Myocardial Infarction in Young Adults: Risk Factors, Pathophysiology, and Management Approaches
Vishakha Maheshwari1, Gurpreet Kaur Chawla2, Antony Joseph3, Surender Singh4 and Vaibhav Sharma5,*
1Department of Internal Medicine, Armed Forces Medical College, Pune, India
2Department of Internal Medicine, Himalayan Institute of Medical Sciences, Dehradun, India
3Department of Internal Medicine, MGM Medical College and Hospital, Mumbai, India
4Department of Internal Medicine, St Vincent Medical Center, Worcester, MA, USA
5Department of Internal Medicine, Medstar Washington Hospital Center, Washington, DC, USA
Received Date: 07/05/2025; Published Date: 12/06/2025
*Corresponding author: Vaibhav Sharma, M.B.B.S.; Department of Internal Medicine, Medstar Washington Hospital Center, Washington, DC, USA
Abstract
Acute myocardial infarction (AMI) in young adults (≤ 45 years) presents unique diagnostic and management hurdles. Despite a generalized reduction in the incidence of AMI in the general population, the incidence of this condition in young adults increased during the past decade. This review synthesizes recent evidence on risk factors, pathophysiologic mechanisms, diagnostic characteristics, management, and preventive interventions for AMI in young adults. Traditional cardiovascular risk factors like smoking, obesity, dyslipidemia, and family history are most relevant; however, recently recognized risk factors like lipoprotein(a) elevation, psychological stress, and substance abuse require special attention in this age group. Non-atherosclerotic causes like spontaneous coronary artery dissection (SCAD) and myocardial infarction with non-obstructive coronary arteries (MINOCA) are more common in younger patients than in older patients. Diagnostic challenges are based on atypical presentation and the selective use of traditional risk assessment modalities. Management strategies must emphasize both emergent interventions and long-term reduction of cardiovascular risk. This review emphasizes the necessity for more effective screening modalities, including lipoprotein(a) assessment, and vigorous risk factor modification in this high-risk population.
Keywords: Myocardial infarction; Young adults; Lipoprotein(a); Cardiovascular risk factors; Atherosclerosis
Introduction
Cardiovascular disease continues to dominate the cause of death worldwide with acute myocardial infarction (AMI) being a dominant contributor to its disease burden [1]. It has been thought of as an illness that traditionally affects older people; however, recent epidemiology has shown us a worrying escalation of its presence in younger populations, i.e., individuals <45 years old [2]. This change of demographics poses real challenges to our current paradigms of cardiovascular risk assessment and intervention.
Young AMI patients pose special management and diagnostic challenges because of atypical presentation, special risk factors, and possibly varied pathophysiological mechanisms of the disease [3]. The long-term burden of early-onset coronary artery disease is significant, with possible effects on quality of life, economic productivity, and healthcare resource use [4]. Young adults with AMI are, nevertheless, a less-researched group.
This mini-review is intended to integrate existing evidence regarding epidemiology, risk factors, pathophysiological mechanisms, diagnostic strategies, management, and preventive strategies for AMI in young adults. By targeting this particular age group, we can increase clinical awareness and optimize outcomes in this vulnerable population.
Epidemiology
The epidemiology of AMI in young adults shows impressive trends. Although the overall rate of AMI has reduced in developed nations over the last few decades with better primary prevention and control of risk factors, the percentage of AMI in young adults has risen [2]. US-based data have shown that about 10% of AMI is seen in patients less than 45 years of age, with a higher percentage of males (male: female ratio is around 4:1) [3]. But this gender disparity diminishes with increasing age, especially in young adults (those younger than 35 years) [3].
Recent data suggest that the incidence of acute myocardial infarction (AMI) in young women may be increasing at a higher rate than in their male peers, potentially reflective of changing risk factor profiles and underdiagnosis in females [5]. A large trend study of AMI hospitalizations in young adults aged 35-54 from 2001 through 2022 showed a 2% per year increase in this age category, in contrast to declining incidence in older age categories [1].
