Early Integration of Panniculectomy Following Bariatric Surgery in a High-Risk Patient: A Case Report and Review of the Literature
Abshiro H Mayow1,*, Sachika Gandhi2, Naira Nuritdinova1, Asem Saefan3 and Frederick Tiesenga4
1St George’s University School of Medicine, Grenada
2Spartan health sciences university
3Windsor University School of Medicine, St. Kitts
4Department of Surgery, Community First Medical Center, Chicago, IL, USA
Received Date: 25/05/2025; Published Date: 11/07/2025
*Corresponding author: Abshiro H Mayow, St George’s University School of Medicine, Grenada
Abstract
Morbid obesity is a critical risk factor for cardiovascular disease, and bariatric surgery is a cornerstone intervention to achieve substantial weight loss and mitigate cardiovascular risk. However, massive weight reduction often results in a residual abdominal pannus—an overhanging apron of skin and adipose tissue—that poses clinical challenges. Many post-bariatric patients develop a large panniculus, particularly those older or with higher preoperative BMIs. This redundant tissue contributes to intertriginous skin infections, hygiene difficulties, and mechanical limitations that hinder mobility, potentially blunting weight loss’s full cardiovascular and metabolic benefits. Despite its prevalence, there is a limited consensus on the optimal timing and patient selection for panniculectomy (surgical removal of the pannus) as an adjunct to bariatric surgery. Current guidelines typically advise deferring such body-contouring until weight has plateaued (often 12–18 months post-surgery), leaving a gap in care for patients with persistent functional impairment due to an extensive pannus.
We report a case of a 60-year-old African American male (BMI 60.8) with type 2 diabetes mellitus, cardiomyopathy, obstructive sleep apnea, and other obesity-related comorbidities who underwent a staged approach of laparoscopic adjustable gastric banding followed by panniculectomy one year later. Intraoperatively, a 15.23 kg pannus was excised without complication. At one-year follow-up post-panniculectomy, the patient’s BMI decreased to 45.1, with marked improvements in glycemic control, cardiac function, mobility, and overall quality of life. Thus, this case highlights the potential benefits of integrating panniculectomy relatively early in the bariatric treatment course for select patients. In those with refractory morbid obesity and a debilitating pannus impeding further weight loss or exercise, early removal of excess abdominal tissue may enhance functional recovery and amplify the cardiovascular risk reduction achieved by bariatric surgery.
Introduction
Panniculectomy has become increasingly common in the setting of rising obesity and bariatric surgery rates, aiming to relieve functional impairments caused by excess skin and subcutaneous tissue following massive weight loss [1]. Panniculectomy is a procedure performed on patientswith a large overhanging abdominal panniculus. A panniculus is a severe form of lymphedema and excessive folds of adipose tissue settled in the abdominal area and is often associated with morbid obesity [2]. This is a debilitating condition most commonly observed in individuals with longstanding morbid obesity. Affecting mobility, hygiene, and quality of life, this condition often persists despite significant weight loss, particularly following bariatric surgery [3]. Obesity continues to affect over 42% of adults in the United States, and more than 9% meet the criteria for severe obesity (BMI ≥ 40 kg/m²), making complications such as panniculus formation increasingly prevalent [4]. The pathophysiology involves progressive adipose hypertrophy, compromised lymphatic drainage, and mechanical strain on the abdominal wall, leading to chronic inflammation and tissue edema. Clinically, patients present with secondary symptoms such as chronic skin infections, intertriginous rashes, ventral hernias, and mobility impairment [5]. Despite its significant functional burden, panniculus morbidus remains underdiagnosed and undertreated, and literature describing its post-bariatric course is limited. Diagnostic assessment is primarily clinical and supported by imaging in complex cases, yet consensus on optimal timing and indications for surgical intervention remains unclear [6]. Given the growing prevalence and impact of panniculus morbidus, understanding the therapeutic role and risks of surgical intervention is essential.
