Left Paraduodenal Hernia: A Rare but Potentially Life-Threatening Cause of Small Bowel Obstruction
Kamal Khadija1, Benzidane Kamal1,*, Rayadi Mahassine1, Bouali Ichrak1, Ettaoussi abdelhak1, Majd Abdessamad1, Bouali Mounir1, Elbakouri Abdelillah1, Khaleq Khalid2 and El Hattabi Khalid1
1Department of Visceral Surgery emergency, Ibn Rochd Hospital, Hassan II University, Faculty of Medicine and Pharmacy, Casablanca, Morocco
2Department of Anesthesia and Resuscitation, Ibn Rochd Hospital, Hassan II University, Faculty of Medicine and Pharmacy, Casablanca, Morocco
Received Date: 10/02/2026; Published Date: 20/04/2026
*Corresponding author: Benzidane Kamal, Department of Visceral Surgery emergency, Ibn Rochd Hospital, Hassan II University, Faculty of Medicine and Pharmacy, Casablanca, Morocco
Abstract
Left Paraduodenal Hernia (LPDH) is the most frequent type of congenital internal hernia, resulting from an error of midgut rotation during embryogenesis. Despite its congenital nature, it often remains clinically silent until adulthood and may present with nonspecific abdominal symptoms or acute small bowel obstruction.
We report the case of an 18-year-old woman with no prior medical or surgical history who presented with chronic abdominal pain with acute exacerbation over 48 hours, associated with postprandial vomiting. Computed tomography demonstrated a left paraduodenal hernia. Surgical management was initiated laparoscopically but required conversion to midline laparotomy due to dense intrasaccular adhesions.
This case highlights the diagnostic difficulty of left paraduodenal hernia in young patients with chronic abdominal pain and no surgical history. Early recognition using CT imaging and timely surgical intervention are essential to prevent serious complications and ensure favorable outcomes.
Keywords: Left paraduodenal hernia; Internal hernia; Small bowel obstruction; Landzert’s fossa; Congenital mesocolic hernia
Introduction
Internal hernias are an uncommon cause of intestinal obstruction, accounting for less than 1% of all bowel obstruction cases and approximately 5.8% of small bowel obstructions [1,2]. Among them, paraduodenal hernias represent the most frequent congenital type, comprising nearly 53% of all internal hernias [3].
Left paraduodenal hernia arises from an embryological error during midgut rotation, leading to herniation of small bowel loops through the fossa of Landzert, a peritoneal recess located to the left of the fourth portion of the duodenum and posterior to the Inferior Mesenteric Vein (IMV) and the ascending branch of the left colic artery [4,5]. Although congenital, most patients present in adulthood, often with vague, intermittent abdominal pain or acute small bowel obstruction [6].
We report the case of a young woman presenting with chronic abdominal pain and acute exacerbation, in whom imaging revealed a left paraduodenal hernia. This observation underscores the importance of considering this rare entity in patients with unexplained abdominal symptoms and a virgin abdomen, and highlights the role of computed tomography and surgical exploration in establishing the diagnosis and guiding treatment.
Case Presentation
An 18-year-old woman, with no significant past medical history and no prior surgery, was admitted to the emergency department for chronic abdominal pain evolving over six months, with acute worsening over the previous 48 hours. The pain was associated with postprandial vomiting, without bowel transit disturbances or fever.
On clinical examination, the patient was conscious and hemodynamically stable. Abdominal examination revealed a non-distended abdomen with tenderness localized to the left flank, while the remainder of the abdomen was soft. Digital rectal examination revealed a rectal ampulla containing fecal matter.
An abdominal computed tomography scan, performed initially prior to presentation at the emergency department, showed a thin layer of intraperitoneal fluid, clustering of small bowel loops in the left hypochondrium, mesenteric hyperemia, and anterior displacement of the inferior mesenteric vein trunk. These findings were suggestive of a left paraduodenal hernia.