Risk Factors
Traditional Risk Factors
Traditional cardiovascular risk factors are a leading cause of AMI in young adults, but with different relative contributions compared to older age groups (Table 1). Smoking remains highly linked and has a high relative contribution, and figures of up to 70% of young AMI patients being current smokers have been cited [6]. Smoking promotes atherosclerosis through multiple mechanisms: endothelial dysfunction, enhanced platelet aggregation, and increased inflammation [7].
Dyslipidemia, especially elevated LDL-C, is another modifiable risk factor that is significant. Premature familial CAD is also significantly more frequent in young AMI patients than in elderly patients, which suggests strong genetic influences [8].
Metabolic risk factors have gained prominence among young adults. The rising prevalence of obesity and diabetes mellitus type 2 (T2DM) among adolescents is paralleled by the rising prevalence of AMI among adolescents [9]. Obesity promotes systemic inflammation and endothelial dysfunction, which accelerates the progression of atherosclerosis [10], while early-onset T2DM puts adolescents at risk for extended exposure to hyperglycemia, markedly elevating cardiovascular morbidity [11].
Novel and Emerging Risk Factors
Apart from classical risk factors, certain new and emerging risk markers have particular use in young adults with AMI (Table 1).
Raised lipoprotein(a) [Lp(a)] is currently recognized as a key independent risk factor for AMI in young people. Investigations have established that nearly 1 out of 3 young people with AMI have normal LDL but raised Lp(a) (>80th percentile, about 125 nmol/L) [12]. In contrast to other conventional risk factors, the levels of Lp(a) are under genetic control and are relatively stable over a lifetime, and therefore early detection is highly worthwhile [13].
Substance abuse is another critical determinant in young adults. Cocaine and methamphetamine abuse can provoke AMI through coronary vasospasm, increased platelet aggregation, and heightened myocardial oxygen demand [14]. Cannabis abuse has been linked with heightened cardiovascular events in younger age groups, though the mechanisms behind it remain partly unclear [14].
Psychosocial determinants such as depression, anxiety, and chronic stress are found to have more significant relations to AMI among younger than older adults [15]. They may have direct pathophysiologic effects via the neuroendocrine and inflammatory pathways and indirectly via harmful health behaviors [15].
Table 1: Risk Factors for Myocardial Infarction in Young Adults.
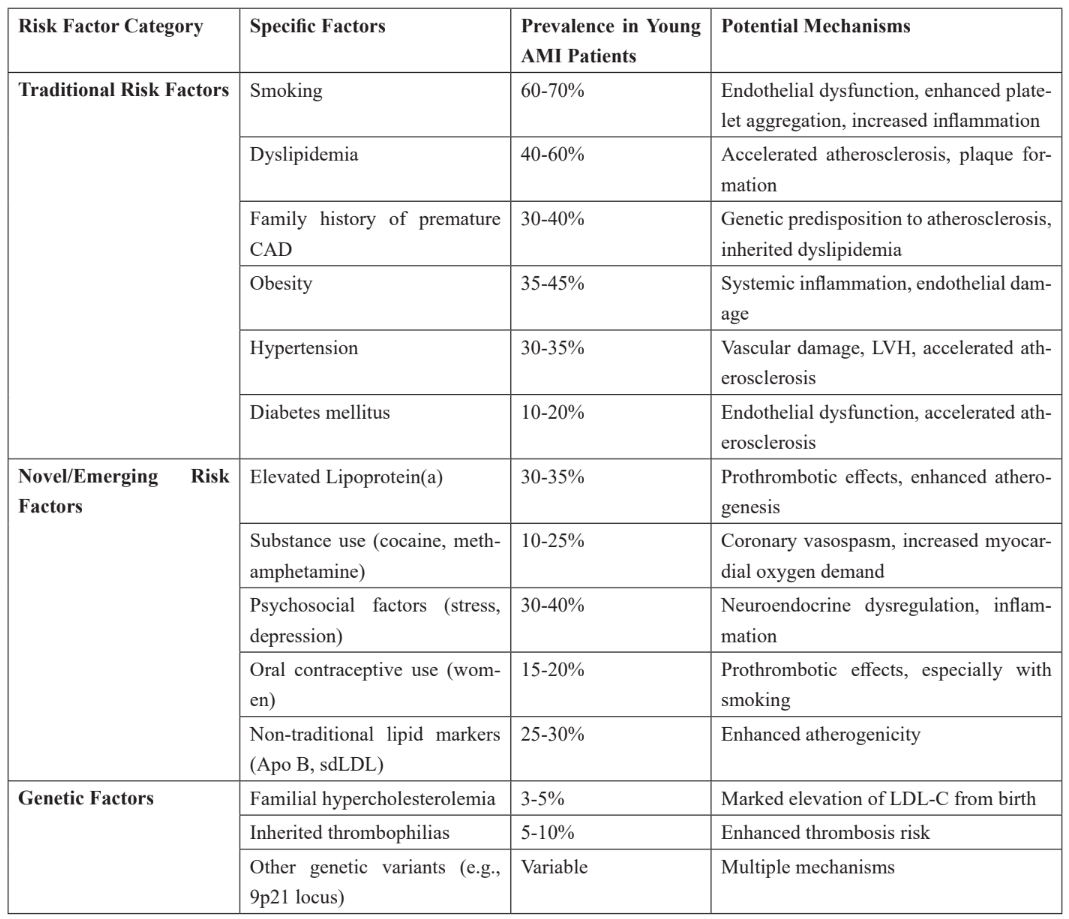
CAD: Coronary artery disease; LVH: Left ventricular hypertrophy; Apo B: Apolipoprotein B; sdLDL: Small dense LDL particles
Pathophysiological Mechanisms
