Ectopia Cordis: Fatal Disease or Maybe Not?
Ivona Vučić1,*, Mateja Mirčić1, Željko Đurić2, Sanja Konosić1, Dorotea Bartoniček3, Filip Rubić3 and Željko Čolak1
1Department of Anesthesiology, University hospital Zagreb, Croatia
2Department of Cardiac Surgery, University hospital Zagreb, Croatia
3Department of Pediatrics, University hospital Zagreb, Croatia
Received Date: 04/11/2025; Published Date: 12/12/2025
*Corresponding author: Ivona Vučić, Department of Anesthesiology, University hospital Zagreb, Croatia
Abstract
Background: Ectopia cordis (EC) is a rare and severe congenital anomaly characterized by complete or partial displacement of the heart outside the thoracic cavity. Prognosis is generally poor, particularly when associated with intracardiac or extracardiac malformations.
Case Presentation: We present a full-term male newborn diagnosed postnatally with thoracoabdominal ectopia cordis without associated intracardiac defects. Prenatal ultrasound findings were reported as normal. After birth, the patient exhibited an anterior thoracic wall defect with both ventricles located extrathoracically. Imaging con-firmed normal atrioventricular concordance and a hemodynamically significant patent ductus arteriosus. The pa-tient was transferred to our institution on day 5 of life and underwent three staged surgical procedures aimed at gradual repositioning of the heart and closure of the thoracic and abdominal defects. Only skin and soft tissue clo-sure was achievable without compromising hemodynamic stability. Postoperatively, the patient required inotropic support and prolonged ventilatory assistance. Difficulty in weaning from mechanical ventilation led to tracheoto-my, after which stable spontaneous breathing was achieved.
Discussion: Survival in EC is strongly dependent on the presence or absence of concomitant cardiac anomalies and the ability to cover and protect the exposed heart. This case is notable for the absence of intracardiac malfor-mations and successful staged management despite significant respiratory challenges.
Conclusion: Thoracoabdominal ectopia cordis without associated cardiac defects is extremely rare. Early multi-disciplinary intervention, protection of the exposed heart, and individualized staged repair can lead to favorable outcomes, although postoperative respiratory complications remain common.
Introduction
Ectopia cordis (EC) is a severe congenital anomaly of the sternal wall in which the heart is completely or partially displaced outside of the thoracic cavity [1].
The prevalence of this condition is 0.1% among all heart defects with an incidence of 5.5 to 7.9 per million births.
The etiology of EC is not yet understood, but several theories are available. The first theory involves primary failure of heart descent and midline fusion in early embryological development. Another theory stated that EC may occur due to rupture of the chorion and/or yolk sac thus leading to the formation of fibrous bands that prevent midline fusion because of the compression. The latest theory is that this anomaly may occur due to the lack of a functional Bone Morphogenetic Protein (BMP2) gene. The presence of that gene mediates heart tube formation and ventral body wall closure [2].
Patient may present with other cardiac anomalies such as ventricular or atrial septal defects, double outlet right ventricle and Tetralogy of Fallot as well as non-cardiac defects such as omphalocele, scoliosis, central nervous system disorders and others [3].
Ectopia cordis has been classified into five categories: cervical, thoracocervical, thoracic, thoracoabdominal and abdominal depending on the location of the ectopic heart [4].
Prognosis is determined by the extent of the defect, level of exposure of the heart as well as the presence of concomitant intracardiac anomalies. In severe forms, prenatal diagnosis can lead to a therapeutic abortion [5].
The first attempted repair of EC was performed in 1925 by Cutler and Wilens. In 1975 Koop achieved the first successful repair of thoracic EC in two stage repair. Twenty years later Amato et al. reported a successful single-stage repair of thoracic EC [6].
This condition presents as a surgical emergency and demands early and specialised intervention. The monitoring and treatment of this rare anomaly varies from patient to patient and there is currently no consensus to determine the therapeutic plan.
