Case Report of Endobronchial Chondroma Presenting with Recurrent Respiratory Infections – A Rare Benign, But Troublesome Bronchial Tumor
Maciej Paciorkowski1,*, Lukas Kern2, Tino Schneider1, Florent Baty1, Natalia Vélez Char3 and Martin Brutsche1
1Department of Pneumology & Sleep Medicine Kantonsspital St. Gallen, St. Gallen, Switzerland
2Division of Pulmonary Medicine, Kantonsspital Winterthur, Winterthur, Switzerland
3Department of Pathology, Kantonsspital St. Gallen, St. Gallen, Switzerland
Received Date: 12/02/2025; Published Date: 20/03/2025
*Corresponding author: Maciej Paciorkowski, Department of Pneumology & Sleep Medicine Kantonsspital St. Gallen, St. Gallen, Switzerland
Abstract
We report the case of a 78 –year-old male, still practicing pediatrician, with a medical history of recurrent respiratory infections for the past decades treated with antibiotics. He was referred with a suspicion of an endobronchial malignancy with endoluminal polypoid lesion occluding the right lower lobe bronchus. The tumor was exstirpated completely using laser cauterization. Tissue sampling showed fragments of mature hyaline cartilage with no evidence of malignancy, consistent with the diagnosis of chondroma. Chondromas are rare tumors of the tracheobronchial tree usually involving the lung parenchyma. They usually do not cause any symptoms, however in some cases, they may lead to non-specific symptoms like cough, pneumonia, hemoptysis, wheezing or dyspnea. Benign endobronchial tumors should be considered as a differential diagnosis in recurrent respiratory infections and evaluation with chest CT and bronchoscopy is warranted. Bronchoscopic resection is considered standard of care in cases without involvement of lung parenchyma.
Keywords: Benign tumors; Pulmonary lesion; Chondroma; Respiratory infections
Introduction
Endobronchial chondromas are rare benign tumors of the respiratory system. They are described in the medical literature almost exclusively in case reports [1-3]. Chondromas usually do not cause any specific symptoms, but in some cases, they may cause bronchial obstruction, cough or recurrent respiratory infections or may incidentally be found in computed tomography (CT) scans.
We present a case of a successful diagnosis and management of an endobronchial chondroma that caused recurrent respiratory infections and was incidentally detected on a chest-CT scan.
Case Report
A 78 –year-old male still practicing paediatrician and nonsmoker with no relevant past medical history was referred to our pulmonary consultation after detection of a partially calcified endobronchial tumor in a CT scan. His medical history was remarkable for recurrent respiratory infections treated with antibiotics. The episodes had been present for the past years and occur 2 to 3 times per year. The patient reported recurrent acute illness with productive cough and purulent sputum. During the infection-free interval he reported no dyspnea, wheezing or cough. Clinical examination upon presentation was normal. The patient was afebrile and normotensive with normal pulmonary auscultation. Pulse oximetry showed a saturation of 95% upon breathing room air. His pulmonary function test was normal (FEV1 3.02 L – 93% predicted, FVC 4.52L – 103% predicted with an FEV1/FVC of 67%. A methacholine challenge test was negative. Laboratory studies revealed a normal blood count. Immunoglobulins, including IgG, IgM and IgG were within normal range. CT scan of the chest demonstrated an endoluminal, calcified polypoid lesion of 9mm diameter, occluding the right lower lobe bronchus with no signs of post-obstructive lung alterations or lymphadenopathy (Figure 1 and 2).
Consecutively, flexible bronchoscopy was performed and showed an almost complete obstruction of the right lower bronchus by a solid, spherical, pediculated and vascularized endobronchial mass at the medial aspect of the lower lobe bronchus (Figure 3). Biopsies taken by forceps revealed well-differentiated hyaline cartilage located under the normal respiratory epithelium.
A few days later the patient was admitted to the hospital to undergo rigid bronchoscopy under general anesthesia and the tumor was resected in total using laser cauterization (Figures 4 and 5). After resection, a localized ectasis of the lower lobe bronchus was evident.
