Doctor-Patient Relationship: “The Doctor as The Drug”
Fatimah Lateef*
Senior Consultant, Department of Emergency Medicine, Singapore General Hospital, Core Faculty, Emergency Medicine Residency, Sing Health, Professor, Duke NUS Graduate Medical School, Yong Loo Lin School of Medicine, National University of Singapore and Lee Kong Chian Medical School, Nanyang Technological University, Director, Sing Health Duke NUS Institute of Medical Simulation (SIMS), Faculty, Duke NUS Global Health Institute, Singapore
Received Date: 04/07/2025; Published Date: 20/08/2025
*Corresponding author: Fatimah Lateef, FRCS (A&E), MBBS, FAMS (Em Med), Senior Consultant, Dept of Emergency Medicine, Singapore General Hospital, Core Faculty, Emergency Medicine Residency, Sing Health, Professor, Duke NUS Graduate Medical School, Yong Loo Lin School of Medicine, National University of Singapore and Lee Kong Chian Medical School, Nanyang Technological University, Director, Sing Health Duke NUS Institute of Medical Simulation (SIMS), Faculty, Duke NUS Global Health Institute, Singapore
Abstract
The “Doctor as the Drug” concept originated from Michael Balint, who proposed that the doctor-patient relationship can be a very powerful therapeutic ‘agent’, just like how a drug can alleviate pain and suffering. The doctor’s presence, personality and actions are important as these can have impact on patients. This therapeutic effect of the ‘drug’ can be positive or negative, depending on factors such as the doctor’s performance and the patient’s expectations.
Balint also proposed that; ‘the most powerful drug we can prescribe is ourselves’. Despite the fact that this proposal has been around for a long time, it seems to have been forgotten, not studied or pursued actively or emphasized in the general practice of Medicine. The concept may not have been readily understood as some may go on to enquire, if the doctor is the ‘drug’ then what is the dose, frequency and form of delivery/ prescription? It is also about how to use the ‘drug’ so that many can benefit. Balint did acknowledge these. He found it challenging to propose the correct dosage (referring to the frequency of visits; too many or frequent visits could have an addictive property and over-reliance on the doctor) or side-effects of the “drug” (referring to what harm the doctor can do) and so on. Perhaps it would be more appropriate for generations of practitioners to define these themselves. The author feels it is a very good analogy, which may have been overlooked but should not be subjected to abuse or misinterpretation, ie. some may misconstrue it as the Doctor being the “drug dealer”, which should not be the case.
The author also feels that the concept of the “Doctor as the Drug” can be brought back and refreshed against the evolving background of the doctor-patient relationship today. It can be used in medical schools at the undergraduate level as well as post-graduate and practitioner level. The author herself, a senior Emergency Physician is a strong proponent of the concept and utilizes it in her training of healthcare staff. Her view remains that despite all the technological advances over the years, compassionate, caring and healing doctors remain the best therapeutic tool in Medicine.
Keywords: Doctor-patient relationship; Communications
Introduction: Consultation Models
In the delivery of care, a comprehensive and practical consultation framework can help foster an effective doctor-patient rapport. The central element in this relationship is appropriate, effective and impactful communications [1]. In building a positive doctor-patient relationship there are the following consultation models to consider [2,3]:
1. A Doctor-centric model [4]:
This is where the doctor will take the history of the chief complaint, history of the present illness, past medical history, do systems review and then take the family, social and drug history. This will be followed by the physical examination to attain their perspective of the biological diagnosis and then the disease management part, where there will be investigations, prescribing and disposition plans. These steps make up the process of clinical reasoning.
2. A Patient-centric model [3,4]:
In this model the patient’s ideas, concerns, expectations and impact of their problem is shared with the doctor. This will enable the astute doctor to add on any relevant psycho-social diagnosis and thus, plan further management, which may include education, explanation, counselling and reassurance.
