HRCT Chest and Nasopharyngeal Swab PCR Co-relation in Suspected Covid-19 Patients- A Multi-center Review of Patients
Sadia Azam, Abdulrehman Khalid, Zohaib Ramzan, Vishal Farid Raza*, Muhammad Ahmad and Abid Ali
University of Lahore, Department of Medical Imaging, Gujrat, Pakistan
Sir Ganga Ram Hospital, Pakistan
Muhammad Ahmad, DHQ Hospital Sheikhupura, Department of Cardiology
Received Date: 29/04/2021; Published Date: 05/05/2021
*Corresponding author: Vishal Farid Raza,Sir Ganga Ram Hospital, Lahore, Pakistan. Email: vishalraza@hotmail.com; ORCID ID 0000-0002-1133-6170.
Abstract
Introduction: COVID-19 pandemic has placed a large onus on radiologists to help the diagnosis of patients, especially in cases where PCR results may not tie up with clinical situation.
Methods: Prospective cohort study was done with 76 participants who were suspected for COVID-19 infection and were followed to evaluate PCR and HRCT reporting in tandem with clinical symptoms.
Results: 86.8% of patients had a dry cough, followed most commonly with shortness of breath. 57.9% of patients had ground-glass opacities of haze on HRCT followed by 43.4% who had consolidations present. 84.2% patients had a positive PCR whereas 67.1% had an HRCT that was suggestive of having COVID-19 pneumonia. Sensitivity of HRCT using PCR as a gold standard was calculated at 65.6% and specificity was 25% while accuracy was calculated at 59%.
Conclusion: Triple assessment with clinical symptomatology, HRCT findings and PCR should be utilized, especially in areas where there is a lower positivity rate for COVID-19.
Keywords: COVID-19 Pneumonia; HRCT; PCR; Pakistan
Introduction
The COVID-19 pandemic is the fifth pandemic to be encountered in modern times that is documented, originating from China in 2019. It has changed the way modern medicine is conducted and introduced a component of infectious diseases to all disciplines of medicine due to it its unpredictable course in patients and it’s continual widespread [1]. A large onus falls on radiologists to help the diagnosis of patients with COVID-19, as many patients may have positive PCR but be asymptomatic, however pulmonary involvement may exist [2]. Radiologists developed the CO-RADS criteria for streamlining radiological findings on chest CT scans for the diagnosis and severity grading of COVID-19 infections. This grading involves 1 being least likely possibility of COVID-19 through to 6 which is documented covid-19 infection; the severity scale goes from unlikely to atypical infection to typical infection with a high suspicion [3]. Further the CO-RADS criteria developed was done so with typical and atypical findings in sight. Typical findings may contain crazy paving, consolidations with ground glass opacities, amongst others. Atypical findings may contain halo sign, infiltrates, and effusions amongst others [4]. Even though HRCT is a useful adjunct tool in screening of early manifestations in the lung parenchyma, it remains an adjunct to the PCR as PCR remains the gold standard. However, it is not unheard of that HRCT may show early changes in symptomatic patients, where a PCR is negative. The utility of both tools, PCR and HRCT cannot be undermined in the current pandemic, and the utility of HRCT as a follow up tool for pulmonary manifestations extension and remission remains vital, further HRCT may be considered sensitive however PCR remains specific [5]. Though there is no dearth of literature on COVID-19 patients, with extensive publications occurring in the wake of the pandemic- with evolving strains [6] and ever-growing change in presentation and findings, literature on COVID-19 remains a constant need to establish better and clearer management and diagnosis criteria.
Materials and Methods
This study was conducted from November 2020 till January 2021, where files of suspected COVID-19 patients were reviewed and followed-up until PCR result became available and HRCT was done. This prospective cohort study was done with the objective to study the relationship between PCR results and HRCT results amongst suspected COVID-19 patients. Data was collected from three different tertiary care hospitals in Pakistan in the 3 months period. Informed consent was taken from all patients and ethical approval taken from ethical review board. SPSS V 24.0 was used to analyses the data of 76 patients that presented as suspected COVID-19 patients in these hospitals over the study period.
Results
Of our 76 participants, mean age of participants was 55.6 years S.D 14.6, the oldest patient was 87 years old and the youngest was 19 years old. 34.2% were female and 65.8% were male.
Of the three most common symptoms, 77.6% had shortness of breath; 86.8% had a dry cough, 57.9% had fever and 6.6% (n=5) had chest pain or tightness.
Findings on examination showed that 15.8% (n=12) patients had a clear chest, 43.4% (n=33) had bilateral crackles, 10.5% (n=8) had bilateral crepitations, and 5.3% (n=4) had bilateral wheeze. 25% (n=19) patients had decreased air entry.
