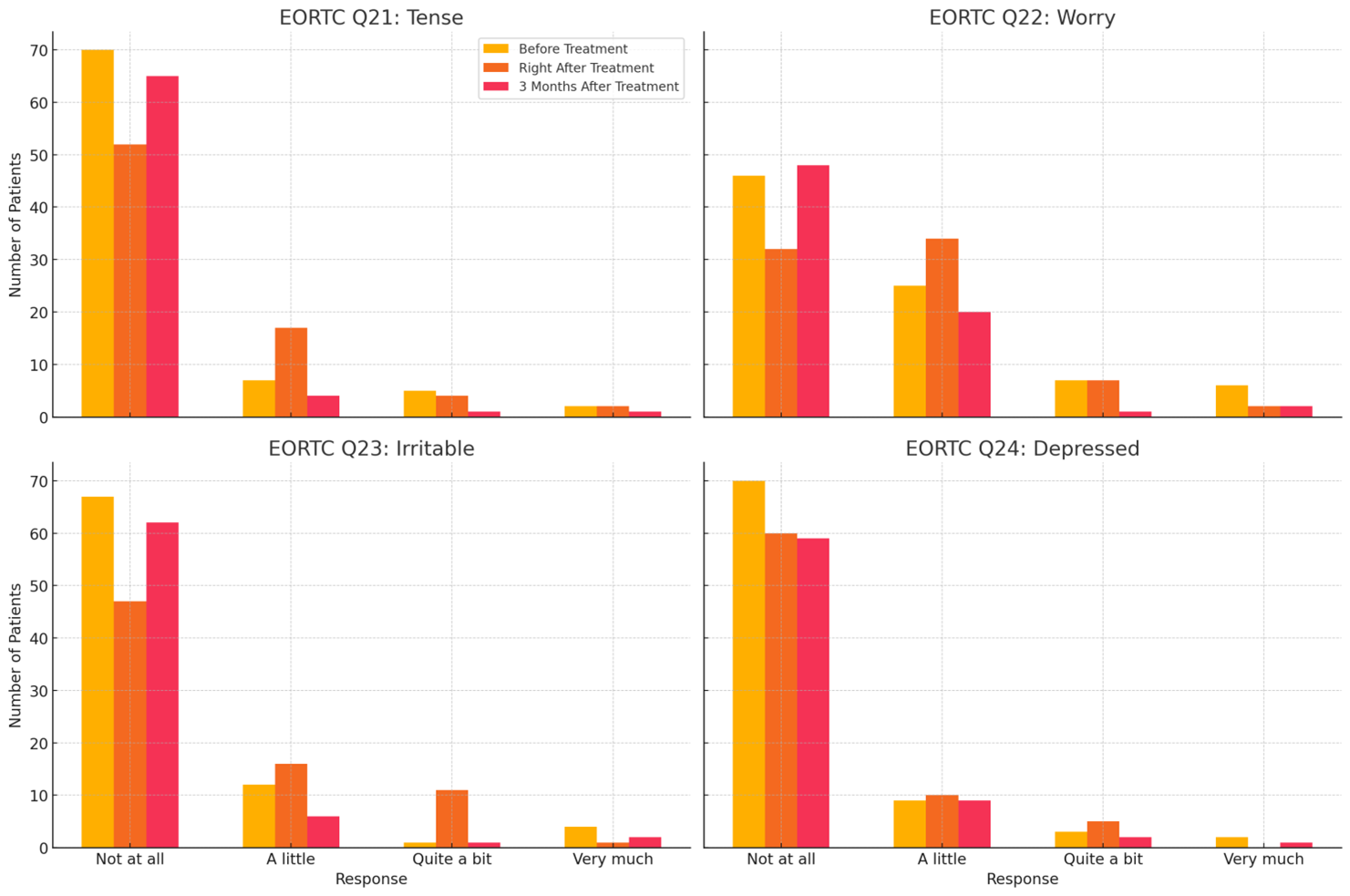
Figure 1: Illustration of the EORTC questions 21-24 (Tense, Worry, Irritable, and Depressed) across the three time points: before treatment, at the end of treatment, and three months after the end of treatment. Each subplot represents one of the emotional responses, allowing for a clear comparison of how patient-reported emotional distress levels change over time.
