A Rare Case of Multifocal Hydatidosis: Imaging Insights into Mediastinal, Splenic, Renal, and Peritoneal Localizations
Ismail Neftah*, Fariss Dehayni, Nidal El Hassani, Hafsa Riache, Ittimade Nassar and Kaoutar Imrani
Department of Central Radiology, Ibn Sina Hospital, Faculty of Medecine and Pharmacy of Rabat, Morocco
Received Date: 28/10/2025; Published Date: 14/11/2025
*Corresponding author: Ismail Neftah, Department of Central Radiology, Ibn Sina Hospital, Faculty of Medecine and Pharmacy of Rabat, Morocco
Abstract
Hydatid disease, caused by the larval stage of Echinococcus granulosus, remains a significant public health concern in many developing and livestock-raising regions. Humans are accidental intermediate hosts, and infection occurs through ingestion of parasite eggs. The disease typically affects the liver and lungs, which account for nearly 90% of cases. However, hydatid cysts can occasionally develop in unusual locations such as the spleen, mediastinum, kidneys, and peritoneum. The coexistence of multiple atypical localizations in the same patient is exceedingly rare and poses both diagnostic and therapeutic challenges.
Keywords: Hydatid disease; Echinococcus granulosus; Mediastinal hydatid cyst; Hepatic hydatid disease; Splenic hydatid disease; Renal hydatid cyst; Peritoneal hydatid disease; Radiology; CT scan; MRI
Introduction
Hydatid disease, also known as cystic echinococcosis, is a parasitic zoonosis caused by the larval stage of Echinococcus granulosus. It remains an important public health concern in endemic regions. The disease primarily affects the liver (in about 60–70% of cases) and the lungs (20–30%), reflecting the typical route of hematogenous dissemination [1].
However, involvement of atypical sites such as the spleen, mediastinum, kidneys, and peritoneum is rare, occurring either as isolated manifestations or secondary to rupture or dissemination of a primary cyst. Multivisceral hydatidosis is exceptionally uncommon and often poses diagnostic and therapeutic challenges due to its variable clinical presentation and the potential for complications such as cyst rupture, infection, or compression of adjacent structures [2].
Imaging plays a central role in the diagnosis, characterization, and staging of hydatid disease. Ultrasound and computed tomography (CT) remain the cornerstone techniques for detecting cystic lesions, assessing their viability, and evaluating complications. Magnetic resonance imaging (MRI) may further contribute by providing superior tissue characterization, particularly in atypical locations or complex cases.
Clinical Observation
A 70-year-old patient from an endemic area presented with chest and abdominal pain, heaviness in the left hypochondrium, dyspnea, and episodes of lower back pain. The patient had no significant past medical history. On clinical examination, he was febrile and reported an unquantified weight loss.
- Biology: positive hydatid serology.
- The chest X-ray revealed indirect signs suggestive of a mediastinal mass:
-Well-defined mediastinal opacity.
-Deviation of adjacent structures, including the trachea and pulmonary hilum.
-Elevation of the left hemidiaphragm.
- Ultrasound is the first-line modality for the abdominal assessment.
It allows identification of the cystic nature, number, size, and localization of the lesions. - Spleen: Rounded anechoic lesions within the splenic parenchyma, the largest containing internal daughter cysts.
- Left kidney: Corticomedullary cystic mass with a thin wall and posterior acoustic enhancement.
- Peritoneum: Multiple free cystic formations with daughter vesicles.
- CT imaging revealed multiple well-defined cystic formations with thin, regular walls and heterogeneous internal content, consistent with hydatid cysts. Several cysts showed areas of varying density, corresponding to daughter vesicles and detached membranes, producing the characteristic “water-lily” and “rosette” appearances. These lesions were distributed in the mediastinum, peritoneal cavity, spleen, and both kidneys, causing mass effect on adjacent structures without signs of invasion. Some cysts demonstrated calcified walls, suggesting chronic evolution, while others retained a typical fluid density, indicating different stages of disease activity.