84.2% of patients in our study had a positive PCR test result that is 64 of the participants, whereas only 12 had a negative result 15.8%.
We reviewed HRCTs and enlisted common findings for pulmonary disease and COVID-19 and found the following:
Table 1: Enlisting of different HRCT findings
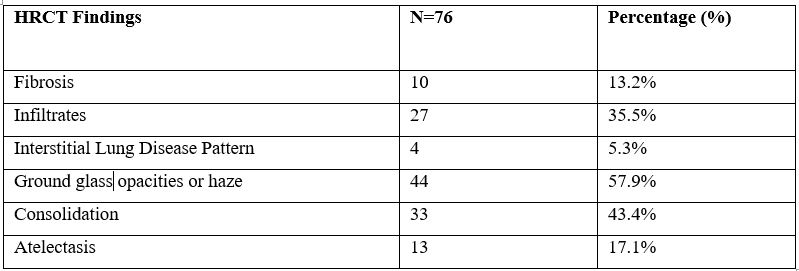
Fibrosis was present in 2 patients who had a history of tuberculosis; however, they were PCR positive.
Of our patients 13.2% (n=10) were diabetic, 21.1% (n=16) were hypertensive, and13.2% (n=10) were smokers. 14.5% (n=11) had re-infections of COVID-19 at the time of presentation and had already had COVID-19 prior to the current presentation at least 2 months before.
13.2% (n=10) patients were on supplemental oxygen at the time of HRCT.
Of the total HRCTs that were done, 67.1% (n=51) were suggestive of COVID-19 pneumonia. Of the 25 HRCTs that were not suggestive of COVID-19 pneumonia, 16 were normal HRCTs.
A chi-square test was done to see if PCR result was significantly associated to HRCT result, a p-value off 0.01 was obtained, thus showing there is a significant association between a positive PCR test and an HRCT suggestive of COVID-19 pneumonia. However, 9 HRCTs were suggestive of COVID-19 pneumonia, when the PCR was negative, and 22 PCR were positive but HRCT was not suggestive of COVID-19 pneumonia.
Most of our participants were nonsmokers, with only 10 smokers of whom 8 had a positive PCR result, we analyzed whether smoking had a correlation with having a positive PCR result or having COVID-19 and found a p-value of 0.69 which was not significant, thus we can surmise that in our cohort of patients smoking was not associated with having COVID-19 pneumonia.
We analyzed using Chi-Square test whether the different findings on HRCT were significantly correlated with the HRCT being suggestive of COVID-19 and found the following results:
Table 2: Findings on HRCT suggestive of COVID-19 Pneumonia
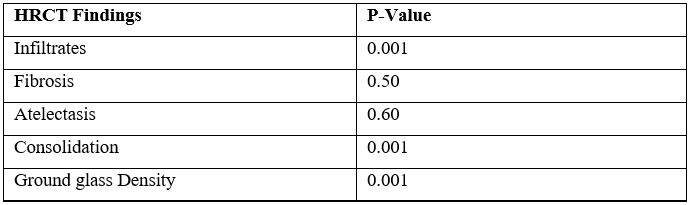
Infiltrates, consolidation and ground-glass haze or densities were positively correlated with having suspicion of COVID-19 pneumonia on HRCT.
Sensitivity of HRCT using PCR as a gold standard was calculated at 65.6% and specificity was 25% while accuracy was calculated at 59%.
Discussion
A study done in Pakistan in 2021 showed that the sensitivity and specificity were 92% and 23% respectively while accuracy was 51%. While they had a sensitivity of 92%, our sensitivity was lower at 65.6% showing that the true positive rate with HRCT in our study was lower, however, their specificity was 23%, ours was 25% as in our study there were only 3 participants that had HRCTs that were negative for COVID-19 and had a negative PCR result as well. Of the twelve PCRs that were negative, 9 patients had symptoms and HRCT findings that were suggestive of COVID-19 pneumonia [7].
A systematic review done found that the sensitivity was higher, especially in areas where the epidemic was more profound; with values above 90%, however in areas where the cases were lower sensitivity was down to even 61%. We can appreciate this in Pakistan’s case where cases are lower and positivity rates are lower than most other regions, with the highest positivity rate being around 25% in May 2020. The systematic review further noticed that specificity rate were variable with higher specificities in areas of higher positivity and where the pandemic has greater hold, with other areas reporting specificities as low as 25% [8]. This raises the question that the 9 patients that were PCR negative in our study who were treated as suspected COVID-19 due to HRCT findings coupled with symptomatology, perhaps they had a false negative PCR result, but the HRCT was correctly positive in this situation.