3. The Doctor-Patient Relationship [2,5]:
This is a two-fold interaction between a patient and the doctor. It refers to when the rapport is first established, facilitated and continue to be nurtured throughout the consultation and care provision for the patient. The relationship is about service provision on the one hand, and treatment-based communications between two parties in a potentially healing effect, on the other hand. Empathy is an essential element which patients can discern during the consultation with their doctors (during history taking, examination and discussion on management). A positive and good consultation process will end with the closing of the doctor-patient relationship and partnership on a positive note and will likely result in a higher compliance rate to the advice/ medication/ treatment provided. Positive doctor-patient relationship will increase both patients’ and doctors’ satisfaction, uplift compliance rates by the patients, enhance quality of care and ensure more effective use of healthcare resources.
In our busy practice, it is often that we may be very good and efficient with the Doctor-centric model as it is faster and tend to be driven by the medical professional. It is also a very task-driven model, which works well with the heavy patient load most doctors encounter today. This functional model generally works but may not have a significant doctor-patient bond established. Some more senior or experienced doctors may be able to combine and integrate the Doctor-centric and patient-centric models better to foster the positive doctor-patient relationship. This will usually give the patient a more satisfactory experience of the consultation [5,6].
The patient’s presentation style and the way the doctor respond to the illness is very important in establishing the doctor-patient relationship. If there is a mismatch or incompatibility, complications and disagreement may arise. Also, it has to be borne in mind that not all patients are forthcoming with sharing all their symptoms openly as they may want to be perceived as a “good patient” [6].
Transformation of the Doctor-Patient Relationship
Over the years, with the changes in the practice of Medicine, there has been evolution of the doctor-patient relationship. This is despite the fact that this relationship remains the core of the practice of Medicine and relationships are the foundation of experience [7,8]. Some of the reasons for this would include:
- The widespread use of technologies and IT (Information technology), which affects connection
- The changes in the structure of the clinical encounter e.g., teleconsultation, greater choices of healthcare providers
- Presence of newer pathologies and methodologies in Medicine today, which has resulted in specialization and sub-specialization which may thrust practice towards more siloed care.
- The greater medicalization of day-to-day life, contributed to by platforms such as Dr Google.
- Stronger presence of medical marketing
- Impact of the pharmaceutical industry which has expanded globally
- Influence of media and also the use of social media
- Greater awareness of medico-legal issues, in general
Besides the above factors, generational changes too has effect on the doctor-patient relationship. The strong face to face bonds nurtured by the Traditionalist and Baby Boomers generations may be less obvious today. The short attention span, savviness with IT usage, mobility and values of Generation Y and Z, will certainly foster a different kind of doctor-patient relationship, which may tend to be more cursory and fleeting. (8-11)). In fact, today, with the greater availability of information, platforms such as Dr Google, it is likely that younger and informed patients will be asking for repeat prescriptions for medication and not really going through a formal face to face consultation, as in the old days [2,9].
All these changes have led to the re-engineering of the doctor-patient relationship. From the small, solo practice of old to the more complex healthcare ecosystem of today. With large Academic Medical Centers and hospitals, the patient-doctor relationship continues to evolve:
- From individualized care delivery, it is now about team-based care and inter-professional processes. Patients have interaction with multiple doctors from various specialties and with each one they would have a unique relationship. Also, beyond just doctors, there are now nurses, allied health professionals, administrative healthcare staff and more that patients have to interact with in the course of seeking healthcare. The various permutations will make the relationships more intricately inter-woven.
- The old adage of “care for the patient, care for his family” may not hold true today. With nuclear families and children living away from parents, individual family members will seek their own care pathway with different professionals. They will thus establish their own relationships. The concept of family driven care delivery has now been altered.
- Technological development and progress mean we now have various machines, e-tools, devices and support services in the delivery of care. These “toys” used in the delivery of care to patients may tend to make consultations more “cold”, impersonal and less human, especially in the eyes of the more senior and geriatric patients, who are able to compare this practice with the olden days.
