Cystoperitoneal Shunt Complication in Pediatrics: Sigmoid Colon Perforation with Anal Extrusion
Stitou Kaoutar*, Zahir Ilias**, Hmamouch Mohamed Oualid, Hammoud Marouane, Fayçal Lakhdar, Mohammed Benzagmout, Khalid Chakour, Chaoui El faiz Mohammed
Department of Neurosurgery, University Hospital Hassan II, Fez, Morocco
These authors contributed equally to this work and share first authorship.
Received Date: 30/08/2025; Published Date: 19/09/2025
*Corresponding author: Stitou Kaoutar*, Neurosurgeon, Department of Neurosurgery, University Hospital Hassan II, Fez – Morocco; Zahir Ilias**, Neurosurgeon, Department of Neurosurgery, University Hospital Hassan II, Fez, Morocco
Abstract
Background: Cystoperitoneal shunts (CPS) are an effective treatment for symptomatic arachnoid cysts in infants, particularly in cases of raised intracranial pressure (ICP). Although shunt procedures are generally safe, rare but serious abdominal complications may occur. We report a unique case of sigmoid perforation with anal extrusion of a CPS catheter in a neonate.
Case Description: A previously healthy one-month-old infant presented with signs of increased ICP, including vomiting, tense anterior fontanelle, and rapid head circumference enlargement. Imaging revealed a large right fronto-temporo-parietal arachnoid cyst. A Cystoperitoneal shunts was placed, leading to resolution of symptoms. Four months later, the distal catheter extruded through the anus. CT confirmed sigmoid colon perforation with intraluminal migration of the catheter, but no peritonitis. The shunt was completely removed, antibiotics were administered, and the colonic defect closed spontaneously. At six months follow-up, the child remained neurologically intact, with no recurrence of the cyst.
Conclusion: Sigmoid perforation with anal extrusion is an exceptionally rare complication of CPS. This case highlights the importance of recognizing silent gastrointestinal events, emphasizes the need for prompt intervention to avoid infection, and suggests that some arachnoid cysts may remain stable after initial decompression.
Keywords: Cystoperitoneal shunt; Arachnoid cyst; Sigmoid perforation; Pediatric neurosurgery; Anal extrusion
Introduction
Intracranial arachnoid cysts are benign, CSF-filled lesions, representing approximately 1% of pediatric intracranial masses [1]. When symptomatic—particularly due to raised Intracranial Pressure (ICP)—surgical intervention is warranted. Cystoperitoneal Shunting (CPS) is a widely accepted and effective treatment for large or symptomatic arachnoid cysts.
Although CPS is generally safe, complications related to the distal catheter may arise. Bowel perforation, though rare, is among the most serious, with a reported incidence between 0.1% and 0.7% in shunt-dependent patients [2]. Sigmoid perforations are particularly uncommon and even more rarely associated with cystoperitoneal shunts, as most reports involve ventriculoperitoneal shunts.
We present a rare case of sigmoid perforation with anal extrusion of a CPS catheter in a neonate, successfully managed with shunt removal and conservative bowel management.
Case Report
A one-month-old female infant presented with repeated vomiting, poor feeding, bulging anterior fontanelle, and accelerated head growth. Neurological examination was otherwise normal.
Cranial ultrasound, CT (Figure 1), and MRI (Figure 2) demonstrated a large right fronto-temporo-parietal extra-axial cystic lesion with significant mass effect and midline shift. Laboratory results were normal.
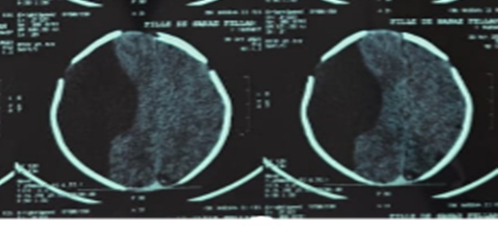
Figure 1: Non-contrast axial CT scan demonstrating a large right fronto -temporo-parietal extra-axial hypodense collection, exerting significant mass effect on the midline structures.