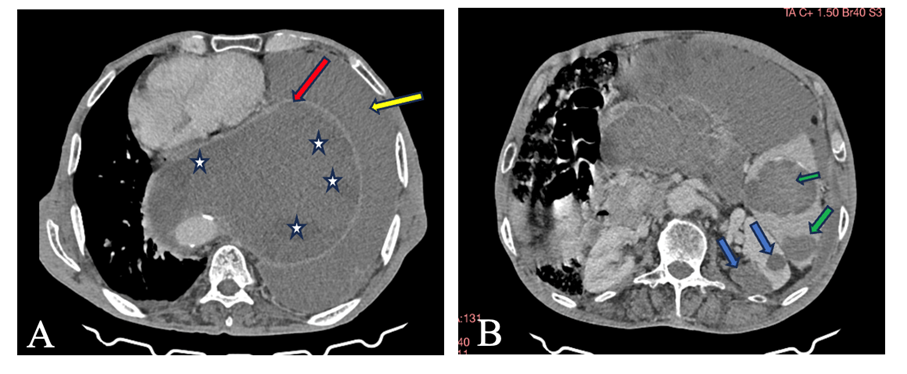
Figure A: Axial CT scan with contrast injection, large cystic posterior mediastinal mass (red arrow) with areas of variable density (daughter cysts) (white stars).
Large left pleural effusion (yellow arrow).
Figure B: Axial CT scan with contrast injection, cystic formations with the same characteristics in the spleen (green arrows) and left kidney (blue arrows).
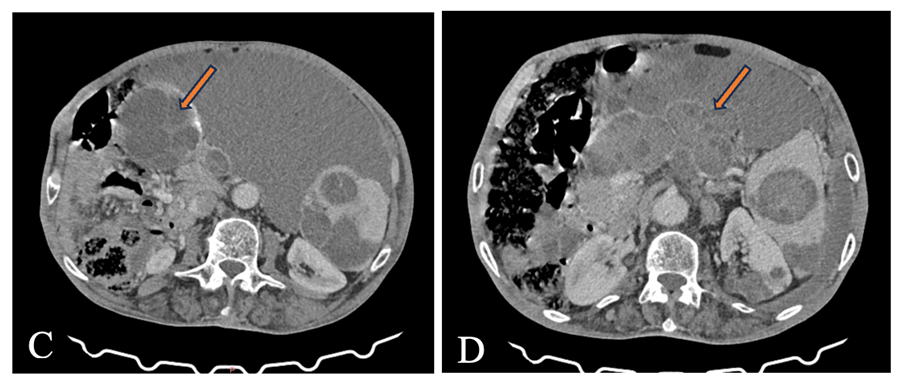
Figures: Abdominal CT scan with contrast injection, showing multiple intraperitoneal cystic formations in the right flank (Figure C) and the antro-pyloric region (Figure D).
Evolution
The postoperative course was initially stable under albendazole therapy and supportive care. However, the patient’s condition progressively deteriorated within a few days, with the onset of persistent fever, increasing dyspnea, and signs of septic shock. Despite intensive management in the intensive care unit, including broad-spectrum antibiotics and hemodynamic support, the patient developed multiorgan failure. Unfortunately, he passed away ten days after surgery due to septic complications related to the extensive dissemination of the hydatid disease.
This unfavorable outcome highlights the severity and complexity of multifocal hydatidosis involving vital structures such as the mediastinum, spleen, kidneys, and peritoneum, where the disease burden and risk of postoperative infection are particularly high.
Discussion
The coexistence of mediastinal, splenic, renal, and peritoneal locations is an exceptional presentation. Multimodal imaging is essential for: Detecting lesions, mapping all locations and guiding the therapeutic strategy.
Imaging plays a crucial role in the diagnosis and assessment of multifocal hydatidosis.
In the mediastinum, chest CT typically reveals a thin-walled, non-enhancing hypodense cystic mass that may exert compressive effects on adjacent structures such as the heart or great vessels [2]. MRI provides complementary information, showing a hypo-intense signal on T1-weighted images and a hyper-intense signal on T2-weighted sequences, with thin internal septations and improved visualization of anatomical relationships [3].
In the spleen, ultrasound generally demonstrates a well-defined, rounded anechoic lesion with internal septations, while CT shows a hypodense mass that may occasionally present peripheral calcifications. On MRI, the cystic nature appears clearly with a high T2 signal and a well-defined wall.
Renal involvement, representing approximately 2–4% of all hydatid localizations, typically appears on ultrasound as a cystic lesion with internal septations and, in some cases, distortion of the excretory system [5]. Abdominal CT reveals a hypodense, multivesicular cyst with possible wall calcifications and frequent cortical extension [6]. MRI confirms the cystic pattern, showing a low signal on T1 and a high signal on T2, without internal enhancement, although the appearance may mimic a cystic renal tumor (Bosniak category II–III) [7].
Peritoneal hydatidosis is most often secondary to the rupture or dissemination of a hepatic or splenic cyst. Ultrasound identifies multiple intraperitoneal cystic formations, either free or adherent to adjacent organs [8]. On CT, these lesions appear as scattered hypodense cysts, sometimes exhibiting a multivesicular configuration. MRI, with its superior contrast resolution, shows marked T2 hyperintensity, facilitating differentiation from compartmentalized ascites or mesothelial cysts [9].