Histological examination of the tumor showed fragments of mature hyaline cartilage covered by respiratory epithelium with no evidence of malignancy (Figures 6 and 7). All of the findings were consistent with the diagnosis of pulmonary chondroma.
The patient was discharged after an uneventful recovery. Follow-up bronchoscopy performed 3 months after the resection revealed no residual tumor tissue or tumor recurrence. The patient remained asymptomatic after the resection; no further infection appeared.
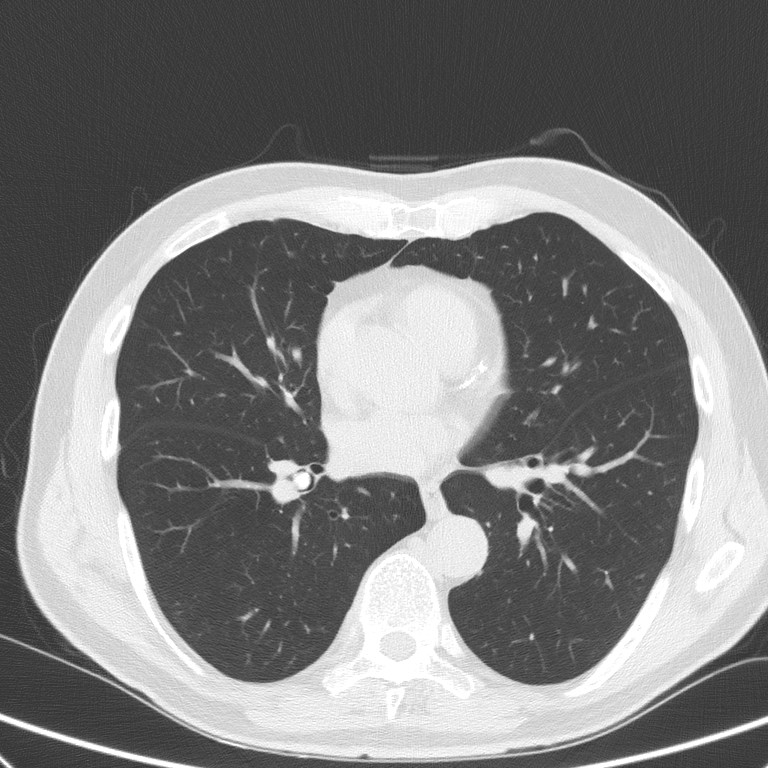
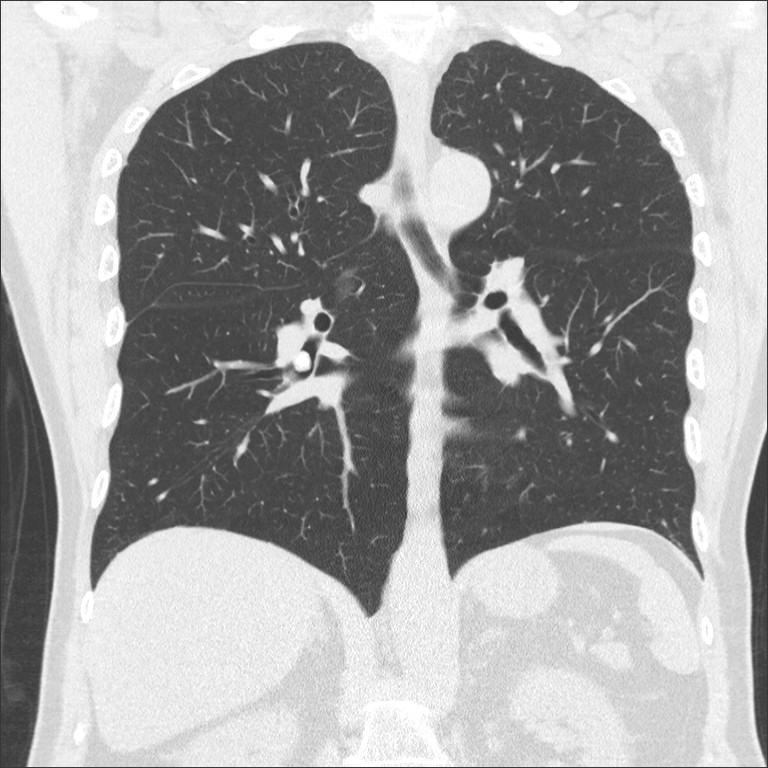
Figure 1 and 2: Chest CT: Lobulated, well-defined endobronchial lesion in the right lower bronchus of the lung and no post-obstructive changes.
