Spontaneous Corneal Clearing After Traumatic Rupture and Detachment of Descemet’s Membrane During Phacoemulsification
Harrar Youssef*
Faculty of Medicine and Pharmacy, Mohammed Ist University, Morocco
Received Date: 21/09/2025; Published Date: 03/10/2025
*Corresponding author: Harrar Youssef, Faculty of Medicine and Pharmacy, Mohammed Ist University, Morocco
Abstract
Rupture of Descemet’s membrane is a rare complication that may lead to corneal endothelial decompensation following intraocular surgery, particularly cataract surgery.
We report a case of spontaneous corneal clearing after a Descemet’s membrane rupture in which approximately 60% of the membrane was suddenly torn during routine phacoemulsification.
This resulted in severe corneal edema, initially managed with medical therapy, which showed an excellent spontaneous recovery.
The patient achieved significant improvement in visual acuity without surgical intervention.
Through this case, we provide an updated review of the condition, its management strategies, and its clinical evolution.
Introduction
Descemet’s membrane is a dense, transparent, acellular layer that separates the corneal stroma from the underlying endothelial cells. It plays a crucial role in maintaining corneal transparency and serves as a barrier regulating the exchange of nutrients and growth factors between the corneal stroma and the aqueous humor.
The membrane has elastic properties and may regenerate after injury [1].
In ophthalmic clinical practice, Descemet’s membrane detachment (DMD) is the most frequently encountered pathology involving this structure.
DMD refers to the separation of Descemet’s membrane, along with the endothelial cell layer, from the corneal stroma [2]. It is most commonly observed during or after intraocular surgery, especially cataract surgery.
Here, we report a case of extensive rupture and detachment of Descemet’s membrane involving nearly 60% of the cornea, which surprisingly evolved with spontaneous reattachment and corneal clarity restoration, without surgical intervention.
Case Report
A 61-year-old female patient, with a history of uneventful cataract surgery in the left eye, was admitted to our department for scheduled posterior subcapsular cataract extraction in the right eye.
She had no systemic comorbidities or relevant medical history.
Phacoemulsification was performed on the right eye using the Alcon Centurion® active system. Surgery progressed smoothly until viscoelastic washout, when a whitish membrane floating in the anterior chamber and attached to the irrigation-aspiration (IA) probe was observed.
Initially suspected to be residual cortical material, it was subsequently identified as a large portion of Descemet’s membrane, which had been torn, detached, and partially aspirated by the IA probe.
The reflux function was activated, surgery was completed, and an intracameral air bubble was placed at the end of the procedure.
On postoperative day one, the patient presented with counting fingers visual acuity, epiphora, and marked corneal edema involving nearly two-thirds of the lateral cornea (Figure 1). Intraocular pressure was 16 mmHg.
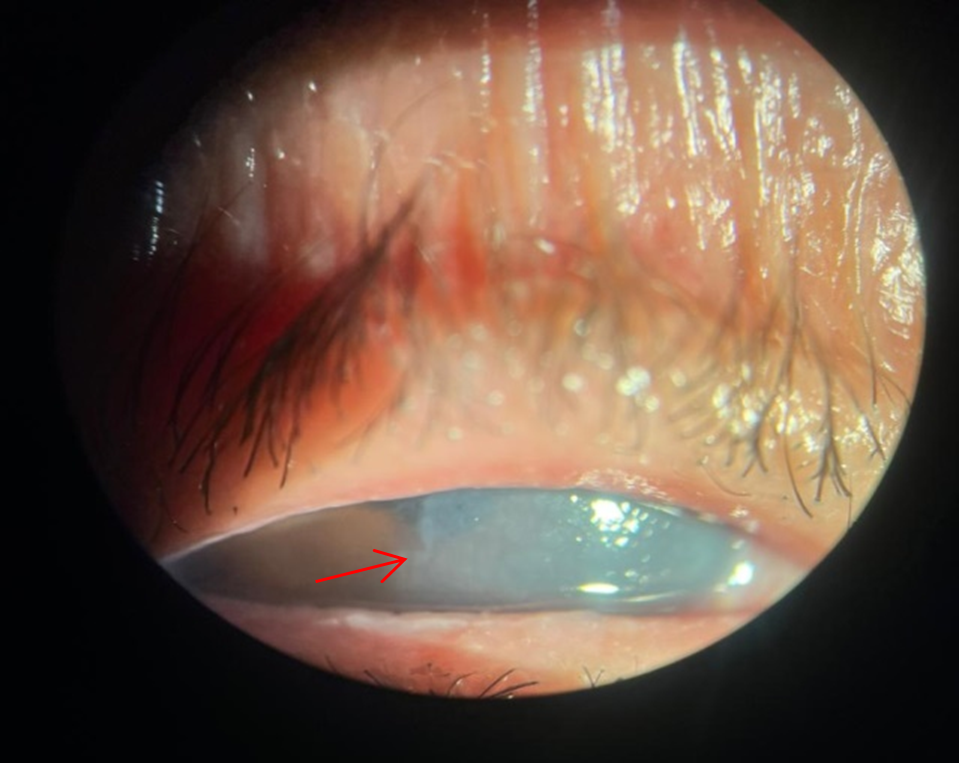
Figure 1: Slit-lamp image of the right eye on postoperative day one showing extensive corneal edema corresponding to the zone of Descemet’s membrane detachment (DMD). The red arrow indicates the margin between the clear cornea and the ruptured zone of Descemet.
