Gallbladder Agenesis: A Case Report and Review of the Literature
Essaidi Zakaria1, Benzidane Kamal1,*, Kabir Mohamed Amine1, Bouali Ichrak1, Ettaoussi Abdelhak1, Majd Abdessamad1, Kamal Khadija1, Bouali Mounir1, Elbakouri Abdelillah1, Khaleq Khalid2 and El Hattabi Khalid1
1Department of General surgery, Faculty of Medicine and Pharmacy, Ibn Rochd University Hospital Center, Hassan II University, Casablanca, Morocco
2Department of Anesthesia and Resuscitation, Faculty of Medicine and Pharmacy, Ibn Rochd University Hospital Center, Hassan II University, Casablanca, Morocco
Received Date: 10/02/2026; Published Date: 24/04/2026
*Corresponding author: Benzidane Kamal, Department of General surgery, Faculty of Medicine and Pharmacy, Ibn Rochd University Hospital Center, Hassan II University, Casablanca, Morocco
Abstract
Background: Gallbladder Agenesis (GA) is an extremely rare congenital anomaly of the biliary system, with an estimated incidence ranging from 0.01% to 0.06%. It results from a developmental failure of the embryonic hepatic diverticulum and manifests in approximately one-third of cases with symptoms mimicking biliary lithiasis.
Case presentation: We report the case of a 52-year-old woman with a history of psychotic disorders who presented with right upper quadrant pain, jaundice, and signs of sepsis. Abdominal ultrasonography and computed tomography revealed dilatation of the bile ducts without visualization of the gallbladder, associated with a subhepatic collection suggesting a perforated acute cholecystitis. During surgical exploration, the gallbladder could not be identified despite extensive dissection. Two large stones were found in the common bile duct and removed, followed by external biliary drainage.
Postoperative Magnetic Resonance Cholangiopancreatography (MRCP) and T-tube cholangiography confirmed the complete absence of the gallbladder and cystic duct, thus establishing the diagnosis of gallbladder agenesis.
Discussion: This case highlights the diagnostic challenge posed by gallbladder agenesis, a rare but clinically significant condition. MRCP remains the imaging modality of choice when the gallbladder is not visualized on initial imaging studies. Awareness of this anomaly is essential to avoid hazardous dissections and iatrogenic bile duct injuries.
Conclusion: When the gallbladder is not visualized on imaging, gallbladder agenesis should always be considered. Early recognition and appropriate imaging—particularly MRCP—can prevent unnecessary surgical procedures and improve patient safety.
Keywords: Gallbladder agenesis; MRCP (biliary MRI); Biliary tract anomalies; Cholangitis; Biliary surgery
Introduction
Gallbladder agenesis (GA) is defined as the complete congenital absence of the gallbladder and cystic duct. It results from a developmental failure of the embryonic hepatic diverticulum occurring between the fourth and fifth weeks of gestation [1,2].
Its incidence is very low, estimated between 0.01% and 0.06% in the general population [3]. Most cases are discovered incidentally; however, approximately one-third of patients present with symptoms mimicking gallstone disease [4].
Preoperative diagnosis remains challenging, as ultrasonography may be misleading, suggesting an atrophic or scleroatrophic gallbladder.
Magnetic resonance cholangiopancreatography (MRCP) is the key diagnostic modality, allowing confirmation of gallbladder absence and helping to avoid unnecessary surgical intervention [5,6].
We report a typical case of gallbladder agenesis discovered intraoperatively and provide a review of the literature focusing on embryology, radiological diagnosis, operative pitfalls, and appropriate management.
Case Report
A 52-year-old woman, followed for psychotic disorders since 1989, was admitted to the emergency department for right hypochondrial and epigastric pain evolving over 10 days, with worsening symptoms during the two days prior to admission. The pain became more intense and was associated with cholestatic jaundice, occurring in a context of feverish sensations and deterioration of general condition.
On clinical examination, the patient was conscious, hemodynamically and respiratory stable, febrile at 38.7°C, with conjunctival jaundice. Abdominal examination revealed a positive Murphy’s sign, while the remainder of the abdomen was soft.