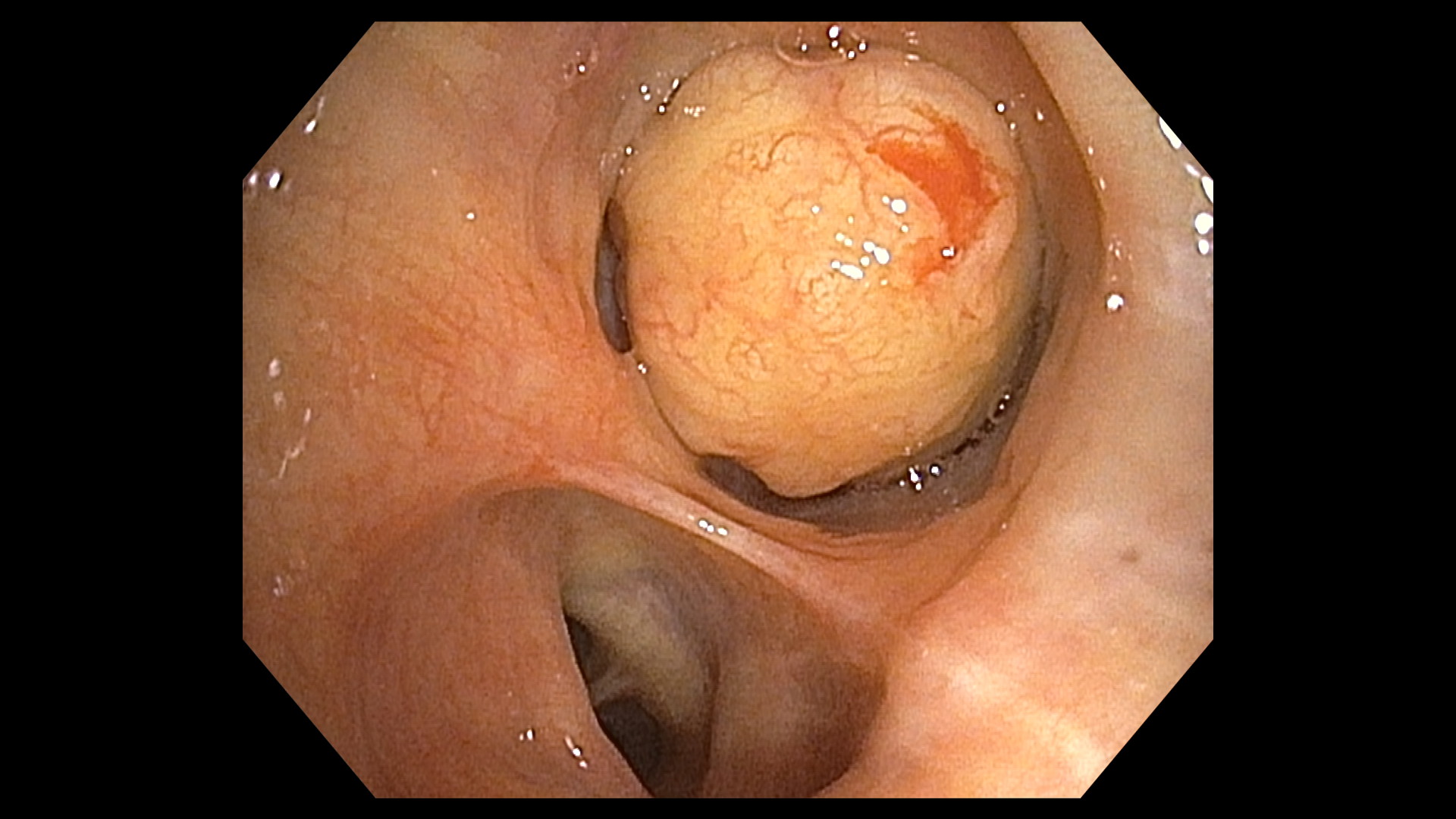
Figure 3: Bronchoscopic images showing a pediculated, round endoluminal tumor with smooth surface growing on the medial wall and almost completely obstructing the right lower bronchus.