Correlation Between Emotional Functioning and Patient Satisfaction
To explore the relationship between psychological status and patient satisfaction with services, Spearman's correlation analysis was performed. Preliminary results suggest that patient-reported emotional distress was inversely correlated with their satisfaction in specific service categories, particularly for nursing and radiation technologist services.
Patients who reported higher levels of tension or worry (EORTC21 and EORTC22) during or after treatment were more likely to report lower satisfaction with certain aspects of care (Spearman's r = -0.246, p = 0.033 for "appetite loss" and doctor-patient relationship).
Emotional distress related to feeling depressed or irritable (EORTC23 and EORTC24) correlated less strongly with service evaluation but showed trends consistent with dissatisfaction in areas related to personal communication with healthcare providers.
Correlation of QoL and Patient Satisfaction
Spearman’s rank correlation coefficient (Spearman's r) was used to assess the strength and direction of the association between ranked variables, specifically between the various health sections from the EORTC QLQ-C30 and EORTC QLQ-H&N35 questionnaires and patient satisfaction with medical, nursing, and technologist services, as well as the doctor-patient relationship. The p-value represents the probability of observing the given correlation by chance. A p-value of less than 0.05 was considered statistically significant. Table 4 presents the correlations between different functional and symptomatic QoL domains (e.g., physical functioning, pain, swallowing, etc.) and the evaluation of these service aspects as can be also depicted in Figure 2.
Table 3: Correlation of EORTC QLQ-C30 and EORTC QLQ-H&N35 with Service Evaluation Questionnaire.
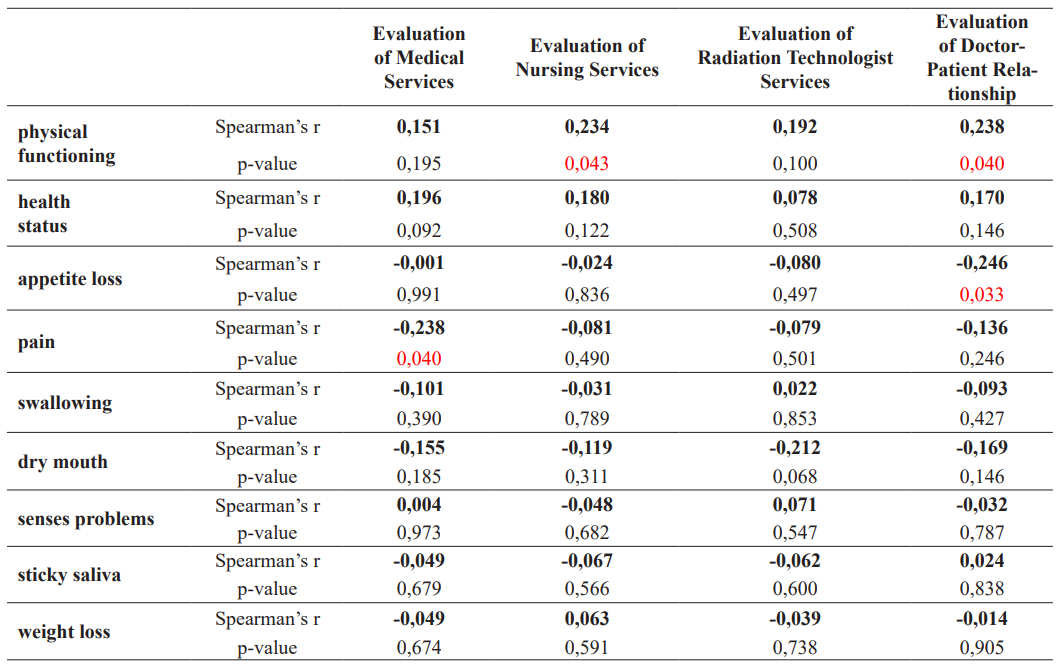
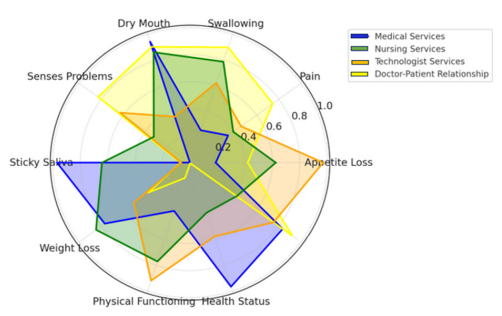
Figure 2: Radar chart depicting the correlations between the EORTC QLQ-C30 and EORTC QLQ-H&N35 domains with the Service Evaluation Questionnaire. Each axis represents one of the domains (e.g., physical functioning, health status), and the colored lines correspond to the different service evaluations: Medical Services, Nursing Services, Radiation Technologist Services, and Doctor-Patient Relationship.