Abdominal ultrasonography showed a liver of normal size and regular contours, with a well-defined, oblong, anechoic, non-vascularized subcapsular lesion in the left lobe, measuring approximately 72.3 × 15.7 mm. There was marked dilatation of the intrahepatic bile ducts and the common bile duct, with an anteroposterior diameter of 15.9 mm measured at the hepatic hilum, without clearly identifiable obstruction. The gallbladder was not visualized. No significant intraperitoneal fluid collection was detected.
Computed tomography of the abdomen revealed two large stones within the common bile duct, responsible for upstream dilatation of the intrahepatic bile ducts. The gallbladder was not visualized. A lentiform subcapsular fluid collection exerting scalloping on segment IV was noted, measuring 60 × 30 mm, associated with marked fat stranding around the lesion and the gallbladder bed. The liver was of normal volume with regular contours and no focal lesions. Minimal perihepatic fluid was present, with mild thickening of the peritoneal layers.
Overall, the CT findings suggested a subhepatic collection related to a perforated or scleroatrophic gallbladder, complicated by common bile duct lithiasis.
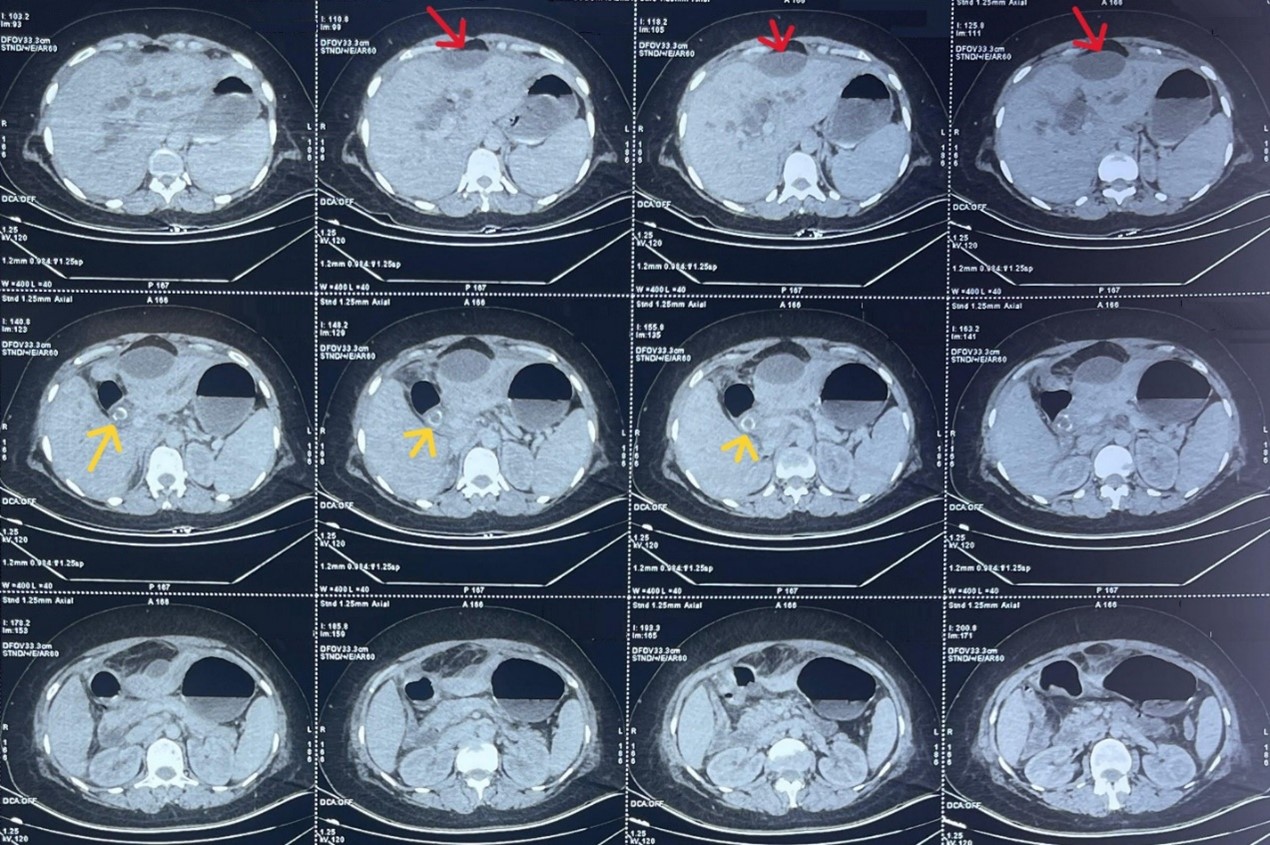
Figure 1: Computed tomography image showing a subhepatic fluid collection (red arrow) and stones within the common bile duct (yellow arrow).
