Rectal Adenocarcinoma Associated with a Giant Tarlov Cyst: A Surgical Challenge
Bachar Amine, Benzidane Kamal*, Brahmi Soufiane, Essaidi Zakaria, El Abbassi Taoufik and Bensardi Fatima Zahra
Hassan II University of Casablanca, Morocco Institution: Department of Visceral Surgery, Ibn Rochd University Hospital, Casablanca, Morocco
Received Date: 14/07/2025; Published Date: 12/08/2025
*Corresponding author: Benzidane Kamal, Hassan II University of Casablanca, Morocco Institution: Department of Visceral Surgery, Ibn Rochd University Hospital, Casablanca, Morocco
Abstract
Background: Tarlov cysts are rare perineural formations that typically remain asymptomatic and incidentally discovered. Their coexistence with rectal adenocarcinoma represents a unique diagnostic and surgical challenge, especially when the cysts are large and involve the pelvic space.
Case Presentation: We report the case of a 35-year-old female presenting with rectal syndrome and a histologically confirmed mid-rectal adenocarcinoma. Imaging revealed a T4aN+Mx tumor with mesorectal invasion and contact with pelvic organs. Further radiological workup identified giant bilateral Tarlov cysts displacing the rectal fascia, complicating the surgical field. A multidisciplinary approach led to neoadjuvant chemoradiotherapy, followed by abdominoperineal resection. Neurosurgical involvement was anticipated but not required intraoperatively.
Conclusion: This case highlights the importance of thorough preoperative imaging and interdisciplinary collaboration when managing rectal cancer associated with presacral masses. Awareness of perineural cysts and their potential surgical implications is essential to avoid intraoperative complications and optimize outcomes.
Keywords: Rectal adenocarcinoma; Tarlov cyst; Laparoscopy; Surgical difficulty; Abdominoperineal resection; Multidisciplinary approach
Introduction
Tarlov cysts, or perineural cysts, are cerebrospinal fluid-filled sacs that typically develop at the sacral level near the dorsal root ganglia. Though often asymptomatic, their presence can pose significant diagnostic and therapeutic challenges when associated with pelvic pathologies. Concurrent rectal cancer and large presacral Tarlov cysts are extremely rare and present a unique set of surgical considerations. This report details the management of a rectal adenocarcinoma complicated by the presence of a giant Tarlov cyst, underscoring the importance of preoperative planning and multidisciplinary collaboration.
Case Report
A 35-year-old female patient, with no significant past medical history, presented with rectal syndrome associated with mild rectal bleeding and alternating diarrhea and constipation, evolving over the past 7 months in a context of weight loss of 10 kg.
Initial clinical examination found a patient with a Performance Status (PS) of 0. Digital rectal examination revealed a right-sided, hemispheric, budding rectal mass, located 4 cm from the anal verge. The remainder of the clinical exam was unremarkable: no suspicious palpable lymphadenopathy, no hepatomegaly, and no flank dullness.
A colonoscopy showed, between 5 to 9 cm from the anal verge, a right-sided, non-stenosing hemispheric mass, which was biopsied. The rest of the colon was normal. Histopathological examination revealed a well-differentiated Lieberkühnian adenocarcinoma infiltrating the muscularis mucosae.
A pelvic MRI demonstrated a tumoral process of the mid and upper rectum, located 55 mm from the anal verge, extending 75 mm in height, infiltrating the right mesorectum with 28 mm of extramural extension, involving the mesorectal fascia, and associated with mesorectal lymph nodes. The tumor was classified as T4aN+Mx.
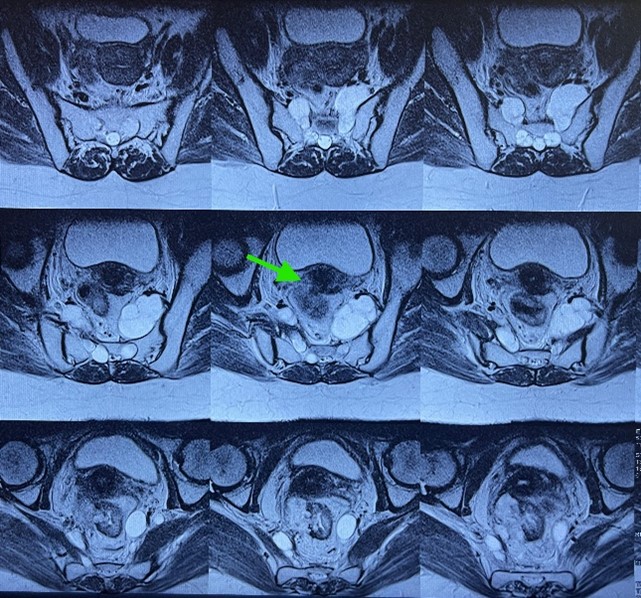
Figure 1: MRI image showing a tumoral process of the mid and upper rectum, infiltrating the right mesorectum.