This case report describes the management of the fourth type of ectopia cordis meaning thoracoabdominal type without accompanied cardiac defects.
Case Description
A term male newborn, 40 weeks of gestation, BW 3625 g, was delivered in a medical centre without specialized congenital pediatric cardiac facilities, and was referred to our institution.
The patient was born from a regularly controlled pregnancy with an uncomplicated course. Prenatal ultrasound examinations were described as normal. The mother was hospitalized on the day of delivery, and the delivery was completed vaginally.
After delivery, a defect in the anterior chest wall was noticed, as well as a supraumbilical opening in the anterior abdominal wall. An ultrasound of the heart and a CT scan of the
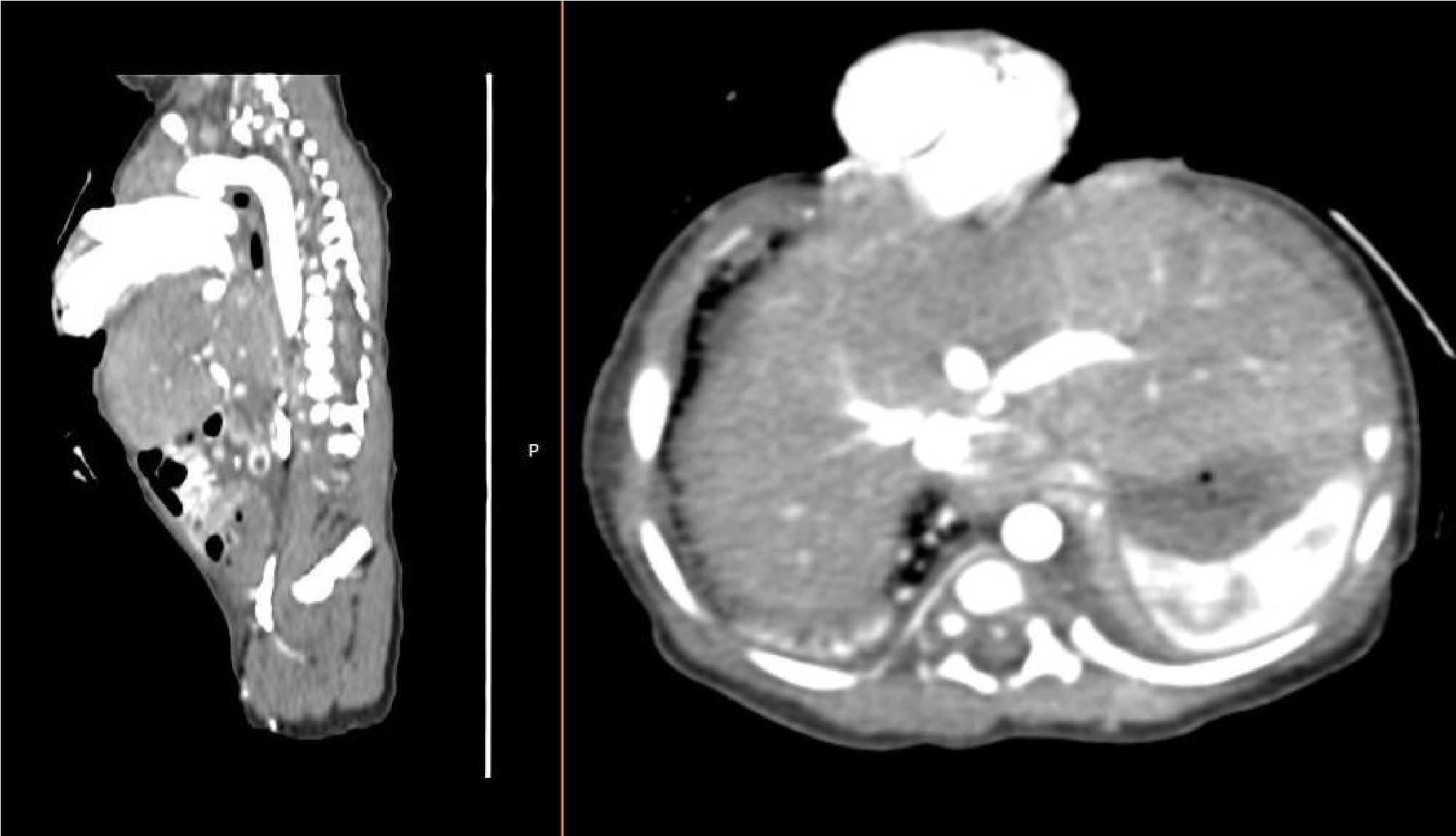
Figure 1: CT of the newborn. Both ventricles are located extrathoracic protruding through a defect in the thoracic wall, which is 4 cm wide.