From a biological standpoint, laboratory investigations revealed anemia with a hemoglobin level of 8.5 g/dL, hypochromic and microcytic in nature, leukocytosis of 14,850/mm³ with neutrophil predominance, and a markedly elevated C-reactive protein level of 411 mg/L. Cholestatic parameters were abnormal, with total bilirubin at 71 mg/L, conjugated bilirubin at 53 mg/L, unconjugated bilirubin at 18 mg/L, gamma-glutamyl transferase (GGT) at 205 U/L, and alkaline phosphatase at 384 U/L. Liver enzymes were within normal limits (AST 80 U/L, ALT 39 U/L), and serum lipase was normal at 16 IU/L.
Given the clinical presentation suggestive of localized biliary peritonitis, the patient was taken emergently to the operating room. Abdominal access was achieved through a right subcostal incision. Surgical exploration revealed dense colohepatic, omentohepatic, and gastrohepatic adhesions. Laborious adhesiolysis exposed a collection of approximately 200 mL of infected bile, which was aspirated and evacuated. The common bile duct was markedly dilated to 3 cm and contained two large stones, with a thickened and inflamed wall. The gallbladder could not be clearly identified due to advanced inflammatory changes in the subhepatic region, making further dissection hazardous.
The operative procedure consisted of extraction of the common bile duct stones followed by drainage using a T-tube (Kehr drain). Subhepatic lavage with saline solution was performed, along with pre- and retro-pedicular drainage using two Delbet drains, subhepatic drainage with a Redon drain, and interhepato-diaphragmatic drainage using a Salem tube.
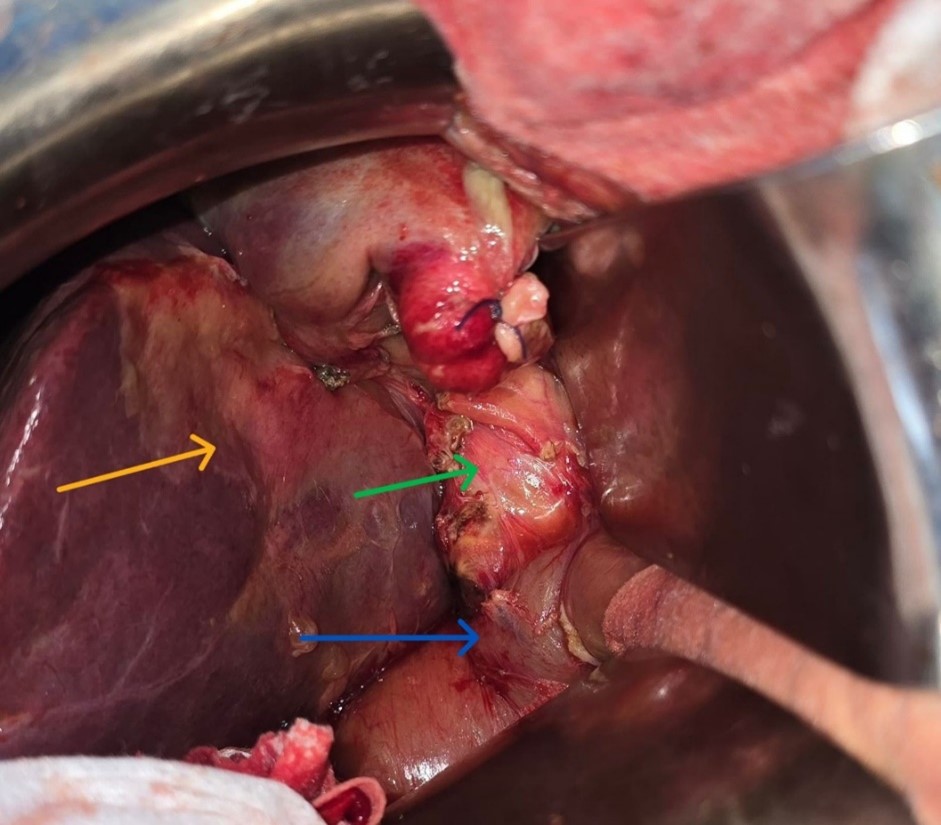
Figure 2: Intraoperative view demonstrating absence of the gallbladder (gallbladder fossa, yellow arrow), a dilated common bile duct (green arrow), and the duodenum (blue arrow).