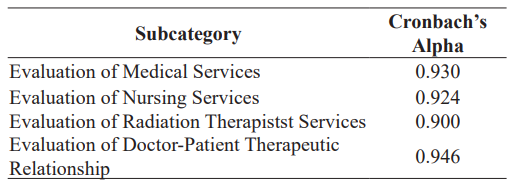
Cronbach’s Alpha was used to assess the internal consistency and reliability of the survey subjects within each subcategory of the Service Evaluation Questionnaire. A higher Cronbach’s Alpha value, closer to 1, indicates greater reliability and consistency in measuring the intended concept within each subcategory. Table 5 presents the Cronbach’s Alpha values for four subcategories, reflecting the reliability of questions related to the evaluation of medical, nursing, and technologist services, as well as the doctor-patient therapeutic relationship.
Table 5: Cronbach’s Alpha of the Subcategories in the Service Evaluation Questionnaire.
Discussion
This study aimed to evaluate patient satisfaction among patients with head and neck cancer that are undergoing VMAT Radiation Therapy The research focused on patient satisfaction of medical, nursing, and radiation technologist services. Moreover, correlations between patient satisfaction and quality of life (QoL) were explored, providing a more comprehensive understanding of patient experiences, including psychological factors under the scope of psycho- oncology.
Patient Demographics
The demographics of the participants revealed a predominance of male patients (73.3%) compared to females (26.7%). The majority of patients were over 62 years of age (51%) and had completed either primary (40%) or secondary (45.3%) education. Most participants were married or cohabiting (72%), and a large proportion (56%) were retired. These findings align with typical patient demographics for head and neck cancer, where advanced age and retirement are common due to the median onset age of the disease and the significant role that treatment can have on patients’ physical and cognitive functions.
Service Satisfaction
Patient satisfaction with medical services was overwhelmingly positive. High levels of satisfaction were reported regarding the behavior of the medical staff (98.6% rated as good or very good), information provided about disease progression (96%), and the guidance on treatment and lifestyle (94.7% and 96%, respectively). This high satisfaction level is crucial, as effective communication and support from medical professionals can significantly impact patient outcomes and adherence to treatment regimens.
Satisfaction with nursing services was similarly high. Participants reported excellent behavior (100%), service speed (100%), and communication (100%) from nursing staff. The support provided by nurses in addressing patient problems was highly appreciated, with 69.3% reporting extreme satisfaction. This suggests that nursing staff plays a critical role in patient care, providing not only medical but also emotional support, which is vital for patients undergoing challenging treatments for head and neck cancers.
Radiation therapists received uniformly positive evaluations across all measured dimensions. All participants reported good or very good behavior, service speed, communication, and interest from technologists (100%). This highlights the critical role of technologists in ensuring the smooth operation of diagnostic and therapeutic procedures, contributing to the overall patient experience.
The notable levels of trust (98.7%) and the desire to continue medical visits (98.7%) highlight the importance of fostering strong, supportive doctor-patient relationships, which are essential for effective care and patient compliance.
Trust in nursing and radiation therapists staff was also very high (98.6% and 100% respectively), further underlining their importance in the healthcare team and indicate their significant impact on patient comfort and confidence in the treatment process.
Psychosocial Factors and Psychological Well-being
The data derived from the EORTC QLQ-C30 questionnaire, specifically from questions 21 to 24, provide insight into the emotional responses of patients with head and neck cancer across three different time points: before treatment, at the end of treatment, and three months post-treatment. These questions focus on four key emotional domains: tension, worry, irritability, and depression.