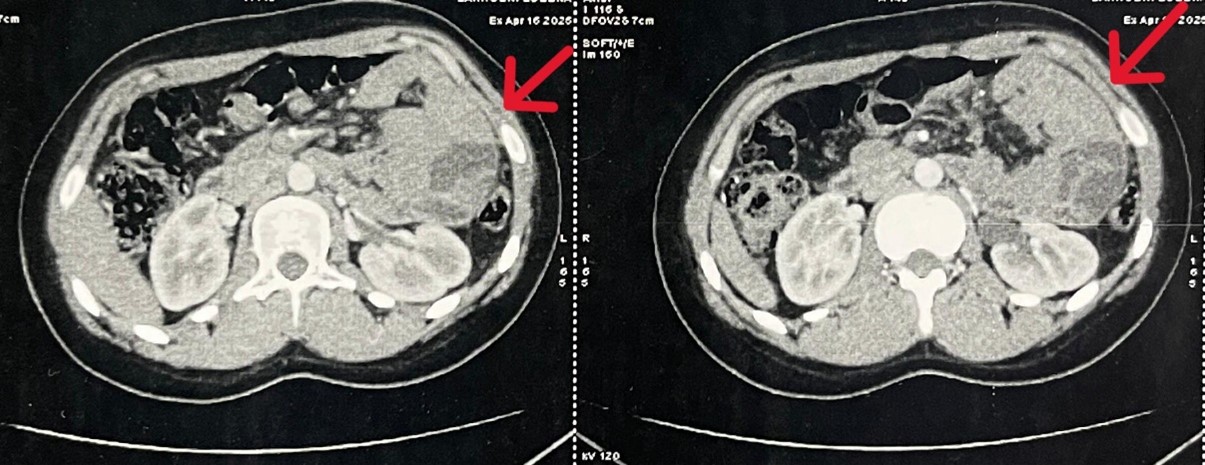
Figure 1: Computed tomography image demonstrating a left paraduodenal hernia.
The patient was admitted urgently to the operating room after appropriate preoperative management. A laparoscopic approach was initially chosen. Initial exploration revealed a small amount of purulent peritoneal effusion and a left paraduodenal hernia. Reduction of the hernia contents was not feasible laparoscopically due to dense intrasaccular adhesions. Consequently, conversion to a midline laparotomy was performed.
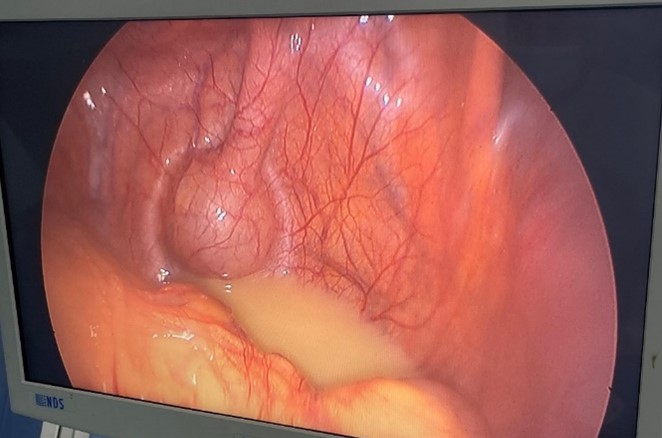
Figure 2: Purulent peritoneal effusion observed during laparoscopic exploration.
Careful reduction of the hernia contents was achieved, consisting of approximately 2.30 meters of viable small bowel. The hernia defect was closed using absorbable sutures.
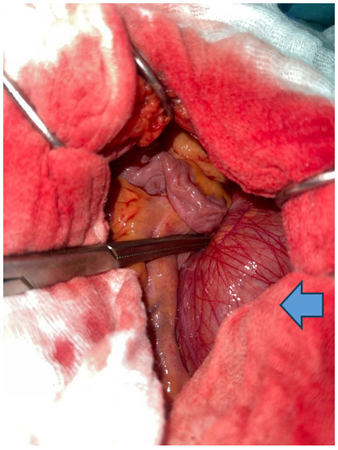
Figure 3: Intraoperative view before reduction of the hernia contents.
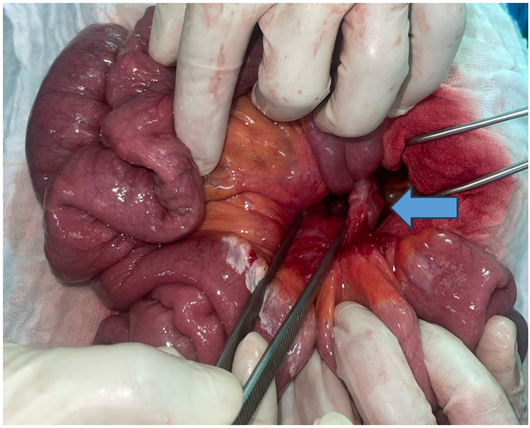
Figure 4: Intraoperative view after complete reduction of the hernia contents.