A thoraco-abdominal CT scan did not show any secondary localization (no peritoneal, hepatic, pulmonary, or other metastases). Tumor markers were negative.
The case was discussed in a Multidisciplinary Tumor board (MDT), and the patient received concomitant neoadjuvant chemoradiotherapy.
Follow-up imaging showed on pelvic MRI a 30% reduction in tumor volume, with persistent mesorectal invasion and contact with the posterior wall of the uterus and vagina, with loss of the fat plane between them.
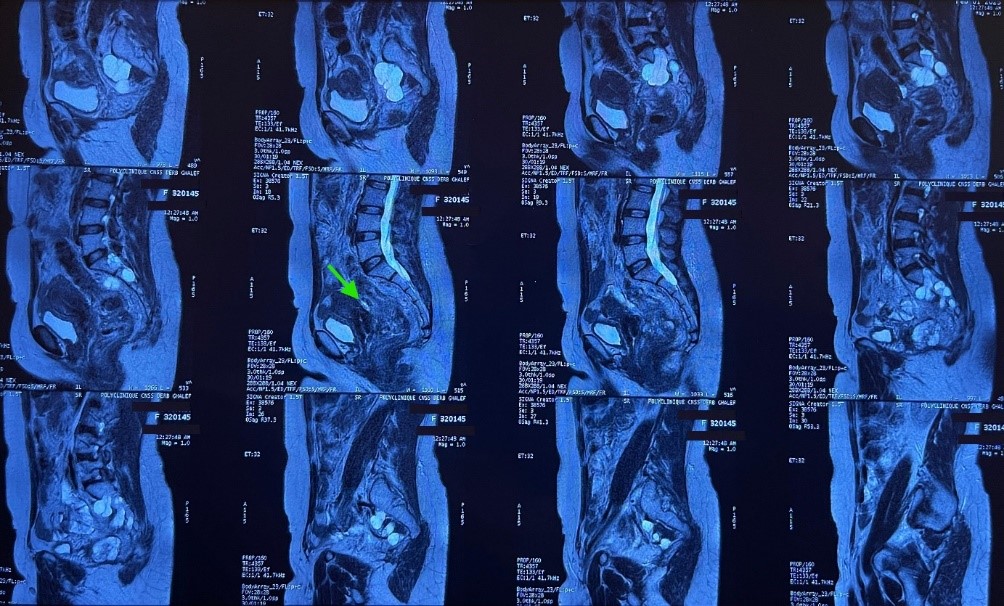
Figure 2: MRI image showing the contact of the tumor with the posterior wall of the uterus and vagina.
The follow-up thoraco-abdominal CT scan showed no secondary lesions, but the presence of two presacral formations, more prominent on the left, appearing to follow the S1 and S2 nerve roots at the sacral foramina, possibly corresponding to Tarlov cysts.
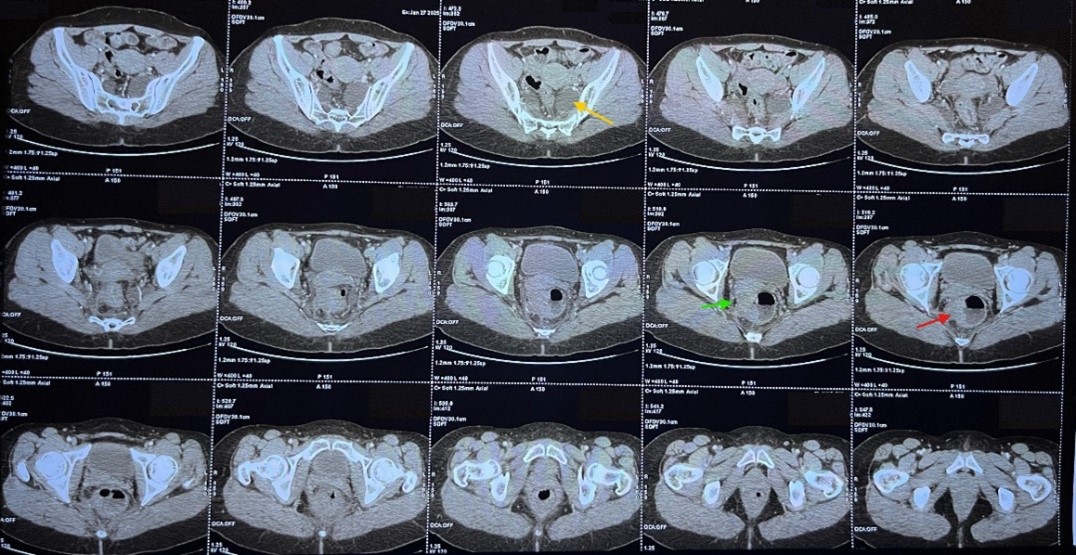
Figure 3: CT scan image demonstrating the Tarlov cysts (yellow arrow), the tumoral processus (red arrow) and the contact between the tumor and the uterus (green arrow).