Emotional Responses Over Time
The results indicate a notable trend in the patients' emotional responses. Before treatment, a significant majority of patients reported low levels of emotional distress, with over 83.3% indicating they were "not at all" tense, irritable, or depressed, and slightly fewer (54.8%) reporting no worry. This suggests a relatively mild emotional burden before treatment. However, immediately after treatment, there was a noticeable increase in emotional distress, with fewer patients reporting no distress across all emotional domains. For instance, the percentage of patients who reported "not at all" tense decreased from 70% to 52%, and those reporting "not at all" worried dropped from 46% to 32%. This increase in distress is expected as patients face the physical and psychological challenges of cancer treatment. Three months after treatment, patients' emotional states showed improvement, with many returning to similar levels as before treatment. Although the number of patients reporting "not at all" tense, irritable, or depressed approached pre-treatment levels, there was a slight increase in mild worry, indicating some ongoing emotional burden post-treatment.
Despite the overall trend of increased emotional distress before and immediately after treatment, the emotional responses of these patients remain predominantly mild across all time points. Even at the peak of distress (right after treatment), the majority of patients report only mild or moderate levels of tension, worry, irritability, and depression. This consistent reporting of mild emotional distress, even in the face of a life-threatening disease, raises important questions regarding the accuracy and authenticity of these self-reported outcomes.
One potential explanation for these findings is that patients may be reluctant to acknowledge or express severe emotional distress, possibly due to the social stigma associated with mental health issues or a desire to appear resilient [23,24]. This reluctance might stem from an internal need to believe that they are coping well, as a part of psychological defense mechanism—a form of illness denial [25]. This phenomenon aligns with the psychological concept of defense mechanisms and the stages of grief described by Elisabeth Kübler-Ross. According to Kübler-Ross's model, denial is a common initial reaction to a life-threatening diagnosis, which might be reflected in these patients' reluctance to report severe emotional distress.
Moreover, this tendency to underreport emotional distress might be linked to the Theory of Cognitive Dissonance [26]. Patients may experience cognitive dissonance when their actual emotional state (which may be one of significant distress) conflicts with their desire to be perceived (by themselves and others) as strong and coping well [27,28]. To resolve this dissonance, they might downplay their emotional struggles, reporting them as less severe than they actually are [29].
Trust in the Procedure and Psycho-oncology Considerations
The results also raise questions about the trustworthiness of self-reported emotional distress in this patient population. If patients are consistently underreporting their emotional struggles, this could indicate a gap in the effectiveness of the current patient care model in oncology [30,31]. This gap might be further exacerbated by the possibility of patients not fully trusting the questionnaire as a tool for capturing their emotional state or feeling that their emotional struggles are less valid or important than their physical symptoms [31,32].
These observations are supported by existing literature in psycho-oncology, which suggests that cancer patients often struggle with acknowledging and articulating their emotional distress [33]. Psycho-oncological research indicates that patients with head and neck cancer, in particular, may experience alexithymia, a condition characterized by difficulty in identifying and expressing emotions [34,35,36]. This could contribute to the tendency of these patients to report lower levels of emotional distress, even when they are experiencing significant psychological challenges [37].
Further research in psycho-oncology has shown that the emotional well-being of cancer patients is crucial for their overall quality of life and treatment outcomes [38]. Studies suggest that patients who are engaged in psychological interventions, such as cognitive-behavioral therapy (CBT) or psychosocial support groups, often report better emotional and physical outcomes [39,40]. This emphasizes the importance of integrating comprehensive psycho-oncological care into the treatment plans of head and neck cancer patients.
However, the observed tendency to report only mild distress, despite the severity of the situation, suggests that current methods of assessing emotional well-being might not be entirely effective [41]. It raises the question of whether patients are receiving adequate psychological support and whether healthcare providers are fully aware of their patients' emotional needs.
Internal Consistency and Factor Analysis
The internal consistency of the service evaluation survey was commendable, with Cronbach's alpha values ranging from 0.900 to 0.946 for different subcategories. This indicates that the questionnaire is a reliable tool for assessing patient satisfaction across various dimensions of healthcare services. The exploratory factor analysis revealed a clear factor structure for each category, explaining substantial variance in: medical services (71.5%), nursing services (70%), technologist services (70%), and doctor-patient relationship (82.1%). These findings suggest that each category of the questionnaire robustly captures distinct aspects of service quality, providing a detailed and nuanced understanding of patient experiences.