The pathophysiology of AMI in young adults encompasses both atherosclerotic and non-atherosclerotic mechanisms, with several distinctive features compared to older populations.
Atherosclerotic Mechanisms
Atherosclerotic plaque rupture is still the most frequent mechanism of AMI in young adults, just like in older adults [16]. Atherosclerotic disease in young adults, though, can be of a different character, with increased single-vessel disease and left anterior descending artery dominance [4]. Young patients' plaques are more likely to contain larger lipid cores and thinner fibrous caps, which may make them susceptible to rupture even with lower overall plaque burden [4].
Atherosclerosis in young adults is promoted by a number of factors. Smoking is especially favorable to atherogenesis by oxidative stress, inflammation, and endothelial dysfunction [7]. Obesity at a young age promotes systemic inflammation and insulin resistance, whereas early-onset T2DM promotes vascular damage by a number of mechanisms such as advanced glycation end products, oxidative stress, and disrupted vascular repair mechanisms [11].
Non-atherosclerotic Mechanisms
Non-atherosclerotic etiologies of AMI are increasingly relatively more significant in young adults than in elderly populations (Figure 1). Spontaneous coronary artery dissection (SCAD) is responsible for up to 35% of AMI in women under the age of 50 years, with extremely high frequency in peripartum women [17]. SCAD results from spontaneous dissociation of layers of the coronary artery, which forms a false lumen that compresses the true lumen and compromises coronary flow [17].
Myocardial infarction with non-obstructive coronary arteries (MINOCA) is an emerging entity in young adults, occurring in approximately 10-15% of acute myocardial infarction (AMI) presentations in this age group [18]. MINOCA involves a variety of pathophysiological mechanisms, such as coronary vasospasm, coronary microvasculature dysfunction, coronary thromboembolism, and myocarditis [18].
Other less common but important mechanisms in young adults are coronary anomalies, coronary vasculitis associated with systemic inflammatory processes, and thrombophilias [3]. Substance-related AMI, that is, cocaine- and methamphetamine-induced, primarily occurs in young patients and results from mechanisms like severe coronary vasospasm, enhanced platelet aggregation, and accelerated atherosclerosis [14].
Diagnostic Considerations
Young adults' diagnosis of AMI has some specific challenges. Younger patients more often have atypical presentation, which may result in diagnostic delays [5]. It has been described that 30% of young adults with AMI may not have typical chest pain, and atypical presentations such as isolated dyspnea, epigastric pain, or severe fatigue are more frequent, especially in women [5].
