Parasitic Brain Infection as the Initial Presentation of Newly Diagnosed HIV in a Young Female Patient
Dalia Najami-Shahin1, Razi Najar1 and Saher Srour1,2,*
1Diagnostic Radiology Department, Ziv Medical Center
2Azrieli Faculty of Medicine, Bar Ilan university, Safed Israel
Received Date: 24/10/2025; Published Date: 10/11/2025
*Corresponding author: Saher Srour, Diagnostic Radiology Department, Ziv Medical Center; Azrieli Faculty of Medicine, Bar Ilan university, Safed Israel
Abstract
Background: HIV plays an important role in predisposing immunocompromised patients with low CD 4 counts to variety of opportunistic infections including cerebral toxoplasmosis [1] characterized classically by involving specific locations such as basal ganglia, cortico-medullary junction and thalamus lesion [2].
Case Presentation: our case present atypical radiological presentation of neurotoxoplasmosis in a previously healthy young female who was found to have newly diagnosed HIV concomitant with cerebral toxoplasmosis.
Discussion: the importance of this case is to highlight the role of neuroimaging methods in establishing diagnosis as well as to raise suspicion of parasitic brain infection even with atypical radiological presentation as well as the importance of MRS role in establishing diagnosis.
Conclusion: despite the atypical radiological presentation and incompatibility of clinical presentation and radiological findings early recognition and integration are essential to avoid miss diagnosis and guide timely management.
Keywords: Atypical; Immunocompromised; Basal ganglia; MRS; Neuro-toxoplasmosis
Introduction
Neuro-toxoplasmosis is an opportunistic infection caused by toxoplasma gondii, an intracellular protozoon that infects humans via direct contact of cat feces and undercooked meat unwashed fruits and vegetables [3].
Acute infection is usually asymptomatic in immunocompetent system; it can become latent in neuroparenchyma [2]. The latent infection can be reactivated in patients who are immunocompromised or low CD 4 counts such as in HIV patients [1,2]. acute encephalitis constitutes an unusual initial manifestation.
Neurological symptoms are nonspecific like headache, fever dizziness and altered consciousness [3].
Radiological representative presentation is multiple rings enhancing abscess, centered in basal ganglia corticomedullary junction and thalamus with variable degree of enchantment according to immune system, it can have nodular enhancement in immunocompetent patient and can be even absent in immunocompromised [2,3]. Characteristic sign is target sign (Figure 1) [4]. The lesion is accompanied by edema and mass effect [2].
Clinical diagnosis classically made by a response to empirical treatment of pyrimethamine-sulfadiazine and folic acid that show a reduction in lesion size after around 10 days [2].
Case Report
a previously healthy 41-year-old female tourist presented to our outpatient clinic for interpretation of recent symptoms of headache, dizziness as well as complains about recent fever two days prior to her presentation. Her vital signs were stable and neurological physical examination was average. LAB results were normal CRP and mild leukopenia.
She initiated with NCCT (non-contrast enhanced CT) that showed hypo-dense poorly defined lesion at the base of left frontal lobe, she continued with CECT (contrast-enhanced CT) that showed no defined enhancement (Figure 2, 3).
The initial suspected diagnosis assumed is a primary malignancy of astroglial tumor or a secondary metastasis. On the other hand, inflammation was another category in differential diagnosis such as encephalitis or focal brain abscess.
MRI was recommended.
Result of MRI was at T1WI hypointense lesion as seen on (Figure 4), at fluid sensitive sequences T2WI \ FLAIR the lesion is hyperintense as shown in (Figure 5), after GAD enhancement there's irregular ring enhancement of the lesion (Figure 6). Followed by vasogenic edema that is visible in flair sequence at the medial aspect of base of frontal lobe that also affects the head of caudate nucleus. No diffusion restriction was seen in DWI and ADC sequences (Figure7a,7b). In SWI there's no detection of blood products.
On paralleled examination, LP was done that showed increased level of lymphocytes and protein and normal glucose level. These results made a high suspicion of lesion secondary to immunocompromised system and raised suspicion of lymphoma.
Our patient continued with PET-CT scan that showed no pathological FDG uptake. MRS was suggested at this point that showed an increase level of choline with normal NAA:Cr ratio (Figure 8). These levels support brain abscess rather than lymphoma or primary glioma and increase the suspicion of infections like toxoplasmosis.
A PCR result at this point returned positive for toxoplasmosis in blood and CSF and at the same time positive for HIV.