Correlation Analysis
The analysis revealed statistically significant correlations between physical activity and satisfaction with nursing services (r = 0.234, p = 0.043) and the doctor-patient relationship (r = 0.238, p = 0.040). This suggests that patients who maintain higher levels of physical activity might perceive more positively the care they receive from nurses and their relationship with doctors. Additionally, there were significant negative correlations between pain and satisfaction with medical services (r = -0.238, p = 0.040), and between appetite loss and the doctor-patient relationship (r = -0.246, p = 0.033). These findings highlight that higher levels of discomfort or adverse symptoms can negatively impact patient satisfaction, which underscores the importance of effective symptom management in enhancing patient experiences.
The remarkably high percentages of patient satisfaction observed across all categories in this study are noteworthy and warrant deeper consideration. While it is encouraging to see such positive feedback, these findings raise several important questions about the underlying factors contributing to this overwhelming satisfaction.
Firstly, one must consider the possibility of biased responses. Patients might feel compelled to provide favorable feedback due to the nature of their relationship with healthcare providers or because or due to the challenges of a potentially life-threatening condition [42,43]. This raises the question: Are patients genuinely satisfied, or are they being exceptionally polite and appreciative, perhaps as a coping mechanism in facing a serious illness?
Secondly, the psychological impact of confronting a cancer diagnosis could play a significant role in how patients perceive and report their satisfaction. The fear and uncertainty associated with cancer might lead patients to value any form of care highly, creating a predisposition towards positive evaluations [44]. On a psychological level, some patients may have reached a stage of acceptance, leading to a heightened sense of appreciation for their care team and the services provided, regardless of their actual quality [45].
Another dimension to consider is the patients' understanding of their condition and treatment. The complexity of medical information and treatment protocols in oncology might leave patients feeling disoriented or unable to fully grasp the details of their care [46,47]. Consequently, they might express satisfaction simply because they lack the clarity or knowledge to critically evaluate the services they receive.
These observations suggest that there might be a need for further investigation into the authenticity of patient satisfaction reports. To ensure that feedback accurately reflects patient experiences, more nuanced and context-sensitive approaches to patient satisfaction surveys should be implemented [48]. Additionally, both patients and medical staff could benefit from appropriate training. For patients, enhanced education on their condition and treatment options could empower them to provide more informed feedback [49]. For healthcare providers, training in psychological and ethical aspects of patient care could help them better understand and support their patients' emotional and cognitive states during treatment [50].
In conclusion, while the high satisfaction rates are promising, they also highlight the importance of critically examining and understanding the factors that contribute to such positive evaluations. Addressing these questions through further research and training could lead to more meaningful insights into patient experiences and ultimately enhance the quality of care provided in head and neck cancer.
Conclusion
To summarize, this study demonstrates high levels of patient satisfaction with medical, nursing, and radiation therapists’ services among head and neck cancer patients undergoing VMAT radiation therapy, reinforcing the critical role of healthcare providers in fostering patient comfort, trust, and confidence throughout treatment. Our findings highlight the importance of effective communication, strong patient-provider relationships, and emotional support in delivering quality care. However, the data on emotional responses reveal a complexity in accurately assessing psychological well-being, particularly with the observed tendency for patients to report only mild emotional distress. This raises concerns about the potential for underreporting, which may stem from inherent biases in self-reported QoL assessments and patient satisfaction surveys. These methods, while valuable, may not fully capture the complexity of patient experiences, as patients might unintentionally provide skewed responses influenced by factors such as subjective perceptions, limited understanding of their condition, or the pressure to provide favorable feedback.
Through a comprehensive survey of patient satisfaction, psychological status, and symptom reporting, this research uniquely integrates psycho-oncological principles to better understand how patients' emotional states influence their perception and communication of symptoms. By examining patterns of satisfaction, psychological well-being, and the nuances of patient-reported outcomes, we uncover the potential discrepancies that may arise in the subjective reporting of symptoms and treatment experiences. These findings suggest that a more holistic approach to symptom assessment, one that combines objective measures with PROs, is crucial for achieving a more accurate understanding of treatment efficacy and patient well-being.
Ultimately, this study emphasizes the need for healthcare providers to be attuned not only to the physical symptoms of head and neck cancer patients but also to their psychological and emotional health. Incorporating psychological interventions, such as cognitive-behavioral therapy or psycho-social support, may further improve the accuracy of symptom assessments and enhance the overall treatment experience. Addressing these factors through enhanced education and psycho-oncological care will ensure a more comprehensive, patient-centered approach to treatment, leading to better outcomes for both patient satisfaction and quality of life.
