Sirolimus Therapy in Unilateral Orbital Lymphangioma: A Case Report and Clinical Evolution
Harrar Youssef*, Ayoub Amara, Mabrouki Fatimazahra and Sekhsoukh Rachid
Faculty of Medicine and Pharmacy, Mohammed Ist University, Oujda, Morocco
Received Date: 31/08/2025; Published Date: 24/09/2025
*Corresponding author: Harrar Youssef, Faculty of Medicine and Pharmacy, Mohammed Ist University, Oujda, Morocco
Abstract
Orbital lymphangioma is a rare, unencapsulated vascular malformation of the lymphatic system, most often presenting during childhood, typically within the first decade of life.
The management of these lesions is challenging and requires both patience and a multidisciplinary approach.
We report the case of a 7-year-old girl with orbital lymphangioma successfully treated with medical therapy, achieving an excellent outcome.
Through this case and a review of the literature, we provide an updated overview of the condition and current management strategies.
Introduction
Orbital lymphangioma is an uncommon, benign, and unencapsulated vascular malformation of the lymphatic system that predominantly affects children, most frequently during the first decade of life [1,2].
Although benign, it can have serious functional and aesthetic consequences.
Its clinical course is often unpredictable, with recurrent hemorrhage, progressive enlargement, and exophthalmos posing significant therapeutic challenges.
Management is typically complex and requires a multidisciplinary approach, with options ranging from observation to medical or surgical interventions [2].
Case Report
We report the case of a 10-year-old girl with no relevant medical or surgical history and no history of orbital trauma, who presented to our Ophthalmology Emergency Department with rapidly progressive left-eye exophthalmos associated with active hemorrhage and left-sided facial deformation (Figure 1).
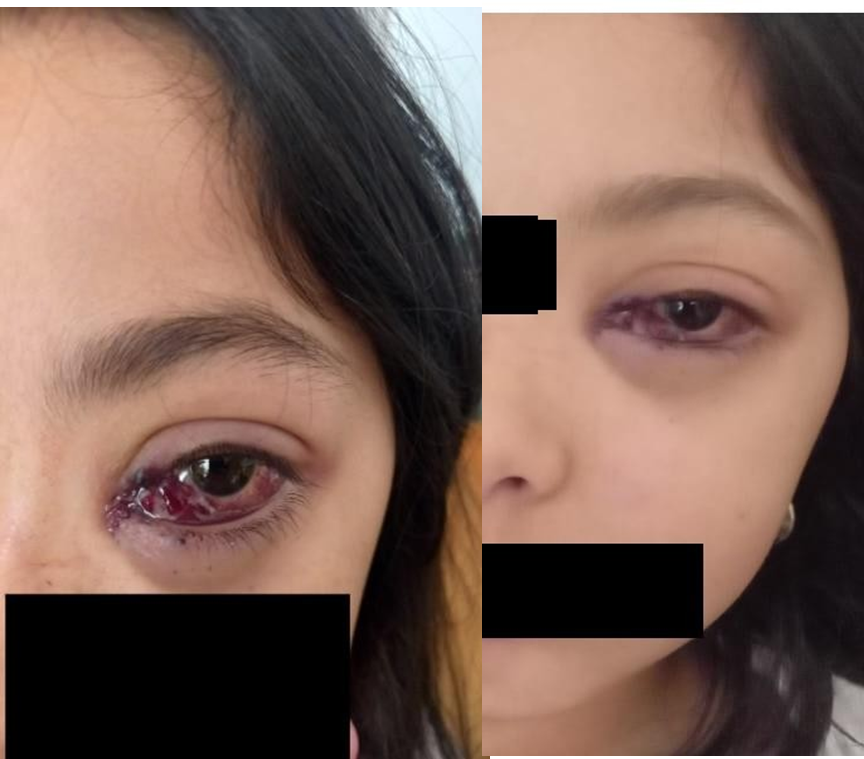
Figure 1: Inner punctate haemorrhaging in the left eye, accompanied by proptosis and subconjunctival haemorrhaging. Note the slight lateral eye dystopia and facial dysmorphia.
The history of the condition dates back 5 months, when her family noticed a small lesion at the inner corner of the left eye. The lesion progressively increased in size and was associated with episodes of diffuse subconjunctival hemorrhage without obvious cause, which spontaneously regressed after a few days of symptomatic treatment.
The family also reported occasional headaches. Ophthalmological examination revealed:
- Visual acuity of 10/10 in both eyes on the Snellen
- Left non-axial exophthalmos with minimal inferotemporal dystopia, without
- Hemorrhagic
- Normal anterior segment
- Normal fundus examination, with no optic disc
Oculomotor assessment showed a slightly limited elevation of the left eye, without diplopia.
