Lumbar Spinal Schwanoma
Dehayni Fariss*, Neftah Ismail, Nassar Itimad and Imrani Kaoutar
Department of Central Radiology, Ibn Sina Hospital, Faculty of Medicine and Pharmacy of Rabat, Morocco
Received Date: 13/08/2025; Published Date: 11/09/2025
*Corresponding author: Dehayni Fariss, Department of Central Radiology, University Mohammed V, Morocco
Abstract
Background: Spinal schwannomas are the most common intradural extramedullary tumors, arising from the nerve root sheaths, with a slow-growing course and an annual incidence of 0.3–0.5 per 100,000 individuals. They are predominantly found in the thoracic and cervical spine.
Case Presentation: We report the case of a 56-year-old man with a history of renal colic, presenting with right lower back pain and lumbar spinal syndrome. Magnetic Resonance Imaging (MRI) revealed features consistent with a spinal schwannoma.
Discussion: Spinal schwannomas typically present with radicular pain, paraesthesia, and paraparesis. MRI is the modality of choice, demonstrating characteristic signal intensities on T1 and T2-weighted images, often with contrast enhancement. Surgical resection remains the treatment of choice for symptomatic tumors, with gross total resection aimed at preserving neurological function. Large tumors with extraforaminal extension may pose higher surgical risks.
Conclusion: Early recognition and MRI evaluation of spinal schwannomas are critical for planning surgical management and optimizing neurological outcomes.
Introduction
Spinal schwannomas are benign, slow-growing tumors arising from the Schwann cells of spinal nerve roots and represent the most common intradural extramedullary spinal tumors. Although they can occur along any segment of the spine, they are most frequently found in the thoracic and cervical regions. The annual incidence is estimated at 0.3–0.5 per 100,000 individuals.
Clinically, spinal schwannomas may present with a spectrum of symptoms, including radicular pain, sensory disturbances, and motor deficits such as paraparesis, often progressing gradually due to the tumor’s slow growth. Magnetic resonance imaging (MRI) is the diagnostic modality of choice, providing high-resolution visualization of tumor location, extent, and characteristic signal patterns on T1- and T2-weighted images. Contrast enhancement further aids in delineating tumor margins.
Surgical intervention, typically aiming for gross total resection, is indicated for symptomatic cases to relieve pain, preserve nerve function, and prevent neurological deterioration. However, tumors with extensive extraforaminal extension may pose additional surgical challenges. This article presents the case of a 56-year-old man with a lumbar spinal schwannoma, highlighting diagnostic imaging findings and considerations for surgical management.
Case Description
56 years old man, with antecedent of renal colic, presenting with right lower back pain becoming inflammatory with lumbar spinal syndrome.
Discussion
Spinal schwannomas, which arise from spinal nerve root sheaths, are the most common intradural extramedullary spinal tumours, with an incidence of 0.3–0.5/100,000 individuals annually [1] and are commonly found in the thoracic and cervical spine. They are slowly growing tumours.
The classic presentation of spinal schwannomas includes radicular pain, paraesthesia and/or paraparesis.
MRI is the diagnostic modality of choice due to its noninvasive nature and high accuracy on spinal tumours. The critical MRI indicators for spinal schwannomas include:
Signal intensity that is equal or less than that of spinal cord on T1 weighted images and a mild to marked hyperintensity on T2-weighted images. Focal areas of even greater hyperintensity on T2-weighted images often correspond to cystic regions, whereas hypointensity may represent hemorrhage, dense cellularity, or collagen deposition [2.3]. Virtually, 100% enhance on T1 C+.