References
- Seol KH, Bong SH, Kang DH, Kim JW. Factors Associated with the Quality of Life of Patients with Cancer Undergoing Radiotherapy. Psychiatry Investig, 2021; 18(1): 80-87. doi: 10.30773/pi.2020.0286.
- Samant R, Cisa-Paré E, Balchin K, Renaud J, Bunch L, Wheatley-Price P, et al. Assessment of Patient Satisfaction Among Cancer Patients Undergoing Radiotherapy. J Cancer Educ, 2022; 37(5): 1296-1303. doi: 10.1007/s13187-020-01950-8.
- Ferreira DC, Vieira I, Pedro MI, Caldas P, Varela M. Patient Satisfaction with Healthcare Services and the Techniques Used for its Assessment: A Systematic Literature Review and a Bibliometric Analysis. Healthcare (Basel), 2023; 11(5): 639. doi: 10.3390/healthcare11050639.
- Nolazco JI, Chang SL. The role of health-related quality of life in improving cancer outcomes. J Clin Transl Res, 2023; 9(2): 110-114.
- Elkefi S, Asan O. The Impact of Patient-Centered Care on Cancer Patients' QOC, Self-Efficacy, and Trust Towards Doctors: Analysis of a National Survey. J Patient Exp, 2023; 10: 23743735231151533. doi: 10.1177/23743735231151533.
- Voskanyan V, Marzorati C, Sala D, et al. Psychosocial factors associated with quality of life in cancer survivors: umbrella review. J Cancer Res Clin Oncol, 2024; 150: 249. https://doi.org/10.1007/s00432-024-05749-8.
- Howren MB, Christensen AJ, Karnell LH, Funk GF. Psychological factors associated with head and neck cancer treatment and survivorship: evidence and opportunities for behavioral medicine. J Consult Clin Psychol, 2013; 81(2): 299-317. doi: 10.1037/a0029940.
- Naughton MJ, Weaver KE. Physical and mental health among cancer survivors: considerations for long-term care and quality of life. N C Med J, 2014; 75(4): 283-286. doi: 10.18043/ncm.75.4.283.
- Smith HR. Depression in cancer patients: Pathogenesis, implications and treatment (Review). Oncol Lett, 2015; 9(4): 1509-1514. doi: 10.3892/ol.2015.2944.
- Carlson LE, Bultz BD. Benefits of psychosocial oncology care: improved quality of life and medical cost offset. Health Qual Life Outcomes, 2003; 1: 8. doi: 10.1186/1477-7525-1-8.
- Gitonga I, Desmond D, Duda N, Maguire R. Impact of connected health interventions on psychological wellbeing and quality of life in patients with cancer: A systematic review and meta-analysis. Psychooncology, 2022; 31(10): 1621-1636. doi: 10.1002/pon.6019.
- Nakao M, Shirotsuki K, Sugaya N. Cognitive-behavioral therapy for management of mental health and stress-related disorders: Recent advances in techniques and technologies. Biopsychosoc Med, 2021; 15(1): 16. doi: 10.1186/s13030-021-00219-w.
- Grassi L, Spiegel D, Riba M. Advancing psychosocial care in cancer patients, 2017; 6: 2083. doi: 10.12688/f1000research.11902.1.
- Lang-Rollin I, Berberich G. Psycho-oncology. Dialogues Clin Neurosci, 2018; 20(1): 13-22. doi: 10.31887/DCNS.2018.20.1/ilangrollin.
- Wang Y, Feng W. Cancer-related psychosocial challenges. Gen Psychiatr, 2022; 35(5): e100871. doi: 10.1136/gpsych-2022-100871.
- Licu M, Ionescu CG, Paun S. Quality of Life in Cancer Patients: The Modern Psycho-Oncologic Approach for Romania-A Review. Curr Oncol, 2023; 30(7): 6964-6975. doi: 10.3390/curroncol30070504.
- Kiafi P, Kouri MA, Patatoukas G, Kougioumtzopoulou A, Chalkia M, Nicolatou-Galitis O, et al. Unravelling Quality of Life for Head and Neck Cancer Patients after VMAT Radiation Therapy: Insights from Toxicity, Dosimetry and Symptoms Correlation. Clin Pract, 2024; 14(3): 1085-1099. doi: 10.3390/clinpract14030086.