Anterior segment optical coherence tomography (AS-OCT) confirmed a large Descemet’s tear and detachment associated with stromal edema (Figure 2).
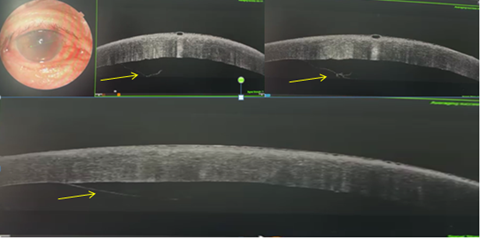
Figure 2: AS-OCT image showing extensive Descemet’s membrane detachment (yellow arrows) with stromal edema and early subepithelial bullous changes.
The patient was treated with topical hyperosmotic agents, dexamethasone drops (8 times/day for the first week, then 6 times/day during the second week), and prophylactic systemic and topical antibiotics.
At the 2-week follow-up, visual acuity had improved to 1/10 (Monoyer chart).
Slit-lamp examination demonstrated regression of corneal edema, with a well-centered intraocular lens and a persistent margin of edema delineating the area of DMD (Figure 3). OCT evaluation revealed partial reapplication of Descemet’s membrane with persistent stromal edema (Figure 4).
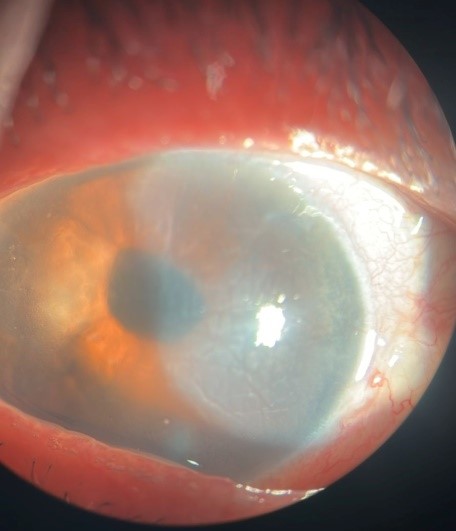
Figure 3: Slit-lamp image after 2 weeks showing regression of corneal edema localized to the nasal zone, with visible iris details and intraocular lens reflex.
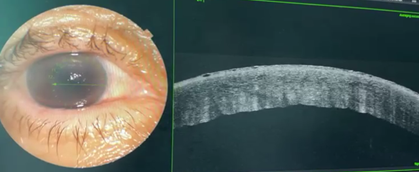
Figure 4: AS-OCT after 2 weeks showing partial reattachment of Descemet’s membrane with residual stromal edema and endothelial scarring.
Medical therapy was continued, with gradual tapering of corticosteroid drops (reduced by one instillation per week). At 6 weeks, follow-up revealed spectacular improvement, with complete corneal clearing (Figure 5) and visual acuity of 8/10.
No surgical intervention was required, suggesting spontaneous regeneration and functional recovery of Descemet’s membrane.
