A Rare Case report of Pleomorphic Adenoma in the Nasogenian Region: Diagnostic Challenge and Surgical Management
Naanani Othmane*, Rhnia A, Larhrabli I, Lahjaouj M, Loudghiri M, Bijou W, Oukessou Y, Rouadi S, Abada RL, Roubal M and Mahtar M
ENT and Cervicofacial Surgery Department, CHU Ibn Rochd, Faculty of Medicine and Pharmacy, Hassan II University, Casablanca
Received Date: 29/06/2025; Published Date: 30/07/2025
*Corresponding author: Naanani Othmane, ENT and Cervicofacial Surgery Department, CHU Ibn Rochd, Faculty of Medicine and Pharmacy, Hassan II University, Casablanca
Abstract
Background: Pleomorphic adenoma is the most common benign tumor of the salivary glands, typically affecting the parotid and minor salivary glands in the oral cavity. Ectopic localizations, particularly in the nasogenian or nasal vestibular region, are extremely rare and may lead to diagnostic confusion.
Case Presentation: We report the case of an 85-year-old man who presented with a longstanding, progressive swelling of the left nasogenian sulcus, along with an ulcerated mass on the inner right cheek. Imaging revealed two separate lesions without bony erosion or skin infiltration. Biopsy of the cheek lesion confirmed a pleomorphic adenoma. The left lesion was initially presumed to be a vestibular cyst.
Surgical excision of both lesions was performed: a para-lateral nasal approach for the left lesion due to dense adhesions, and an intraoral approach for the cheek lesion. Final histopathology surprisingly revealed that both lesions were pleomorphic adenomas of salivary gland origin, including an ectopic localization in the left nasal vestibule.
Conclusion: This case highlights an atypical presentation of pleomorphic adenoma in an unusual location, emphasizing the importance of including salivary gland tumors in the differential diagnosis of long- standing nasal vestibular masses. Histopathological confirmation remains essential, and complete surgical excision is the treatment of choice.
Keywords: Pleomorphic adenoma; Ectopic salivary tumor; Nasal vestibule; Nasogenian sulcus; Benign salivary gland tumor; Surgical excision
Introduction
Pleomorphic adenoma is the most common benign neoplasm of the salivary glands, typically arising from the parotid or minor salivary glands of the oral cavity, particularly in the hard palate, buccal mucosa, or lips. These tumors are characterized by their slow, painless growth, well-circumscribed nature, and biphasic histological composition involving epithelial and myoepithelial components within a mesenchymal-like stroma.
While the majority of pleomorphic adenomas present in predictable anatomic locations, ectopic or unusual localizations are rare and can present a diagnostic challenge.
Due to their atypical presentation and long-standing indolent course, such lesions are often misdiagnosed as epidermoid cysts, dermoid cysts, or benign soft-tissue masses. Preoperative imaging and histological confirmation are essential for appropriate surgical planning and to rule out the potential for malignant transformation.
Here, we present a rare case of a pleomorphic adenoma located in the nasogenian region of an 85-year-old man, initially presumed to be a benign cyst.
Case Report
We report the case of an 85-year-old male with no significant past medical history who presented to our department with a swelling in the region of the left nasal vestibule. The lesion had been progressively evolving over the past five years and was associated with an ulcerative, exophytic lesion on the internal aspect of the right cheek. No other associated symptoms were reported (Figure 1, 2).
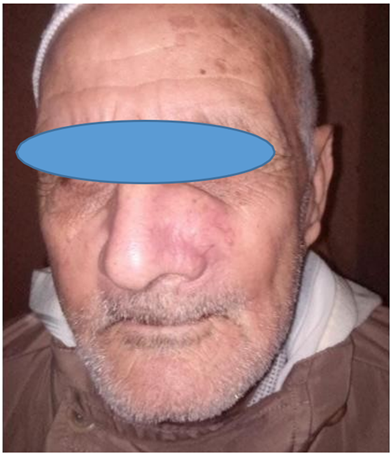
Figure 1: Image showing a swelling over the left nasogenian sulcus.
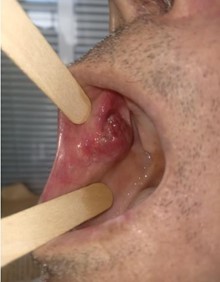
Figure 2: Image illustrating an ulcerative budding lesion lesion of the inner surface of the right cheek.
A maxillofacial CT scan was performed (Figure 3), revealing a lesion in the left nasogenian sulcus measuring 21.6 × 26 × 12.7 mm. It was in contact with the nasal bone and maxilla without any evidence of bony erosion. A second lesion was also identified in the right nasogenian sulcus, located anterior to the right masticator space and external paramaxillary region. This lesion was ovoid, well-defined, and measured 20 × 23 × 27 mm, with no evidence of infiltration or cutaneous thickening.