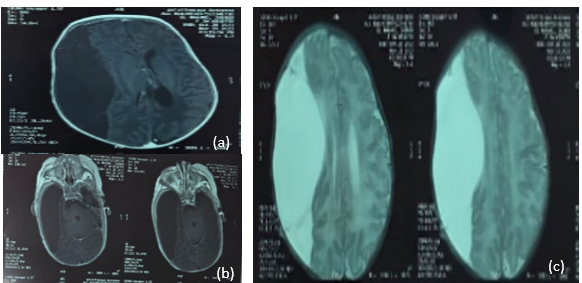
Figure 2: Axial MRI demonstrating a right fronto-temporo-parietal extra-axial lesion. The lesion appears hypointense on non-contrast T1-weighted images (A), does not enhance after contrast administration on T1-weighted images, and is hyperintense on T2-weighted images, with no evidence of hemorrhage.
A CPS was inserted via a right parietal burr hole. The cyst fluid was clear and under pressure. The distal catheter was tunneled into the peritoneal cavity. Postoperative CT and radiographs (Figure 3) confirmed proper positioning. The infant’s symptoms resolved, feeding normalized, and developmental milestones were appropriate.
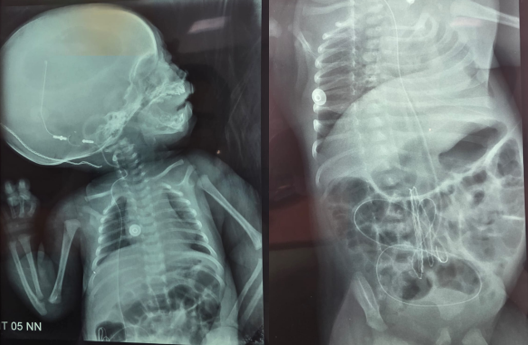
Figure 3: Standard radiographs, including frontal skull, chest, and abdominal views, confirming correct placement of the catheter.
At four months post-surgery, the parents noted extrusion of the catheter tip through the anus (Figure 4). The child was afebrile, alert, and had no abdominal tenderness. CT and radiographs (Figures 5 and 6) revealed sigmoid perforation with intraluminal catheter migration into the rectum. Importantly, no pneumoperitoneum, abscess, or signs of peritonitis were present.
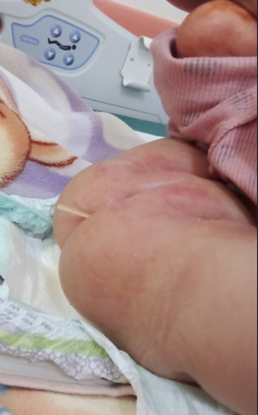
Figure 4: Clinical photograph showing distal migration of the Cystoperitoneal shunt catheter, exteriorized through the anal orifice in a pediatric patient.
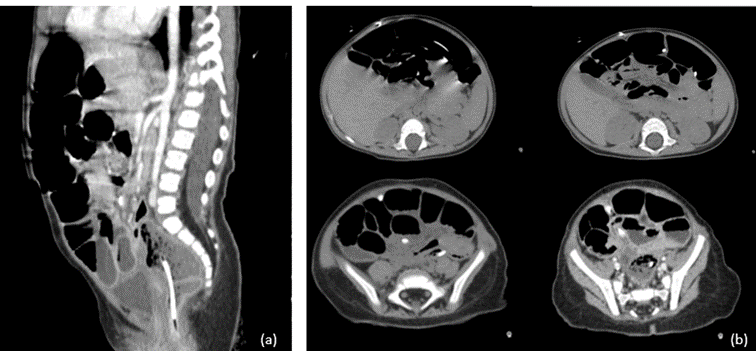
Figure 5: Abdominal CT scans demonstrating the distal cystoperitoneal catheter. (a) Sagittal view showing the catheter within the sigmoid colon. (b) Axial view confirming intraluminal migration of the catheter into the rectum.
