Case Report of Acquired Wandering Spleen Phenomenon with Splenic Torsion in the Context of Idiopathic Thrombocytopenic Purpura
Mike Akaraphanth1,3,, Chris Cribari1,5, Samantha McGrath3,6, Michael J Rogan4 and Travis Walker1,2,*
1University of Colorado School of Medicine, Aurora, Colorado, USA
2UC Health Surgical Clinic – Longs Peak Medical Center, Longmont, Colorado, USA
3Colorado State University, Fort Collins, Colorado, USA
4Regional West Medical Center, Scottsbluff, Nebraska, USA
5UC Health, Medical Center of the Rockies Trauma Center, Loveland, Colorado, USA
6Perspectus Technology, Inc., Fort Collins, Colorado, United States, USA
Received Date: 15/09/2025; Published Date: 02/10/2025
*Corresponding author: Travis Walker, MD, MS, University of Colorado School of Medicine, Aurora, Colorado, USA; UC Health Surgical Clinic – Longs Peak Medical Center, Longmont, Colorado, USA. 1760 E. Ken Pratt Boulevard, Suite 205, Longmont, CO 80504
Abstract
Wandering spleen is a rare condition characterized by the organ's displacement from its typical anatomical position due to increased mobility. This arises due to congenitally absent or weakened splenic suspensory ligaments that anchor the spleen. The wandering spleen is at risk of splenic torsion and can lead to mechanical occlusion of the vascular pedicle, splenic ischemia, and infarction. Patients often present with acute abdominal pain. Prompt diagnosis and intervention, typically via splenopexy or splenectomy, is paramount. A review of the literature reveals that these surgical cases are exceedingly rare, with few reported cases. This case report presents a novel instance of wandering spleen with splenic torsion in a 57-year-old multiparous female with a history of idiopathic thrombocytopenic purpura (ITP).
Keywords: Wandering Spleen; Splenic torsion; Hypermobile spleen; Idiopathic thrombocytopenic purpura; Virtual reality imaging; Hypermobile spleen
Introduction
The wandering spleen is a very rare clinical presentation of abnormal splenic positioning that was first described in 1667 [1,2]. Since its first observation, there have been sparse reports in recorded literature [1-4]. A potentially severe complication is splenic torsion, which occurs secondary to splenic hypermobility, leading to mechanical torsion of the vascular pedicle and subsequent splenic ischemia and infarction. Consequently, accurate and urgent recognition of the condition is critical. Theories for its etiology include congenitally absent or malformed splenic suspensory ligament or systemically weakened suspensory ligaments, precipitated by multiple cycles of relaxin, resulting in a bimodal distribution of pediatric and multiparous adult female patients [4,5]. In this paper, we present a rare and novel case of wandering spleen in a multiparous female patient with a history of ITP. The purpose of this surgical case is to review an atypical presentation of a rare but life-threatening medical emergency and to provide awareness of its presentation.
Case Report
A 57-year-old multiparous (gravida 4, para 4) female presented to the emergency department with a several-week history of vague, intermittent left upper quadrant abdominal pain and nausea that acutely intensified over the 48 hours prior to presentation. CT of the abdomen with contrast (Figure 1, with virtual reality reconstruction in Figure 2) revealed that the spleen was abnormally rotated on its axis, with the hilum facing the lateral position, engorged hilar vessels, and both standard and 360-degree rotation of the splenic artery and vein. There was also heterogeneous enhancement of the spleen, strongly suggestive of acute splenic torsion. Of note, a CT abdomen scan performed six weeks prior revealed a normal-appearing spleen in the correct anatomic position (Figure 3).
Prior surgical history consisted of left thoracotomy with diaphragm plication that resulted in a paralyzed left hemidiaphragm, laparoscopic cholecystectomy, and hysterectomy, but otherwise, no other disorder of the spleen. Past medical history is remarkable for a history of ITP. At time of presentation, the patient was notably thrombocytopenic, with a platelet count of 71×109/L. Otherwise, her preoperative blood count revealed a hemoglobin level of 13.4 g/dL and a white blood cell count of 5.1 ×109/L. Lactate was normal at 0.54 mmol/L.
