Bladder Papillomatosis Associated with Condylomas and HPV Positivity: About a Case
Anas Tmiri*, Mehdi Bennani, Oussama Bjane, Yassine Daghdagh, Adil Kbirou, Amine Moataz, Mohamed Dakir, Adil Debbagh and Rachid Aboutaieb
Department of Urology, University hospital center Ibn Rochd, Casablanca, Morocco
Faculty of Medicine and Pharmacy, Hassan II University, Casablanca, Morocco
Received Date: 07/02/2026; Published Date: 03/04/2026
*Corresponding author: Anas Tmiri, Department of Urology, University hospital center Ibn Rochd, Casablanca, Morocco; Faculty of Medicine and Pharmacy, Hassan II University, Casablanca, Morocco
Abstract
HPV infections are now well known as an STD and as a promoter of genital cancers. The most well-known lesions are warts and condylomas. Intravesical location remains rare, which poses a diagnostic problem with urothelial carcinomas, which usually develop within the bladder.
We report a case of intravesical condylomas following a positive HPV infection in a 26-year-old woman.
Keywords: Condylomas; HPV infection; Risk of cancer; Sexually transmitted disease
Introduction
Human Papillomaviruses (HPV) are responsible for common benign mucocutaneous infections. The most well-known lesions are warts and condylomas. In the anogenital region, they constitute a genuine Sexually Transmitted Infection (STI). Intravesical involvement remains rare, which poses a diagnostic challenge, distinguishing them from urothelial carcinomas, which typically develop within the bladder [1].
We describe a case of bladder papillomatosis with condylomas induced by a confirmed HPV infection in a 26-year-old woman.
Case Report
Patient aged 26 years, hypertensive under amplodine, End-stage renal failure in October 2023, Hemodialysis for about 9 months, Kidney transplant in July 2024, living related donor (husband), Post-transplant ureterovesical anastomosis narrowing which benefited from ureterovesical reimplantation with placement of a double J stent in November 2024, with a history of recurrent multi-resistant urinary tract infections, Incomplete resection of bladder papillomatosis + change of right JJ stent in 09/2025.
The history of the illness dates back to August 2025 following a control ultrasound which revealed suspicious bladder lesions, supplemented by a CT uroscan which revealed a focal and budding endoluminal wall thickening of the right anteroinferior wall, heterogeneously enhanced after injection of iodinated contrast medium, measuring 16.2 mm in maximum thickness.
The patient underwent an initial incomplete resection of a bladder papilloma in month 09/25 and a change of JJ with anatomopathological examination of an epidermoid papilloma with focal presence of HPV stigma, confirmed by PCR for HPV which came back positive.
She presented for further resection of bladder lesions (Figure 1).
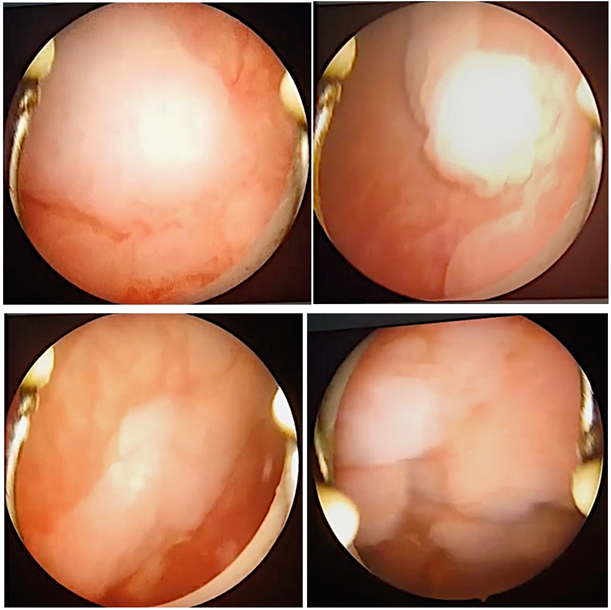
Figure 1: Condylomas affecting all bladder walls.