- As more institutions and healthcare clinics embark on the use of e-health records and electronic records system, consultations need not take as much time as before and details are available at the finger tips very readily. This may be viewed as more ‘superficial consultation’ by some patients as the doctor may not have to ask as many questions as before.
- With modern technology and increasing drug efficacy, doctors can now divert their attention to images, scans and Xray’s, as well as focus on the disease instead of the patients. All these developments are already driving how care is being delivered today.
- There is the rise of the assertive and empowered patients today. This is different from the past where patients were highly reliant on their physicians. Today, patients are better informed, well-read and expect the best and the latest in terms of care. There may seem to be a shift in the authority; from the doctor to the patient. This can certainly alter the doctor-patient relationship towards anew transactional impact.
With these rapid changes, training the new generation of doctors need to adapt as well. Reinforcements that humanism must continue to be maintained in the age of technology is crucial. Medical faculty and medical teachers nurturing the next generation of providers must be clear in their messaging and also be good role models themselves [12-14].
Illness Behaviour
One aspect of the doctor-patient relationship often overlooked is the illness behavior of the patient. It is not always possible in places such as the Emergency Department and very busy clinics to spend a sufficient amount of time with the patient. Thus, short cuts may be taken and the illness behavior portion is the one often left out. Illness behavior refers to how a person feels, thinks about and react to his illness. This is about how his symptom is perceived and what prompted him to seek medial consultation. It involves a complex process with multiple variables to consider [2,4]. There are many factors which can influence illness behavior. Some of these are [1,2,9]:
- Age: the young and geriatric age-groups may tend to utilize more medical services
- Gender: may tend to be country or area specific
- Race: also, may be county or area specific
- Learned behavior, which may arise in the case of use of placebo to acknowledge somatization pain. This may send the signal and perception that the doctor feels the patient has serious symptoms
- Accessibility to service, often affected by the urban-rural divide
- Their previous experience and beliefs
- Social class, which affects affordability. Social class also influence educational, income and status levels, as well as
- Locus of control: Some people are independent and believe things are under their control. These people have an internal locus of control. Others may feel they have no or less control over their life; they will have an external locus of control and will tend to seek more medical help.
Illness denial may happen because it is not easy for a patient to show his ‘weakness or vulnerabilities’. The presence of illnesses may impact their self-esteem. Doctors may tend to come across as authoritative figures in some societies. This may cause challenges for some patients to interact with the doctors. The issue of affordability and prioritizing other more pressings daily needs may also affect health seeking behavior [15,16].
People may tend to self-medicate and tolerate their ailments. Any increase in self-care may be linked to factors such as:
- The shift of symptoms from the acute to the more chronic ones
- Dissatisfaction with the care or the doctor
- Limitation of what modern or western medicine can offer
- Increasing use of traditional and alternative medicine
- Wish for personal control and
- Increased awareness of lifestyle effects on health
Fig 1 shows the Illness Framework from the patient’s perspective versus the Disease Framework thinking process of the doctor. Patients’ illness behavior will impact their Illness Framework thinking. These would include their feelings and thoughts about their illness, concerns and expectations they would expect from the consultation and also the effects of their symptoms. All these are very variable and unique, according to each individual patient [2,12,14]. The Disease Framework on the other hand, is relatively more constant and depicts what doctors would go through as part of the clinical reasoning process in managing their patients. Both frameworks need to be integrated adequately for an optimal doctor-patient relationship. If there are gaps not addressed, it will affect satisfaction and trust levels in the relationship. This is also why besides performing the task driven Disease Framework approach, doctors need to be aware of their patients’ Illness Framework and address these adequately [5,6,10,17].