Surgical panniculectomy is the primary treatment for symptomatic panniculus when conservative management fails [1].. Though technically elective, panniculectomy can offer substantial functional benefits, including enhanced ambulation, infection reduction, and improved psychosocial well-being. However, it is not without risk—recent multicenter analysis reports postoperative complication rates as high as 56%, particularly among patients with elevated BMI, diabetes, and cardiopulmonary comorbidities [7]. Surgical site infections, seromas, wound dehiscence, and delayed healing are among the most common complications. While panniculectomy is often deferred until weight loss has plateaued, this traditional approach may not serve all patients, especially those with severe comorbidities whose health status may benefit from earlier intervention. Literature lacks consensus on the safety and utility of performing panniculectomy in tandem with, or shortly after, bariatric procedures [8]. As a result, more clinical data are needed to inform guidelines on timing, patient selection, and outcome optimization.
This report presents the case of a 60-year-old African American male with a BMI of 59.4 kg/m² and a history of multiple obesity-related comorbidities, including type 2 diabetes mellitus, hypertension, cardiomyopathy, and sleep apnea. Despite undergoing laparoscopic adjustable gastric banding (lap band), the patient had limited functional improvement due to a massive abdominal pannus, prompting surgical panniculectomy. The patient tolerated the operation well and had a panniculus of 15.23 kg. Surgery was uneventful, and the patient was discharged the same day of the procedure. At three months follow-up, the patient had no complaints or signs of infections or reactions. This case explores the role of panniculectomy as a therapeutic adjunct to bariatric surgery, examining its impact on cardiometabolic risk, functional recovery, and overall patient well-being. It raises the question: Can early integration of panniculectomy in select high-risk patients enhance outcomes beyond what bariatric surgery alone can offer?
Case Presentation
A 60-year-old morbidly obese African American male patient was referred for a bariatric consult by his primary physician. Two years ago, he had laparoscopic adjustable gastric banding (lap band) due to morbid obesity. After the intervention, his BMI remained high, and he still had severe medical problems due to his comorbidities, including hypertension, hypercholesterolemia, diabetes, arthritis, emphysema, sleep apnea, cardiomyopathy, and aortic sclerosis. His surgical history included arthroscopic knee procedure, laparoscopic cholecystectomy, and an incarcerated open recurrent incisional hernia repair. On physical examination, he had abundant abdominal fat, which aggravated his chronic conditions and limited his mobility. His functional status was significantly impaired by the pannus, which resulted in hygiene problems, limited activity, and emotional discomfort in social settings. On follow-up visits, the patient complained of a painful intertrigo with fungal infections, physical and emotional distress significantly impacting his daily life. The patient reported pain and limitation, such as in routine activities (walking, hygiene, and sleeping), prompting him to seek surgical intervention.
Upon assessing the patient, it was clear that the pannus, as observed in Figure 1a (Sagittal view) and Figure 1b (Frontal view), was very large and visibly impacted his quality of life. The excess fat brought The patient was complaining about the persistent abdominal obesity, which was not permitting him to enjoy the optimum outcomes of his previous lap band surgery. Based on a thorough evaluation of the patient's cardiovascular risk factors and his poor functional status, it was agreed to proceed with panniculectomy to ease the physical burden and improve his health. Because of the severity of his comorbid conditions, sleep apnea, and cardiomyopathy, a decision was made that removal of his excess panniculus would not only improve his quality of life. However, it may enhance the control of his chronic diseases. After risks and benefits were discussed, the patient consented to the procedure.
