Multiple Cerebral Infarctions Revealing Metastatic Choriocarcinoma
Aasmi H*, Khattab H, Sikkal A, El Otmani H, Rafai MA and El Moutawakil B
Department of Neurology, University of Hassan II Casablanca, Casablanca, Morocco
Received Date: 19/01/2026; Published Date: 09/03/2026
*Corresponding author: Aasmi H, Department of Neurology, University of Hassan II Casablanca, Casablanca, Morocco
Abstract
Introduction: Choriocarcinoma is a highly malignant trophoblastic neoplasia with a propensity for early metastasis, particularly to the lungs, liver, vagina, and Central Nervous System (CNS). The later, as a rare manifestation, can sometimes be the initial clinical presentation.
Observation: We report a case of a 44-year-old female who presented a proportional and total left hemiplegia with lateral hemianopsia. Brain imaging revealed multiple bilateral ischemic strokes in different vascular territories. The D-dimer level was elevated at 510 ng/mL, and the serum human chorionic gonadotropin (β-hCG) level was >1,000 IU/mL. Metastatic choriocarcinoma was diagnosed, and chemotherapy was initiated.
Conclusion: Cancer-related coagulopathy, micro tumoral emboli, or both could be implicated in the pathogenesis of cerebral infarctions. In such a scenario, the serum measurement of β-hCG should be included in the panel of tumor markers in cases of ischemic strokes in young women.
Keywords: Choriocarcinoma; Stroke; Gestational trophoblastic disease; Metastases
Introduction
The choriocarcinoma is one clinical manifestation within the spectrum of Gestational Trophoblastic Disease (GTD); it is a highly malignant form that can rapidly spread through the bloodstream to the lungs, vagina, liver, kidneys, ovaries, and the brain. Approximately 20% of choriocarcinoma patients experience central nervous system (CNS) involvement, with clinical presentations including intracranial hypertension, intracerebral hemorrhage, and stroke [1,2]. We report a case of metastatic choriocarcinoma incidentally discovered during the evaluation of a patient who presented with multiple bilateral strokes.
Case Report
A 44-year-old woman, with a history of miscarriage in 2019 and uninvestigated uterine bleeding since october 2022. She was admitted on December 2022, due to left hemiplegia with facial palsy and language disturbances. These symptoms were preceded by behavioral changes, characterized by agitation and incoherent speech, developing progressively over the preceding month. Physical exam revealed confusion and left hemiplegia. Brain MRI revealed multiple bilateral ischemic strokes involving carotid and vertebrobasilar territories (Figure 1). Due to clinical worsening on the second day of hospitalization, a cerebral CT scan showed a new ischemic stroke of the right middle cerebral artery (Figure 2).
The electrocardiogram and transthoracic echocardiography showed no abnormalities. Transesophageal echocardiography could not be performed due to agitation. Hemogram, sedimentation rate, electrolytes, renal, hepatic, and thyroid functions were normal. LDL cholesterol level was 1.52 g/L, and D-dimer levels were elevated at 510 ng/L.
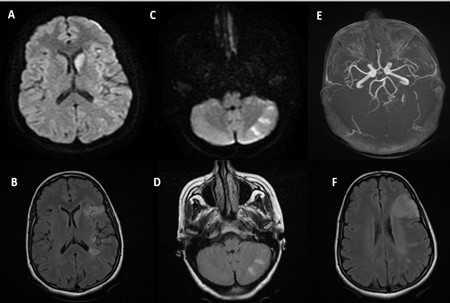
Figure 1: Brain MRI showing multiple ischemic strokes in different territories (A, B, C, D, F) with normal arterial MR angiography (E).
A lumbar puncture could not be performed due to the mass effect observed on the control imaging. The multiple nature of the strokes suggested an embolic origin. A tumor-related cause was considered, given the history of uterine bleeding. Among the indicated tumor markers, β-hCG levels were elevated (>15,000 mIU/mL with normal range <100 mIU/mL), increasing to 44,574 mIU/mL after 5 days. Thoraco-abdomino- pelvic computed tomography (CT) revealed the presence of a hypodense and heterodense endoluminal content at the level of both the left lower lobar artery and the left lower pulmonary vein without involvement in other locations.
