The Utility of Magnetic Resonance Imaging to Diagnose Asymptomatic Radiograph-Negative Hip Fractures in Patients on Chronic Steroids: A Case Report of Simultaneous Bilateral Non-Traumatic Femoral Neck Fractures
Sean Kean Ann Phua* and Jegathesan T
Department of Orthopaedic Surgery, Tan Tock Seng Hospital, Singapore
Received Date: 18/07/2025; Published Date: 26/08/2025
*Corresponding author: Sean Kean Ann Phua, Medical Officer, Department of Orthopedic Surgery, Tan Tock Seng Hospital, 11 Jln Tan Tock Seng, Singapore
ORCID ID: https://orcid.org/0000-0002-7750-4456
Abstract
The incidence of atraumatic simultaneous bilateral neck of femur fractures is rare, but may be predisposed by metabolic bone disorders. While magnetic resonance imaging is recommended to rule out occult hip fractures in symptomatic patients with predisposing factors, the approach to asymptomatic patients is unclear. The authors report herein a rare case of a patient with significant history of long-term, high-dose glucocorticoid usage who presented with a displaced right neck of femur fracture without antecedent trauma, who was subsequently diagnosed with contralateral undisplaced neck of femur fracture following magnetic resonance imaging scan. The importance of having an index of suspicion for bilateral fracture incidence in patients on chronic steroids, as well as the utility of magnetic resonance imaging to rule out undisplaced contralateral hip fracture even in the absence of symptoms or suspicious radiographic features, are discussed.
Keywords: Neck of femur fracture; Magnetic resonance imaging; Steroid; Asymptomatic; Bilateral
Introduction
Though there is rising prevalence of unilateral hip fractures following low-velocity trauma globally, atraumatic simultaneous bilateral neck of femur fractures remain rare. Possible contributing factors within existing literature include severe osteoporosis, hypophosphatemic rickets disease [1], renal osteodystrophy [2] and anti-epileptic usage [3]. While magnetic resonance imaging is recommended to rule out occult hip fractures in patients with hip pain and underlying predisposing factors, the approach to asymptomatic patients is unclear.
We report a rare case of a patient with significant history of long-term, high-dose glucocorticoid usage who presented with a displaced right neck of femur fracture without antecedent trauma, who was subsequently diagnosed with an asymptomatic left undisplaced neck of femur fracture that was undetected on radiographs, after undergoing magnetic resonance imaging scan. To the authors' knowledge, this has not been reported in literature and highlights the importance of having an index of suspicion for bilateral fracture incidence in patients on chronic steroids, and the need to consider magnetic resonance imaging to rule out undisplaced contralateral hip fracture even in the absence of symptoms.
Case Report
This case report describes a 74-year-old Chinese lady with simultaneous bilateral atraumatic neck of femur fractures. She first presented to the emergency department of a tertiary hospital in April 2025 for one month history of worsening right hip. It was described as a sharp pain over her right groin, radiating towards the lateral and distal aspect of her right thigh. Her pain was worse with weightbearing and mobilization, and was refractory to oral analgesia. She denied prior trauma to her hip throughout her life.
Of significance, she received long-term, high-dose glucocorticoid usage for left necrotizing sclerouveitis. She initially received a short course of intravenous methylprednisolone 1g which was oralized to once-daily prednisolone 60mg in end March 2024. Prednisolone dosage was gradually tapered each week to once-daily 20mg regime by end April 2024. Due to disease recurrence in end April 2024, she was re-admitted for another short-course of IV methylprednisolone 1g. Prednisolone dosage was gradually tapered according to disease control: from 30mg daily in April 2024, to 10mg daily in July 2024, and finally to 2.5mg daily from Jan 2025 until the date of presentation. This was additionally complicated by steroid-induced hyperglycemia and multi-level lumbar spine compression fractures. Her other past medical history included hypertension, hyperlipidemia and anemia of chronic disease. Prior to onset of symptoms, she required assistance for her activities of daily living, and was home ambulant with a walking frame.
On examination, the patient had a cushingoid appearance. Her right lower limb was shortened and externally rotated. There was significant pain on flexion, internal rotation and axial loading of her right hip. There was no left lower limb shortening or pain on left hip mobilization.
