Acute myeloid leukaemia with NPM1 and FLT-3 ITD involving the CSF
van Staden Quintin Andre1,2,* and van Marle Anne-Cecilia1,2
1Department of Hematology and Cell Biology, School of Pathology, Faculty of Health Sciences, University of the Free State, Bloemfontein, South Africa
2Universitas Academic Hospital Laboratory, Department of Hematology and Cell Biology, National Health Laboratory Service, Bloemfontein, South Africa
Received Date: 09/09/2025; Published Date: 26/09/2025
*Corresponding author: Quintin Andre van Staden, Department of Haematology and Cell Biology, School of Pathology, Faculty of Health Sciences, University of the Free State, 205 Nelson Mandela Drive, PO Box 339 (G2), South Africa
A 67-year-old HIV-negative woman presented with confusion. Clinically, she had no splenomegaly, lymphadenopathy, or hepatomegaly. Her initial complete blood count and differential count revealed a leucocytosis of 62.30 x 109/L with macrocytic anaemia (Haemoglobin 58 g/L; MCV 111.1 fL), thrombocytopenia (platelet count 11 x 109/L), and a neutrophil and lymphocyte count of 5.67 x 109/L and 1.50 x 109/L, respectively. Notably, her lactate dehydrogenase (LDH) was markedly increased at 1047 U/L. A peripheral blood smear revealed ±85% blasts. Blasts were medium to large in size, with the majority displaying a nuclear cup morphology and occasional Auer rods (Figure 1A). Flow cytometry of her peripheral blood demonstrated a dim cluster of differentiation (CD) 45 positive blast population with heterogenous myeloperoxidase (MPO) positivity and bright CD33 expression (Figure 1B). No aberrant lymphoid markers and no additional myeloid or monocytic markers were expressed. The same blast population was identified in the cerebrospinal fluid (CSF) (Figure 1c). Molecular work-up confirmed an NPM1 exon 12 insertion (83%) together with an FMS-like tyrosine kinase 3 (FLT3) internal tandem duplication (ITD) (74%).
Although less than 1% of acute myeloid leukaemia presents with central nervous system involvement, when CSF is involved, FLT3-ITD is the most common molecular mutation [1]. In addition to the markedly increased LDH, the co-occurrence of an FLT3-ITD with NPM1 mutation demonstrated in this patient has been shown to further increase the risk of CNS involvement [2].
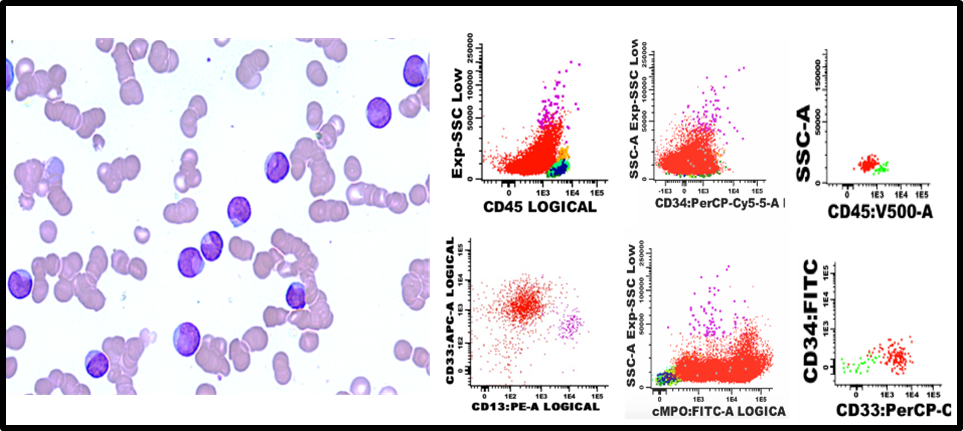
Figure 1: (A) bone marrow aspirate, hematoxylin and eosin stain, 50x objective, original magnification x500; (B) initial acute leukaemia orientation tube (ALOT) and AML panel using the FACSCantoTM II flow cytometer instrument (Becton Dickinson, San Jose, California, USA) and the Infinicyt TM version 2.0 software (Cytognos, Santa Marta de Tormes, Salamanca, Spain) of the peripheral blood; (C) customised antibody panel for cerebrospinal fluid flow cytometry.
All authors approved the submission of this image.
No authors have any financial declaration to make.
Contributorship statement, all authors contributed equally to drafting the manuscript, editing and both gave final approval to submit.
Ethics approval was granted by Health Sciences Research Ethics Committee, reference number: UFS- HSD2025/0293
Funding information: no author was funded to produce this article
References
- Gonzalez-Lugo JD, et al. AML-560 Molecular Features Associated With CNS Disease in Acute Myeloid Leukemia. Clin. Lymphoma Myeloma Leuk, 2024; 24: S321.
- Alakel N, et al. Symptomatic central nervous system involvement in adult patients with acute myeloid leukemia. Cancer Manag. Res, 2017; 9: 97–102.