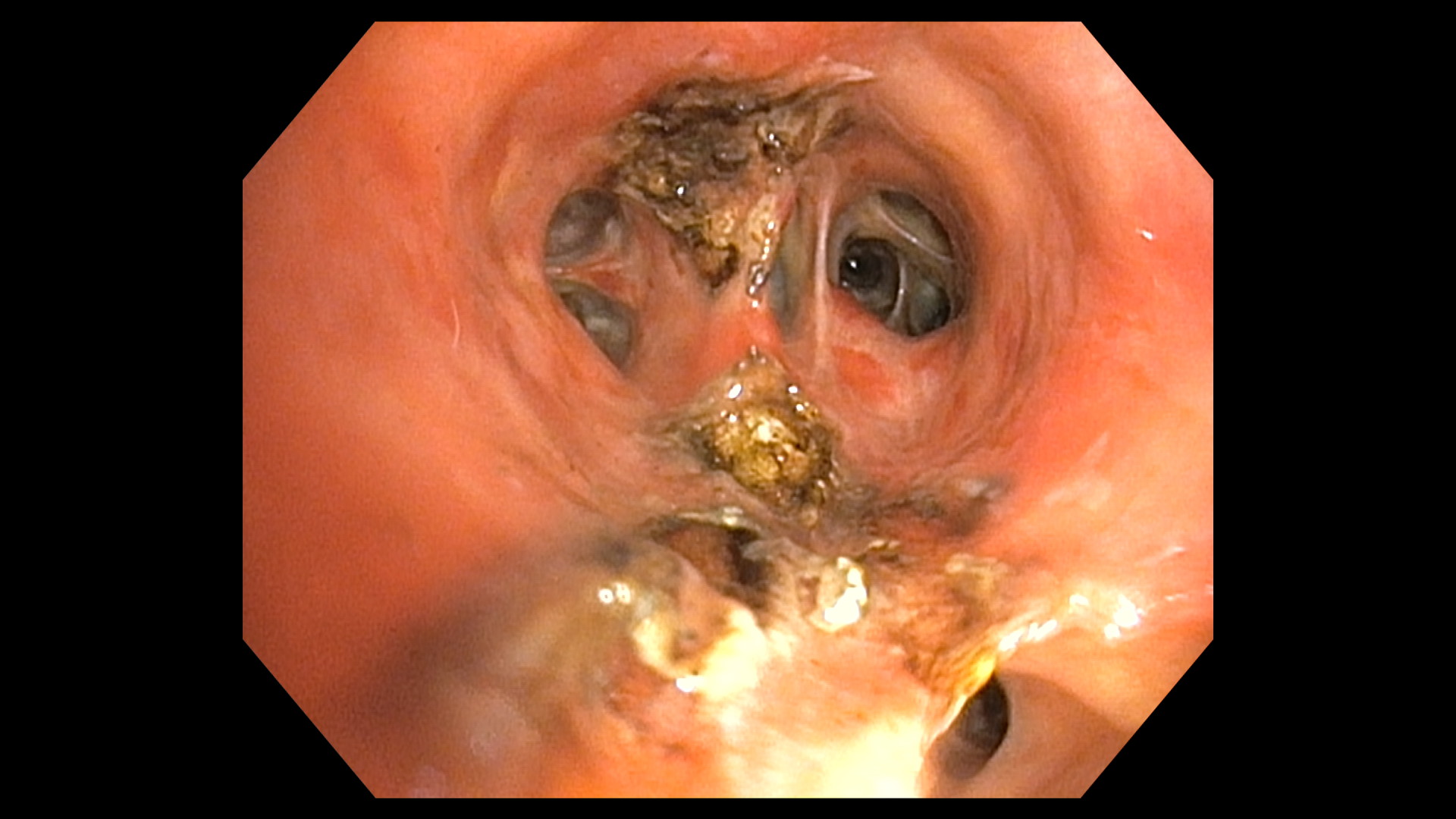
Figure 4: Images of rigid bronchoscopy showing the right lower bronchus after tumor debulking.