Postoperative Course
Postoperatively, the Kehr T-tube drained approximately 400 mL of bile per 24 hours.
The subhepatic Redon drain and the interhepato-diaphragmatic Salem tube drained small amounts of serohematic fluid and were removed on postoperative day 3.
The pre- and retro-pedicular Delbet drains initially returned serous fluid; from postoperative day 6, they drained approximately 30 mL of bile per 24 hours for five days, followed by minimal biliary output and spontaneous closure of the fistula. The Delbet drains were removed on postoperative day 20.
From a therapeutic standpoint, the patient received intravenous antibiotic therapy (ceftriaxone and metronidazole) for five days, followed by oral antibiotics for 15 days, along with thromboprophylaxis and gastric protection.
A series of imaging studies was performed to investigate the presence of the gallbladder.
Magnetic Resonance Cholangiopancreatography (MRCP)
The liver was of normal size and regular contours. Multiple (at least seven) rounded, well-defined nodular lesions were identified in segments V, VII, and VIII, appearing hypointense on T1-weighted images and hyperintense on T2-weighted images, with diffusion restriction and peripheral enhancement after gadolinium administration. The largest lesion was located in segment VII and measured 14 × 11 mm.
The gallbladder was not visualized, either in its anatomical bed or in an ectopic location. The common hepatic duct was dilated to 10 mm, with marked wall thickening and intense enhancement following gadolinium injection. Moderate dilatation of the intrahepatic bile ducts was noted. Aerobilia was present within the common hepatic duct and intrahepatic bile ducts, producing focal signal voids in certain areas. There was no dilatation of the common bile duct or the main pancreatic duct.
The Kehr T-tube was visualized within the common bile duct, extending to the level of the biliary confluence. The distal tips of the Redon drains were identified in the perihepatic region (adjacent to segment VIII) and in the subhepatic space (adjacent to segment III).
The pancreas was enlarged, predominantly at the head (anteroposterior diameter of 35 mm), with loss of normal lobulation and homogeneous enhancement after gadolinium administration, consistent with a reactive appearance (normal serum lipase). Diffuse infiltration of the mesenteric fat was observed both above and below the mesocolon. No significant peripancreatic fluid collection was identified.
A small amount of intraperitoneal fluid was present in the perihepatic and perisplenic regions, as well as within the paracolic gutters.
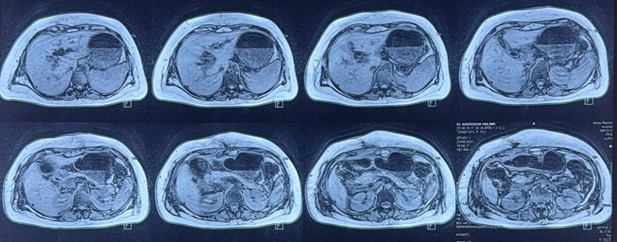
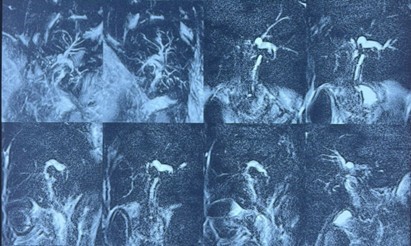
Figure 3: MRCP showing multiple nodular lesions located in hepatic segments V, VII, and VIII, with absence of gallbladder visualization in the gallbladder fossa.
T-tube Cholangiography
No calcified opacity was identified projecting over the hepatic area. Surgical drainage tubes were visualized in the subhepatic region. Digestive gas was present.
Following opacification with iodinated contrast medium injected through the Kehr T-tube, the T-tube was confirmed to be in place. Mild dilatation of the proximal right and left intrahepatic bile ducts was observed, containing a few filling defects consistent with aerobilia. There was slight dilatation of the common bile duct, without any clearly identifiable obstructive lesion. The gallbladder and cystic duct were not visualized. Contrast medium passed freely into the duodenum, with no evidence of contrast extravasation.