Two pulmonary veins on each side merge into one larger blood vessel, which flows into the enlarged left atrium. Atrioventricular concordance id normal. The left ventricle is located on the right and extrathoracic. From the left ventricle, the elongated LVOT bends towards the back and is located inside the thorax where the aorta arises from it. At the level of isthmus of the aorta there is a wide ductus arteriosus (9mm). The right ventrice location is also extrathoracic. The RVOT bends towards the back and is located intrathoracic and is elongated leading to the well-placed outlet of the pulmonary artery, with braches of appropriate size. The lung parenchyma is hypoventilated with dystelectasis and posterior ground glass areas. The domes od dyaphragm are without sings of disruption. Thorax and abdomen were performed before the transfer (Figure 1).
The echocardiogram findings did not show any intracardial malformations except for an open ductus arteriosus that was hemodynamically significant with left to right shunt. Both ventricles were located outside the thoracic wall, with four pulmonary veins entering the left atrium and cardinal veins entering the right atrium.
Newborn was transferred in the Neonatal Intensive Care Unit (NICU) of our institution on the 5th day of life for surgical management of ectopia cordis where he was examined by neonatologists, cardiac and abdominal surgeons, and anesthesiologists. After the multidisciplinary consultation, informed consent was obtained from the parents.
The patient was referred to the operating room on the 6th day of life spontaneously breathing, tachydyspnoic, hemodynamically stable, with a urinary catheter and peripheral venous access on the dorsum of the right hand. The sternal and abdominal defect was covered with a sterile moist dressing to prevent desiccation.
Given the existence of retrognathia, a lowered tip of the nose, as well as a defect of the anterior thoracic wall, difficult intubation was expected. Standard ASA monitoring was set. Prophylactic antibiotics were administered upon arrival to operating room.
After preoxygenation, the induction of anesthesia with midazolam 0.3 mg/kg, sufentanil 0.3 mcg/kg and neuromuscular relaxation with rocuronium 0.6 mg/kg was administered. He was intubated with a direct laryngoscope with a flat spatula, ETT No 3 cuff. Anesthesia was maintained with sevoflurane in an oxygen/air mixture, continuous analgesia with sufentanil 0.6 mcg/kg/h along with rocuronium boluses for neuromuscular relaxatio. The child was ventilated with a pressure control form of ventilation. Monitoring during the procedure included: 5-channel ECG, SpO2, capnography, Sedline, central arterial catheter, central venous catheter and temperature probe (Figure 2).