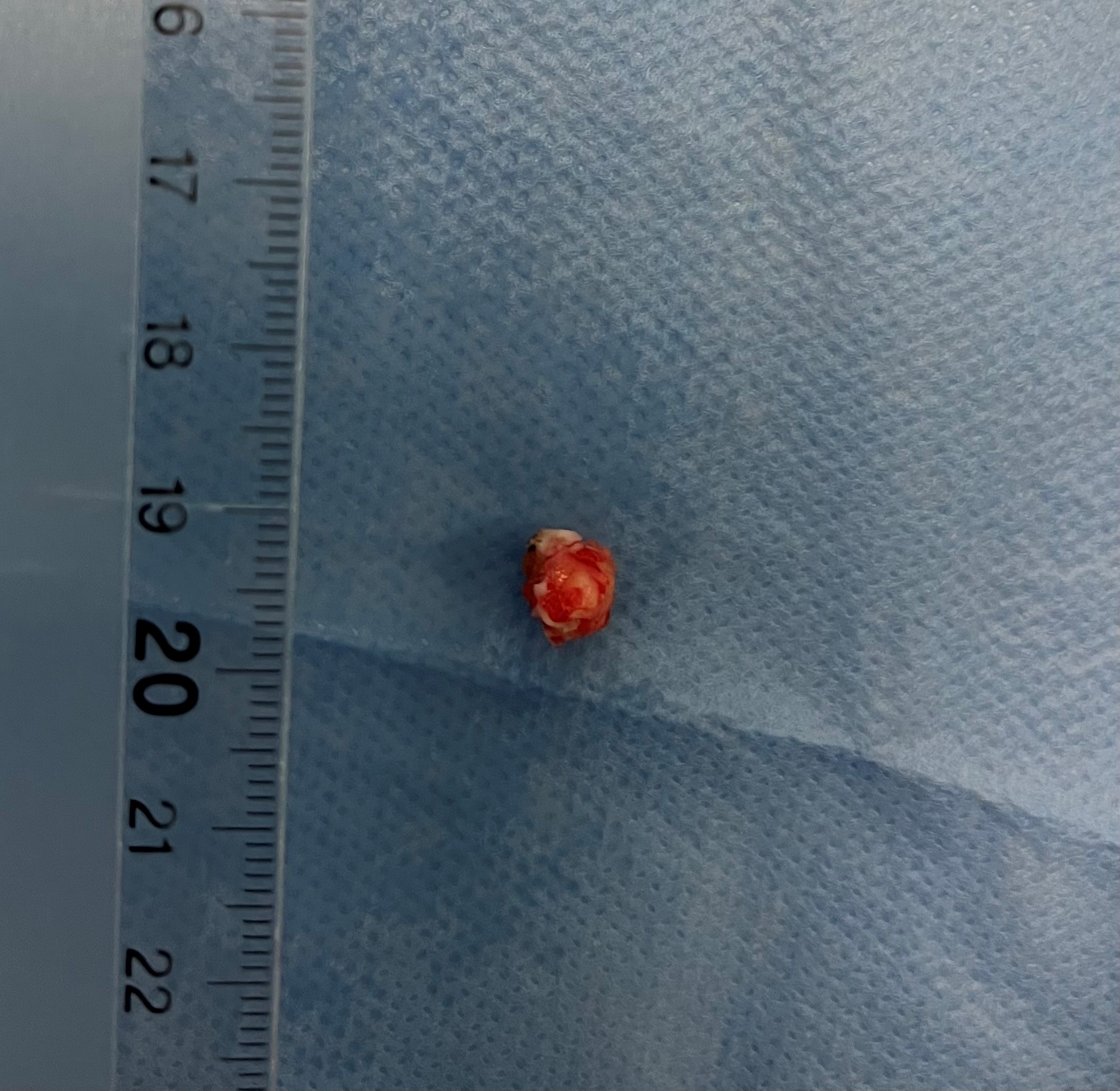
Figure 5: The endobronchial tumor after resection.