Initial radiographs demonstrated a displaced right neck of femur fracture (Figure 1), with no grossly significant femoral neck fracture noted on the left hip. Considering her atraumatic presentation, further imaging was planned to rule out a pathological cause. Subsequent magnetic resonance imaging of her pelvis demonstrated a subacute, displaced right neck of femur fracture. Additionally, an undisplaced left neck of femur fracture was incidentally noted (Figure 2). There was no radiological evidence of a pathological cause.
Biochemical markers (erythrocyte sedimentation rate, adjusted calcium, phosphate, alkaline phosphatase, 25-hydroxy Vitamin D and parathyroid hormone) did not suggest any underlying metabolic bone disease to account for the bilateral and atraumatic presentation. Her bone mineral density was in the osteopenic range with reported T-score of -2.3.
The patent underwent cemented right hip bipolar hemiarthroplasty and surgical fixation of her undisplaced left hip fracture using the femoral neck system. Post-operatively, she underwent rehabilitation by the therapist and ambulated with a rollator walking aid. She was concurrently managed for her other medical issues including cholestatic transaminitis, acute kidney injury, delirium and urinary tract infection. Approximately two weeks following surgery, she was transferred to the community hospital for further rehabilitation.
The patient was reviewed at the outpatient clinic at six weeks following surgery, and was assessed to have mild right lateral hip pain. On examination, her surgical wounds were well-healed and there was minimal tenderness over the right lateral hip. Her hip flexion was 5 degrees, internal rotation was 10 degrees and external rotation was 20 degrees bilaterally. Radiographs showed healing left proximal femur fracture without any signs of peri-implant loosening or mal-alignment, as well as a stable right hip bipolar hemiarthroplasty prosthesis (Figure 3).
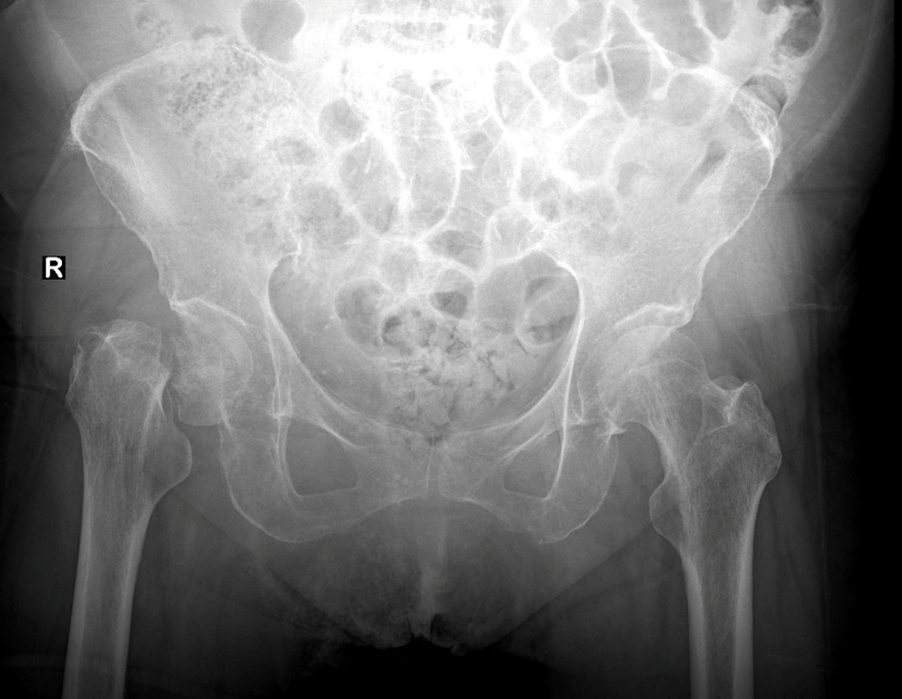
Figure 1: Initial anteroposterior pelvis radiograph demonstrating displaced right neck of femur fracture with no obvious fracture over the left proximal femur.