Traditional diagnostic methods continue to play a central role in AMI diagnosis in young adults. Serial 12-lead ECGs have been shown to enhance diagnostic sensitivity, especially in those with initially non-diagnostic ECGs [19]. Their sensitivity for MI, however, is still poor (AUC 0.55 vs. 0.83 for troponin) [20]. High-sensitivity cardiac troponin assays have transformed AMI diagnosis, and serial measurements (baseline and 3-6 hours later) have been shown to be highly accurate for ruling in and ruling out MI [21].
Coronary angiography is still the gold standard for definitive diagnosis and directs future management. The diagnostic strategy must be extended in young adults to include additional investigation where necessary, especially when mechanisms other than atherosclerotic are being evaluated. Intravascular imaging (intravascular ultrasound or optical coherence tomography) can identify SCAD, plaque morphology, and other mechanisms not visible on standard angiography [17].
Cardiovascular magnetic resonance (CMR) imaging is now an obligatory method, especially in the event of suspected MINOCA, since it enables the diagnosis of myocarditis, stress cardiomyopathy, and microvascular dysfunction [18]. In some situations, computed tomography coronary angiography (CTCA) can be useful, primarily in the diagnosis of coronary anomalies [3].
Management Approaches
Acute Management
Acute treatment of AMI in young adults is typically in keeping with standard guidelines for the overall population, but with some particular considerations. Primary PCI remains the ideal reperfusion therapy for STEMI if feasible within guideline-recommended time frames [16]. For NSTEMI, early invasive management is typically preferable with the extended life expectancy and potential for progression of disease [16].
There are significant management subtleties to specific etiologies. In SCAD, a conservative strategy is preferable when possible because PCI in SCAD has greater technical failure and complication rates than in atherosclerotic disease [17]. Medical therapy, such as dual antiplatelet therapy, statins, beta-blockers, and angiotensin-converting enzyme inhibitors/angiotensin receptor blockers, must be tailored to the particular mechanism of AMI and patient factors [16].
Long-term Management and Secondary Prevention
Long-term care is focused on active secondary prevention because the exposure to risk factors is prolonged, and guideline-directed medical therapy (GDMT) is the drug treatment of choice [16]. However, medication compliance is a complex problem in young adults, and studies have shown that younger patients are more prone to early discontinuation of secondary prevention therapy [22].
Marked risk factor reduction is required, with particular emphasis on smoking cessation, which can reduce recurrent MI risk by up to 50% within one year [7]. Lipid modification must involve marked LDL-C reduction, with high-intensity statin therapy being recommended in the majority of young post-MI individuals [23]. In those with elevated Lp(a), novel drugs aimed at this lipoprotein are potentially beneficial, but clinical outcome data are yet to emerge [13].