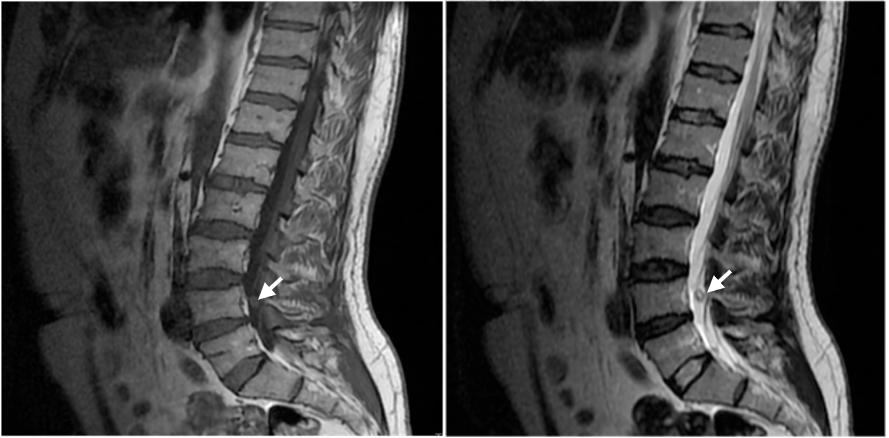
Figure 1: Sagittal T1 weighted image.
Figure 2: Sagittal T2 weighted image.
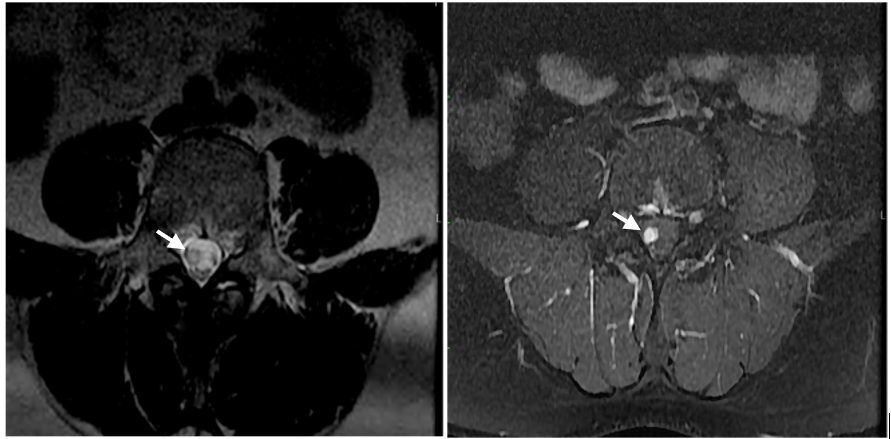
Figure 3: Axial T2 weighted image.
Figure 4: Axial Contrast+ image.
The treatment of choice for symptomatic spinal schwannomas is surgery, aiming for gross total resection (GTR) with preservation of the nerve and sustained or improved neurological function [4-6]. Surgical complications often occur in large tumors with extraforaminal extension since they require more extensive approaches [7].
References
- Sun I, Pamir MN. Non-syndromic spinal schwannomas: a novel classification. Front Neurol, 2017; 8: 318.
- Liu WC, Choi G, Lee SH, Han H, Lee JY, Jeon YH, et al. Radiological findings of spinal schwannomas and meningiomas: focus on discrimination of two disease entities. Eur Radiol, 2009; 19(11): 2707-2715.
- Raper D, Yen CP, Mukherjee S, Sheehan J. Decreased calcification of a petroclival meningioma after gamma knife radiosurgery. BMJ case reports, 2014; 2014.
- Emel E, Abdallah A, Sofuoglu OE, Ofluoglu AE, Gunes M, Guler B, et al. Long-term Surgical Outcomes of Spinal Schwannomas: Retrospective Analysis of 49 Consecutive Cases. Neurosurg, 2017; 27: 217–225.
- Ottenhausen M, Ntoulias G, Bodhinayake I, Ruppert F-H, Schreiber S, Förschler A, et al. Intradural spinal tumors in adults-update on management and outcome. Rev, 2019; 42: 371–388.
- Apostolov G, Kitov B, Poryazova E, Kehayov I. Sporadic spinal schwannomas and neurofibromas—A review. Folia Med, 2021; 63: 309–314.
- Nanda A, Kukreja S, Ambekar S, Bollam P, Sin AH. Surgical Strategies in the Management of Spinal Nerve Sheath Tumors. World Neurosurg, 2015; 83: 886–899.