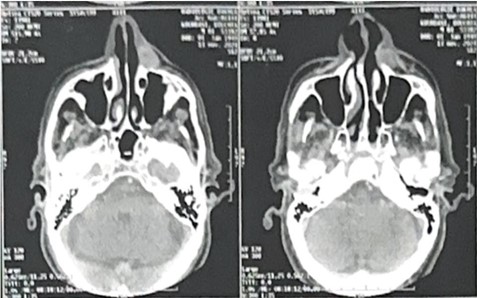
Figure 3: Axial facial CT scan showing the location of the mass in relation to the nasolabial fold.
A biopsy was performed on the ulcerated lesion of the inner cheek, and histopathological analysis revealed a pleomorphic adenoma. The lesion in the left nasogenian sulcus was initially considered to be a nasal vestibular cyst.
The therapeutic approach was surgical. The initial plan was to excise the left-sided lesion via a vestibular approach. However, due to subcutaneous tissue infiltration and strong adhesion of the mass to superficial planes, a para-lateral nasal approach was adopted instead.
Complete surgical excision was achieved.The lesion of the inner cheek was resected via an intraoral approach with layered closure (Figure 5, 6).
The postoperative course was uneventful, and the patient was discharged the following day.
Unexpectedly, the definitive histopathological examination of the lesion in the left nasal vestibule revealed a rare and atypical localization of a pleomorphic salivary gland adenoma.
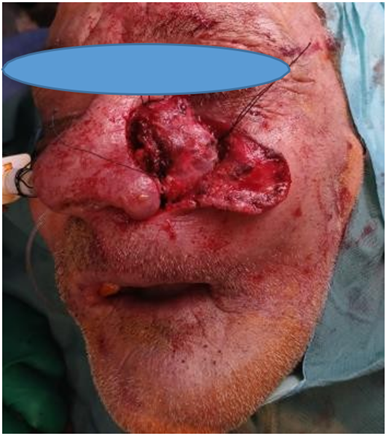
Figure 4: Intra operative view showing tumor resectionthrough a para-lateral nasal approach.
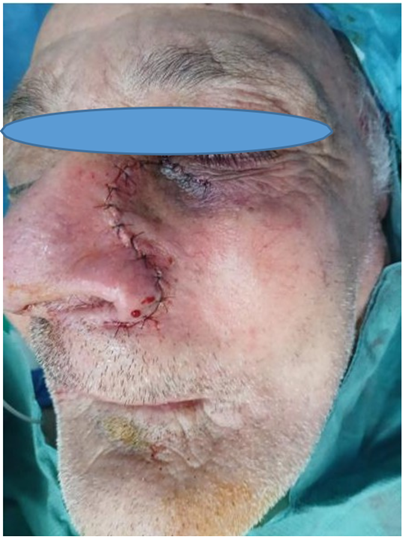
Figure 5: Postoperative view.
Discussion
Pleomorphic Adenoma (PA) is the most common benign salivary gland tumor, accounting for approximately 60–70% of benign salivary neoplasms and about 40% of all salivary gland tumors [1,2]. It primarily affects the parotid gland, followed by the minor salivary glands— most frequently located in the hard palate, upper lip, and buccal mucosa [3]. Ectopic or unusual presentations, particularly in the nasal vestibule or nasogenian region, are extremely rare and often misdiagnosed due to their atypical location and indolent progression.
The pathogenesis of PA in ectopic sites is not fully understood. Two main hypotheses have been proposed: (1) heterotopic salivary tissue remnants during embryologic development, particularly in areas where salivary glands are normally sparse (e.g., nasal cavity, nasopharynx, upper neck), and (2) neoplastic transformation of minor salivary gland cells present in ectopic mucosa or subcutaneous tissue [4,5].
Clinically, PA typically presents as a slow-growing, painless, and well-circumscribed mass. Its indolent evolution often leads to diagnostic delays, particularly in elderly patients who may ignore or adapt to the mass. In our case, the patient had a five-year history of a growing lesion without alarming symptoms. The simultaneous presence of a second lesion (inner cheek) added diagnostic complexity and initially suggested distinct etiologies.
Radiologically, PA appears as a well-defined, homogenous soft-tissue mass. On CT scans, it typically shows a non-invasive, rounded lesion without bone erosion or calcifications. MRI, which was not used in this case but is considered superior for soft tissue characterization, usually shows a lesion with low-to-intermediate signal intensity on T1-weighted images and high intensity on T2-weighted images, often with a well-defined capsule [6,7]. In our patient, the CT showed regular, ovoid lesions without bony destruction or signs of deep invasion, which supported a benign etiology.