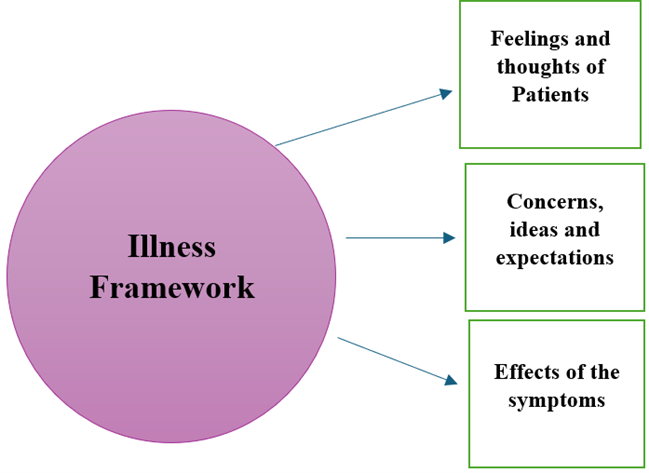
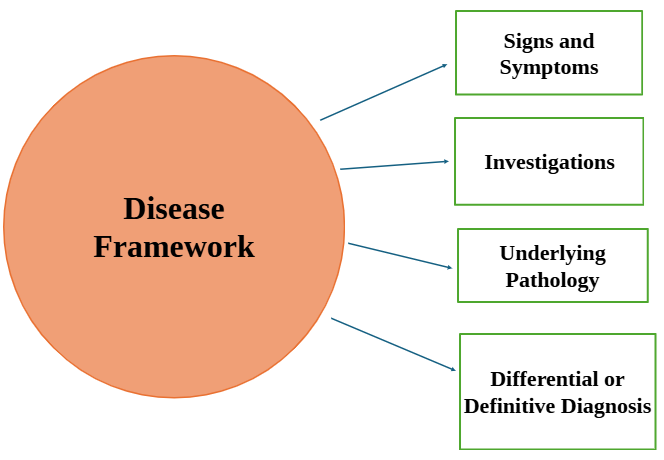
Figure 1: Illness versus Disease Frameworks of the Patients and their Doctors respectively.
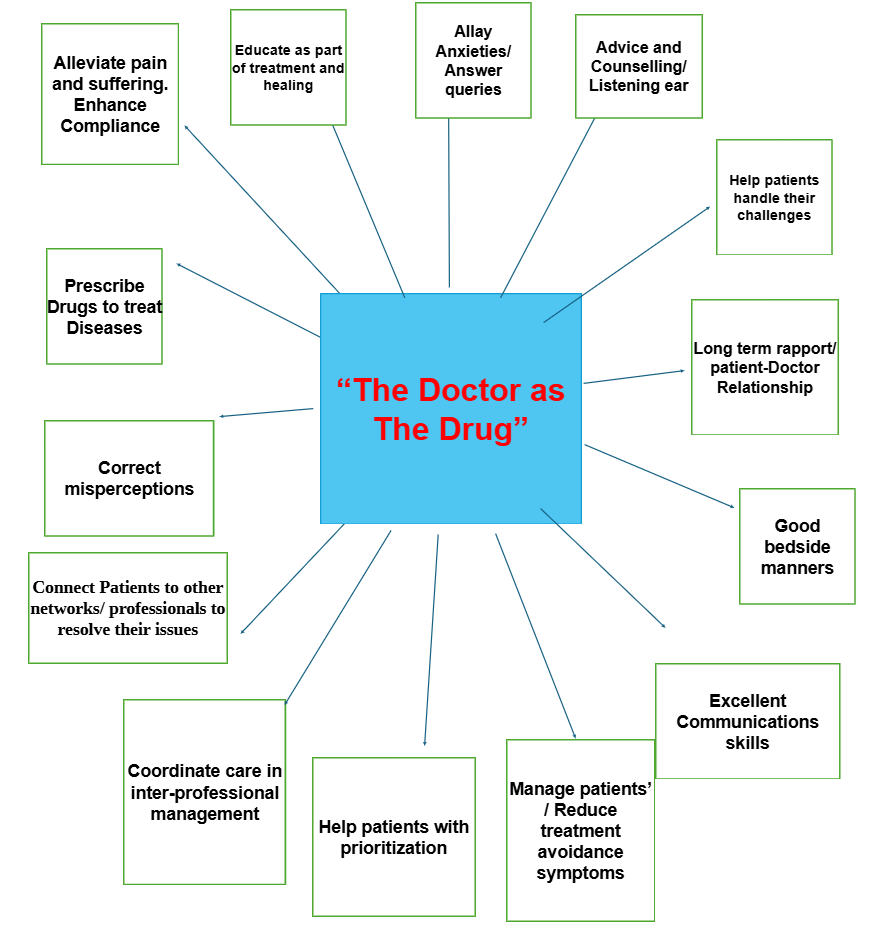
Figure 2: Roles of the Doctor as the “Drug”.