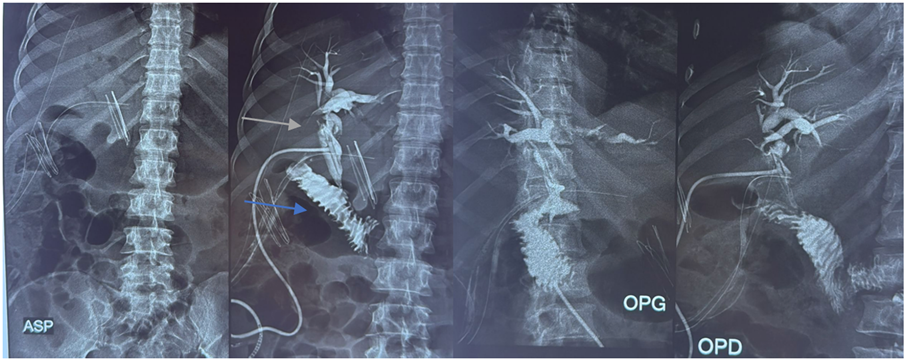
Figure 4: T-tube cholangiography demonstrating adequate opacification of the biliary tree with free passage of contrast into the duodenum, but without visualization of the gallbladder. Dilated common bile duct with visualization of the Kehr T-tube (green arrow) and the duodenum (blue arrow).
In view of the imaging findings confirming gallbladder agenesis and their concordance with postoperative exploration, the patient was discharged on postoperative day 21 and subsequently reviewed on day 28 for removal of the Kehr T-tube.
Discussion
1. Embryology and Epidemiology
Gallbladder agenesis (GA) is related to an embryological developmental anomaly resulting from the failure of differentiation of the cystic bud from the hepatic diverticulum. This defect occurs at a very early stage of embryogenesis, explaining the complete absence of both the gallbladder and the cystic duct [1,2].
The incidence of this malformation remains very low, estimated between 0.01% and 0.06% according to published series [3,4]. A clear female predominance has been reported, and the condition is most often diagnosed in adulthood, typically between 40 and 60 years of age [5].
Most cases are asymptomatic; however, approximately 30% of patients present with symptoms suggestive of cholecystitis or cholangitis [4,6].
2. Imaging and Diagnosis
Ultrasonography is the first-line imaging modality but may be misleading. The gallbladder may appear “contracted” or “scleroatrophic,” and acoustic shadows may be misinterpreted as gallstones. When the gallbladder is not visualized, gallbladder agenesis should be considered, and further investigations are warranted.
Computed tomography confirms biliary dilatation but does not consistently allow visualization of the cystic duct.
Magnetic resonance cholangiopancreatography (MRCP) is the reference imaging modality. It enables detailed mapping of the biliary tree, confirms the absence of the gallbladder, and allows the search for an ectopic gallbladder (intrahepatic, retroduodenal, retropancreatic, or left-sided locations) [5,7].
Hepatobiliary scintigraphy may demonstrate non-visualization of the gallbladder; however, this finding is nonspecific and must be interpreted cautiously [8].
Accordingly, the recommended diagnostic algorithm is as follows:
- Initial ultrasonography;
- If the gallbladder is not visualized or findings are equivocal → MRCP;
- If gallbladder agenesis is confirmed → conservative management;
- If discovered intraoperatively → cautious exploration and postoperative imaging confirmation.
3. Diagnostic Pitfalls and Operative Difficulties
The main diagnostic pitfall is confusion with a scleroatrophic gallbladder. This error may lead to extensive dissection of the hepatic pedicle and significantly increase the risk of bile duct injury [9].
When the gallbladder cannot be identified intraoperatively, further dissection should be avoided. The recommended strategy follows the principles of “Safe Cholecystectomy” as defined by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) [10], including achievement of the Critical View of Safety, performance of intraoperative cholangiography when feasible, or a reasoned bail-out strategy in cases of uncertain anatomy.
In our case, the surgeon opted to drain and manage the common bile duct without attempting to identify the gallbladder, thereby avoiding a potentially major biliary injury.
4. Management and Outcome
When diagnosed prior to any surgical intervention, gallbladder agenesis does not require surgery. Management is conservative and symptomatic, targeting functional biliary pain, sphincter of Oddi dysfunction, or common bile duct stones when present.