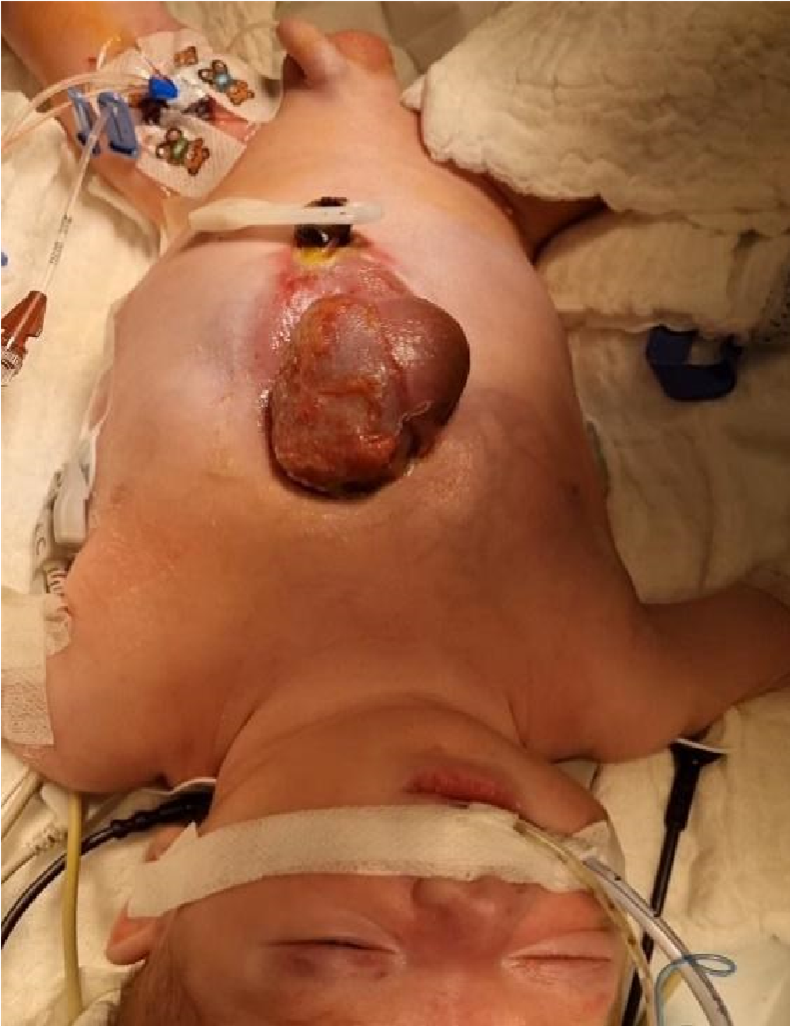
Figure 2: Picture after induction of anesthesia.
During the first operative procedure after enlargement of sternal defect patent ductus arteriosus was closed. When the heart was placed in the thoracic cavity hypotension and signs of low cardiac output state occurred and we opted for inotropic support with epinephrine 0.05 mcg/kg/min. Optimizing the volume status was paramount avoiding the volume overload while maintaining adequate preload bearing in mind possible compression of great vessels and multiple organ systems – heart, lungs as well as abdominal structures. In addition to hemodynamic instability, hypoxia occurred and inspiratory fraction of oxygen risen to 100% when the chest wall was partially closed (Figure 3). Through the course of 3 operations, the defect was successfully closed only with skin and soft tissue (Figure 4).
Pediatric intensivists where able to wean the patient of inotropic support in the next few days, which was followed by weaning from the ventilator and extubation. Following first extubation, paresis of the left diaphragm was observed after which tracheotomy was
performed. The patient was successfully weaned from the ventilator with proper gas exchange through a tracheal cannula (3,5 mm; no cuff).