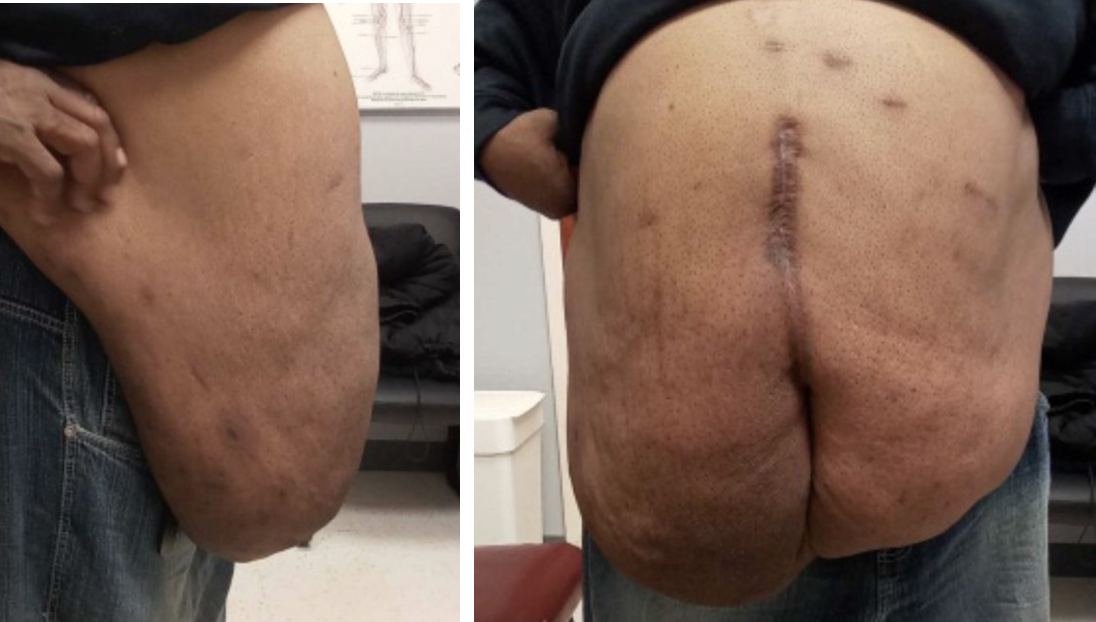
Figure 1a (left): Lateral View of the Abdomen Pre-Panniculectomy;
Figure 1b (Right): Anterior View of the Patient Pre-Panniculectomy.
Surgical Procedure
The patient underwent panniculectomy in a sterile surgical setting. He was supine and secured with Sequential Compression Devices (SCDs) on his legs. After administering anesthesia, the abdomen was prepped and draped, and a timeout was performed to confirm the surgical site. A circular incision was made around the umbilicus, and a low transverse incision was made between the anterior superior iliac spines at the pubic symphysis. A large flap of excess panniculus was removed, totaling 15.23 kg. The umbilicus was repositioned through a midline trephine, and the surgical site was meticulously closed in layers. Drains were placed, and a vacuum-assisted closure (VAC) was applied to promote healing.
Post-Operative Course and Recovery
The procedure was uneventful. The pannus biopsy showed chronic inflammation, vascular congestion, and the presence of inflammatory cells in the epidermis and dermis, as seen in Figure 2, which highlights the inflammatory process. The adipose tissue was examined under histological analysis, and Figure 3 illustrates some fat cells in the tissue. This biopsy finding was significant because the chronic inflammation and tissue destruction in the panniculus produced the patient's chronic signs of skin irritation, potential for infection, and restricted mobility. This tissue had to be removed to improve both his overall physical health and reduce cardiovascular risks due to his excess fat in the abdomen. The patient was discharged after surgery on the same day with an abdominal binder and provided with written and verbal discharge instructions.
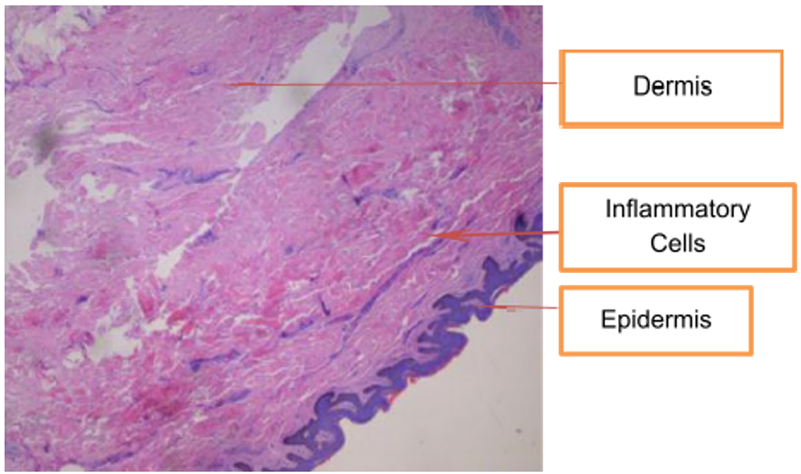
Figure 2: Shows that epidermis and dermis both contain inflammatory cells.