Discussion
The peak incidence of genital HPV infections occurs between the ages of 20 and 25. The cumulative incidence of HPV carriage detected by PCR or hybrid capture in young people several years after their first sexual intercourse is over 50%. Only 5 to 10% of women with high-risk HPV will develop cytological abnormalities, and less than 1% of these persistent forms will lead to cancer. Several publications have demonstrated the importance of viral load and clearance. Virus in the determinism of this evolution [2,3].
No similar cases of intravesical papillomas induced by HPV infection have been found in the literature; this location remains very rare and has never been described. The most frequently described locations were cutaneous, anorectal, and genital lesions [1,2,3].
The link between HPV and certain cancer or precancerous lesions is now well established. However, HPV infection is, as we will see later, a common condition and few lesions will transform. The demonstration of this oncogenic potential was based on epidemiological and clinical data, and its mechanism on experimental data. The virus can be currently considered a necessary but not sufficient factor in this transformation, which involves many other cofactors. Thus, cervical cancer is the leading cancer solid gynecological lesion of proven viral origin[4,5,6].
The diagnosis of any HPV-related mucosal condition should be considered as that of a sexually transmitted disease and a systematic search for an associated STD should be carried out, in particular by performing serology for the human immunodeficiency virus (HIV) and an examination of the sexual partner(s).
Protected intercourse, although debatable for virus-induced dysplasias, is, for this reason, inseparable from treatment [1,2].
Therapeutic vaccines intended for patients already infected with HPV and suffering from severe induced lesions (cancer) face numerous challenges. They must act on the local immune system, specifically by recognizing the viral proteins expressed by infected and transformed cells. The early E6 and E7 proteins are even expressed by cancer cells. Therefore, these are the targets being studied for vaccine development. Aside from a few inconclusive experiments on advanced cases in humans, such a vaccine is currently being tested only in animals [7].
Conclusion
HPV infections are now well known as an STD and as a promoter of genital cancers. Recent advances in the field of organotypic cultures and the production of pseudo particles viral infections have allowed us to better understand the viral cycle, the mechanisms of oncogenesis and to begin the first prophylactic vaccinations.
References
- Douvier S, Dalac S. Infections à papillomavirus. EMC-Maladies Infectieuses, 2004; 1: 235–261.
- Weissenbacher ER, Schneider A, Gissmann L, Gross G, Heinrich J, Hillemanns P, et al. Recommendations for the diagnosis and treatment of HPV infections of the femal tract. Eur J Infect Immunol Dis Obstet Gynecol, 2001; (suppl 2): 1–2.
- Ylitalo N, Sorenso P, Josefsson AM, Magnusson PK, Andersen PK, Ponten J, et al. Consistent high viral load of human papillomavirus 16 and risk of cervical carcinoma in situ. Lancet, 2000; 355: 2194–2198.
- Bosch FX, Rohan T, Schneider A, Frazer I, Pfister H, Castellsague X, et al. Papillomavirus research update: highlights of the Barcelona HPV 2000 international papillomavirus conference. J Clin Pathol, 2001; 54: p. 163–175.
- Walboomers JM, Jacobs MV, Manos MM, Bosch FX, Kummer JA, Shah KV, et al. Human papillomavirus is a necessary cause of invasive cervical cancer worldwide. J Pathol, 1999; 189: 12–19.
- Wallin KL, Wiklund F, Angstrom T, Bergman F, Stendahl U, Wadell G, et al. Type-specific persistence of human papillomavirus DNA before the development of invasive cervical cancer. N Engl J Med, 1999; 341: 1633–1638.
- Wang TL, Ling M, Shih IM, Pham T, Pai SI, Lu Z, Kurman RJ, et al. Intramuscular administration of E7-transfected dendritic cells generates the most potent E7-specific antitumor immunity. Gene Ther, 2000; 7: 726–733.

