Deep Annular Granuloma and the Reverse Koebner Phenomenon: Case Report of Post-Biopsy Regression
Rihame Al Heyasat¹,*, Hanane Baybay¹, Layla Tahiri Elousrouti², Ikram Bejja¹, Saadia Boughaleb¹, Zakia Douhi¹, Meryem Soughi¹, Sara Elloudi¹ and Fatima Zahra Mernissi¹
¹Department of Dermatology, Hassan II University Hospital, Fez, Morocco
²Department of Pathology, Hassan II University Hospital, Fez, Morocco
Received Date: 28/01/2026; Published Date: 30/03/2026
*Corresponding author: Rihame Al Heyasat, Dermatology, Hassan II University Hospital, Sidi Mohamed Ben Abdellah University, Fez, Morocco
Abstract
Deep Annular Granuloma (DAG), also known as subcutaneous annular granuloma, is a rare, benign granulomatous skin disorder that primarily affects children and young adults. Clinically, it presents as erythematous to violaceous papules or plaques with well-defined, slightly elevated borders and central clearing, forming an annular configuration. Lesions typically involve the lower extremities, forearms, buttocks, hands, and feet.
We report the case of a 52-year-old male with a history of insulin-treated diabetes mellitus for eight years, hypertension managed with amlodipine, and chronic kidney disease under regular follow-up, who presented with non-pruritic, erythematous, infiltrated plaques on both legs evolving over one month. Dermatological examination revealed multiple orange-red papules with a waxy appearance, arranged annularly with active borders. Dermoscopy showed white structures on an erythematous background with focal lipid-like areas.
Skin biopsies confirmed the diagnosis of deep annular granuloma. Remarkably, at follow-up ten days later during suture removal, all lesions had completely resolved, leaving only mild residual hyperpigmentation. No additional treatment was administered.
This case highlights a rare phenomenon: spontaneous resolution of deep annular granuloma following biopsy. It suggests that tissue injury may trigger an immune response contributing to lesion regression and raises the possibility that biopsy may serve not only as a diagnostic procedure but also as a therapeutic stimulus in DAG, warranting further investigation.
Keywords: Subcutaneous granuloma annulare; Reverse Koebner phenomenon; Spontaneous regression
Introduction
Granuloma annulare is a benign, self-limiting granulomatous dermatosis characterized histologically by necrobiotic collagen surrounded by palisading histiocytes, the etiology of which remains poorly understood. Several clinical variants have been described, including localized, generalized, perforating, and subcutaneous forms [1], each differing in presentation, prognosis, and age distribution.
Deep annular granuloma, also known as subcutaneous granuloma annulare, represents a rare variant that predominantly affects children and young adults. It typically presents as asymptomatic, firm, subcutaneous nodules, most commonly involving the extremities. Due to its clinical resemblance to other subcutaneous tumors or inflammatory conditions, diagnosis often requires histopathological confirmation [2].
The Koebner phenomenon, first described by Heinrich Koebner in patients with psoriasis, refers to the development of typical lesions at sites of cutaneous trauma and has since been reported in numerous dermatological disorders [3]. Conversely, traumatic events such as surgical procedures or skin biopsies have, in rare instances, been associated with lesion regression rather than induction [4].
This paradoxical response is referred to as the reverse Koebner phenomenon, defined as the partial or complete disappearance of lesions following cutaneous injury. This phenomenon remains exceptionally rare, with only a limited number of cases documented in the literature across various dermatoses [5,6].
The objective of this report is to describe a rare case of deep annular granuloma demonstrating spontaneous resolution following a diagnostic skin biopsy, thereby contributing to the limited literature on the reverse Koebner phenomenon and highlighting its potential role in the pathophysiology of annulare granuloma.
Case Presentation
A 52-year-old patient with a medical history of insulin-treated diabetes mellitus for eight years, hypertension treated with amlodipine, and chronic kidney disease under regular nephrological follow-up presented with non-pruritic, erythematous, infiltrated plaques on both legs evolving over a one-month period.
Dermatological examination revealed bilateral, circumferential, orange-erythematous plaques with an infiltrated and partially sclerotic appearance. The lesions were composed of multiple erythematous papules, some with a waxy appearance, arranged in annular configurations with an active peripheral border (Figure 1). Dermoscopic examination demonstrated white structureless areas on an erythematous background with focal lipid-like features (Figure 2).