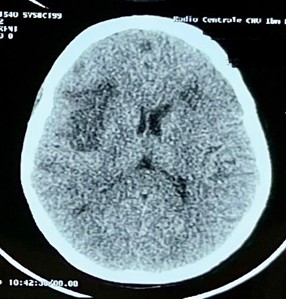
Figure 2: Brain CT scan revealing a new contralateral ischemic stroke: Right Sylvian ischemic stroke with mass effect.
The combination of this radiological appearance and the elevation of β-HCG in a young female patient strongly suggested gestational trophoblastic disease.
Curative anticoagulation with low molecular weight heparin (LMWH) was initiated before transferring the patient to the oncology department for further management.
Meanwhile, the β-hCG levels continued to rise (66,019 mIU/mL). The clinical course was marked by the emergence of cerebral metastases, and the patient death one month after the vascular event (Figure 3, 4).
Discussion
Strokes are common in cases of cancer, occurring in 15% of patients and significantly worsening their prognosis [3]. The frequency of ischemic strokes is comparable to that of cerebral hemorrhages [4]. Strokes can occur either following the initial cancer diagnosis [5] or precede the diagnosis of the cancerous condition, as described in our case [6]. The first major autopsy study, conducted in 1985 by Graus et al. demonstrated that the most common complication of the central nervous system in cancer patients was metastases, followed by cerebral infarction and hemorrhage [7]. It has also been reported that patients experiencing a stroke during active cancer are typically younger, and cryptogenic strokes are more severe and more frequent [3].
The time interval between the cancer diagnosis and the stroke varies widely and also depends on the type of cancer. In fact, Solid tumors tend to develop strokes later than malignant hematologic conditions [8]. The study by Graus et al. described the primary clinical presentation of strokes in cancer patients as more resembling diffuse encephalopathy rather than a typical sudden-onset with focal deficits [7]. Our patient also exhibited features of encephalopathy, characterized by psychiatric disturbances and a confusional state, well before the acute stroke presentation. This could be attributed to the diverse mechanisms of stroke in patients with a cancerous condition, which may be directly related to the cancer or caused by its complications, such as coagulation disorders, infections, leptomeningeal extension, or therapeutic interventions (eg. chemotherapy and radiotherapy…) [7,9].
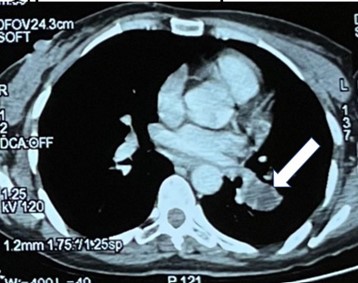
Figure 3: Thoracic CT scan revealing a transcissural process at the level of the left lower lobar artery.
Generally, cancer-associated ischemic strokes are described as affecting multiple vascular territories [3,10,11], accompanied by elevated D-dimer levels and a pro- inflammatory component such as low hematocrit and elevated CRP levels [12- 15], as well as fibrin degradation products [12-14] a tumor marker can further support the diagnosis [16].
The management of cancer-associated strokes depends on the type of event. For ischemic strokes, intravenous thrombolysis may be considered, with a wide indication for anticoagulants. Additionally, hemorrhages and cerebral venous thrombosis are managed according to established protocols [9].
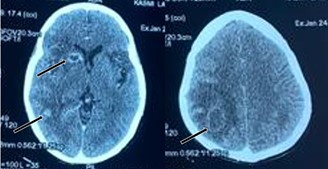
Figure 4: Brain CT with contrast injection showing multiple brain metastases.
Regarding our case, choriocarcinoma as a tumor entity is characterized by its high metastatic potential and chemosensitivity. Its diagnosis is primarily based on biological markers, specifically plasma β- hCG levels [17,18]. This condition develops rapidly and metastasizes to the lungs, liver, and less frequently to cerebral blood vessels, causing thrombosis or more commonly the formation of a neoplastic aneurysm, leading to ischemic strokes or intraparenchymal hemorrhage, respectively [5,19,20].