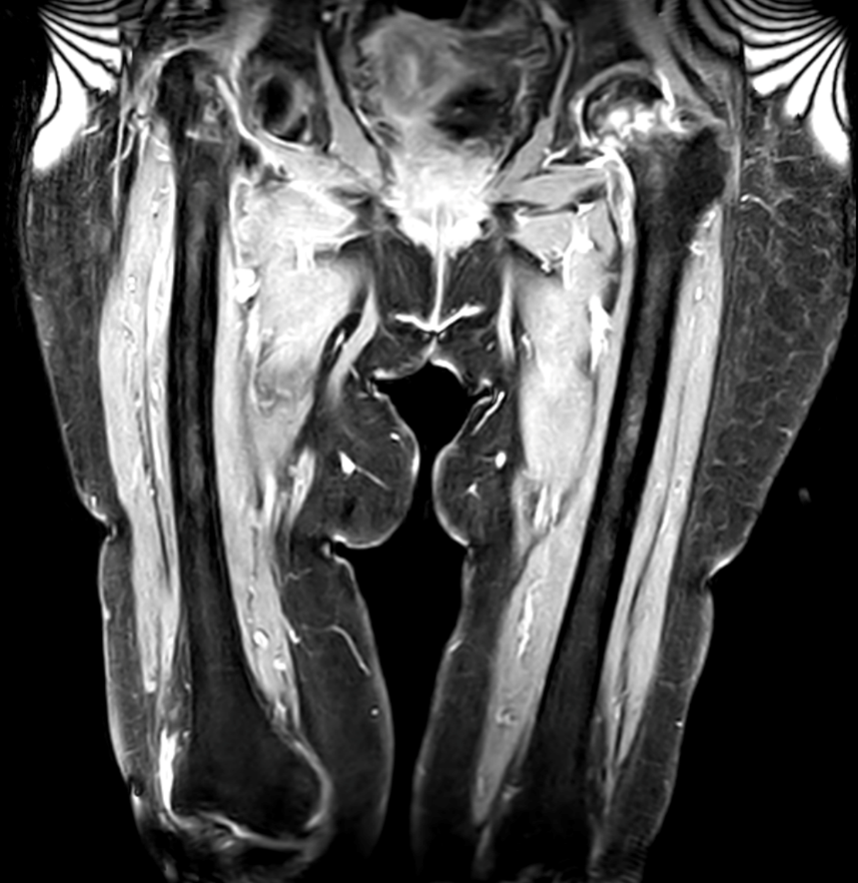
Figure 2: Pre-operative T1-weighted, gadolinium-enhanced magnetic resonance image demonstrated simultaneously-occurring undisplaced left neck of femur fracture.
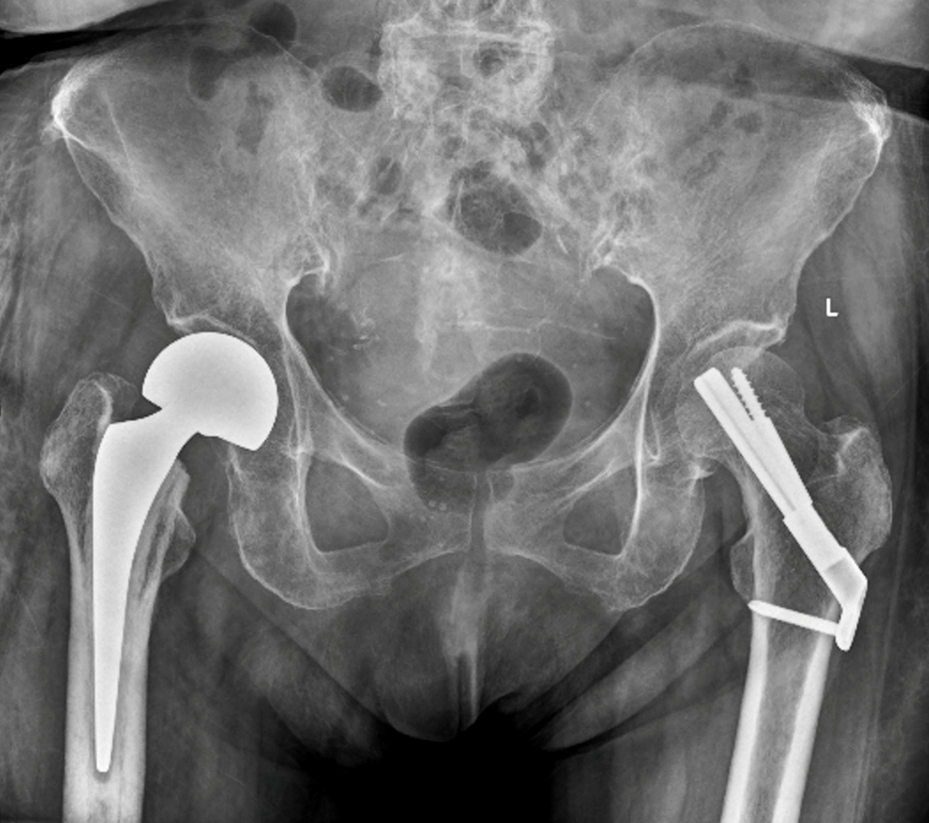
Figure 3: Anteroposterior pelvis radiograph at six weeks after surgery demonstrating right hip bipolar hemiarthroplasty and surgical fixation of the left proximal femur with the femoral neck system.