Cardiac rehabilitation is especially beneficial in young AMI patients, focusing on long-term lifestyle modification, psychosocial issues, and enhancing long-term outcomes [22]. The mode of delivery can be changed in the young, and mobile and digital health-based interventions have been shown to be promising in them [22].
Table 2: Key Management Considerations for AMI in Young Adults.
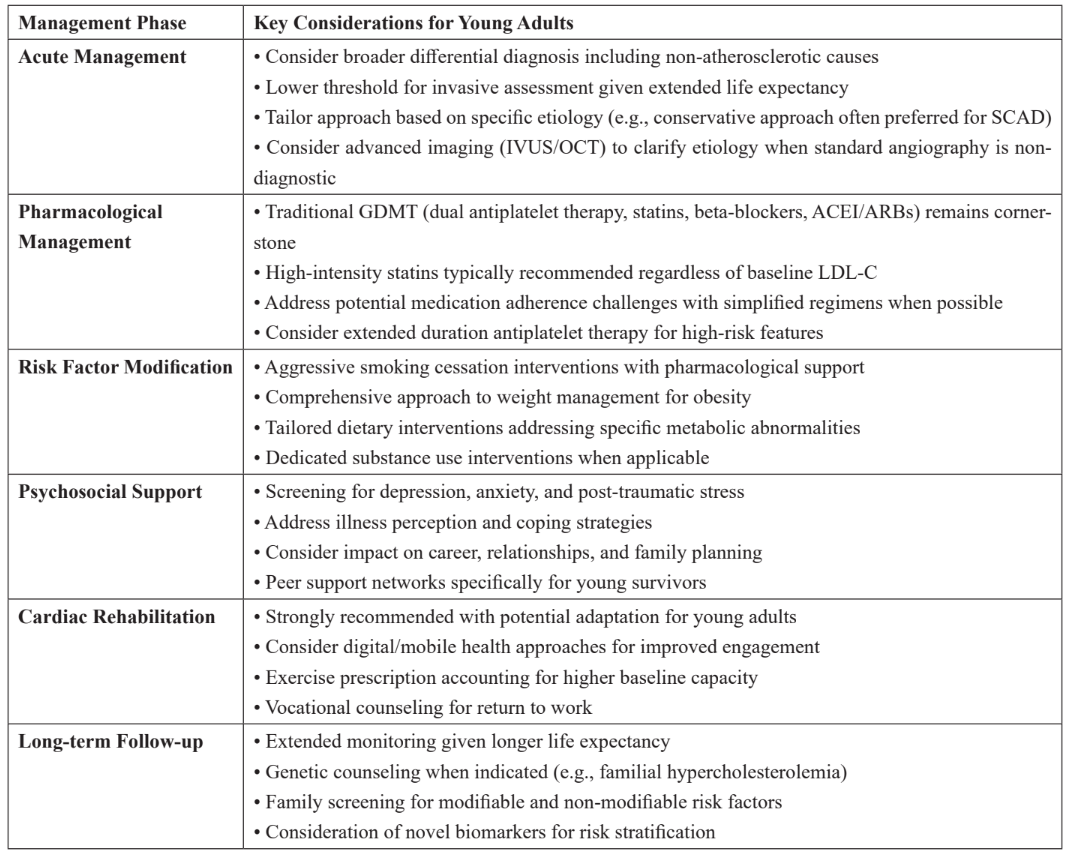
SCAD: Spontaneous coronary artery dissection; IVUS: Intravascular ultrasound; OCT: Optical coherence tomography; GDMT: Guideline-directed medical therapy; ACEI: Angiotensin-converting enzyme inhibitor; ARB: Angiotensin receptor blocker; LDL-C: Low-density lipoprotein cholesterol
Risk Assessment and Prevention
Risk Assessment
Older conventional risk prediction measures like the Pooled Cohort Equations fall significantly short in young adults [23]. They underperform below the actual risk in young adults with strong risk factors because age significantly affects the algorithms [23]. Additionally, they fail to include strong young adult risk factors like premature CAD family history or high Lp (a).
Better methods to evaluate risks to young adults are:
- Earlier and more extensive screening for familial hypercholesterolemia and other genetic conditions in patients with family history of premature CAD [8].
- Lp(a) measurement in young patients with a history of premature CAD despite normal LDL-C levels [12]. Measurement of Lp(a) in young patients with familial CVD or with high modifiable risk factors despite low atherosclerotic cardiovascular disease (ASCVD) scores, according to the National Heart, Lung, and Blood Institute (NHLBI) [24].
- The evaluation of atypical lipid markers, such as apolipoprotein B, can provide more sophisticated risk stratification in young adults than standard lipid profiles [13].
- Coronary artery calcium (CAC) scoring in well-selected young adults with intermediate risk or positive family history, though the utility is less well established in older adults [23].
Prevention Strategies
Primary prevention in young adults must be tailored to early detection and control of modifiable risk factors. Current American Diabetes Association (ADA) and American College of Cardiology/American Heart Association (ACC/AHA) guidelines suggest risk-based dysglycemia screening in overweight adolescents [11] and 4-6 yearly ASCVD risk estimation in adults aged 20-39 years, with a focus on HbA1c, lipid profile, and lifestyle counseling [25].
Lifestyle change is the cornerstone of prevention, with specific focus on:
- Tobacco prevention and quitting, with special programs directed at young people and young adults [7].
- Prevention of obesity by early interventions in life for both diet and physical activity [10].
- Early treatment and detection of hypertension and dyslipidemia, which remain undetected in young adults [25].
- Mental health care and stress management strategies, embracing the role of psychosocial factors towards cardiovascular risk [15].