- McCabe R, Healey PGT. Miscommunication in Doctor-Patient Communication. Top Cogn Sci, 2018; 10(2): 409-424. doi: 10.1111/tops.12337.
- Amelung D, Whitaker KL, Lennard D, Ogden M, Sheringham J, Zhou Y, et al. Influence of doctor-patient conversations on behaviours of patients presenting to primary care with new or persistent symptoms: a video observation study. BMJ Qual Saf, 2020; 29(3): 198-208. doi: 10.1136/bmjqs-2019-009485.
- Chang EM, Gillespie EF, Shaverdian N. Truthfulness in patient-reported outcomes: factors affecting patients' responses and impact on data quality. Patient Relat Outcome Meas, 2019; 10: 171-186. doi: 10.2147/PROM.S178344.
- Nguyen H, Butow P, Dhillon H, Sundaresan P. A review of the barriers to using Patient-Reported Outcomes (PROs) and Patient-Reported Outcome Measures (PROMs) in routine cancer care. J Med Radiat Sci, 2021; 68(2): 186-195. doi: 10.1002/jmrs.421.
- Unni E, Coles T, Lavallee DC, Freel J, Roberts N, Absolom K. Patient adherence to patient-reported outcome measure (PROM) completion in clinical care: current understanding and future recommendations. Qual Life Res, 2024; 33(1): 281-290. doi: 10.1007/s11136-023-03505-y.
- Seiler A, Jenewein J. Resilience in Cancer Patients. Front Psychiatry, 2019; 10: 208. doi: 10.3389/fpsyt.2019.00208.
- Hughes L, Taylor RM, Beckett AE, Lindner OC, Martin A, McCulloch J, et al. The Emotional Impact of a Cancer Diagnosis: A Qualitative Study of Adolescent and Young Adult Experience. Cancers (Basel), 2024; 16(7): 1332. doi: 10.3390/cancers16071332.
- Temiz R. Existential Social Work in Coping with Death and Grief. Clin Soc Work J, 2024. https://doi.org/10.1007/s10615-024-00922-5
- Bran A, Vaidis DC. On the Characteristics of the Cognitive Dissonance State: Exploration Within the Pleasure Arousal Dominance Model. Psychol Belg, 2020; 60(1): 86-102. doi: 10.5334/pb.517.
- Cancino-Montecinos S, Björklund F, Lindholm T. A General Model of Dissonance Reduction: Unifying Past Accounts via an Emotion Regulation Perspective. Front Psychol, 2020; 11: 540081. doi: 10.3389/fpsyg.2020.540081.
- O'Donnell EK, Shapiro YN, Yee AJ, Nadeem O, Laubach JP, Branagan AR, et al. Quality of life, psychological distress, and prognostic perceptions in caregivers of patients with multiple myeloma. Blood Adv, 2022; 6(17): 4967-4974. doi: 10.1182/bloodadvances.2022007127.
- Cancino-Montecinos S, Björklund F, Lindholm T. Dissonance reduction as emotion regulation: Attitude change is related to positive emotions in the induced compliance paradigm. PLoS One, 2018; 13(12): e0209012. doi: 10.1371/journal.pone.0209012.
- Lyu XC, Jiang HJ, Lee LH, Yang CI, Sun XY. Oncology nurses' experiences of providing emotional support for cancer patients: a qualitative study. BMC Nurs, 2024; 23(1): 58. doi: 10.1186/s12912-024-01718-1.
- Elkefi S, Asan O. The Impact of Patient-Centered Care on Cancer Patients' QOC, Self-Efficacy, and Trust Towards Doctors: Analysis of a National Survey. J Patient Exp, 2023; 10: 23743735231151533. doi: 10.1177/23743735231151533.
- Spurrier GF, Shulman K, Dibich S, Benoit L, Duckworth K, Martin A. Physical symptoms as psychiatric manifestations in medical spaces: A qualitative study. Front Psychiatry, 2023; 13: 1074424. doi: 10.3389/fpsyt.2022.1074424.
- Dekker J, Karchoud J, Braamse AMJ, Buiting H, Konings IRHM, van Linde ME, et al. Clinical management of emotions in patients with cancer: introducing the approach "emotional support and case finding". Transl Behav Med, 2020; 10(6): 1399-1405. doi: 10.1093/tbm/ibaa115.