The “Doctor as The Drug”
This concept originated from Michael Balint, who proposed that the doctor-patient relationship can be a very powerful therapeutic ‘agent’, just like how a drug can alleviate pain and suffering, beyond just the specific medical interventions or treatment. The doctor’s presence, personality and actions are important as these can have impact on patients. This therapeutic effect of the ‘drug’ can be positive or negative, depending on factors such as the doctor’s performance, communications (verbal and nonverbal), demeanor and behavior, considered against the patient’s expectations [18,19].
The general definition of a ‘drug’ can be any substance that can be used to prevent, diagnose, treat or relieve symptoms of a disease or abnormal condition. A “drug” can also affect bodily functions, mood, thoughts, feelings and behaviour. Figure 2 depicts the variety of roles the doctor can execute and fulfill in line with the broad definition of “drug”. Using the concept of “Doctor as the drug”, it needs to be viewed from a broadened perspective.
What Balint is proposing is that; ‘the most powerful drug we can prescribe is ourselves’. This proposal has been around for a long time but it seems to have been forgotten, not studied or pursued actively and not emphasized [18]. Some may ask: if the doctor is the ‘drug’ then what is the dose, frequency and form of delivery/ prescription? It is also about how to use the ‘drug’ so that many can benefit. Balint did acknowledge that little was known about the “drug”: example, the correct dosage (referring to the frequency of visits; too many or frequent visits could have an addictive property and over-reliance on the doctor), side-effects of the “drug” (referring to what harm the doctor can do) and so on. Thus, the pharmacology of the patient-doctor relationship can be therapeutic with just the right balance of things and sufficient reassurance [18,20]. Just as when a drug is being administered, along the lines of patient safety practices, it should be the right drug, given in the right dose, right frequency, for the right duration and in the right concentration [19]. Despite all the technological advances over the years, compassionate, caring and healing doctors remain the best therapeutic tool in Medicine.
Adequate communications are central to the concept of “Doctor as the Drug”. Doctors must learn to listen attentively and filter all the relevant information their patients share with them. They should be able to make their patients feel at ease to facilitate their sharing and asking questions, some of which can be very intimate [21]. Empathetic communications are very apt as it can help the doctor associate himself with the situation of the patient. The use of words of kindness and support is important; just as the selection of the choice of appropriate words and phrases. The communications should preferably provide hope for the patients, but not false hope. The doctor has to be sufficiently assertive, but not aggressive so as to put the patient off from asking questions. Exploring the patients’ social status, educational background, religious beliefs and cultural practices can be very useful for the doctor to understand their perspectives and thus, their Illness Framework. Every patient will be unique and no two conversations will be the same. Reducing confusion and misunderstanding is also important. Using non-medical jargon, setting aside platform for questions and ‘repeating back’ the information shared are also very useful. There are also unique situations such as conversations with seniors, geriatric patients and interacting with pediatric patients. These would require a lot of innovative approaches, customization, creativity and thinking out of the box [6,15,16].