This was further evaluated with a lumbar MRI, which revealed multiple bilateral periradicular cysts involving the S1-S2, S2-S3, and S3-S4 foramina, with endopelvic extension and bony scalloping. The largest cyst, on the left at S1-S2, measured 41 x 28 x 71 mm, displacing the rectal fascia.
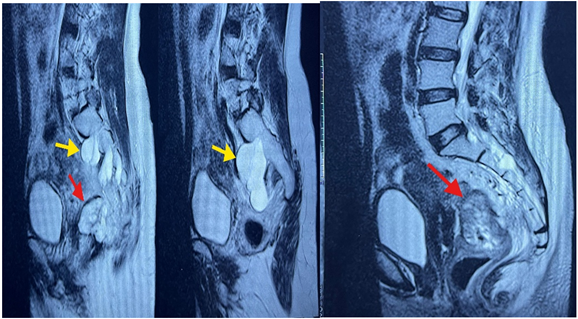
Figure 4: lumbar MRI image showing the Tarlov cysts (yellow arrow) and the rectal tumor (red arrow).
Neurosurgical consultation was requested. Given the absence of neurological symptoms, the decision was for therapeutic abstention, with instructions to be contacted intraoperatively if needed.
The patient was initially approached laparoscopically, with placement of a 10 mm umbilical trocar for optics, a 12 mm trocar in the right iliac fossa, and three 5 mm trocars in the right and left subcostal regions, and one suprapubic trocar.
Exploration revealed no peritoneal effusion, no hepatic nodules, and no peritoneal carcinomatosis. After douglasotomy and extrafascial dissection of the rectum, multiple Tarlov cysts were identified, the largest on the left, and a tumor of the mid and lower rectum, more pronounced on the posterolateral right side, appearing to invade the posterior aspect of the uterus.
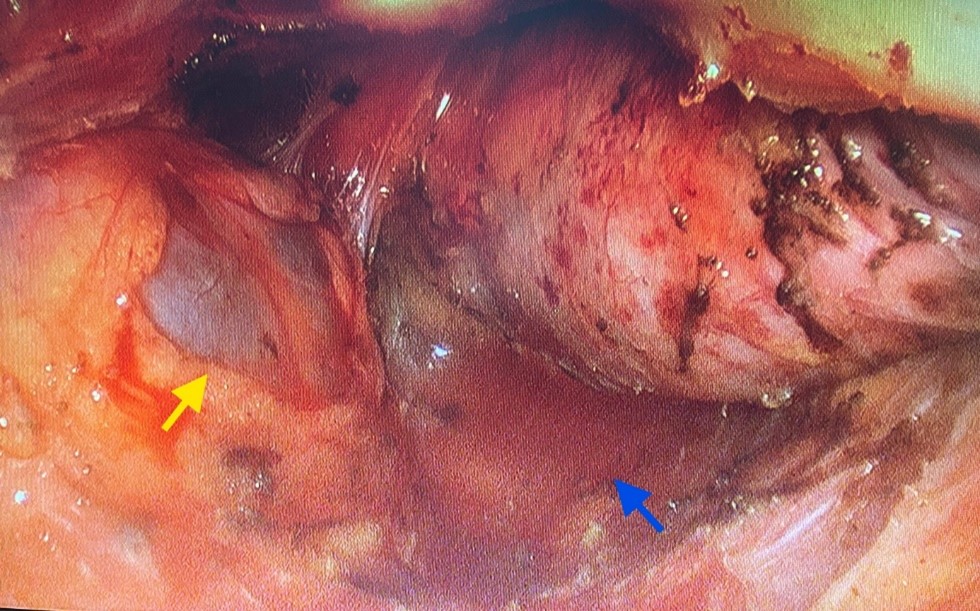
Figure 5: Laparoscopic image demonstrating the left Tarlov cyst (yellow arrow) after the extrafascial posterior dissection (blue arrow).