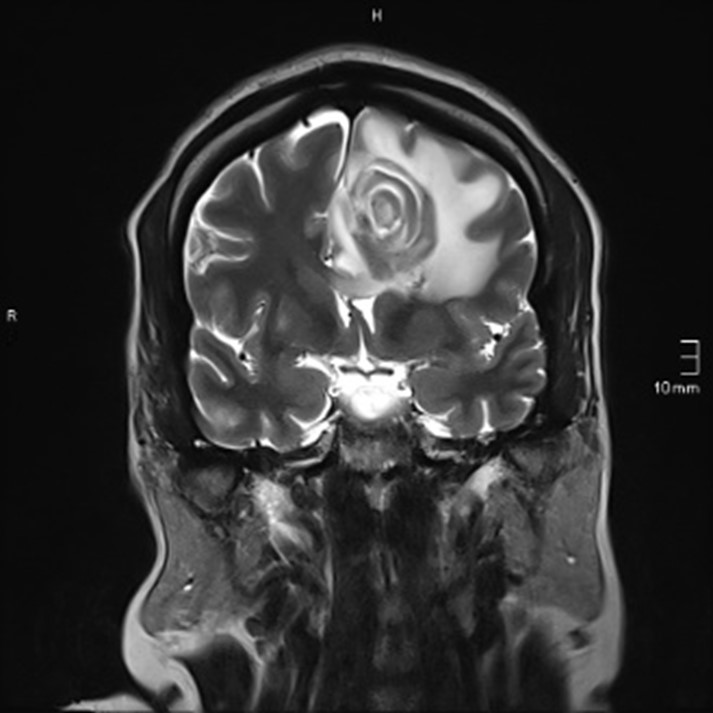
Figure 1: Coronal T2WI shows series of concentric rings with hyperintense and hypointense \isointense signals alternatingly [3].
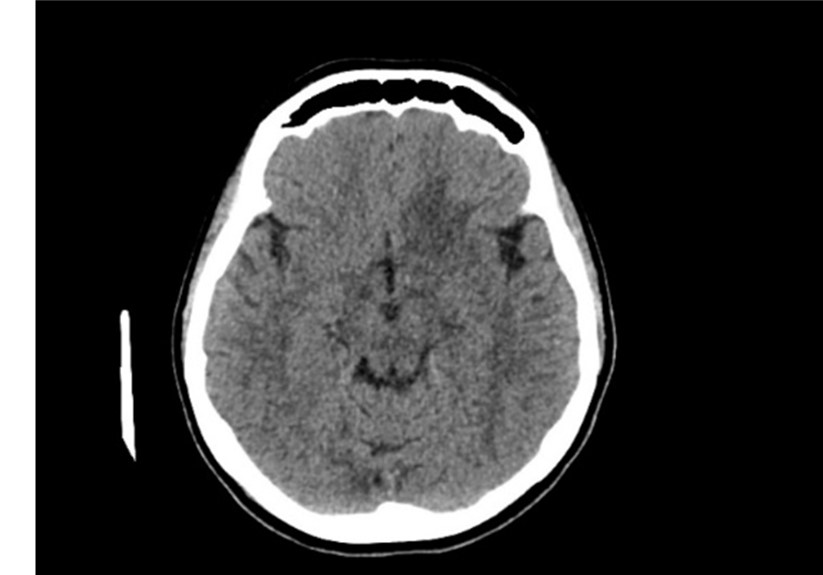
Figure 2: Axial NNCT (non-contrast enhanced CT) shows poorly defined hypodense lesion at the base of LT frontal lobe.
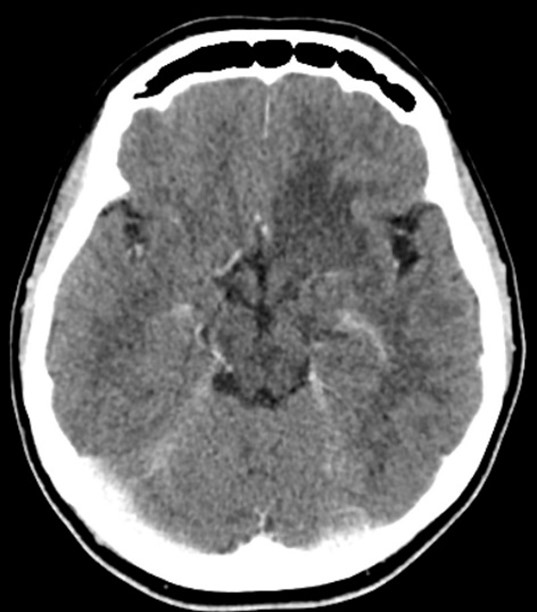
Figure 3: Axial CECT (contrast enhanced CT) shows no specific enhancement of the lesion.