Discussion
To the authors' knowledge, this is the first report of simultaneous atraumatic bilateral neck of femur fracture occurring in a patient with significant background of chronic glucocorticoid usage. In particular, undisplaced neck of femur fracture in the contralateral hip was incidentally detected on magnetic resonance imaging – despite the absence of pain, trauma or concerning radiographic features. This case highlights two important points: first, clinicians should have an index of suspicion for bilateral fracture incidence in patients with long-term glucocorticoid usage; second, in cases of chronic glucocorticoid usage with known unilateral fragility hip fracture, magnetic resonance imaging should be considered to rule out contralateral radiograph-negative hip fracture even in the absence of symptoms.
Presence of simultaneous bilateral neck of femur fractures following low-velocity injury or without antecedent trauma should raise suspicion of an underlying systemic etiology. Amongst the limited reports of such cases in existing literature, possible contributing factors include severe osteoporosis, hypophosphatemic rickets disease, renal osteodystrophy and anti-epileptic usage. Arisumi et al. reported a case of a 33-year-old gentleman with severe osteoporosis and vitamin-D deficiency who developed simultaneous bilateral neck of femur fractures without antecedent trauma [4], while Uzun et al. reported a case of a 26-year-old lady with significant history of autosomal recessive hypophosphatemic rickets disease with similar atraumatic presentation during the postpartum period [1]. John et al. reported three cases of end-stage renal disease with renal osteodystrophy with simultaneous bilateral neck of femur fractures after episodes of grand mal convulsions [2]. Sadiq et al. reported a case of low-energy simultaneous bilateral neck of femur fractures in a 50-year-old epileptic patient on long-term phenytoin who fell from bed [3].
Considering that our patient's bone mineral density was in the osteopenic range, our case demonstrates that chronic glucocorticoid usage may be an independent risk factor for simultaneous bilateral neck of femur fractures even without severe osteoporosis. The incidence of fragility fractures may be predisposed by glucocorticoid usage through several mechanisms: suppressed osteoblastic activity, reduced intestinal and renal calcium absorption and/or increased calcium excretion [5]. The net effect is inhibition of bone formation, as well as increased bone resorption (resulting from secondary hyperparathyroidism) [5]. These alterations in bone physiology may similarly explain the incidence of delayed union or non-union of surgically-treated hip fractures in patients with chronic glucocorticoid usage, and the proposed use of anabolic drugs such as teriparatide in such patients to facilitate osteoblastic activation [6].
Importantly, clinicians should be aware that both short-term high glucocorticoid exposure, as well as high cumulative glucocorticoid exposure over time, predispose incidence of hip fracture. In a population-based study using the Danish National Health Service data, consisting of 81,342 patients, Amiche et al. demonstrated that the risk of hip fractures was independently increased by both high daily prednisolone dose (i.e., exceeding 15mg per day) (adjusted odds ratio (OR) 2.50 (2.19-2.85)) and high cumulative prednisolone dose (i.e., exceeding 1g) (adjusted OR 1.64 (1.54-1.74)) [7]. This risk was further compounded when the prednisolone regime consisted of both a high daily and cumulative dose (adjusted OR 2.94 (2.52-3.42)).