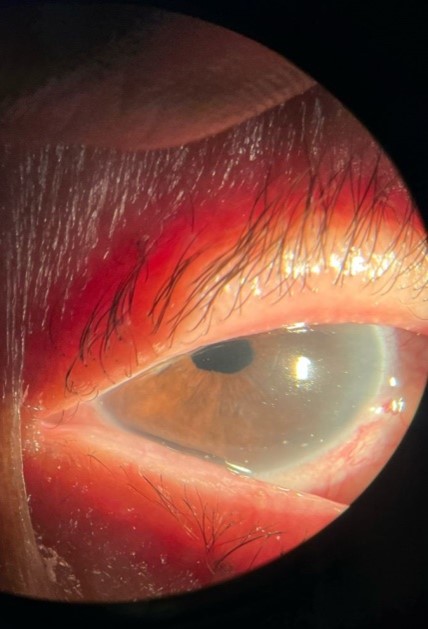
Figure 5: Slit-lamp image at 6 weeks showing a clear cornea with significant improvement compared to previous findings.
Discussion
Rupture and detachment of Descemet’s membrane (DM) are uncommon but significant complications of cataract surgery. They are usually caused by intraoperative trauma, inadvertent manipulation, or fluid turbulence during phacoemulsification [3].
Large tears often lead to persistent corneal edema and endothelial failure, which typically require surgical management such as descemetopexy or keratoplasty [4].
In our case, however, despite a rupture involving nearly two-thirds of the cornea, the patient demonstrated spontaneous corneal clearance with conservative medical therapy, underscoring the regenerative potential of the corneal endothelium and the ability of DM to reattach under favorable conditions.
Interestingly, parallels can be drawn with spontaneous visual improvement observed in certain patients with Fuchs endothelial corneal dystrophy (FECD). In FECD, despite chronic endothelial dysfunction and guttae formation, there have been reports of transient corneal clearing when endothelial cells redistribute or migrate to cover denuded areas [5]. This mechanism may share similarities with our patient’s recovery, where surviving endothelial cells likely repopulated and re-established functional integrity over the previously detached and ruptured DM.
Additionally, cases of spontaneous corneal clearance have been described after Descemet’s stripping without endothelial keratoplasty (DSAEK) procedures, where corneal transparency improved despite the absence of donor endothelial replacement [6].
In those cases, migration and proliferation of peripheral healthy endothelial cells allowed functional recovery, resulting in corneal clarity and improved vision. Our case demonstrates a similar phenomenon, where conservative management led to an excellent outcome without surgical intervention.
This case emphasizes the importance of individualized management. While prompt surgical intervention remains the gold standard in large DMDs with progressive edema or vision-threatening involvement [7], a trial of medical therapy with corticosteroids, osmotic agents, and regular follow-up may be justified in select patients. The excellent visual recovery in our patient supports the hypothesis that, under certain conditions, Descemet’s membrane may regenerate and endothelial function may recover sufficiently to restore corneal transparency without keratoplasty.
Conclusion
This case highlights the rare occurrence of spontaneous corneal clearance after extensive Descemet’s membrane rupture and detachment during phacoemulsification. Similar to observations in Fuchs endothelial corneal dystrophy and after Descemet’s stripping without endothelial replacement, our findings suggest that surviving endothelial cells may retain the capacity to migrate, repopulate, and restore corneal clarity even after significant structural injury. Conservative medical therapy with close monitoring may therefore be a reasonable initial strategy in selected cases before proceeding to surgical intervention.
References
- Singhal D, Sahay P, Goel S, et al. Descemet membrane detachment. Surv Ophthalmol, 2020; 65: 279–293.
- Dua HS, Sinha R, D’Souza S, et al. “Descemet Membrane Detachment”: a novel concept in diagnosis and classification. Am J Ophthalmol, 2020; 218: 84–98.
- Jain R, Mohan N, Ghosh S. Descemet membrane detachment following phacoemulsification: risk factors and management. Eye (Lond), 2013; 27(5): 626–632.
- Price MO, Price FW Jr. Descemet’s stripping endothelial keratoplasty. Curr Opin Ophthalmol, 2007; 18(4): 290–294.
- Mehta JS, et al. Corneal endothelial cell biology in Fuchs dystrophy: insights into disease mechanisms and management. Prog Retin Eye Res, 2020; 74: 100777.
- Borkar DS, Veldman P, Colby KA. Treatment of Fuchs endothelial dystrophy by Descemet stripping without endothelial keratoplasty. Cornea, 2016; 35(10): 1267–1273.
- Sharma N, Agarwal T, Titiyal JS. Management of Descemet membrane detachment after intraocular surgery. Surv Ophthalmol, 2015; 60(4): 242–255.