Due to the locally advanced nature of the tumor, the procedure was converted to open surgery via a Pfannenstiel incision. After careful extrafascial dissection, the tumor was found to invade the posterior vaginal wall.
The procedure performed was an abdominoperineal resection, removing the mid and lower rectal tumor along with a vaginal cuff, followed by a definitive left iliac colostomy (subperitoneal) and pelvic drainage with a Salem tube, and perineal drainage with a Joly drain.
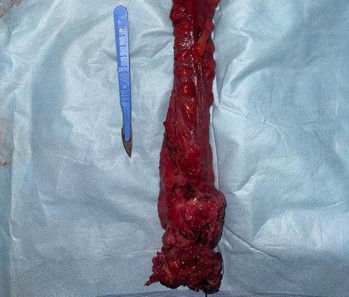
Figure 6: Surgical specimen from an abdominoperineal resection encompassing a tumor located in the lower and mid rectum.
Postoperative course was uneventful: oral feeding was allowed 6 hours post-op, and the stoma was functional by postoperative day 1. The drains, which collected only a few cc of serosanguinous fluid, were removed on post-op day 4. The patient showed no wound or pelvic infections and was discharged on postoperative day 5 with a referral letter to oncology and neurosurgery.
Discussion
Tarlov cysts are perineural cysts that form between the perineurium and endoneurium, typically near the dorsal root ganglion. Although they can develop at any level of the spine, they most commonly occur around the sacral nerve roots, with the S2 level being the most frequently affected [1].
The exact aetiology of Tarlov cysts remains unclear. These cysts are unlikely to regress spontaneously and may enlarge due to Cerebrospinal Fluid (CSF) inflow through a one-way valve mechanism. This valve effect is created by circular scarring of the arachnoid mater at the cyst's opening, which becomes a key target in certain surgical techniques aimed at restoring normal CSF dynamics and promoting cyst regression [2].
A recent meta-analysis reported a global prevalence of 4.27%, with a slightly lower rate of 3.82% in the United States. The condition shows a higher incidence in females [1].
Only 15.59% of Tarlov cysts are symptomatic [1]. When symptoms are present, patients typically report chronic or acute-on-chronic back pain, which may have a radicular character, accompanied by dermatomal pain, paresthesia, or motor weakness. On physical examination, findings can include diminished reflexes, reduced anal tone, sensory deficits, or muscle weakness [2].
Advancements in imaging, particularly CT myelography and MRI, have improved the identification of perineural cysts. Non-contrast CT may reveal cystic lesions isodense with CSF, often at the neural foramina. These lesions can lead to foraminal enlargement due to chronic pressure remodeling. Associated signs may include asymmetry of epidural fat and a widened dural sac. CT myelography can highlight the cyst with minimal contrast entry. However, MRI is the preferred imaging modality for evaluating sacral cysts due to its superior soft tissue resolution, lack of bony artifact, and multiplanar capabilities. Furthermore, MRI is noninvasive, obviating the need for a myelogram. On MRI, the cysts typically show low signal intensity on T1-weighted images and high intensity on T2-weighted sequences, consistent with CSF [3].
Treatment options include conservative, medical, and surgical approaches. For incidentally discovered and asymptomatic Tarlov cysts, conservative management is generally favored [2]. Surgical interventions, when indicated, may involve cyst excision or fenestration, followed by imbrication and dural repair. These repairs are often reinforced with a patch or fibrin sealant to minimize the risk of cerebrospinal fluid leakage.
We reported a case of a female patient who presented with rectal adenocarcinoma and was a candidate for surgical treatment following chemoradiotherapy. Pelvic MRI revealed the presence of an asymptomatic perineural (Tarlov) cyst. After multidisciplinary discussion with the neurosurgery team, it was decided that surgical treatment of the cyst was not indicated, as it could expose the patient to unnecessary complications associated with invasive procedures. However, we anticipated that the excision could be technically challenging due to the risk of inadvertent injury to the cyst, which would necessitate intraoperative repair. Therefore, the neurosurgery team was on standby to intervene if such a complication occurred.