The differential diagnosis of multifocal cystic lesions includes several entities depending on the site of involvement. In the spleen, the main differentials are epidermoid cysts, bacterial abscesses, and cystic metastases. Mediastinal cystic lesions may mimic bronchogenic cysts, lymphangiomas, or cystic germ cell tumors. In the kidney, differential considerations include cystic renal tumors categorized by the Bosniak classification and pyogenic abscesses. Peritoneal cystic formations can be confused with compartmentalized ascites, mesothelial cysts, or peritoneal carcinomatosis. However, the presence of radiological features characteristic of hydatid disease—such as multivesicularity, internal septations, peripheral calcifications, and the coexistence of lesions in multiple locations—strongly supports the diagnosis of hydatidosis.
The management of hydatid disease combines medical and surgical approaches, depending on the location, size, and impact of the cysts.
Medical treatment relies primarily on benzimidazole derivatives, with albendazole being the drug of choice, administered at a dose of 10–15 mg/kg/day divided into two daily doses, in 28-day cycles separated by 14-day intervals. Mebendazole can be used as an alternative in cases of intolerance. The main objectives of antiparasitic therapy are to reduce the viability of the parasite prior to surgery, prevent secondary dissemination, and treat small or inoperable cystic lesions. Close biological monitoring of hepatic function and blood count is mandatory throughout treatment to detect potential drug-related toxicity.
Surgical treatment remains essential in cases where cysts are large, symptomatic, or exert compressive effects. The approach varies according to the site of involvement.
For mediastinal localizations, surgery via thoracotomy or video-assisted thoracoscopic surgery (VATS) is indicated, aiming for complete excision of the cyst without rupture to prevent dissemination or anaphylactic shock. The residual cavity should be irrigated with a scolicidal solution such as hypertonic saline, hydrogen peroxide, or 20% sodium chloride.
For splenic, renal, or peritoneal localizations, surgical management includes cystectomy or partial/total pericystectomy, depending on accessibility and extent. Total splenectomy is performed in cases of diffuse splenic involvement, while partial or total nephrectomy may be necessary for destructive renal forms. Peritoneal cysts are managed by simple excision or drainage, depending on the degree of dissemination.
Conclusion
Multifocal hydatid disease involving the mediastinum, peritoneum, spleen, and kidneys is a rare and complex presentation. Imaging plays a central role in recognizing specific features, ruling out differential diagnoses, and guiding management.
In endemic areas, any thoracic or abdominal cystic mass should raise suspicion of hydatid disease, especially when it is multiple and multivisceral.
References
- Suryawanshi KH, Jagtap SV, Kadam PN, et al. Multiple disseminated abdominal hydatidosis: A rare case report. Indian J Pathol Microbiol, 2009; 52(2): 240–242.
- El Fakir Y, Benali A, Chihabeddine K, et al. Multiple disseminated hydatidosis with rare locations: Mediastinal, pancreatic and pelvic. Eur J Med Health Sci, 2024; 6(1): 94–98.
- Zidi A, Zannad-Hantous S, Mestiri I, Ghrairi H, Baccouche I, Djilani H, et al. Hydatid cyst of the mediastinum: 14 case reports. J Radiol, 2006; 87: 1869-1874. doi:10.1016/S0221-0363(06)74167-1.
- Sitmangil T, Toker A, Sebit S, Erdik O, Tunc H, Gorur R. A novel terminology and dissemination theory for a subgroup of intrathoracic extrapulmonary hydatid cysts. Med Hypotheses, 2003; 61: 68-71. doi:10.1016/S0306-9877(03)00108-7.
- Gilsanz V, Lozano F, Jimenez J. Renal hydatid cysts: communicating with collecting system. AJR,1980; 135: 357–361
- Horchani A, Nouira Y, Kbaier I, Attyaoui F, Zribi AS. Hydatid cyst of the kidney: a report of 147 controlled cases. Eur Urol,2000; 38: 461–467.
- Ödev K, Kilinç M, Arslan A, et al. Renal hydatid cysts and the evaluation of their radiologic images. Eur Urol,1996; 30: 40–49.
- Hajar N, et al. Expression particulière d’une hydatidose péritonéale. J Afr Hépato-Gastroentérol, 2011; 5(2): 117-120.
- Hmoud M, Elazzouzi Y, Elazzouzi A. Peritoneal hydatidosis: A rare form of hydatid disease. Eurorad, 2023; Case 18998.

