Scleroderma Renal Crisis with Digital Ischemia in Limited Cutaneous Systemic Sclerosis
Allaw Ghadir1, Khazzaka Lynn2, Mahdi Mohammad2 and El Mawla Zeinab3,*
1Department of Nephrology, Sahel Hospital, Beirut, Lebanon
2Faculty of Medicine, Lebanese University, Beirut, Lebanon
3Faculty of Medicine, Department of Pulmonary & Critical Care, Lebanese University, Beirut, Lebanon
Received Date: 27/10/2025; Published Date: 05/12/2025
*Corresponding author: El Mawla Zeinab, Faculty of Medicine, Department of Pulmonary & Critical Care, Lebanese University, Beirut, Lebanon
Abstract
Background: Systemic sclerosis (SSc) is a chronic autoimmune connective tissue disorder characterized by immune dysregulation, progressive fibrosis, and widespread vasculopathy. Scleroderma renal crisis (SRC) is a rare, potentially fatal complication, more common in diffuse cutaneous SSc but occasionally seen in limited variants such as CREST syndrome. Digital ischemia is another severe manifestation of SSc vasculopathy, which may lead to tissue necrosis.
Case Presentation: We report a 52-year-old male with known CREST syndrome who presented with nausea, vomiting, dizziness, and diffuse abdominal pain. Examination revealed necrotic fingertips due to critical ischemia. Laboratory findings demonstrated acute kidney injury (creatinine 3.9 mg/dL) and high-anion gap metabolic acidosis. Blood pressure was 180/80 mmHg. The patient received supportive care, resumed home medications, and started Rituximab for progressive cutaneous involvement. Partial renal recovery was observed (creatinine 2.3 mg/dL), and digital amputation was planned due to irreversible necrosis.
Discussion: This case highlights that limited cutaneous SSc can be complicated by life-threatening SRC and severe digital ischemia. Systemic vascular involvement underscores the need for early recognition and timely management to prevent morbidity and mortality.
Conclusion: Clinicians should remain vigilant for SRC and digital ischemia in patients with limited SSc. Prompt diagnosis and targeted management are critical for improving outcomes.
Keywords: Systemic sclerosis; CREST syndrome; Scleroderma renal crisis; Digital ischemia; Vasculopathy; Case report
Introduction
Systemic sclerosis (scleroderma) is a chronic autoimmune connective tissue disorder characterized by immune dysregulation, progressive fibrosis, and widespread vasculopathy affecting the skin and internal organs. Although the precise pathogenesis remains incompletely understood, endothelial injury, immune activation, and abnormal fibroblast function collectively contribute to tissue fibrosis and organ dysfunction [1]. Clinically, SSc is classified into diffuse cutaneous systemic sclerosis (dcSSc) and limited cutaneous systemic sclerosis (lcSSc). The latter is often referred to as CREST syndrome, an acronym for calcinosis, Raynaud’s phenomenon, esophageal dysmotility, sclerodactyly, and telangiectasias [1,2]. The global prevalence of SSc is estimated at 18.87 cases per 100,000 individuals [2].
Raynaud’s Phenomenon (RP), a hallmark of SSc, represents an exaggerated vascular response to cold or emotional stress. While RP may be idiopathic, it is frequently secondary to connective tissue diseases and can progress to digital ischemia, ulceration, or gangrene in severe cases [3,4]. Another serious and potentially fatal complication is Scleroderma Renal Crisis (SRC), which occurs in approximately 20% of affected patients. SRC is characterized by sudden-onset malignant hypertension and acute kidney injury, and despite advances with Angiotensin-Converting Enzyme Inhibitors (ACEi), it remains a medical emergency [3].
We present a case of limited cutaneous systemic sclerosis complicated simultaneously by SRC and critical digital ischemia. This report illustrates the systemic nature of SSc vasculopathy, emphasizes the importance of early recognition of life-threatening complications, and demonstrates the need for timely, targeted management to optimize patient outcomes.
Case Presentation
A 52-year-old male with a history of limited systemic sclerosis (CREST syndrome), pulmonary arterial hypertension, and hypertension treated with Ramipril, presented to the hospital with nausea, vomiting, dizziness, and diffuse abdominal pain. His home medications included mycophenolate mofetil and systemic corticosteroids.
On examination, the patient exhibited blackish discoloration and necrosis of the fingertips, (Figure 1) most pronounced at the terminal tufts, consistent with dry gangrene due to critical ischemia. The surrounding skin appeared shiny and taut, reflecting underlying sclerodermatous changes. No other significant organ abnormalities were observed.
Vital signs on admission were notable for a blood pressure of 180/80 mmHg, heart rate of 56 bpm, oxygen saturation of 98% on room air, and afebrile temperature. Laboratory evaluation revealed serum creatinine of 3.9 mg/dL (normal 0.7–1.3 mg/dL) and serum bicarbonate of 13 mmol/L (normal 22–29 mmol/L). C-reactive protein was mildly elevated at 3.2 mg/L, while other laboratory values were unremarkable. Arterial blood gas analysis showed a pH of 7.151, PaCO₂ of 25 mmHg, and HCO₃⁻ of 9 mmol/L, consistent with high-anion gap metabolic acidosis with partial respiratory compensation.