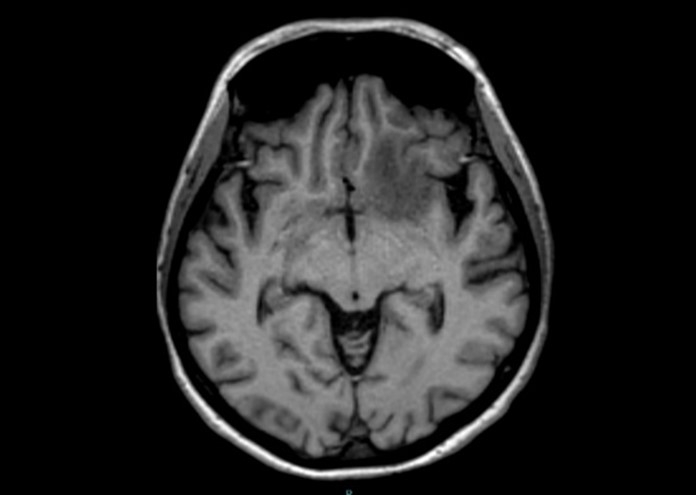
Figure 4: Axial T1WI shows hypointense lesion at the LT frontal lobe.
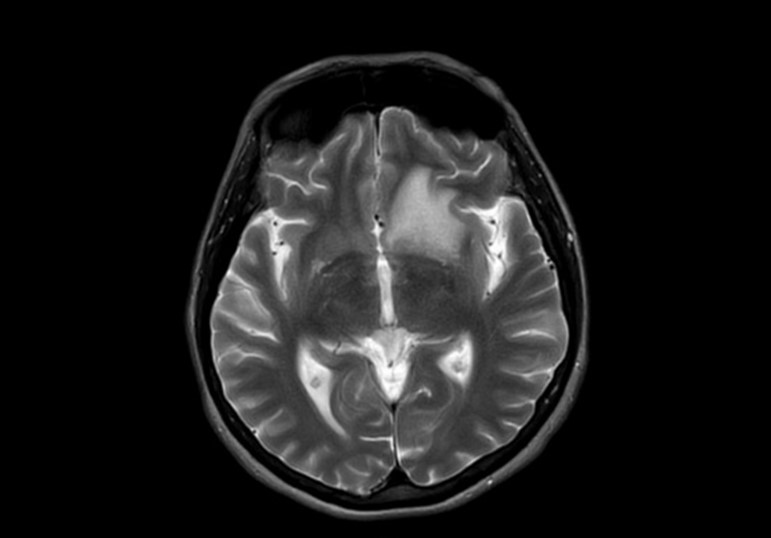
Figure 5: Axial T2WI shows hyperintense lesion.
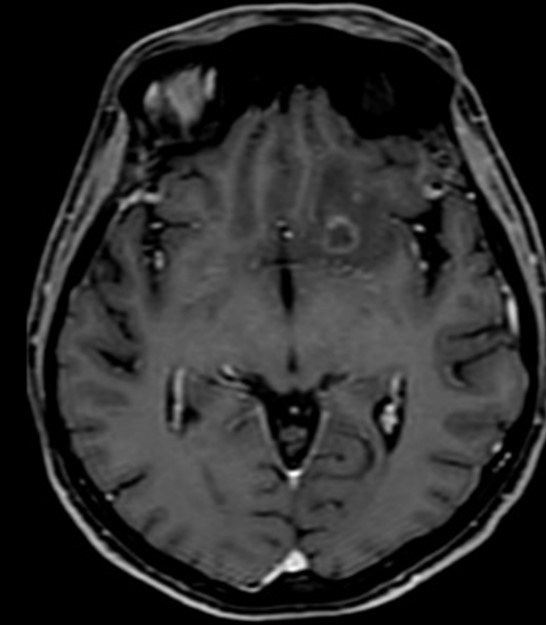
Figure 6: Axial T1+GAD shows irregular ring enhancing lesion.