In the doctor-patient partnership, during consultation, “Doctor as the Drug” is demonstrated by the following [22,23]:
- The consultation process, whereby the doctor listens to the patient’s history and complaints. This is rather cathartic and may have a ‘cleansing’ effect on the patient as they ‘let it all out’ and are able to tell someone about their issues and ventilate appropriately
- The empathetic and active listening by the doctor is very valuable and means a whole lot to the patients, in helping to allay their anxieties and concerns. Good, empathetic communications comprise of attentive, active listening, with positive verbal and non-verbal communications techniques. These are like ‘drugs’ to the patient
- During the conversation, the doctor will usually be able to filter out the patient’s concerns and misperceptions. These will present as opportunities for the doctor to correct and address these and as a result may not make the patient unnecessarily worried
- After listening and understanding the problems, the doctor will plan the management and treatment. Besides this, he can also make the needed referrals and connect the patient with other professionals and services required to manage their problem in its entirety. This means the consultation can help channel patients to resources which they may not know of or are unable to access on their own
- Literally, during treatment, the appropriate drugs can be prescribed for the patient
The doctor can also usually help the patient prioritize their issues and complaints because they can create link between symptoms and tie this to one diagnosis or otherwise. This can then be explained to the patient to uplift their own level of understanding of the potential medical problems
Discussion
The 21st century patients are co-producers of their own health. They will actively participate as co-decision makers in their healthcare issues. This shared model is a thrust towards patient centricity as healthcare professionals strive to put patients at the heart of all they do. This mutual participatory model seems to be the way forward into the future of healthcare provision. The doctor-patient relationship is now re-engineered due to technological advancement, changing expectation of patients and a more collaborative and digitally driven dynamic. Whilst trust, communications and empathy still remain crucial, patient are now prioritizing factors such as convenience, access, digital engagement, alongside the doctors’ reputation, capabilities, knowledge and empathy [24-27]. This re-engineered relationship with their patients must also consider some of the following factors, which are often overlooked from the organization’s, patient’s and public’s perspectives [27,28]:
- The overwhelming and extremely heavy patient load in today’s practice
- The sense of under-appreciation and insufficient recognition of the part of many doctors
- The problem of inadequate pay or renumeration, which is not uncommon
- Being asked to perform low-value work
- Lack of work-life balance
- High rate of burn-out, especially within some disciplines
For doctors to deliver optimal patient care and for them to be the best possible “drug”, as proposed by Balint, these issues will need to be addressed appropriately.
Conclusion
Medicine remains, in the words of William Osler, “a science of uncertainty and an art of probability”. A strong partnership with patients and a positive doctor-patient relationship can certainly bring on more certainties. This relationship is defined by the length (duration) of care provided, the consultation experiences and the depth of such a bond. Each new interaction is influenced by the previous experiences of both parties. In a positive match, patients will value both the clinical (physician’s professional expertise) as well as the interpersonal quality of care. [29]. In such circumstances, the positive doctor-patient relationship may even move on from “commanding to connection” and “hierarchy to humility”.
References
- Calman K. The profession of medicine. BMJ, 1974; 309: 1140-1143.
- Li J. The patient-physician relationship: Covenant or contract? Mayo Clin Proceedings, 1996; 71: 917-918.
- Epstein RM. The science of patient-centred care. J Fam Pract, 2000; 49(9): 805-807.
- Steiner-Hofbauer V, Schrank B, Holzinger A. What is a good doctor? Wien Med Wochenschr, 2018; 168915-16: 398-405.
- Dieppe P, Fussell J, Warber SL. The power of caring in clinical encounters. BMJ, 2020; 371: m4100.
- Curran J. The doctor, his patients and the illness. BMJ, 2007; 335(7627): 941.
- Ridd M, Shaw A, Lewis G, et al. The patient-doctor relationship: a synthesis of the qualitative literature on patients’ perspectives. Br J Gen Pract, 2009; 59(561): e116-e133.