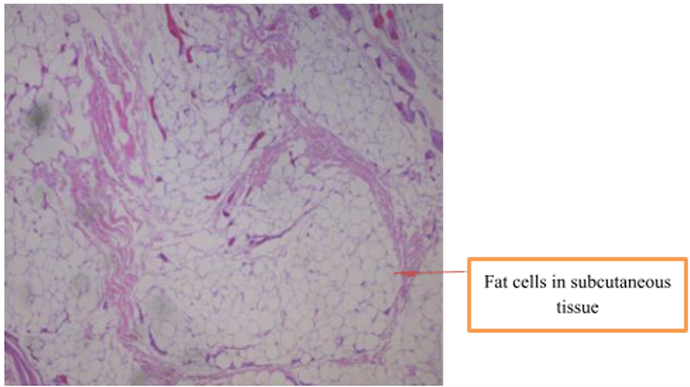
Figure 3: Shows adipose tissue containing fat cells.
The patient was free of complications at the initial follow-up, one week post-operatively. The wound healed well, with no infection, erythema, or edema. The patient experienced some pain, but this was adequately controlled with pain medication. The patient's functional status was improved at this point, with less pain on movement. Three months later, the patient's BMI remained 42.68 kg/m², a significant drop from pre-op. The patient was more active, had more energy, and could perform daily activities, which he could not do because of the pannus. All his post-operative vital signs were in range, and all was well at the surgery site. The patient was closely monitored in the post-operative months and has responded well to the combined treatment strategy. Our Patient’s BMI decreased significantly, to 45.1, compared to a noteworthy improvement from preoperative values. Laboratory data reported an improvement in his blood glucose control (glucose: 121 mg/dL) and hemoglobin levels (Hb: 8.3), reflecting better metabolic function. Functionally, the patient reported increased mobility, higher activity level during the day, and reduced physical discomfort. Panniculectomy combined with lap band adjustment allowed for substantial weight loss and better management of his comorbidities, with a general superb outcome.
Discussion
Obesity continues to represent a significant global health burden, affecting more than 650 million adults worldwide and contributing to substantial morbidity and disability [9]. Severe obesity (BMI ≥ 40 kg/m²) significantly elevates the risk of chronic conditions such as type 2 diabetes, sleep apnea, and functional limitations [5]. Bariatric surgery, including laparoscopic adjustable gastric banding, is often indicated when lifestyle and pharmacological interventions fail to achieve meaningful weight loss or metabolic control [10]. However, even after surgical intervention, many patients experience excess abdominal skin (pannus), which contributes to persistent physical discomfort, limited mobility, poor hygiene, and psychosocial distress [3]. These impairments justify the consideration of panniculectomy as a reconstructive, rather than cosmetic, procedure to restore baseline function and quality of life [2]. These widespread clinical impairments set the foundation for evaluating surgical options like panniculectomy, not only as aesthetic procedures but as medically necessary interventions in select high-risk patients.
In this case, a 60-year-old African American male with a BMI of 59.4 kg/m² and multiple comorbidities, including type 2 diabetes, hypertension, cardiomyopathy, and obstructive sleep apnea, underwent laparoscopic adjustable gastric banding with only modest weight loss. His progress plateaued due to a massive, symptomatic pannus that restricted movement and daily activities. The patient subsequently underwent panniculectomy, resulting in the excision of 15.23 kg of panniculus tissue. Following surgery, the patient experienced a significant enhancement in his ability to engage in physical activities such as daily exercises, which led to massive weight reduction and improved glycemic control. At 3-month and 1-year follow-up, his increased mobility allowed him to walk longer distances and maintain an active lifestyle, reducing his BMI to 45.1 kg/m² and improving his glycemic control and overall metabolic function. Such changes illustrate that panniculectomy is instrumental in restoring functional independence, improving physical activity, and enhancing the benefits of prior bariatric surgery. This patient’s postoperative course highlights the value of addressing pannus-related limitations early in the treatment trajectory to achieve gains beyond what bariatric surgery alone could offer The justification for panniculectomy in this clinical setting is reinforced by the challenges of managing panniculus morbidus, which not only causes mechanical strain and intertriginous infections but also serves as a barrier to physical activity, an essential component of long-term weight maintenance [5]. Although this might appear straightforward, panniculectomy can present significant complications due to the fragile nature of the tissue and comorbidity burden in this patient population, emphasizing the importance of careful patient optimization and perioperative planning [1]. For instance, a recent meta-analysis examining complication rates and surgical outcomes of body contouring after massive weight loss highlighted the critical role of patient selection and procedural timing in optimizing outcomes [11]. According to another investigator in a 2015 study of 325 patients, further demonstrated the feasibility of combining panniculectomy with bariatric