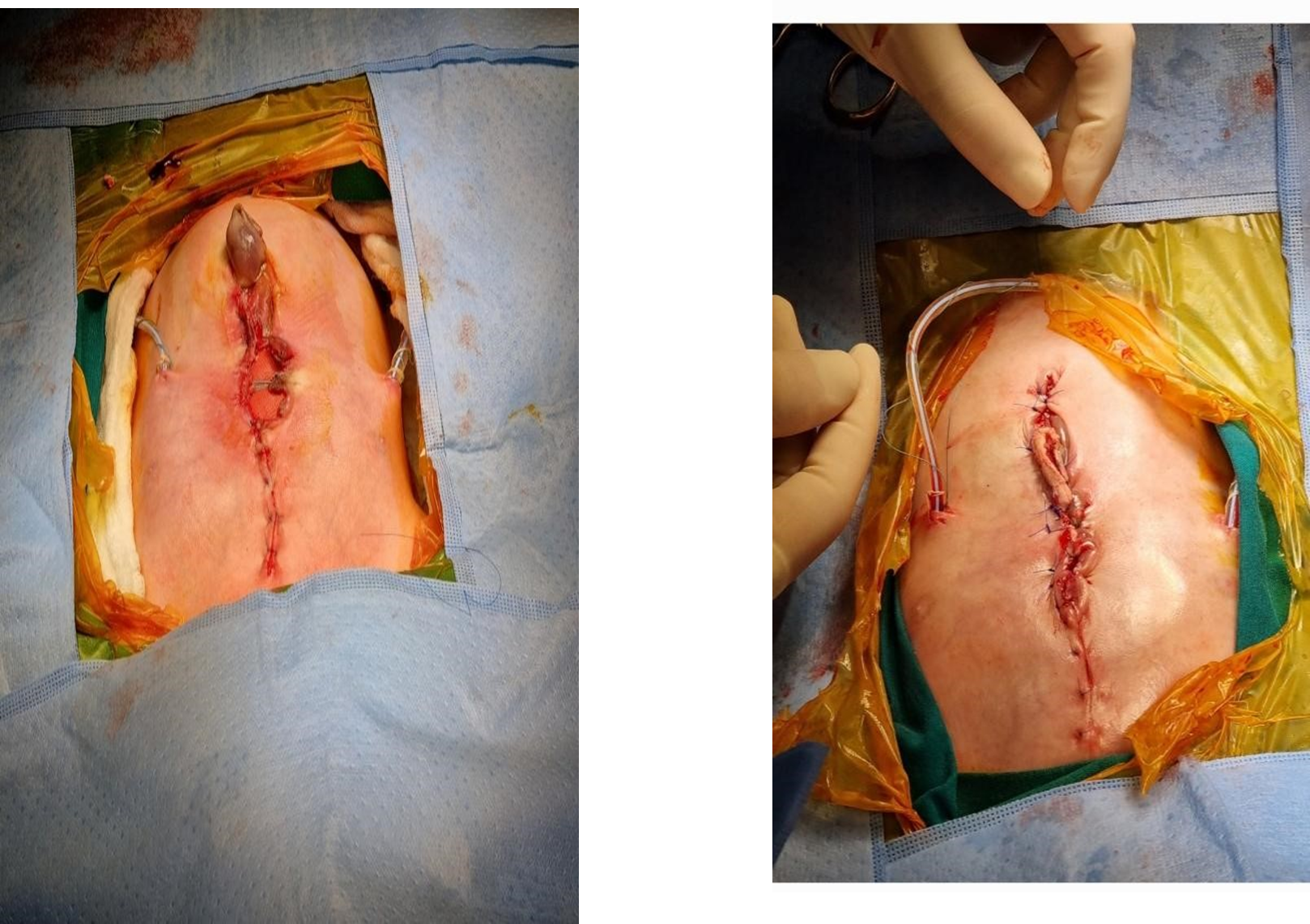
Figure 3: Results following the 1st procedure.
Figure 4: Results following the 3rd procedure.
Discussion
In the majority of cases with ectopia cordis the prognosis is poor and most infants are still born or die within the first few days of life. The mortality rate is the highest within the group of patients that have associated malformations. This is especially true for patients that have pentalogy syndrome described by Cantrell in 1958. It consists of distal sternum defect, midline supraumbilical abdominal wall defect, ventral diaphragmatic hernia, defect of the apical pericardium with free communication into the peritoneal cavity, and congenital intracardiac defects.
Ultimate survival of these patients depends on the presence or absence of intrinsic cardiac defects. These disorders can result in stillbirth or death in early neonatal period in most cases due to cardiac complications such as cardiac rupture, tamponade, endocarditis, arrhythmias and sudden cardiac death [8].