- Turabian JL. The wrong transformation of the doctor-patient relationship in drug-patient relationship: From doctor himself as a drug to doctor as a drug dealer. Chronicle of Med and Surg, 2018; 2(1); 298-301.
- Hafferty FW. Beyond curriculum reform: confronting medicine’s hidden curriculum. Acad med, 1998; 73(4): 403-407.
- Lateef F, Rahman MAA. The Dynamics of Intergenerational Relations in Emergency Medicine: Issues at The Frontline. Digital J Sci, 2025; 2(5): 134.o
- Fatimah Lateef. “High Technology, High Touch: Implementing Virtual Reality Education and Ensuring the Elements of Humanism are Not Forgotten.” MAR Case Reports, 2023; 6(5): 1-16.
- Lateef F. Embedding medical students in the ED: The Teachable moments. Edu in Med J, 2015; 5: 20.
- Fatimah Lateef, Suppiah M, Too XY. High technology, High touch: implementing VR education and training and ensuring the elements of humanism are not forgotten. J Med and Research, 2022; 6(5): 1-15.
- Fatimah Lateef. Seasons of life for an emergency physician. HSOA J of Emerg Med, Trauma and Surgical care, 2024; 10: 074.
- Pellegrino ED. Educating the humanist physician: an ancient ideal reconsidered. JAMA, 1974; 227: 1288-1294.
- Wang Y, Wu Q, Wang Y, et al. The effects of physicians’ communications and empathy ability on physician-patient relationship from patients; and physicians’ perspectives. J Clin Psychol Med Settings, 2022; 28: 1-12.
- Street RL Jr, O’Malley KJ, Cooper LA, et al. Understanding the concordance in patient-physician relationships personal to ethnic dimensions of shared identity. Ann Fam Med, 2008; 6(3): 198-205.
- Lakasing E. Michael Balint: an outstanding medical life. Br J of gen Pract, 2005; 724-725, 537-542.
- Johnson AH. The Balint Movement in America. Fam Med, 2001; 33(3): 174-177.
- Balint M. The doctor, his patient and the illness. London, Putman, Watson GI: Int J of Clin Pract. 1957, pp355. https://doi.org/10.1111/j.1742-1241.1957.tb02439.
- Warnecke E. The art of communications. Aust fam Physician, 2014; 43(3): 156-158.
- Aleshchenko EA, Kashtalap VV. “Doctor as a drug” in a stroke follow up. Complex Issues of cardiovascular Diseases, 2022; 11(1): 107-111.
- Schnelle C, Jones MA. Protocol for a qualitative study on doctors’ opinion on and experiences of exceptionally good doctors. Adv Med Edu Pract, 2022; 13: 103-109.
- Fones CSL, Kua EH, Goh LG. What makes a good doctor? View of the medical profession and the public in setting priorities for medical education. SMJ, 1998; 39(12): 537-542.
- Fatimah Lateef, Yeong YQ, Galwankar S, et al. Emergency Physicians: Creating ripples, expanding domains and negotiating VUCA situations. Journal of Emergencies, Trauma and Shock, 2025; 18(2): 69-73.
- Lacy BE, Chan JL. Physician burnout: The hidden healthcare crisis. Clin gastroenterology and hepatology, 2018; 16: 311-317.
- Lee YY, Medford ARL, Sukari AH. Burnout in physicians. The Journal of The Royal Coll of Physicians of Edin, 2015; 45(2): 104-107.
- Duong D, Vogel L. Overworked healthcare workers are “part of the point of exhaustion” Canadian Med Association J, 2023; 195(8): E309-E310.
- Dorr Goold S, Lipkin M Jr. The doctor-patient relationship: challenges, opportunities and strategies. J Gen Intern Med, 1999; 14 (Suppl 1): S26-S33.