Laboratory investigations, including complete blood count, liver function tests, lactate dehydrogenase, thyroid function tests, and serum electrolyte levels, were within normal limits. Renal function tests (serum creatinine and urea) were stable and consistent with the patient’s known baseline values, without evidence of acute deterioration. Serological tests for hepatitis B and C viruses and human immunodeficiency virus were negative. Serum Angiotensin-Converting Enzyme (ACE) levels were within normal limits, and chest imaging showed no evidence of hilar lymphadenopathy or pulmonary involvement, allowing sarcoidosis to be reasonably excluded.
Skin biopsies obtained from the leg lesions revealed an unremarkable stratified squamous epithelium with an intact basement membrane and no interface changes. The papillary dermis was edematous and highly vascularized, with congested capillaries and a mild lymphocytic infiltrate associated with multinucleated giant cells. The mid and deep dermis showed no significant abnormalities. In contrast, the hypodermis demonstrated thickened fibrous septa with fibrosis extending into the adipose lobules, accompanied by a periadipocytic inflammatory infiltrate composed of lymphocytes and macrophages. These histopathological findings were consistent with a diagnosis of deep (subcutaneous) granuloma annulare (Figure 3). The clinically waxy appearance of the papules was attributed to secondary dermal changes, including papillary dermal edema and vascular congestion, rather than primary dermal granulomatous involvement.
Remarkably, at follow-up ten days later during suture removal, the lesions had completely resolved, leaving only mild residual hyperpigmentation (Figure 4). Dermoscopic reassessment showed disappearance of the lupoid-like pattern, with the emergence of a pigment network and residual whitish structures (Figure 5). No additional treatment was initiated.
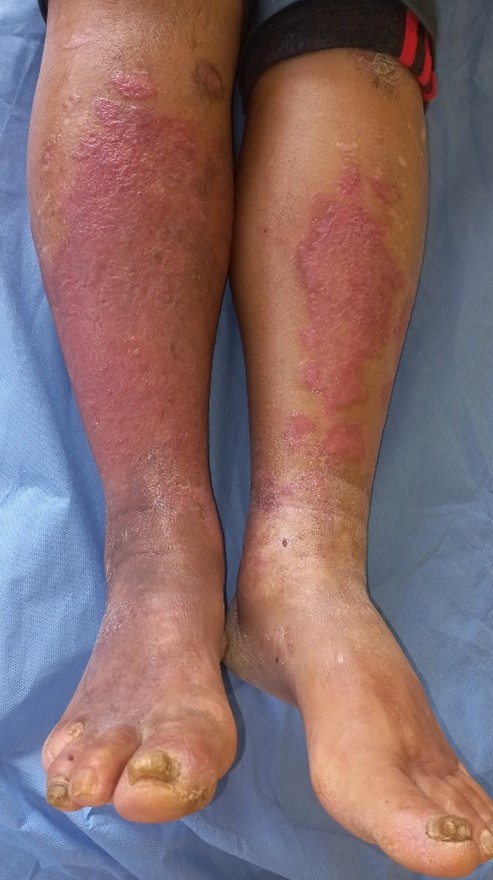
Figure 1: Dermatological examination showing bilateral, circumferential, orange-erythematous plaques with an infiltrated and sclerotic appearance. The lesions consist of multiple erythematous papules, some with a waxy texture, arranged in annular configurations with active peripheral borders.