A CT scan revealed a large, heterogeneous, polylobulated, isodense intra- and extraconal orbital lesion on the left side, measuring approximately 25 × 22 × 39 mm. This lesion caused significant proptosis of the left globe, extended into the masticatory space and the palpebral region, and was associated with secondary left hemimandibular dysmorphia (Figure 2).
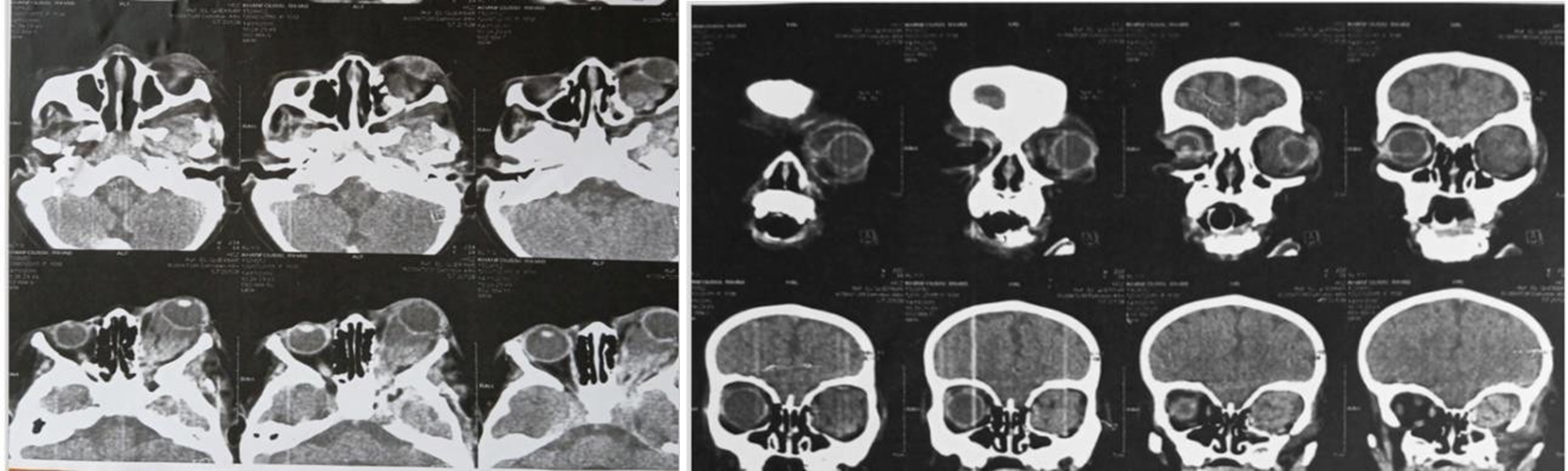
Figure 2: Large orbital heterogenous lesion in the intraconal space with proptosis of the left globe and hemimandibular dysmorphia.
MRI confirmed a large, fusiform, multilobulated lesion with hyperintensity on T2-weighted and FLAIR sequences, consistent with a low-flow venolymphatic orbital malformation. It caused ocular proptosis and extended parasellarly through the orbital apex, involving the eyelid and ipsilateral masticatory space.
A diagnosis of isolated orbital lymphangioma was made. After an interdisciplinary consultation, the decision was to initiate conservative medical therapy with sirolimus and regular follow-up.
Oral Sirolimus was administered at a dose of 0.8 mg/m² (0.05 mg/kg) twice daily for 6 months.
At the end of this first course, there was spectacular regression of the tumor, with marked reduction of dystopia and proptosis (Figure 3).
The decision was made to continue therapy for an additional 6 months, with further evaluation scheduled.
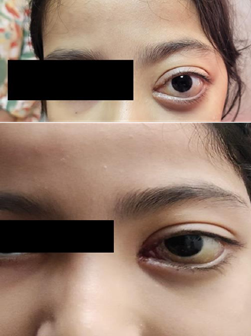
Figure 3: After six months of therapy using sirolimus, we note a good outcome with regression of the haemorrhagic protrusion.
Discussion
Lymphangiomas are vascular malformations with a fragile endothelial and lymphatic component, often presenting with cystic structures [5,7]. They can occur in various locations, but orbital involvement is rare, representing only about 2% of orbital tumors. These lesions are benign, but can have severe functional and aesthetic consequences.
According to the International Orbital Society [2], orbital lymphangiomas are classified as Type 1 (low-flow, with no connection to the vascular system) malformations. Lesions with vascular connections are classified as Type 2.
Clinically, orbital lymphangiomas usually present with progressive exophthalmos (axial or non-axial), often associated with dystopia, limited ocular motility, and tissue infiltration, depending on tumor location.