The patient received intravenous hydration, optimization of blood pressure, and close monitoring of renal function. His home medications were resumed, and Rituximab therapy was initiated for progressive cutaneous involvement. During hospitalization, clinical status improved and serum creatinine decreased to 2.3 mg/dL, indicating partial renal recovery. Due to irreversible tissue necrosis and risk of infection, the medical team recommended amputation of the affected fingers.
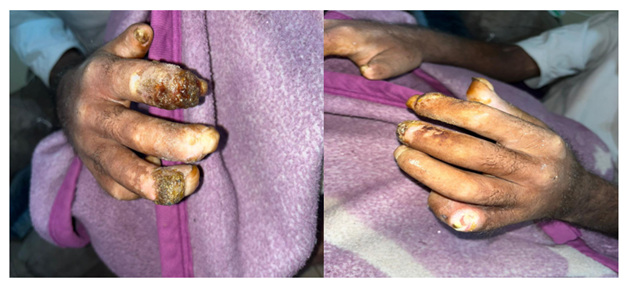
Figure 1: Image showing blackish discoloration and necrosis of the fingertips.
Discussion
Scleroderma renal crisis is a rare but potentially fatal complication characterized by abrupt-onset malignant hypertension and rapidly progressive acute kidney injury. Vasculopathy of the renal arterioles leads to endothelial injury, intimal proliferation, luminal narrowing, renal ischemia, and activation of the renin-angiotensin-aldosterone system, perpetuating hypertension and kidney injury [5,6]. While SRC most frequently occurs in early, rapidly progressive diffuse cutaneous SSc, this case demonstrates that limited cutaneous SSc can also be affected.
Our patient presented with nausea, vomiting, dizziness, and diffuse abdominal pain, reflecting uremia. Laboratory evaluation confirmed acute kidney injury with high-anion gap metabolic acidosis and partial respiratory compensation, accompanied by severe hypertension. Partial renal recovery following supportive care and ACE inhibitor therapy emphasizes the importance of early recognition and prompt intervention in SRC, even in patients already receiving ACE inhibitors [7].
In addition, the patient exhibited severe digital ischemia with fingertip necrosis, highlighting systemic vascular involvement in SSc. Chronic Raynaud’s phenomenon, microvascular constriction, and compromised tissue perfusion contribute to the development of digital ulcers and gangrene. In advanced cases, irreversible necrosis necessitates surgical intervention to prevent infection and further systemic complications [4,8]. Cutaneous manifestations, including skin tightness, pigmentary changes, telangiectasias, and calcinosis, serve both diagnostic and prognostic roles, reflecting disease severity and vascular compromise [9]. The coexistence of SRC and digital necrosis in this patient underscores the extensive, systemic vasculopathy of SSc and highlights the need for vigilant monitoring for multi-organ involvement.
Conclusion
Limited cutaneous systemic sclerosis, while traditionally associated with lower risk of renal involvement, can present with life-threatening scleroderma renal crisis. The simultaneous presence of digital ischemia further illustrates systemic vascular compromise. Clinicians should maintain vigilance for SRC and peripheral vascular complications in limited SSc, ensuring early recognition and prompt, targeted management to prevent irreversible organ and tissue damage.
References
- Kowalska-Kępczyńska A. Systemic Scleroderma—Definition, Clinical Picture and Laboratory Diagnostics. J Clin Med, 2022; 11(9): 2299.
- Tian J, Kang S, Zhang D, Huang Y, Zhao M, Gui X, et al. Global, regional, and national incidence and prevalence of systemic sclerosis. Clin Immunol, 2023; 248: 109267.
- Cole A, Ong VH, Denton CP. Renal Disease and Systemic Sclerosis: an Update on Scleroderma Renal Crisis. Clin Rev Allergy Immunol, 2022.
- McMahan ZH, Wigley FM. Raynaud’s phenomenon and digital ischemia: a practical approach to risk stratification, diagnosis and management. Int J Clin Rheumatol, 2010; 5(3): 355–370.
- Hussein MS, Alshammari F, Sultan F, et al. Overview of Scleroderma Renal Crisis—a review. J Pharm Res Int, 2021; 4: 334–340.
- Woodworth TG, Suliman YA, Furst DE, Clements P. Scleroderma renal crisis and renal involvement in systemic sclerosis. Nat Rev Nephrol, 2016; 12(11): 678–691.
- Steen VD, Costantino JP, Shapiro AP, Medsger TA. Outcome of renal crisis in systemic sclerosis: relation to availability of angiotensin converting enzyme (ACE) inhibitors. Ann Intern Med, 1990; 113(5): 352–357.
- Schiopu E, Impens AJ, Phillips K. Digital Ischemia in Scleroderma Spectrum of Diseases. Int J Rheumatol, 2010; 2010: 1–8.
- Pearson DR, Werth VP, Pappas-Taffer L. Systemic sclerosis: Current concepts of skin and systemic manifestations. Clin Dermatol, 2018; 36(4): 459–474.