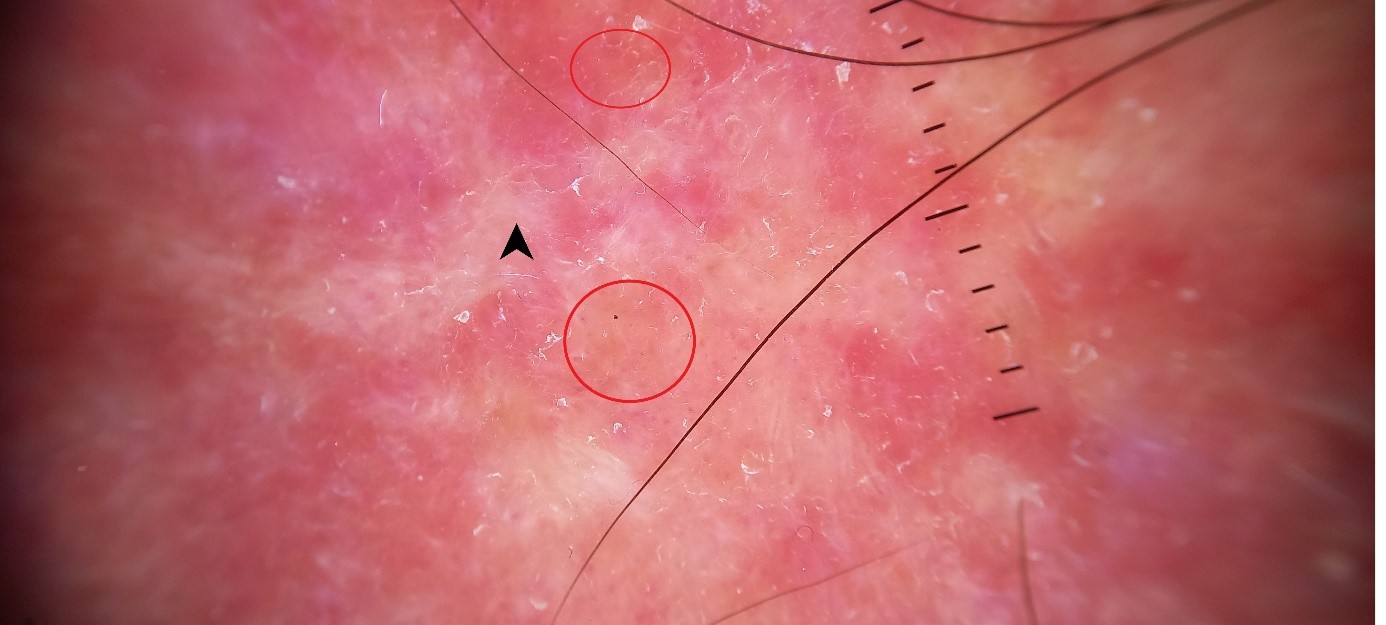
Figure 2: Dermoscopic image showing white structureless areas (black arrow) on an erythematous background, with focal lipid-like areas (red circles).
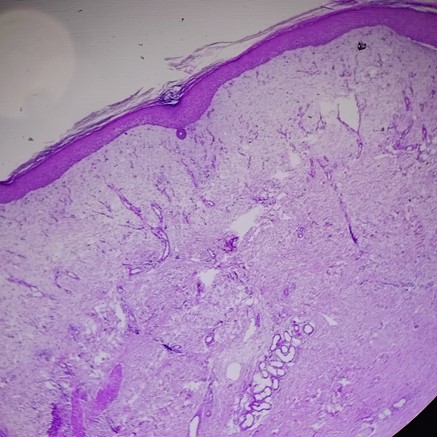
Figure 3: Histopathological examination showing an unremarkable stratified squamous epithelium, papillary dermal edema with vascular congestion and mild lymphocytic infiltrate with multinucleated giant cells.
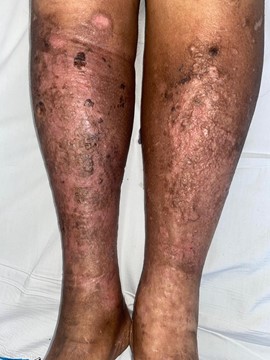
Figure 4: Clinical evolution after biopsy showing complete resolution of the lesions, leaving residual hyperpigmentation and desquamation.
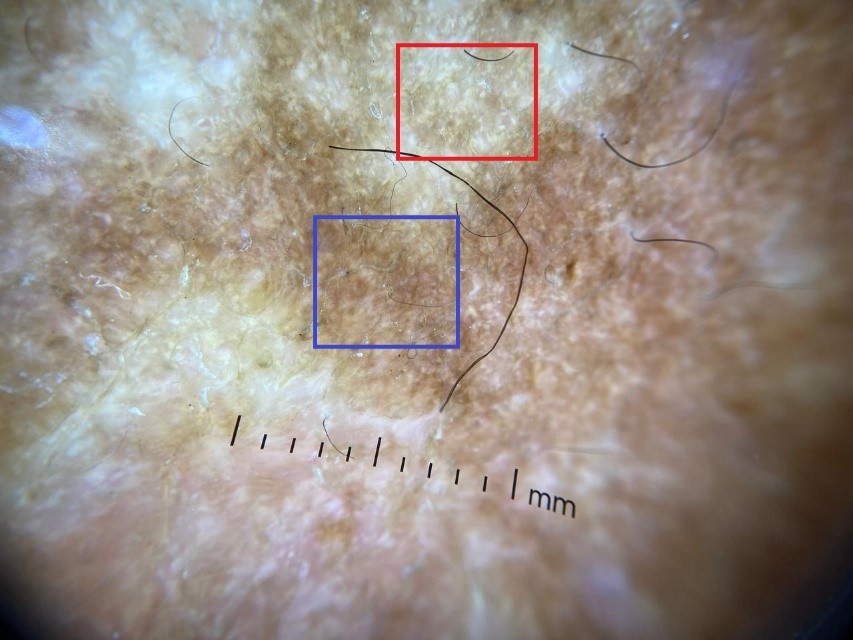
Figure 5: Dermoscopic reassessment showing disappearance of the lupoid-like pattern, with the emergence of a pigment network (blue square) and residual whitish structures (red square).