surgery via laparotomy, reporting manageable complication rates and supporting its role in post-bariatric care [12]. In contrast, this patient experienced significant weight loss after panniculectomy, as removing the 15.23 kg pannus improved mobility, allowing him to participate in physical activities such as walking and weight reduction exercises, suggesting an alternative approach for select high-risk individuals. While literature traditionally favors delaying panniculectomy until weight plateaus, this case highlights that the pannus may impede weight loss and prolong functional limitations. Complication rates remain a concern, with studies reporting rates up to 56% in high-risk populations [7,13,14]. A 2018 study specifically identified diabetes as a significant predictor of adverse events, underscoring the need for meticulous patient selection and perioperative optimization. However, evidence suggests that panniculectomy can be safely performed even in high-BMI patients when tailored to individual risk profiles, yielding substantial quality-of-life improvements and reduced healthcare burdens [6,8]. These findings collectively justify the importance of early panniculectomy in appropriately selected patients to improve physical and psychological outcomes.
Ultimately, this case supports current literature’s emphasis on the need for individualized surgical planning and challenges the dogma of postponing panniculectomy until complete weight loss stabilization [3,12,13]. The patient's successful outcome and increased capacity for exercise underscore panniculectomy’s potential role in reactivating functional improvement and metabolic progression when weight loss is stalled due to mechanical limitations. The excised pannus tissue showed histologic signs of chronic inflammation, possibly contributing to systemic effects impeding recovery [2,15]. Future studies should evaluate early panniculectomy in larger cohorts, identifying patient profiles most likely to benefit from early intervention. Longitudinal data assessing quality of life, weight trajectories, and recurrence of comorbidities will be critical in refining timing criteria and postoperative expectations [16,17]. Beyond physical outcomes, the psychological benefits of post-bariatric interventions are well-documented, with evidence suggesting that procedures like panniculectomy may synergize with metabolic improvements to enhance mental health and body image satisfaction, aligning with findings on the broader psychosocial impact of bariatric care [18,19]. This case urges the potential role of early panniculectomy in optimizing quality of life, functional capacity, and sustained weight loss in high-risk bariatric patients, warranting further investigation through larger, multi-center studies to refine timing, safety, and patient selection criteria.
Conclusion
This case report examines the role of early panniculectomy as a medically necessary adjunct to bariatric surgery in a high-risk patient with morbid obesity and significant functional impairment. Despite undergoing laparoscopic adjustable gastric banding, the patient’s persistent panniculus hindered mobility, hygiene, and further weight loss. Surgical excision of the 15.23 kg pannus resolved these physical limitations, allowing the patient to become more active. This led to a meaningful reduction in BMI and improved management of diabetes and sleep apnea. These outcomes highlight the potential utility of early panniculectomy in restoring physical function and facilitating long-term postoperative progress when a debilitating pannus impedes recovery.
Clinically, this case challenges the traditional view of panniculectomy as purely elective or cosmetic and supports reclassifying it as a functional procedure in select cases. Findings from this case, along with existing literature, emphasize the importance of individualized surgical planning and the potential benefits of earlier intervention in appropriately optimized patients. However, as this is a single case, further prospective research is necessary to determine the ideal timing, patient selection criteria, and long-term quality-of-life outcomes. Early panniculectomy may serve as a pivotal therapeutic tool to unlock the full benefits of bariatric surgery for high-risk patients. As obesity-related surgery evolves, redefining the timing and purpose of adjunct procedures like panniculectomy may be essential to optimizing patient-centered outcomes.
References
- Janis JE, Jefferson RC, Kraft CT. Panniculectomy: Practical Pearls and Pitfalls. Plastic and Reconstructive Surgery Global Open, 2020; 8(8): e3029. https://doi.org/10.1097/GOX.0000000000003029.
- Chen N, Daly TK, Ooi Panniculectomy for a rare end-stage complication of severe obesity and increasing surgical phenomenon. Cureus, 2024.