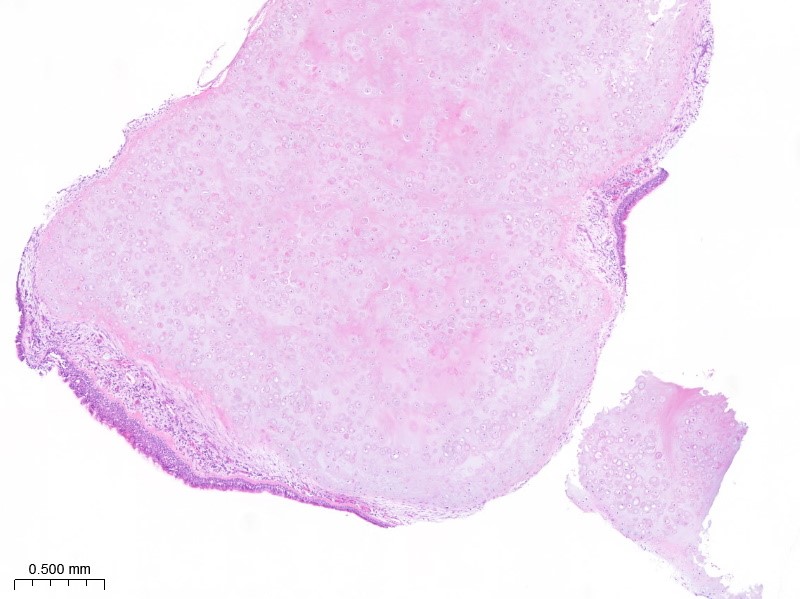
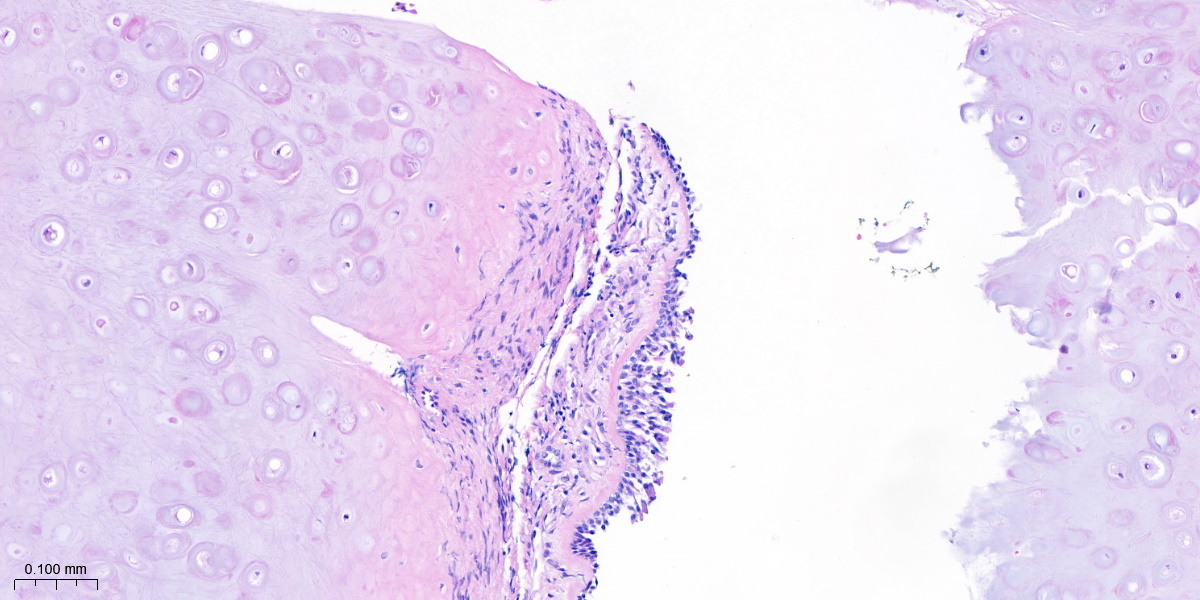
Figure 6 and 7: Pathology section of the mass showing fragments of mature hyaline cartilage partially covered by respiratory epithelium, with no evidence of malignancy.