Histologically, pleomorphic adenoma is composed of a mixture of epithelial and myoepithelial cells embedded in a chondromyxoid stroma. The lesion is usually well- encapsulated but may show microscopic pseudopodial extensions beyond its capsule, which can account for recurrence if incompletely excised [8]. The surprise in our case was the definitive histopathological diagnosis of PA in a highly atypical location—near the nasal vestibule and nasogenian sulcus—where minor salivary glands are not commonly found.
While pleomorphic adenoma is benign, there is a known risk of malignant transformation, particularly in long-standing lesions. The risk of transformation into carcinoma ex- pleomorphic adenoma is estimated at 5–10%, especially in tumors present for more than 10 years or those recurring multiple times [9,10]. Thus, complete surgical excision with adequate margins is essential, regardless of the location.
Surgical management of PA depends on the tumor's location, size, and proximity to critical structures. For intraoral or superficial facial lesions, a transoral or minimal access approach may suffice. In contrast, for lesions adherent to surrounding tissue or located in anatomically confined areas, more extensive approaches may be required. In our case, the para-lateral nasal approach was selected due to the lesion's subcutaneous infiltration and its firm adhesion to superficial planes, allowing for safe and complete removal. The cheek lesion was resected via an intraoral approach, which is standard for such locations [11].
The rarity of pleomorphic adenoma in the nasal vestibule or adjacent areas has been documented only in isolated case reports or small series. Compagno and Wong (1977) first described intranasal PA in a series of 20 cases, emphasizing their histologic similarity with their oral counterparts but clinical variability [12]. Since then, sporadic reports have described PA in locations such as the nasal septum, columella, and even the lateral nasal wall [13–15].
Our case is notable for presenting two synchronous pleomorphic adenomas, one in a typical site (inner cheek) and another in a highly atypical one (left nasogenian sulcus / nasal vestibule), both histologically benign. To our knowledge, such a synchronous dual presentation in an elderly patient is extremely rare.
Conclusion
Pleomorphic adenoma can present in unusual, ectopic locations, making clinical diagnosis difficult, particularly in elderly patients with long-standing masses. Imaging and biopsy can guide preoperative suspicion, but definitive diagnosis relies on histopathological analysis. Complete surgical excision remains the gold standard for treatment. This case underscores the importance of considering pleomorphic adenoma in the differential diagnosis of persistent nasal or facial swellings, even in atypical sites.
References
- Barnes L, Eveson JW, Reichart P, Sidransky WHO Classification of Tumours. Pathology and Genetics of Head and Neck Tumours. IARC Press, 2005.
- Speight PM, Barrett Salivary gland tumours. Oral Dis, 2002; 8(5): 229–240.
- Vaidya S, Neupane Y, et Pleomorphic adenoma of minor salivary glands: a review. JNMA J Nepal Med Assoc, 2020; 58(229): 240–245.
- Willis The Borderland of Embryology and Pathology. London: Butterworths, 1958.
- DeRoche TC, Wang Unusual locations of pleomorphic adenoma: case series and literature review. Am J Otolaryngol, 2013; 34(6): 703–706.
- Gritzmann N, Ofner D, Helweg G, Henk Real-time sonography of head and neck tumors. Radiol Clin North Am, 1988; 26(1): 129–144.
- Ikeda K, Katoh H, et MRI of salivary gland tumors: usefulness for differentiating benign from malignant lesions. Eur Radiol, 2004; 14(12): 2159–2166.
- Zbären P, Zbären S, et Pleomorphic adenoma of the parotid gland: histopathologic features and risk of recurrence. Laryngoscope, 2005; 115(4): 650–655.
- Olsen KD, Lewis Carcinoma ex pleomorphic adenoma: a clinicopathologic review. Head Neck, 2001; 23(9): 705–712.
- Antony J, Gopalan V, Smith RA, Lam AK. Carcinoma ex pleomorphic adenoma: a comprehensive review of clinical, pathological and molecular Head Neck Pathol, 2012;6 (1): 1–9.
- Iqbal A, Mannan A, et Surgical management of minor salivary gland tumors: a 10-year experience. Br J Oral Maxillofac Surg, 2020; 58(9): 1052–1057.
- Compagno J, Wong Intranasal tumors: a clinicopathologic study of 20 cases. Laryngoscope, 1977; 87(5 Pt 1): 763–773.
- Durbec M, de Bonnecaze G, et al. Pleomorphic adenoma of the nasal septum: diagnostic pitfalls and therapeutic Eur Ann Otorhinolaryngol Head Neck Dis, 2016; 133(2): 127– 130.
- Yao M, El-Naggar AK, et Pleomorphic adenoma of the nasal cavity: a rare site for a common tumor. Ear Nose Throat J, 2001; 80(3): 163–166.
- Gupta R, Rattan KN, et Pleomorphic adenoma of nasal septum: a rare case report and literature review. Indian J Otolaryngol Head Neck Surg, 2011; 63(3): 300–302.