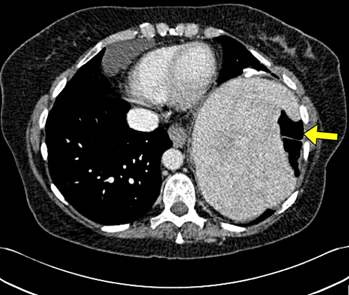
Figure 1: Coronal image of spleen during CT abdominal scan with contrast.
The CT scan demonstrated abnormal rotation of the spleen on its axis, with the hilum facing laterally (yellow arrow) and engorged splenic hilar vessels. There was a 360-degree rotation of the splenic artery and vein, accompanied by heterogeneous enhancement of the spleen. The overall splenic rotation towards the midline corroborated potential torsion.
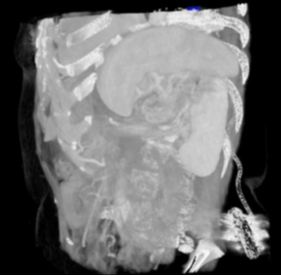
Figure 2: Three-dimensional image reconstruction of splenic torsion from CT data set.
Virtual Reality (VR) image depiction using Perspectus software, demonstrating the 360-degree rotation of the splenic artery and vein.
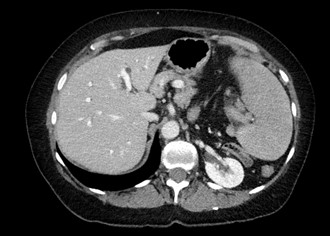
Figure 3: Coronal image of the spleen during CT with contrast of abdominal and pelvis.
A CT of the abdomen and pelvis performed 6 weeks prior to patient presentation revealed a normally positioned and sized spleen, establishing a baseline and supporting the diagnosis of acute splenic torsion.
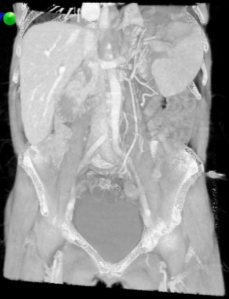
Figure 4: Three-dimensional image reconstruction revealing normal anatomic position of the spleen from CT data set 6 weeks before presentation.
VR image depiction using Perspectus software, demonstrating correct splenic positioning.
The patient underwent laparoscopic splenectomy with operative findings revealing that the splenic hilum was facing laterally, and the splenic vessels appeared engorged with significant edema within the hilum and vessels (Figure 5). The hilum was controlled using a stapler. Notably, the spleen was completely devoid of any suspensory ligaments or attachments. The pathology report revealed splenomegaly with a spleen measuring over 15 cm in length and a weight of 376 grams, and perivascular fibrosis with reactive changes, compatible with a history of ITP. Histologic features were consistent with splenic torsion without any discrete lesions.
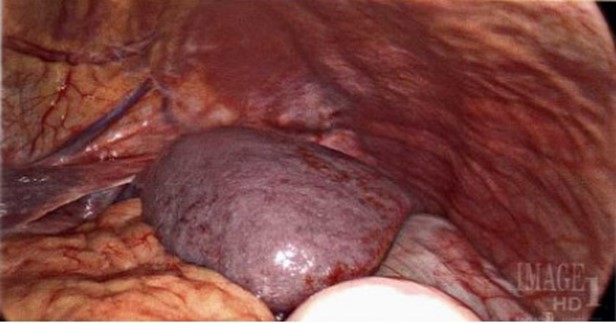
Figure 5: Intraoperative images of laparoscopic splenectomy for management of splenic torsion.
Upon creating a pneumoperitoneum and 12 mm umbilical optical port entry, an enlarged spleen was intraoperatively visualized to be enlarged, rotated with hilum facing laterally, and notably without supporting suspensory ligaments such as splenocolic, splenorenal, or gastrosplenic.
Postoperatively, the patient made an uneventful recovery and was discharged on postoperative day two. In follow-up at 3 weeks, the patient was pain-free, was administered post-splenectomy vaccinations, and the platelet count had risen to 411×109L.
Discussion
Wandering spleen was first reported in 1667, and since then to 2024, there have been less than 600 cases reported in PubMed’s database, with estimates of a 0.2% incidence rate in reported splenectomies [1,2]. The spleen is the largest reticuloendothelial organ in the human body, with essential roles in immunological defense and hematologic maintenance [6]. The average adult spleen measures longitudinally between 9 and 14 cm with an average weight of 135g [6,7]. Its anatomic position in the left upper quadrant is tethered in place by several suspensory ligaments, including the gastrosplenic ligament, splenorenal (also known as lienorenal) ligament, phrenicocolic ligament, and phrenicosplenic ligaments [7].