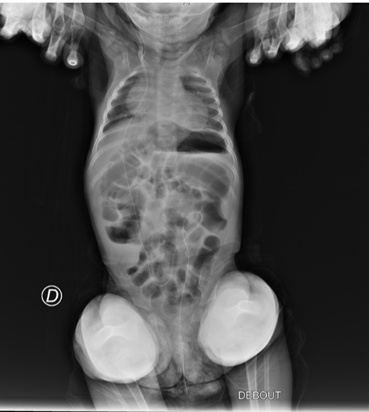
Figure 6: AP radiographs of the thorax and abdomen showing anal extrusion of the distal cystoperitoneal catheter.
The entire shunt system was surgically removed, and broad-spectrum antibiotics were administered. The colonic defect healed spontaneously without resection. At six months follow-up, the patient remained neurologically intact, and imaging showed no recurrence of the arachnoid cyst.
Discussion
CPS remains a safe and effective treatment for symptomatic arachnoid cysts. However, distal catheter complications—particularly bowel perforation—are extremely rare in infants. The mechanisms proposed include chronic catheter irritation, ischemia, and pressure necrosis of thin-walled colonic segments [3,4].
Unlike other abdominal complications (ascites, pseudocysts), bowel perforation may remain clinically silent until catheter extrusion occurs [5,6]. The absence of systemic signs allows conservative management in select cases, provided that prompt shunt removal is performed to prevent central nervous system infections such as meningitis or ventriculitis [2].
In most cases, small colonic perforations close spontaneously after catheter removal if no infection is present [7]. This outcome was observed in our patient, who recovered uneventfully without colonic resection.
Another noteworthy aspect of this case is the absence of cyst recurrence despite shunt removal. Previous pediatric series have reported that a single decompression event may be sufficient for some arachnoid cysts [1]. Nevertheless, close radiological and clinical follow-up is mandatory. In cases requiring re-shunting, alternative diversion routes—such as atrial or pleural shunts—should be considered [8].
Conclusion
Sigmoid perforation with anal extrusion of a CPS catheter is an exceedingly rare but potentially serious complication. Vigilant clinical follow-up is crucial, as symptoms may be subtle or absent. Early recognition and prompt removal of the shunt system are essential to prevent morbidity. Furthermore, this case illustrates that some arachnoid cysts may remain stable after initial decompression, underlining the need for individualized follow-up strategies in pediatric neurosurgery.
References
- Al-Holou WN, Terman S, Kilburg C, Garton HJ, Muraszko KM, Maher CO. Prevalence and natural history of arachnoid cysts in children. J Neurosurg Pediatr, 2010; 5(6): 578–585.
- Sathyanarayana S, Wylen EL, Baskaya MK, Nanda A. Spontaneous bowel perforation due to ventriculoperitoneal shunt: case report and literature review. Surg Neurol, 2000; 54(5): 388–396.
- Harischandra LS, Sharma A, Chatterjee S. Ventriculoperitoneal shunt complications: A review. Surg Neurol Int, 2020; 11: 101.
- Yilmazlar S, Kocaeli H, Dogan S. Bowel perforation complicating ventriculoperitoneal shunt surgery: a review. Turk Neurosurg, 2006; 16(1): 33–36.
- Rainov NG, Schobess A, Heidecke V, Burkert W. Anal extrusion of a ventriculoperitoneal shunt catheter due to rectal perforation. Br J Neurosurg, 1994; 8(6): 723–725.
- Ghritlaharey RK. Trans-anal extrusion of ventriculoperitoneal shunt catheter: review and management strategies. Pediatr Surg Int, 2011; 27(10): 1085–1090.
- Yılmaz N, Kocaogullar Y, Sener U, Erdoğan E. Anal protrusion of a ventriculoperitoneal shunt catheter without peritonitis. Turk Neurosurg, 2013; 23(5): 696–699.
- Browd SR, Ragel BT, Gottfried ON, Kestle JR. Failure of cerebrospinal fluid shunts: part I. Obstruction and mechanical failure. Pediatr Neurol, 2006; 34(2): 83–92.