Only small number of postpartum newborn have been successfully treated and have survived. The goal of early management is to cover the naked heart with skin or synthretic material, followed by enlarging the thoracic cage and placing the heart into the thoracic cavity without compromising hemodynamic and respiratory stability [9].
Junior et al [1] published an article describing four cases of full term newborn with ectopia cordis and associated cardiac anomalies that underwent different treatment approaches with main initial goals being covering the heart with a soft tissue and placing the heart in thoracic cavity. According to them, the most important factor in initial survival is exposure and adequate tissue cover. Our patient had partial cover of the heart with skin, and no accompanied cardiac malformation.
From the published literature, there is only one described case of uncorrected ectopia cordis by Jahan et al. The patient was 6-year-old boy with EC of thoracic localization was first presented in because of the need for corrective surgery for defect closure [10].
Our patient was full term newborn with thoracic presentation of ectopia cordis, without associated cardiac malformations. We were able to close the sternal and abdominal defect with skin and soft tissue. His main complication was weaning of ventilator support, which is why tracheotomy was perfomed with successful result.
Conclusion
Ectopia cordis is a serious anomaly associated with high morbidity and mortality, and associated cardiac disorders determine the prognosis in most cases of ectopic heart.
Even after initial stabilization and corrective surgery, patients with ectopia cordis experience considerable postnatal morbidity and mortality due to increased risk of infection, underdevelopment of the lung, as well as the lack of space in the thoracic cavity and the immaturity of multiple organ systems, especially related to maturity and birth weight.
References
- Araujo Júnior E, Coutinho LG, Bravo-Valenzuela NJ, Aquino P, Rocha LAD, Rizzo G, et al. Ectopia cordis: prenatal diagnosis, perinatal outcomes, and postnatal follow-up of an international multicenter cohort case series. J Matern Fetal Neonatal Med, 2023; 36(1): 2203791. doi: 10.1080/14767058.2023.2203791.
- Gabriel A, Donnelly J, Kuc A, Good D, Doros G, Matusz P, loukas M. Ectopia cordis: A rare congenital anomaly. Clin. Anat., 2014; 27: 1193-1199.
- Nzomvuama A, Nader J, Remendi JP. Ectopia Cordis: An Uncommon Fatal Disease. Ann Thorac Surg. 2021; 112.
- Shad J, Budhwani K, Biswas R. Thoracic ectopia cordis: BMJ Case Reo, 2012; 2021: bcr11120115241. doi: 10.1136./bcr.11.2011.5241.
- Yıldız K, Kır M, Uğurlu ŞB, Genç HZ, Ünal N. Four ectopia cordis cases surgically managed with different strategies. Turk Gogus Kalp Damar Cerrahisi Derg, 2021; 29(1): 114-118. doi: 10.5606/tgkdc.dergisi.2021.19791.
- Pius Simon, AbubakarIbrahim Halima, Bello Mustapha, Bashir Tahir Mohammed. Complete Ectopia Cordis: A Case Report and Literature Review, Case Reports in Pediatrics, 2017; 1858621: 6.
- Smith BJ, Flyer JN, Edwards EM, et al. Outcomes for ectopia cordis. J Pediatr, 2020; 216: 67-72.
- Rashidighader F, Khorgami M, Caruso E, Silvia F, Masihi R. A Case of Antenatal Diagnosis of Ectopia Cordis with Cardiac Disease. CRCP, 2023; 8(1): 34-38.
- Thakur VA, Agrawal P, Vishnoi K, et al. Ectopia Cordis: Case of an Early Diagnosis and Review of Literature. J. Fetal Med, 2022; 9: 105–108.
- Jahan Y, Rahman A. Ectopia Cordis: 6-Year Survival without Surgical Correction. Fetal Pediatr Pathol, 2021; 40(5): 540-542. doi: 10.1080/15513815.2019.1710878.