It raises the question that instead of using PCR as a gold standard, clinical scenarios should be evaluated based on symptomatology, PCR result and HRCT findings; a form of triple testing. Wherein, two positives of the three should be fundamentally the criterion to label someone has being affected by COVID-19 pneumonia.
Though research suggests that the odds of getting severe COVID-19 disease in twice that in smokers, it is interesting to note that a smaller percentage of smokers had disease in our cohort of patients [9]. Pakistan is a country with a high usage of tobacco products, with 19.1% adults using them and above 80% being exposed to second hand smoke in public areas [10], however the percentage of smokers in our participants was much lower than expected. The odds of having COVID-19 and being a non-smoker were 1.06 times more in our participants than being a smoker.
Ground-glass opacities, infiltrates and consolidation were the most specific findings for COVID-19 pneumonia, with most emphasis placed on ground-glass opacities being a typical finding defined by the Dutch Radiological Society [11].
It is interesting to note that these were the findings that were positively correlated in our study to have been found on HRCTs where COVID-19 was confirmed by PCR. Keeping this in view, we can assume that such findings in tandem with the clinical scenario should raise high suspicion for COVID-19 pneumonia for clinicians who may be facing diagnostic dilemmas or entertaining different diagnoses during the pandemic.
Conclusion
We found that COVID-19 pneumonia has typical patterns on HRCT and using the CO-RADs criteria HRCT is a useful tool in establishing a diagnosis. Triple assessment with clinical symptomatology, HRCT findings and PCR should be utilized, especially in areas where there is a lower positivity rate for COVID-19.
Declarations
Funding: All funding was done by the authors themselves
Conflicts of Interest: None to declare
Availability of data and material: Available with corresponding author
Code availability: Available with corresponding author
Author’s contributions: SA, SA, and VFR participated in data collection, writing of manuscript and concept design. AA participated in concept design, final editing of manuscript and proof-editing.
Ethics approval: Approval from ERC was sought and taken to undertake this study.
References
- Liu YC, Kuo RL, Shih SR. COVID-19: The first documented coronavirus pandemic in history. Biomed J. 2020; 43(4): 328-333.
- Shi H, Han X, Jiang N, Cao Y, Alwalid O, Gu J, et al. Radiological findings from 81 patients with COVID-19 pneumonia in Wuhan, China: a descriptive study. Lancet Infect Dis. 2020; 20(4): 425-434.
- Prokop M, van Everdingen W, van Rees Vellinga T, Quarles van Ufford H, Stoger L, Beenen L, et al. CO-RADS: A Categorical CT Assessment Scheme for Patients Suspected of Having COVID-19-Definition and Evaluation. Radiology. 2020; 296(2): E97-E104
- Caruso D, Polidori T, Guido G, Nicolai M, Bracci B, Cremona A, et al. Typical and atypical COVID-19 computed tomography findings. World J Clin Cases. 2020; 8(15): 3177-3187.
- Araujo-Filho JAB, Sawamura MVY, Costa AN, Cerri GG, Nomura CH. COVID-19 pneumonia: what is the role of imaging in diagnosis? J Bras Pneumol. 2020; 46(2): e20200114.
- Awadasseid A, Wu Y, Tanaka Y, Zhang W. SARS-CoV-2 variants evolved during the early stage of the pandemic and effects of mutations on adaptation in Wuhan populations. Int J Biol Sci. 2021; 17(1): 97-106.
- Hanif N, Rubi G, Irshad N, Ameer S, Habib U, Zaidi SRH. Comparison of HRCT Chest and RT-PCR in Diagnosis of COVID-19. J Coll Physicians Surg Pak. 2021; 30(1): S1-S6.
- Xu B, Xing Y, Peng J, Zheng Z, Tang W, Sun Y, et al. Chest CT for detecting COVID-19: a systematic review and meta-analysis of diagnostic accuracy. Eur Radiol. 2020; 30(10): 5720-5727.
- Gulsen A, Yigitbas BA, Uslu B, Dromann D, Kilinc O. The Effect of Smoking on COVID-19 Symptom Severity: Systematic Review and Meta-Analysis. Pulm Med. 2020; 2020: 7590207.
- Saqib MAN, Rafique I, Qureshi H, Munir MA, Bashir R, Arif BW, et al. Burden of Tobacco in Pakistan: Findings from Global Adult Tobacco Survey 2014. Nicotine Tob Res. 2018; 20(9): 1138-1143.
- Shirani F, Shayganfar A, Hajiahmadi S. COVID-19 pneumonia: a pictorial review of CT findings and differential diagnosis. Egyptian Journal of Radiology and Nuclear Medicine. 2021; 52(1): 38.