Discussion
Chondromas are benign tumors originating in chondrocytes. They are most frequently located on the skeleton, but they may also appear in the lungs (intraparenchymal or endobronchial). Benign tumors of the respiratory system such as papillomas, hamartomas, fibromas or chondromas are generally rare (<2% of all airways tumors) with chondromas presenting 0.1 - 0.2% of all masses of the tracheobronchial tree and they usually involve the lung parenchyma [2, 4 – 6]. They may remain asymptomatic or present with non-specific respiratory symptoms like cough, pneumonia, hemoptysis, wheezing or dyspnea [3, 6-11].
Symptoms depend on the localization and size of the tumor.
Computed tomography (CT) is the standard imaging technique for locating pulmonary chondromas [12]. Bronchoscopic findings of chondromas are usually pediculated, vascularised nodules. Histologically, they consist of mature hyaline or mixed-hyaline cartilage [13].
Endobronchial tumors should be resected completely if possible, to prevent complete occlusion with airway obstruction and to provide a histopathological examination for exclusion of malignancy. Pathological differential diagnosis includes hamartoma or chondrosarcoma.
Pulmonary chondromas are also seen as a part of the Carney triad (in addition to gastrointestinal stromal tumors and extra-adrenal paragangliomas) in young adult females [14]. Isolated endobronchial chondromas, as seen in our patient, are particularly rare.
Several management and treatment options of endobronchial chondromas are described in the available literature, such as resection with Neodymium-YAG laser [10], surgical exploration with thoracotomy [3, 6, 9], video-assisted thoracoscopic surgery (VATS), endobronchial cryotherapy or electrocautery snare [8, 15]. An endobronchial treatment should be considered as a first choice, however, according to our knowledge, there are no guidelines regarding treatment recommendations. Management should be tailored individually, according to local resources as well as location and extent of the tumor. Prognosis is excellent for correctly diagnosed patients and complete resection of the tumor. There are no reports of recurrence of chondroma.
We present a case of an endobronchial chondroma that caused recurrent respiratory infections for many years. Because of his occupation as paediatrician, his symptoms were misinterpreted for many years as a natural consequence of close contact with children and exposition to infectious bacteria and viruses and thus were not further investigated. In this case of a 78-years old male patient we conducted an endoscopic resection with complete resection of the tumor. Histological examination was typical for a benign chondroma with no evidence of malignancy. The presence of a Carney triad was considered unlikely; therefore, we did not conduct further tests like positron-emission tomography (PET) scan or gastroscopic examination.
Conclusion
In conclusion, the presence of recurrent bronchial infections should prompt further examination with chest CT scan and eventually bronchoscopy to detect benign endobronchial tumors. Regardless of their benign behaviour, chondromas of the tracheobronchial tree may lead to destruction of lung parenchyma due to bronchial obstruction and subsequent recurrent infections. Symptoms may be misleading. Chest computed tomography and bronchoscopy are well established and recommended diagnostic procedures. Endobronchial resection should be favoured whenever possible.