This clinical vignette adds to the various observations in the literature highlighting the association between cancer and stroke, emphasizing the importance of considering a neoplastic pathology, in addition to cardiovascular origins, whenever faced with multiple lesions. Despite the generally favorable prognosis of choriocarcinoma due to its chemosensitivity, the comorbidity with a vascular event darkens the prognosis and increases the mortality rate [3].
References
- Athanassiou A, Begent RH, Newlands ES, Parker D, Rustin GJ, Bagshawe KD. Central nervous system metastases of choriocarcinoma: 23 years' experience at Charing Cross Hospital. Cancer, 1983; 52: 1728-1735.
- Saad N, Tang YM, Sclavos E, Stuckey Metastatic choriocarcinoma: a rare cause of stroke in the young adult. Australas Radiol, 2006; 50: 481-483.
- Kneihsl M, Enzinger C, Wünsch G, Khalil M, Culea V, Urbanic-Purkart T, et al. Poor short-term outcome in patients with ischemic stroke and active J Neurol, 2016; 263: 150-156.
- Arboix A: Cerebrovascular disease in the cancer patient. Rev Neurol, 2000; 31: 1250-1252.
- Grisold W, Oberndorfer S, Struhal Stroke and cancer: A review. Acta Neurol Scand, 2009; 119: 1-16.
- Taccone FS, Jeangette SM, Blecic SA. First-ever stroke as initial presentation of systemic J Stroke Cerebrovasc Dis, 2008; 17: 169-174.
- Graus F, Rogers LR, Posner Cerebrovascular complications in patients with cancer. Medicine (Baltimore), 1985; 64: 16-35.
- Raizer JJ, DeAngelis Cerebral sinus thrombosis diagnosed by MRI and MR venography in cancer patients. Neurology, 2000; 54: 1222-1226.
- Dardiotis E, Aloizou AM, Markoula S, Siokas V, Tsarouhas K, Tzanakakis G, et al. Cancer-associated stroke: Pathophysiology, detection and management (Review). Int J Oncol, 2019; 54(3): 779-796.
- Liu J, Frishman WH. Nonbacterial Thrombotic Endocarditis: Pathogenesis, Diagnosis, and Cardiol Rev, 2016; 24: 244-247.
- Kim SJ, Park JH, Lee MJ, Park YG, Ahn MJ, Bang OY. Clues to occult cancer in patients with ischemic stroke. PLoS One, 2012; 7: e44959.
- Selvik HA, Thomassen L, Bjerkreim AT, Næss H. Cancer-Associated Stroke: The Bergen NORSTROKE Cerebrovasc Dis Extra, 2015; 5: 107-113.
- Karlińska AG, Gromadzka G, Karliński MA, Członkowska A. The activity of malignancy may determine stroke pattern in cancer J Stroke Cerebrovasc Dis, 2015; 24: 778-783.
- Selvik HA, Bjerkreim AT, Thomassen L, Waje- Andreassen U, Naess H, Kvistad When to Screen Ischemic Stroke Patients for Cancer. Cerebrovasc Dis, 2018; 45: 42-47.
- Cocho D, Gendre J, Boltes A, Espinosa J, Ricciardi AC, Pons J, et al. Predictors of occult cancer in acute ischemic stroke patients. J Stroke Cerebrovasc Dis, 2015; 24: 1324-1328.
- Xie X, Chen L, Zeng J, Qin C, Cheng D, Wei X, et al. Clinical features and biological markers of lung cancer- associated stroke. J Int Med Res, 2016; 44: 1483-1491.
- Jain P, Cietak Post-term choriocarcinoma with unusually low βHCG. Journal of Obstetrics & Gynaecology, 2008; 28: 661–662.
- Gurwitt LJ, Ling JM, Clarh RE. Cerebral metastatic choriocarcinoma: a postpartum cause of Obstet Gynecol, 1975; 45: 583–588.
- Komeichi T, Igarashi K, Takigami M, Saito K, Isu T, Itamoto K. A case of metastatic choriocarcinoma associated with cerebral thrombosis and aneurysmal formation. No Shinkei Geka, 1996; 24: 463–467.
- Kwon HM, Kang BS, Yoon Stroke as the first manifestation of concealed cancer. J Neurol Sci, 2007; 258: 80-83.