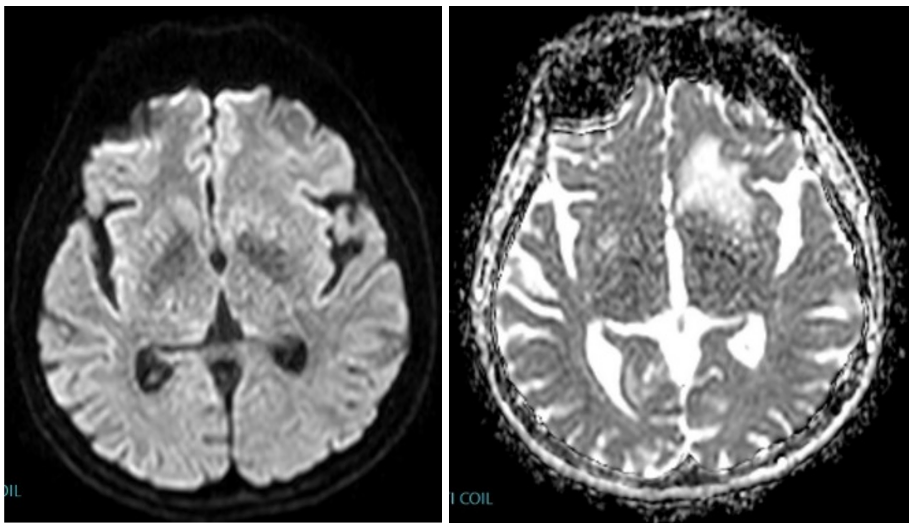
Figure 7: Axial(a) DWI and(b) ADC show no restriction in diffusion.
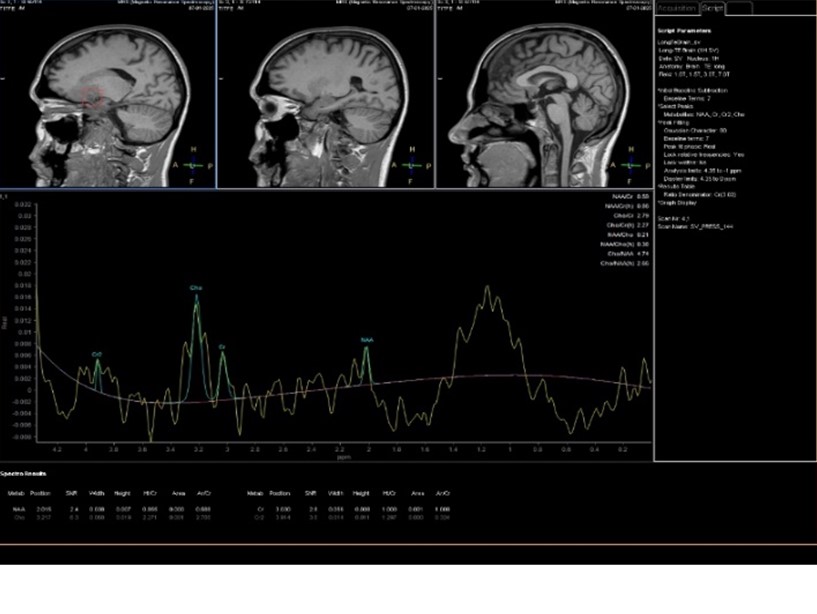
Figure 8: MRS shows increase level of choline and normal ratio of NAA and creatine.
Discussion
Although multiple ring-enhancing lesions involving basal ganglia, corticomedullary junction and thalamus are characteristic of cerebral toxoplasmosis [2], our patient presented with an isolated frontal lobe lesion which is atypical for this diagnosis.
Despite the incompatibility between radiological presentations that basically suggested a neoplasm and neurological clinical result that supported inflammatory process, our patient underwent a variety of radiological and additional examinations to eliminate a list of D.D. (differential diagnosis).
Considering laboratory and imaging findings, cerebral toxoplasmosis was identified as the most probable diagnosis and intracranial neoplasms were excluded by MRS that had important role to avoid misdiagnosis and guide timely management.
This underscores the need for high clinical suspicion of cerebral toxoplasmosis in immunocompromised patients, even when neuroimaging findings are atypical.
References
- Khandelwal N, Gupta AK, Garg A, Singh P, Gaikwad SB, Gupta V, et al. Diagnostic Radiology: Neuroradiology Including Head and Neck Imaging. 4th ed. New Delhi: Jaypee Brothers Medical Publishers, 2019.
- Gupta RK, Kharbanda S. Intracranial infections. In: Adam A, Dixon AK, Gillard JH, Schaefer-Prokop C, editors. Grainger & Allison’s Diagnostic Radiology. Philadelphia: Elsevier; 2021; 4(7): p. 1492–1507.
- Jha P. Neurotoxoplasmosis: Radiology Reference Article. Radiopaedia.org; 2025.
- Kang O. Concentric target sign (cerebral toxoplasmosis). Radiopaedia.org, 2019.