In cases diagnosed intraoperatively, management should prioritize safety, including biliary drainage, stone extraction if necessary, and subhepatic lavage. Postoperative MRCP confirms the diagnosis and allows appropriate follow-up [11].
The clinical outcome is generally favorable, and no additional treatment is required in most cases [12].
5. Review of the Literature
Recent publications confirm both the rarity of gallbladder agenesis and the diagnostic challenges it presents.
- Tagliaferri et al. (2017) proposed an imaging-based diagnostic algorithm to avoid unnecessary surgery [5].
- Bianco et al. (2018) demonstrated a marked female predominance and a surgical incidence below 0.03% [4].
- Piltcher-da-Silva et al. (2022) emphasized the decisive role of MRCP in confirming the diagnosis [6].
- Wei et al. (2024) reported a pediatric case, with MRI images clearly illustrating the absence of both the gallbladder and the cystic duct [3].
All these studies converge on the same conclusion: MRCP is the imaging modality of reference, and gallbladder agenesis should be systematically considered when the gallbladder is not visualized.
6. Application to Our Case
Our case is consistent with these findings. Preoperative imaging revealed biliary dilatation without gallbladder visualization; the gallbladder remained unidentifiable intraoperatively; and postoperative confirmation by MRCP and cholangiography established a definitive diagnosis of gallbladder agenesis.
The cautious surgical approach adopted avoided bile duct injury and allowed a favorable clinical outcome.
7. Perspectives
Gallbladder agenesis remains a rare diagnosis of exclusion.
Advances in imaging techniques, including high-field MRI and endoscopic ultrasound, may improve early detection.
Increased awareness among radiologists and surgeons is essential to reduce unnecessary invasive explorations.
Conclusion
Gallbladder agenesis is an exceptional congenital malformation but one that is crucial to recognize. It may mimic gallstone disease and lead to unnecessary surgical intervention.
When the gallbladder is not visualized on ultrasonography or computed tomography, biliary MRI should be performed before any operative indication. Intraoperatively, if the gallbladder cannot be identified, patient safety must remain the priority: hazardous dissection should be avoided, the common bile duct should be drained if necessary, and the diagnosis confirmed through postoperative imaging.
Our case illustrates the importance of a thoughtful, conservative approach in biliary surgery and highlights the decisive value of MRCP in diagnosing this rare anomaly.
References
- Kasi PM, et Gallbladder agenesis. Case Rep Gastroenterol, 2011; 5: 10-14.
- Hanan B, et Gallbladder agenesis: embryological basis and clinical implications, World J Gastroenterol, 2005; 11: 6228-6231.
- Wei X, et Congenital absence of the gallbladder in a child: a case report. Front Pediatr, 2024; 12: 1440383.
- Bianco G, et Gallbladder agenesis: a case report and brief review. Case Rep Surg, 2018; 1-4.
- Tagliaferri E, et Agenesis of the Gallbladder: Role of Clinical Suspicion and Magnetic Resonance to Avoid Unnecessary Surgery. Case Rep Gastroenterol, 2017; 10: 819-825.
- Piltcher-da-Silva R, et Gallbladder agenesis: a rare and underdiagnosed congenital anomaly. J Surg Case Rep, 2022; rjac505.
- D’Orazio B, et Preoperative diagnosis of Gallbladder Agenesis with MRCP. Cureus, 2020.
- Anderson K, et Intraoperatively diagnosed gallbladder agenesis. Int J Surg Case Rep, 2022; 96: 107287.
- Malde Gallbladder agenesis diagnosed intra-operatively: a case report. J Med Case Rep, 2010; 4: 285.
- Brunt LM, et Safe cholecystectomy multi-society practice guideline and consensus on prevention of bile duct injury. Surg Endosc, 2020; 34: 2827-2849.
- Bennion RS, Thompson JE Jr, Tompkins RK. Agenesis of the gallbladder without extrahepatic biliary atresia. Arch Surg, 1988; 123(10): 1257-1260.
- Peloponissios N, Gillet M, Cavin R, Halkic N. Agenesis of the gallbladder: a dangerously misdiagnosed malformation. World J Gastroenterol, 2005; 11(39): 6228-6231.