The encapsulated spleen is an intraperitoneal organ located at the left hypochondrium of the abdominal cavity. Any compromise to the structural integrity of these ligaments, or their congenital absence, can lead to splenic hypermobility, known as wandering spleen. This condition allows the spleen to migrate to various distant locations, including the pelvis [1]. As a result of this excessive mobility, the vascular pedicle may result in mechanical distortion or torsion.
The vascular pedicle of the spleen is comprised of the gastrosplenic and splenorenal ligaments, with the splenorenal ligament containing the distal splenic artery, vein, and inferior portion of the pancreatic tail [7]. With torsion, the venous return is compromised, leading to vascular congestion and splenomegaly. Arterial flow to the spleen may eventually be compromised, leading to ischemia and infarction, requiring emergent surgical intervention.
Because these cases are rare, determining the incidence is challenging. The incidence previously cited is 0.16% based on a review of thousands of splenectomies in studies conducted in 1981 and 1992 [3,8]. There is a demographic predisposition for the wandering spleen in pediatric cases, accounting for approximately one-third of cases, with presentations typically occurring below the age of 10 years, and a 1:1 male-to-female ratio [8]. This has been previously theorized to result from an abnormal embryologic development of the dorsal mesogastrium merging with the posterior abdominal wall [4], hence defects or congenitally absent gastrosplenic and phrenicosplenic ligaments [8], leading to an elongated splenic vascular pedicle susceptible to axial twisting. The majority of other cases have been historically reported to be in multiparous female populations between the ages of 20-40 years [5], with a recent theorized explanation that both estrogen and progesterone increased relaxin concentrations and its receptor expression on various supporting tissue, thus increasing ligamentous laxity and creating the predisposition of increased risk for the wandering spleen phenomenon [9,10].
The clinical presentation can be asymptomatic or may include nonspecific symptoms such as acute or chronic colicky abdominal pain, dysuria, splenomegaly, or a palpable abdominal/pelvic mass. Patients may also experience gastrointestinal symptoms such as constipation, bloating, nausea, and vomiting. In females, menstrual complications can also occur [11]. According to the National Organization of Rare Disorders, thrombocytopenia and anemia may develop secondary to an enlarged spleen with compromised blood flow, leading to symptoms such as fatigue, weakness, hematochezia, and hematemesis [11]. Although point-of-care ultrasound has been utilized to diagnose wandering spleen in the emergency department, cases are more accurately diagnosed using contrast-enhanced CT of the abdomen [12]. CT imaging findings include abnormal splenic orientation, change in anatomical location, splenic infarction, splenic vein thrombosis, swirling of the vascular pedicle, vascular engorgement, hyper enhancement of the spleen or its vessels, and perisplenic fat stranding [12]. In cases where splenic architecture is distorted or the vascular pedicle is poorly defined, a Technetium-99m sulfur colloid scan may be utilized for a more definitive diagnosis [12].
Definitive treatment is surgical management with splenectomy being recommended [12]; however, a 1989 report reviewed 35 cases of pediatric acute and chronic wandering spleens that additionally underwent splenoplexy using a Dexon mesh or conservative management without deaths reported as well [13]. Due to the elevated mortality rates associated with post-septectomy infections in adults (1.3%) and in children (1.7%), with notably higher rates in those with hematologic disorders such as sickle cell anemia (4.8%) and thalassemia major (5.1%), the importance of administering post-splenic vaccinations cannot be overstated [14].
Our patient presented as a multiparous female with a history of ITP. There have been reported cases of thrombocytopenia in the presentation of a wandering spleen in literature [15], as well as splenomegaly leading up to the cases of wandering spleen observed by Abell in his review [5], however, these findings have been thought to be attributed to the impaired splenic venous return from the rotated vascular pedicle. Chronic ITP was notably mentioned due to the known mechanism by which the majority of IgG autoantibodies bind to platelet glycoprotein surfaces, such as integrin αIIb-βIII complexes, leading to platelet destruction via splenic macrophages [6]. Although the spleen is not usually enlarged in cases of ITP, a palpable spleen may still be palpable in some patients [6].