Pharmacological preventive treatments are required to weigh possible benefit against a lifetime on medication. Young adults with risk factors and increased LDL-C, however, have statin treatment justified even in low 10-year risk scores, especially in the presence of very high lifetime risk [23].
For young women, hormonal contraceptive options must consider cardiovascular risk, with particular care in those with several risk factors, especially smoking [5]. Pregnancy-related cardiovascular risk must be addressed by pre-conception counseling and management of modifiable risk factors [5].
Future Directions
Some promising new areas have the potential for enhancing outcomes among young adults with AMI:
- Sophisticated risk prediction technology using genetic markers, new biomarkers, and artificial intelligence tools can enhance young adult risk stratification [8].
- Mechanism-targeted therapy, such as Lp(a)-lowering therapies (antisense oligonucleotides and small interfering RNA) in clinical trials [13].
- Precision medicine strategies take into account individual genetic, metabolic, and environmental variations to customize preventive and therapeutic measures [8].
- Improved screening strategies, possibly involving polygenic risk assessments, would attempt to detect high-risk individuals who could be benefited by more intensive and aggressive preventive treatments [8].
- These are applied for ongoing monitoring and management of risk factors, especially with relevance and utility for young populations [22].
Conclusion
AMI in young adults is a distinct clinical entity with distinct risk factors, pathophysiologic mechanisms, and management questions. The increasing prevalence in this age group emphasizes the importance of increased risk assessment and aggressive prevention. Elevated Lp(a) is a highly relevant risk factor in young adults and suggests potential benefit from prolonged screening. Management needs to address both acute and chronic cardiovascular issues, with particular attention to psychosocial factors and drug compliance. Future research needs to be directed toward the creation of more effective risk assessment tools, targeted therapeutic regimens, and prevention strategies specifically for young adults at risk of premature coronary artery disease.
Fundings: Nil
Disclosures: Nil
Conflicts of interest: Nil
References
- Virani SS, Alonso A, Aparicio HJ, Benjamin EJ, Bittencourt MS, Callaway CW, et al. Heart disease and stroke statistics, 2021.
- Arora S, Stouffer GA, Kucharska-Newton AM, Qamar A, Vaduganathan M, Pandey A, et al. Twenty-year trends and sex differences in young adults hospitalized with acute myocardial infarction: the ARIC Community Surveillance Study. Circulation, 2019; 139(8): 1047-1056.
- Singh A, Collins BL, Gupta A, Fatima A, Qamar A, Biery D, et al. Cardiovascular risk and statin eligibility of young adults after an MI: partners YOUNG-MI registry. Journal of the American College of Cardiology, 2018; 71(3): 292-302.
- Shah N, Kelly AM, Cox N, Wong C, Soon K. Myocardial infarction in the “young”: risk factors, presentation, management and prognosis. Heart, lung and circulation, 2016; 25(10): 955-960.
- Arora S, Stouffer GA, Kucharska-Newton AM, Qamar A, Vaduganathan M, Pandey A, et al. Twenty-year trends and sex differences in young adults hospitalized with acute myocardial infarction: the ARIC Community Surveillance Study. Circulation, 2019; 139(8): 1047-1056.
- Gulati R, Behfar A, Narula J, Kanwar A, Lerman A, Cooper L, et al. Acute myocardial infarction in young individuals. InMayo Clinic Proceedings, 2020; 95(1): pp. 136-156.
- Klein J, Diaba-Nuhoho P, Giebe S, Brunssen C, Morawietz H. Regulation of endothelial function by cigarette smoke and next-generation tobacco and nicotine products. Pflügers Archiv-European Journal of Physiology, 2023; 475(7): 835-844.
- Khera AV, Chaffin M, Aragam KG, Haas ME, Roselli C, Choi SH, et al. Genome-wide polygenic scores for common diseases identify individuals with risk equivalent to monogenic mutations. Nature genetics, 2018; 50(9): 1219-1224.
- Antza C, Gallo A, Boutari C, Ershova A, Gurses KM, Lewek J, et al. Prevention of cardiovascular disease in young adults: Focus on gender differences. A collaborative review from the EAS Young Fellows. Atherosclerosis, 2023; 384: 117272.