- Sachs D. Panniculectomy. StatPearls, 2023.
- Emmerich SD, Fryar CD, Stierman B, Ogden Obesity and Severe Obesity Prevalence in Adults: United States, August 2021-August 2023. NCHS data brief, 2024; 508: 10.15620/cdc/159281. https://doi.org/10.15620/cdc/159281
- Aruwa CE, Sabiu S. Adipose tissue inflammation linked to obesity: A review of current understanding, therapies and relevance of phyto-therapeutics. Heliyon, 2024; 10(1): e23114. https://doi.org/10.1016/j.heliyon.2023.e23114
- Winicki NM, Florissi IS, Michelotti MJ, Srikureja DP. Panniculus morbidus resection complicated by multiple gastrointestinal hernias: A case report. Annals of Medicine and Surgery, 2022; 80: https://doi.org/10.1016/j.amsu.2022.104177.
- Cadwell JB, Ahsanuddin S, Ayyala HS, Ignatiuk A. Panniculectomy outcomes by body mass index: An analysis of 12,732 cases. Obesity Surgery, 2021; 31(8): 3660–3666. https://doi.org/10.1007/s11695-021-05468-w.
- Kalmar CL, Park BC, Kassis S, Higdon KK, Perdikis G. Functional panniculectomy vs cosmetic abdominoplasty: Multicenter analysis of risk factors and complications. Journal of plastic, reconstructive & aesthetic surgery: JPRAS, 2022; 75(9): 3541–3550. https://doi.org/10.1016/j.bjps.2022.04.057.
- Boutari C, Mantzoros CS. A 2022 update on the epidemiology of obesity and a call to action: As its twin COVID-19 pandemic appears to be receding, the obesity and dysmetabolism pandemic continues to rage Metabolism, 2022; 133: 155217. https://doi.org/10.1016/j.metabol.2022.155217
- Elmaleh-Sachs A, Schwartz JL, Bramante CT, Nicklas JM, Gudzune KA, Jay M. Obesity Management in Adults: A Review. JAMA, 2023; 330(20): 2000–2015. https://doi.org/10.1001/jama.2023.19897.
- Hasanbegovic E, Sørensen JA. Complications following body contouring surgery after massive weight loss: a meta-analysis. Journal of plastic, reconstructive & aesthetic surgery: JPRAS, 2014; 67(3): 295–301. https://doi.org/10.1016/j.bjps.2013.10.031.
- Colabianchi V, Giovannini M, Langella Panniculectomy Combined with Bariatric Surgery by Laparotomy: An Analysis of 325 Cases. Surgery Research and Practice, 2015; 2015(1): 193670. https://doi.org/10.1155/2015/193670.
- Derickson M, Phillips C, Barron M, Kuckelman J, Martin M, DeBarros M. Panniculectomy after bariatric surgical weight loss: Analysis of complications and modifiable risk factors. American journal of surgery, 2018; 215(5): 887–890. https://doi.org/10.1016/j.amjsurg.2018.02.008.
- Kantar RS, Rifkin WJ, Wilson SC, David JA, Diaz-Siso JR, Levine JP, et al. Abdominal panniculectomy: determining the impact of diabetes on complications and risk factors for adverse events.Plast. Reconstr. Surg., 2018; 142(4): pp. 462e-471e. doi: 1097/PRS.0000000000004732.
- Farhana A, Rehman Metabolic Consequences of Weight Reduction. In: StatPearls. Treasure Island (FL): StatPearls Publishing, 2025.
- Datta G, Cravero L, Margara A, Boriani F, Bocchiotti MA, Kefalas The plastic surgeon in the treatment of obesity. Obesity surgery, 2006; 16(1): 5–11. https://doi.org/10.1381/096089206775221989.
- Crossan K, Sheer AJ. Surgical Options in the Treatment of Severe Obesity. In: StatPearls. Treasure Island (FL): StatPearls Publishing, 2025.
- Kubik JF, Gill RS, Laffin M, Karmali The impact of bariatric surgery on psychological health. Journal of obesity, 2013; 837989. https://doi.org/10.1155/2013/837989.
- Francois Z, Rizvi A. Psychiatric Complications of Bariatric Surgery. [Updated 2024 May 17]. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2025.