- Messina A, Fogliani AM, Paradiso S. Alexithymia in oncologic disease: association with cancer invasion and hemoglobin levels. Ann Clin Psychiatry, 2011; 23(2): 125-130.
- Howren MB, Christensen AJ, Karnell LH, Funk GF. Psychological factors associated with head and neck cancer treatment and survivorship: evidence and opportunities for behavioral medicine. J Consult Clin Psychol, 2013; 81(2): 299-317. doi: 10.1037/a0029940.
- Ozonder Unal I, Ordu C. Alexithymia, Self-Compassion, Emotional Resilience, and Cognitive Emotion Regulation: Charting the Emotional Journey of Cancer Patients. Curr. Oncol, 2023; 30: 8872-8887. https://doi.org/10.3390/curroncol30100641.
- Jagannathan A, Juvva S. Emotions and coping of patients with head and neck cancers after diagnosis: A qualitative content analysis. J Postgrad Med, 2016; 62(3): 143-149. doi: 10.4103/0022-3859.184273.
- Bognár SA, Teutsch B, Bunduc S, et al. Psychological intervention improves quality of life in patients with early-stage cancer: a systematic review and meta-analysis of randomized clinical trials. Sci Rep, 2024; 14: 13233. https://doi.org/10.1038/s41598-024-63431-y.
- Nakao M, Shirotsuki K, Sugaya N. Cognitive-behavioral therapy for management of mental health and stress-related disorders: Recent advances in techniques and technologies. Biopsychosoc Med, 2021; 15(1): 16. doi: 10.1186/s13030-021-00219-w.
- Yu HM, Wang L, Pan CZ. The impact of cognitive behavioural therapy-based psychological intervention on emotional improvement in elderly patients with extensive burns. Int Wound J, 2024; 21(2): e14594. doi: 10.1111/iwj.14594.
- Proctor CJ, Reiman AJ, Best LA. Cancer, now what? A cross-sectional study examining physical symptoms, subjective well-being, and psychological flexibility. Health Psychol Behav Med, 2023; 11(1): 2266220. doi: 10.1080/21642850.2023.2266220.
- Dunsch F, Evans DK, Macis M, Wang Q. Bias in patient satisfaction surveys: a threat to measuring healthcare quality. BMJ Glob Health, 2018; 3(2): e000694. doi: 10.1136/bmjgh-2017-000694.
- Mazor KM, Clauser BE, Field T, Yood RA, Gurwitz JH. A demonstration of the impact of response bias on the results of patient satisfaction surveys. Health Serv Res, 2002; 37(5): 1403-1417. doi: 10.1111/1475-6773.11194.
- Mazzocco K, Masiero M, Carriero MC, Pravettoni G. The role of emotions in cancer patients' decision-making. Ecancermedicalscience, 2019; 13: 914. doi: 10.3332/ecancer.2019.914.
- King R, Stafford L, Butow P, Giunta S, Laidsaar-Powell R. Psychosocial experiences of breast cancer survivors: a meta-review. J Cancer Surviv, 2024; 18(1): 84-123. doi: 10.1007/s11764-023-01336-x.
- Wreyford L, Gururajan R, Zhou X. When can cancer patient treatment nonadherence be considered intentional or unintentional? A scoping review. PLoS One, 2023; 18(5): e0282180. doi: 10.1371/journal.pone.0282180.
- Marron JM, Kyi K, Appelbaum PS, Magnuson A. Medical Decision-Making in Oncology for Patients Lacking Capacity. Am Soc Clin Oncol Educ Book, 2020; 40: 1-11. doi: 10.1200/EDBK_280279.
- Larson E, Sharma J, Bohren MA, Tunçalp Ö. When the patient is the expert: measuring patient experience and satisfaction with care. Bull World Health Organ, 2019; 97(8): 563-569. doi: 10.2471/BLT.18.225201.
- Vainauskienė V, Vaitkienė R. Enablers of Patient Knowledge Empowerment for Self-Management of Chronic Disease: An Integrative Review. Int J Environ Res Public Health, 2021; 18(5): 2247. doi: 10.3390/ijerph18052247.
- Bradshaw J, Siddiqui N, Greenfield D, Sharma A. Kindness, Listening, and Connection: Patient and Clinician Key Requirements for Emotional Support in Chronic and Complex Care. J Patient Exp, 2022; 9: 23743735221092627. doi: 10.1177/23743735221092627.