- Wong ND, Sattar N. Cardiovascular risk in diabetes mellitus: epidemiology, assessment and prevention. Nature Reviews Cardiology, 2023; 20(10): 685-695.
- Misra S, Ke C, Srinivasan S, Goyal A, Nyriyenda MJ, Florez JC, et al. Current insights and emerging trends in early-onset type 2 diabetes. The Lancet Diabetes & Endocrinology, 2023; 11(10): 768-782.
- Berman AN, Biery DW, Singh A, Wu WY, Divakaran S, DeFilippis EM, et al. Atherosclerotic cardiovascular disease risk and elevated lipoprotein (a) among young adults with myocardial infarction: The Partners YOUNG-MI Registry. European journal of preventive cardiology, 2021; 28(8): e12-14.
- Tada H, Nohara A, Kawashiri MA. Serum triglycerides and atherosclerotic cardiovascular disease: insights from clinical and genetic studies. Nutrients, 2018; 10(11): 1789.
- DeFilippis EM, Singh A, Divakaran S, Gupta A, Collins BL, Biery D, et al. Cocaine and marijuana use among young adults with myocardial infarction. Journal of the American College of Cardiology, 2018; 71(22): 2540-2551.
- Kivimäki M, Steptoe A. Effects of stress on the development and progression of cardiovascular disease. Nature Reviews Cardiology, 2018; 15(4): 215-229.
- Rao SV, O’Donoghue ML, Ruel M, Rab T, Tamis-Holland JE, Alexander JH, et al. 2025 ACC/AHA/ACEP/NAEMSP/SCAI guideline for the management of patients with acute coronary syndromes: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation, 2025; 151(13): e771-862.
- Hayes SN, Kim ES, Saw J, Adlam D, Arslanian-Engoren C, Economy KE, et al. Spontaneous coronary artery dissection: current state of the science: a scientific statement from the American Heart Association. Circulation, 2018; 137(19): e523-557.
- Tamis-Holland JE, Jneid H, Reynolds HR, Agewall S, Brilakis ES, Brown TM, et al. Contemporary diagnosis and management of patients with myocardial infarction in the absence of obstructive coronary artery disease: a scientific statement from the American Heart Association. Circulation, 2019; 139(18): e891-908.
- Amsterdam EA, Wenger NK, Brindis RG, Casey DE, Ganiats TG, Holmes DR, et al. 2014 AHA/ACC guideline for the management of patients with non–ST-elevation acute coronary syndromes: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Journal of the American college of cardiology, 2014; 64(24): e139-228.
- Riley RF, Miller CD, Russell GB, Soliman EZ, Hiestand BC, Herrington DM, et al. Usefulness of Serial 12-Lead Electrocardiograms in Predicting 30-Day Outcomes in Patients with Undifferentiated Chest Pain (the ASAP CATH Study). The American journal of cardiology, 2018; 122(3): 374-380.
- Sandoval Y, Smith SW, Thordsen SE, Bruen CA, Carlson MD, Dodd KW, et al. Diagnostic performance of high sensitivity compared with contemporary cardiac troponin I for the diagnosis of acute myocardial infarction. Clinical chemistry, 2017; 63(10): 1594-1604.
- Zeitouni M, Nanna MG, Sun JL, Chiswell K, Peterson ED, Navar AM. Performance of guideline recommendations for prevention of myocardial infarction in young adults. Journal of the American College of Cardiology, 2020; 76(6): 653-664.
- Arnett DK, Blumenthal RS, Albert MA, Buroker AB, Goldberger ZD, Hahn EJ, et al. 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Journal of the American College of cardiology, 2019; 74(10): e177-232.
- Al Abid SU, Monower MM, Abrar AK, Riva JA, Bhuiyan MR, Al-Mamun MA, et al. Burden and Predictors of Statin Use for Primary and Secondary Prevention of Cardiovascular Disease in Bangladesh: Evidence from a Nationally Representative Survey. Global Heart, 2025; 20(1): 28.
- Yandrapalli S, Nabors C, Goyal A, Aronow WS, Frishman WH. Modifiable risk factors in young adults with first myocardial infarction. Journal of the American College of Cardiology, 2019; 73(5): 573-584.