Discussion
Deep Annular Granuloma (DAG) is a rare, benign granulomatous dermatosis of unknown etiology affecting both children and adults, with a marked female predominance. Clinically, lesions most commonly involve the lower extremities, forearms, buttocks, hands, and feet. The hallmark lesion is an erythematous to violaceous papule or plaque with a well-demarcated, slightly elevated border and central clearing, forming an annular configuration.
Annulare granuloma has been reported to present as erythematous to brown patches [1] or as erythematous patches that later evolve into annular papules [7]. Lesions are typically asymptomatic, although mild tenderness or discomfort may occasionally occur.
To date, no standardized treatment protocol exists for granuloma annulare. Reported therapeutic options include intralesional corticosteroid injections, cryotherapy, CO₂ laser ablation, and low-dose intralesional interferon-gamma injections, with variable efficacy [2]. Requena/Surgical excision is generally discouraged, as it is rarely curative and may result in scarring. Spontaneous regression of lesions has been well documented and may occur over several months to years [8].
The reverse Koebner phenomenon remains poorly understood due to its rarity. However, it has been reported at biopsy sites in various dermatoses, including psoriasis, leukocytoclastic vasculitis, and annulare granuloma [9].
Levin et al. [8] reported that patch-type annulare granuloma resolved only at the biopsy site, while lesions at unbiopsied areas persisted. In contrast, in our case, complete resolution occurred, affecting both the biopsied site and the previously unbiopsied areas. This observation suggests that the wound healing process may contribute to lesion regression. This response may be mediated by immunomodulatory effects induced by tissue injury, potentially leading to downregulation of the granulomatous inflammatory process and promoting lesion clearance.
Conclusion
This case highlights the rare occurrence of deep annular granuloma regression following skin biopsy. The observation suggests that biopsy-induced tissue injury may trigger immune mechanisms contributing to lesion resolution. This phenomenon underscores the potential therapeutic implications of biopsy in DAG and warrants further investigation to elucidate the underlying mechanisms.
References
- Naveen KN, Pai VV, Athanikar SB, Gupta G, Parshwanath HA. Remote reverse koebner phenomenon in generalized granuloma annulare. Indian Dermatol Online J, 2014; 5: 219-221. doi: 10.4103/2229-5178.131137.
- Requena L, Fernàndez-Figueras MT. Subcutaneous granuloma annulare. Semin Cutan Med Surg, 2007; 26: 96-99.
- Kobner H. Zur aetologie der psoriasis. Vierteljahrsschr Dermatol Syphil, 1877; 8: 559.
- Mulkalwar A, Kharkar V. Granuloma annulare masquerading as Hansen’s disease and showing reverse Koebner phenomenon.international journal of clinical and medical images, 2021; 8: 733. doi: 10.23937/2376-0249/14100733.
- Grekin DA, Van Scott EJ. Dermal role and controls in psoriasis. Arch Dermatol, 1973; 108: 425.
- Martin JM, Conde A, Pinazo I, et al. Reverse koebnerization after radiotherapy in a woman with a mastectomy for a breast carcinoma. J Am Acad Dermatol, 2006; 55: S90-S91. doi: 10.1016/j.jaad.2004.03.042.
- Diya F, Mutasim MD, Alina G. Patch granuloma annulare: clinicopathologic study of 6 patients. J Am Acad Dermatol, 2000; 42: 417-421. doi: 10.1016/s0190-9622(00)90212-3.
- Levin NA, Patterson JW, Yao LL, Wilson BB. Resolution of patch-type granuloma annulare lesions after biopsy. J Am Acad Dermatol, 2002; 46: 426-429. doi: 10.1067/mjd.2002.118344.
- Yadav S, De D, Kanwar AJ. Reverse koebner phenomenon in leukocytoclastic vasculitis. Indian J Dermatol, 2011; 56: 598-599. doi: 4103/0019-5154.87169.