It is difficult to conclusively report the exact cause of the patient's wandering spleen presentation, and it was speculated that her splenomegaly of 376g and corresponding perivascular fibrosis with reactive changes may have played a compounded role. With either systemically weakened or congenitally absent splenic suspensory ligaments (less likely given her acute presentation in adulthood and absent history regarding spleen disorders) and increased spleen mass from initial ITP, the spleen's increased momentum set the stage for splenic torsion.
The possibility of splenoplexy was a management option that was discussed with the patient; however, given the nature of the patient's acute presentation and history of ITP, laparoscopic detorsion would have been procedurally difficult with a high rate of recurrence, given the elongated splenic pedicle. Furthermore, her concurrent history of ITP would also have the highest long-term response rate with a splenectomy [6].
Conclusion
Wandering spleen with splenic torsion is a rare and potentially life-threatening condition that requires a high index of suspicion for timely diagnosis and intervention. This case highlights an unusual presentation of acquired wandering spleen in a multiparous adult female with a history of idiopathic thrombocytopenic purpura (ITP). The absence of splenic suspensory ligaments, combined with splenomegaly and possible perivascular fibrosis, may have contributed to the spleen’s hypermobility and eventual torsion. Contrast-enhanced CT imaging, along with virtual reality reconstruction, proved crucial in the preoperative diagnosis. Surgical management with laparoscopic splenectomy was both diagnostic and therapeutic, leading to a favorable outcome. Given the rarity of this condition, this case adds to the growing body of literature and underscores the importance of considering wandering spleen in patients presenting with acute or chronic abdominal pain and predisposing risk factors.
Ethical approval: Not applicable
Funding: Not applicable
Declaration of competing interest/Competing interests: The authors declare that there are no known conflicts of interest regarding the publication of this surgical case report.
Disclosures: Not applicable
Grant Information: Not applicable
Acknowledgements: Not applicable
References
- Shibiru Ya, Wondimu S, Almaw W. Wandering spleen presenting in the form of right sided pelvic mass and pain in a patient with AD-PCKD: a case report and review of the literature. Journal of Medical Case Reports, 2024; 18(1): p. 259.
- Magowska A. Wandering spleen: a medical enigma, its natural history and rationalization. World J Surg, 2013; 37(3): p. 545-550.
- Qazi SA, et al. Wandering spleen. Saudi Journal of Gastroenterology, 2004; 10(1): p. 1-7.
- Lane TM, South LM. Management of a wandering spleen. Journal of the Royal Society of Medicine, 1999; 92(2): p. 84-85.
- Abell I. Wandering spleen with torsion of the pedicle. Ann Surg, 1933; 98(4): p. 722-735.
- Kenneth Kaushansky MAL, Josef T Prchal, Marcel M Levi, Oliver W Press, Linda J Burns, Michael A Caligiuri. Williams Hematology. 10th Edition ed. 2021, New York: McGraw-Hill Education. 2528 pages.
- Standring S. Gray's Anatomy: The Anatomical Basis of Clinical Practice. 41st ed. 2016, Philadelphia, PA: Elsevier.
- Buehner M, Baker MS. The wandering spleen. Surg Gynecol Obstet, 1992; 175(4): p. 373-387.
- Jawad M, et al. Wandering Spleen: A Rare Case From the Emergency Department. Cureus, 2023; 15(1): p. e33246.
- Dehghan F, et al. The effect of relaxin on the musculoskeletal system. Scand J Med Sci Sports, 2014; 24(4): p. e220-e229.
- Disorders, N.O.f.R. Wandering spleen. 1994, 2003, 2008.
- Reisner DC, Burgan CM. Wandering Spleen: An Overview. Curr Probl Diagn Radiol, 2018; 47(1): p. 68-70.
- Allen KB, Andrews G. Pediatric wandering spleen--the case for splenopexy: review of 35 reported cases in the literature. J Pediatr Surg, 1989; 24(5): p. 432-435.
- Bisharat N, et al. Risk of infection and death among post-splenectomy patients. J Infect, 2001; 43(3): p. 182-186.
- Moll S, Igelhart JD, Ortel TL. Thrombocytopenia in association with a wandering spleen. Am J Hematol, 1996; 53(4): p. 259-263.