The Surgical Difficulty Risk Score (SDRS) is a novel clinical scoring system, aim to assess predictors of surgical difficulty in laparoscopic total mesorectal excision (TME). Key predictive factors identified were [4-7]:
- Male gender: it had significantly more difficult operations, likely due to a narrower pelvis that makes dissection technically harder in low rectal tumors.
- High ASA score: is correlated with increased difficulty. This likely reflects underlying comorbidities, such as obesity.
- Tumor location: Low rectal cancers (including ultralow anterior resection and abdominoperineal resection) were associated with more challenging dissections, consistent with earlier findings.
- Nodal positivity and multivisceral resection: Both are indicators of more advanced disease and were independently associated with increased operative difficulty.
Identifying these variables preoperatively is crucial for improved informed consent regarding surgical risks and complications and selecting patients for alternative approaches [8,9].
Transanal total mesorectal excision (TaTME) was developed to overcome the technical challenges of a minimally invasive (ultra-) low anterior resection. This new technique has recently come under careful scrutiny as technical pitfalls were reported, in specific relation to the transanal approach [10]. Some studies suggest the feasibility of a transanal endoscopic proctectomy (TAEP) when achieving curative resection remains challenging for surgery due to unfavourable characteristics in selected cases. However, they insisted on the need to be cautious before generalizing the technique [11].
Conclusion
The coexistence of rectal adenocarcinoma and a giant Tarlov cyst is exceptionally rare and presents considerable diagnostic and operative challenges. This case illustrates the critical role of comprehensive imaging, MDT involvement, and intraoperative adaptability in managing such complex surgical scenarios. While the Tarlov cyst in this case did not require direct intervention, its presence influenced surgical planning and execution. Surgeons should remain vigilant for such anomalies to ensure safe and effective oncologic resection.
References
- Klepinowski T, Orbik W, Sagan L. Global incidence of spinal perineural Tarlov’s cysts and their morphological characteristics: a meta-analysis of 13,266 subjects. Surg Radiol Anat, 2021; 43(6): 855–863.
- Lim Y, Selbi W. Tarlov Cyst. In: StatPearls. Treasure Island (FL): StatPearls Publishing, 2025.
- Paulsen RD, Call GA, Murtagh FR. Prevalence and percutaneous drainage of cysts of the sacral nerve root sheath (Tarlov cysts). AJNR Am J Neuroradiol, 1994; 15(2): 293–297; discussion 298-299.
- Joseph C Kong, Swetha Prabhakaran, Alison Fraser, Satish Warrier, Alexander G Heriot. Predictors of surgical difficulty in laparoscopic total mesorectal excision. POL PRZEGL CHIR, 2021: 93(6): 33-39.
- Veenhof AA, Engel AF, van der Peet DL, et al. Technical difficulty grade score for the laparoscopic approach of rectal cancer: a single institution pilot study. Int J Colorectal Dis, 2008; 23(5): 469–475.
- Ogiso S, Yamaguchi T, Hata H, et al.: Evaluation of factors affecting the difficulty of laparoscopic anterior resection for rectal cancer: "narrow pelvis" is not a contraindication. Surgical endoscopy, 2011; 25(6): 1907–1912.
- Wu H, Zhang T, Chen X, et al. Factors affecting the difficulty of laparoscopy-assisted triple-port anterior resection. Zhonghua Wei Chang Wai Ke Za Zhi, 2018; 21(7): 779–785.
- Deijen CL, Velthuis S, Tsai A, et al. COLOR III: a multicentre randomised clinical trial comparing transanal TME versus laparoscopic TME for mid and low rectal cancer. Surgical endoscopy, 2016; 30(8): 3210–3205.
- Jayne D, Pigazzi A, Marshall H, et al. Effect of Robotic-Assisted vs Conventional Laparoscopic Surgery on Risk of Conversion to Open Laparotomy Among Patients Undergoing Resection for Rectal Cancer: The ROLARR Randomized Clinical Trial. JAMA, 2017; 318(16): 1569–1580.
- Vannijvel M, Wolthuis AM. Limitations and Concerns with Transanal Total Mesorectal Excision for Rectal Cancer. Clin Colon Rectal Surg, 2022; 35(2): 141–145.
- Rouanet P, Mourregot A, Azar CC, Carrere S, Gutowski M, Quenet F, et al. Transanal endoscopic proctectomy: an innovative procedure for difficult resection of rectal tumors in men with narrow pelvis. Dis Colon Rectum, 2013; 56(4): 408–415.