While current clinical practice recommends the use of magnetic resonance imaging to rule out occult fractures in symptomatic patients with predisposing comorbidities, the diagnostic approach to asymptomatic patients – with or without known unilateral fragility fracture – is unclear. This in turn highlights a gap in current literature on the prevalence of asymptomatic, radiograph-negative hip fractures in patients with predisposing factors: while studies examining the magnetic resonance imaging results of asymptomatic hips exist, the majority of such research focuses on the prevalence of acetabular cartilage loss and labral tears in athletes [8] or avascular necrosis in patients with risk factors such as systemic lupus erythematosus [9]. Future research addressing this specific gap in knowledge will be necessary in determining whether there is utility in routine magnetic resonance imaging to rule out asymptomatic, radiograph-negative hip fractures in patients with risk factors, when balanced against the cost and availability of magnetic resonance imaging capabilities. Our case provides an example where the aforementioned change in clinical approach would have significant clinical utility. Importantly, failure to pick up these occult fractures will lead to debilitating consequences downstream, including fracture displacement with or without trauma, readmission for further treatment, subsequent secondary surgical-related risks and resetting a patient’s rehabilitation post-surgery.
Conclusion
In cases of chronic glucocorticoid usage, clinicians should have an index of suspicion for bilateral fracture incidence. When unilateral fragility hip fracture is known, there is potential utility of routine magnetic resonance imaging to rule out contralateral radiograph-negative hip fracture even in the absence of symptoms. Further research examining the prevalence of such cases will be essential in determining the ideal diagnostic approach to cases with predisposing factors.
Credit Author Statement:
Sean Kean Ann Phua was responsible for acquisition of data from patient’s electronic medical records and manuscript writing.
Jegathesan T was the senior author responsible for conceptualization of study design and contributed towards manuscript writing and approval. All authors read and approved the final manuscript, and guarantee the integrity of the submitted work.
Conflicts of interests: The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Funding & Acknowledgements: The author received no specific funding or support for this work.
References
- Uzun E, Günay AE, Kızkapan TB, Mutlu M. Atraumatic diplaced bilateral femoral neck fracture in a patient with hypophosphatemic rickets in postpartum period: A missed diagnosis. International journal of surgery case reports, 2016; 28: 321-324.
- John R, Kumar P, Aggarwal S, Rajnish RK, Agarwal S, Vatsyan K. Simultaneous, non-traumatic, bilateral neck femur fractures in uremic renal Osteodystrophy: a report of three cases and literature review. Journal of Orthopaedic Case Reports, 2018; 8(2): 90.
- Sadiq M, Kulkarni V, Hussain SA, Ismail M, Nayak M. Low-velocity simultaneous bilateral femoral neck fracture following long-term antiepileptic therapy: A case report. World Journal of Orthopedics, 2019; 10(10): 371.
- Arisumi S, Mawatari T, Ikemura S, Matsui G, Iguchi T, Mitsuyasu H. Spontaneous bilateral femoral neck fractures in a young male adult: a case report and literature review. BMC Musculoskeletal Disorders, 2019; 20: 1-5.
- Dilernia FD, Estefan MM, Zanotti G, Comba F, Piccaluga F, Buttaro M. Simultaneous bilateral femoral neck fracture due to a tonic-clonic seizure and high-dose steroid therapy. Arthroplasty Today, 2020; 6(3): 513-516.
- Mitani Y. Effective treatment of a steroid-induced femoral neck fracture nonunion with a once-weekly administration of teriparatide in a rheumatoid patient: a case report. Archives of osteoporosis, 2013; 8: 1-3.
- Amiche MA, Abtahi S, Driessen JH, Vestergaard P, de Vries F, Cadarette SM, et al. Impact of cumulative exposure to high-dose oral glucocorticoids on fracture risk in Denmark: a population-based case-control study. Archives of Osteoporosis, 2018; 13: 1-10.
- Blankenstein T, Grainger A, Dube B, Evans R, Robinson P. MRI hip findings in asymptomatic professional rugby players, ballet dancers, and age-matched controls. Clinical radiology, 2020; 75(2): 116-122.
- Ibad HA, Ghotbi E, Kasaeian A, Levin AS, Jones LC, Anzai Y, et al. Screening for Asymptomatic Osteonecrosis of the Hip in Systemic Lupus Erythematous: A Systematic Review and Meta-Analysis of MRI-Based Prevalence. Diagnostics, 2024; 14(3): 279.