Disclosures
Authors’ contributions: MP, TS and LK managed the patient and prepared the manuscript. FB prepared the manuscript. MB scientific research supervisor. NVC managed the histologic analysis of the specimens.
Conflicts of interest: None declared.
Acknowledgments: None.
Financial disclosure: None to report.
Consent: Written informed consent was obtained from the patient to publish this case report.
Previous presentation: This case was presented as a poster at a SSP/SSTS Joint Annual Meeting 2024.
References
- Fernandez-Bussy S, Labarca G, Descalzi F, et al. Endobronchial chondromas. Respir Care, 2014; 59(12): e193-e196. doi: 10.4187/respcare.02673.
- Walsh TJ, Healy TM. Chondroma of the bronchus. Thorax, 1969; 24(3): 327-329. doi: 10.1136/thx.24.3.327.
- Papagiannis A, Tsakiridis K, Arikas S, Tzamtzis E, Kyrmanidou E, Zaramboukas T. Endobronchial chondroma: a rare benign bronchial neoplasm. Pneumon, 2010; 23: 172‐175.
- Stevic R, Milenkovic B. Tracheobronchial tumors. J Thorac Dis, 2016; 8(11): 3401-3413. doi: 10.21037/jtd.2016.11.24.
- Shah H, Garbe L, Nussbaum E, Dumon JF, Chiodera PL, Cavaliere S. Benign tumors of the tracheobronchial tree. Endoscopic characteristics and role of laser resection. Chest, 1995; 107(6): 1744-1751. doi: 10.1378/chest.107.6.1744.
- Tian D, Wen H, Zhou Y, Fu M. Pulmonary chondroma: A clinicopathological study of 29 cases and a review of the literature. Mol Clin Oncol, 2016; 5(3): 211-215. doi: 10.3892/mco.2016.945.
- Mahmud T, Nasim Z, Saqib M, Fatima S. Intractable cough due to endobronchial chondroma. Respir Med Case Rep, 2019; 29: 100968. doi: 10.1016/j.rmcr.2019.100968.
- Ryu KM, Myong NH, Kim D. Endobronchial enchondroma: Unusual bronchial tumor. Clin Case Rep, 2022; 10(1): e05292. doi: 10.1002/ccr3.5292.
- Assaad M, El Gharib K, Kassem A, et al. Endobronchial Chondroma: A Rare Case of Benign Tumor with Atypical High Standardized Uptake Value. Cureus, 2022; 14(5): e24800. DOI: 10.7759/cureus.24800.
- Eppinga P, van der Laan KT, Overbeek JJ, Meinesz AF, Postmus PE. Benign endobronchial tumours treated by neodymium-YAG laser. Eur Respir J, 1988; 1(6): 568-570.
- Anrijs S, Weynand B, Pirson F, Rodenstein D, Pieters T. Chondroma: an uncommon case of bronchial tumor. J Bronchology Interv Pulmonol, 2009; 16(4): 270-273. doi: 10.1097/LBR.0b013e3181b64985.
- Wang H, Nie P, Dong C, et al. Computed Tomography Imaging Findings of Pulmonary Chondroma. Biomed Res Int, 2018; 2018: 4387689. doi:10.1155/2018/4387689.
- Bateson EM. Histogenesis of intrapulmonary and endobronchial hamartomas and chondromas (cartilage-containing tumours): a hypothesis. J Pathol, 1970; 101(2): 77-83. doi: 10.1002/path.1711010202.
- Carney JA, Sheps SG, Go VL, Gordon H. The triad of gastric leiomyosarcoma, functioning extra-adrenal paraganglioma and pulmonary chondroma. N Engl J Med, 1977; 296(26): 1517-1518. doi: 10.1056/NEJM197706302962609.
- Teschner M, Gerbatsch KP, Lüllig H. Endobronchiale Chondrome--Bronchoskopische Resektion oder thoraxchirurgische Intervention? [Endobronchial chondroma--bronchoscopic resection or thoracic surgery intervention?]. Pneumologie, 1998; 52(5): 249-253.