Discussion
Left paraduodenal hernias are three times more common in males than females and typically present between the fourth and sixth decades of life, with a mean age of approximately 38–40 years [4,7]. Embryologically, LPDH results from incomplete fusion of the left mesocolon with the posterior parietal peritoneum during midgut rotation, creating a potential space (Landzert’s fossa) into which the small bowel may herniate [5,8].
Clinical manifestations range from asymptomatic incidental findings to life-threatening acute intestinal obstruction. Many patients report a long history of vague, postprandial abdominal pain, nausea, or vomiting, often relieved by changes in posture [6,9]. Acute presentations include closed-loop obstruction, volvulus, strangulation, or ischemia, particularly in patients with no prior abdominal surgery (virgin abdomen) [10,11].
Preoperative diagnosis is challenging due to nonspecific symptoms. Plain abdominal radiographs are often inconclusive. Contrast-enhanced CT (CECT) is the gold standard, with diagnostic accuracy reported up to 95% [7,12].
Typical CT findings include:
- Clustered small bowel loops forming a sac-like mass in the left upper quadrant
- Location posterior to the stomach and pancreas or anterior to the left kidney
- Displacement and engorgement of mesenteric vessels
- Inferior mesenteric vein forming the anterior border of the hernia orifice
These features are consistently described across multiple reports and case series [7,12].
Surgical management is mandatory due to a lifetime incarceration risk exceeding 50% and reported mortality rates ranging from 20% to 50% in acute presentations [6,8,13]. The principles of surgery include:
- Reduction of herniated bowel loops
- Assessment of bowel viability
- Closure or widening of the hernia defect
Care must be taken to avoid injury to the IMV and left colic vessels. Both open and laparoscopic approaches have been described, with laparoscopy offering advantages such as reduced postoperative pain and shorter hospital stay in stable patients [11,14]. However, open surgery remains appropriate in emergency settings or when bowel ischemia is suspected.
Conclusion
Left paraduodenal hernia is a rare but significant cause of small bowel obstruction, particularly in patients without previous abdominal surgery. Its variable and nonspecific clinical presentation often delays diagnosis, increasing the risk of severe complications. Awareness of characteristic CT findings and a high index of suspicion are essential for early diagnosis. Prompt surgical intervention remains the cornerstone of management and significantly improves outcomes.
References
- Davis R. Surgery of left paraduodenal hernia. Am J Surg, 1975; 129: 570–573.
- Newsom BD, Kukora JS. Congenital and acquired internal hernias. Am J Surg, 1986; 152: 279–285.
- Ghahremani GG. Internal abdominal hernias. Radiology, 1984; 150: 63–72.
- Yun MY, et al. Left paraduodenal hernia presenting with atypical symptoms. Yonsei Med J, 2010; 51: 787–789.
- Anklowitz A, et al. Paraduodenal hernias resulting in small bowel obstruction. J Surg Case Rep, 2024; 8: rjae534.
- Hassani KIM, et al. Left paraduodenal hernia: A rare cause of acute abdomen. Pan Afr Med J, 2014; 17: 230.
- Shrestha S, et al. Left paraduodenal hernia causing closed-loop obstruction. Int J Surg Case Rep, 2025; 135: 111858.
- Willwerth BM, et al. Congenital mesocolic hernia: embryologic basis. Am J Surg, 1974; 128: 358–361.
- Falk GA, et al. Left paraduodenal hernia: review of the literature. BMJ Case Rep, 2010.
- Carrillo EH, et al. Left paraduodenal hernia revealed by unique CT findings. ACS Case Reviews, 2024.
- Blachar A, Federle MP. Internal hernia: clinical and imaging findings. Radiology, 2002; 225: 135–145.
- Meyers MA. Dynamic Radiology of the Abdomen. Springer, 2000.
- Dritsas ER, et al. Paraduodenal hernia: report of two cases. Am Surg, 2001; 67: 733–736.
- Uematsu T, et al. Laparoscopic repair of paraduodenal hernia. Surg Endosc, 1998; 12: 50–52.