In some cases, onset is acute, with sudden exophthalmos and decreased visual acuity caused by compressive intra-cystic hemorrhage [3,4].
In our case, the evolution was insidious, later complicated by acute hemorrhage and exophthalmos. Imaging plays a crucial role in diagnosis, assessment of severity, and treatment planning [2,6]:
- Doppler ultrasound: first-line, detects slow-flow cystic
- CT scan: widely available, useful for evaluating tumor extent and its relationship with orbital and facial bones—especially relevant for surgical planning.
- MRI (T1, T2, FLAIR sequences): gold standard, typically shows a heterogeneous, multilobulated lesion with cystic and hemorrhagic MRI also allows precise evaluation of orbital and periorbital extension, involvement of adjacent structures, and detection of other lesions in the face and neck.
In our case, the lesion was purely orbital with slight infiltration of the left upper eyelid.
Management of orbital lymphangioma is difficult, influenced by:
- the young age of most patients,
- the need to preserve visual acuity and prevent
Treatment strategies include:
1. Conservative (medical) therapy:
Sirolimus is currently the most effective systemic treatment. It inhibits the mTOR pathway, exerting anti-lymphangiogenic activity. Wiegand et al. analyzed 28 studies including 105 children (newborn to 17 years) treated with sirolimus for head and neck lymphatic malformations: 91% responded, with treatment durations ranging from 6 months to 4 years. Reported side effects include neutropenia, infections, and hyperlipidemia [1,3].
2. Surgical management:
Challenging because lesions are unencapsulated. Often limited to partial excision or debulking to reduce mass effect, particularly when optic neuropathy is suspected. Intraoperative bleeding is a major risk, but may be minimized using diathermy, CO₂ laser, or fibrin glue injection into cystic components (Boulos et al.) [2].
3. Non-surgical interventional therapy (sclerotherapy)
Agents used include:
- OK-432 (Picibanil)
- Sodium tetradecyl sulfate (5%)
- Sodium morrhuate, Bleomycin A5
These are injected perilesionally to reduce tumor volume, either as definitive treatment or to facilitate subsequent surgery; Patel et al. reported a series of three cases of facial and orbital lymphangiomas successfully treated with sclerotherapy [2].
In our case, the patient was treated conservatively with sirolimus (0.05 mg/kg twice daily) for one year, with no adverse effects reported so far. The decision for medical therapy was taken after a multidisciplinary consultation involving pediatric surgery, neurosurgery, and pediatric oncology. Given the relatively small tumor size, absence of additional lesions, and delicate intra-conal location, surgery or sclerotherapy carried significant risks of ocular or facial ischemia and were therefore avoided.
Conclusion
Orbital lymphangioma is a rare but potentially vision-threatening condition that requires careful evaluation and individualized management. Imaging plays a critical role in diagnosis and assessment of tumor extent, guiding therapeutic decision-making. While surgical and interventional options remain valid in selected cases, they are often limited by anatomical complexity and risk of complications.
Our case illustrates the effectiveness of sirolimus as a safe and well-tolerated medical therapy, leading to significant regression of the lesion and functional improvement.
Conservative management with sirolimus, supported by multidisciplinary discussion, represents a promising therapeutic option for orbital lymphangiomas, particularly in cases where surgical or sclerotherapeutic approaches carry significant risks.
Long-term follow-up remains essential to monitor tumor behavior, treatment response, and potential side effects.
References
- Wiegand S, Dietz A, Wichmann G. Efficacy of sirolimus in children with lymphatic malformations of the head and neck. Eur Arch Otorhinolaryngol, 2022; 279(8): 3801–3810. Sirolimus showed a high response rate among children treated for lymphatic malformations of head and neck regions.
- Karnesh Chandrakant Patel, George Kalantzis, Nabil El-Hindi, Bernard Y. Sclerotherapy for Orbital Lymphangioma – Case Series and Literature Chang/doi:10.21873/invivo.11055
- Sirolimus for pediatric cervicofacial lymphatic malformation: a systematic review and meta-analysis.
- Shoji MK, Shishido S, Freitag SK. The use of sirolimus for treatment of orbital lymphatic malformations: a systematic Ophthalmic Plast Reconstr Surg. Out of 10 patients treated, 3 had complete responses and 7 had partial responses, with manageable side effects, 2020; 36(3): 215–221.
- Treatment of orbital lymphatic malformation with oral sirolimus: a case Arquivos Brasileiros de Oftalmologia.
- Sirolimus-induced regression of a large orbital Case Reports.
- Intraorbital lymphatic-venous malformation in an adult patient: is sirolimus the key?

