Mortality in Neurological Complications Associated with Hematologic Malignancies in Patients Admitted to the Intensive Care Unit
Kenza Damaan*, Amine Abidi, Sabah Benhamza, Mohamed Lazraq, Youssef Miloudi and Abdelhak Bensaid
Intensive care unit, 20 August Hospital 1953, Faculty of Medicine and Pharmacy, Hassan II University of Casablanca, Morocco
Received Date: 10/02/2026; Published Date: 16/04/2026
*Corresponding author: Dr. Kenza Damaan, Intensive Care Unit, 20 August 1953 Hospital, CHU Ibn Rochd, Casablanca, Morocco
Abstract
Background: Central Nervous System (CNS) involvement in hematologic malignancies may result from tumor infiltration or secondary complications. These events are serious and often require Intensive Care Unit (ICU) admission.
Objective: To describe the epidemiological, clinical, radiological, and outcome profiles of patients admitted to the ICU for neurological complications of hematologic malignancies and to identify prognostic factors.
Methods: We conducted a retrospective study in the ICU of the 20 Août Hospital in Casablanca from January 2017 to December 2020. Patients with hematologic malignancies presenting with central neurological involvement, seizures, or altered consciousness were included. Data were collected from medical records and analyzed using Excel and SPSS.
Results: Among 1,274 ICU admissions, 36 patients (2.8%) had neurological complications related to hematologic malignancies. The mean age was 40 years, with male predominance. Acute myeloid leukemia was the most frequent diagnosis. Most patients were admitted for altered consciousness. Brain CT was normal in 44.4% of cases. The main abnormalities were intraparenchymal hematoma and subarachnoid hemorrhage. Mortality was 86%, mainly due to septic shock. Poor prognostic factors included status epilepticus, coma, bone marrow aplasia, hyperleukocytosis, renal failure, and acute leukemia.
Conclusion: Neurological complications in hematologic malignancies are associated with very high ICU mortality. Prognosis mainly depends on sepsis and organ failure. Early ICU admission may improve outcomes.
Keywords: Hematologic malignancies; Central nervous system involvement; Neurological complications; Intensive care unit; Acute leukemia; Status epilepticus; Septic shock; Prognostic factors; Mortality
Introduction
Central nervous system involvement in hematologic malignancies may be related to infiltration of the central nervous system by the tumor process. This most often involves aggressive non-Hodgkin lymphomas, and less frequently low-grade lymphoproliferative disorders or other types of hematologic malignancies (acute myeloid leukemias, multiple myeloma, Hodgkin lymphomas). Other causes of nervous system involvement in these conditions include infectious, vascular, paraneoplastic, immune-mediated, metabolic, or toxic etiologies. Early identification of neurological symptoms allows for prompt etiological investigation and appropriate diagnostic orientation, leading to timely and adapted treatment [1].
Study objective:
This study aims to investigate this specific clinical situation by analyzing the epidemiological, diagnostic, therapeutic, and outcome profiles of patients admitted to the intensive care unit for neurological complications related to hematologic malignancies. It also seeks to assess prognostic factors and to determine the incidence of mortality attributable to neurological involvement within our intensive care unit.
Patients and Methods
This was a retrospective descriptive and analytical study conducted in the intensive care unit of the 20 Août Hospital in Casablanca over a 4-year period, from January 1, 2017 to December 31, 2020.
Patients included in the study were those followed for a hematologic malignancy and presenting with:
- Central neurological involvement documented by brain Computed Tomography (CT) or magnetic resonance imaging (MRI);
- Seizures or status epilepticus;
- Altered level of consciousness.
Patients with peripheral neurological involvement and those with incomplete or non-exploitable medical records were excluded.
Data collection was carried out using a standardized data collection form completed from medical records, in compliance with general ethical principles regarding confidentiality and patient data protection. Data analysis was performed using Microsoft Office Excel and SPSS software.
Results
During the study period, 1,274 patients were admitted to the intensive care unit of the 20 Août Hospital. Among them, 36 patients were admitted due to a central neurological complication of their hematologic malignancy, corresponding to an overall incidence of 2.8%. It should be noted that 100% of hematology patients admitted to the ICU presented with neurological failure.
The mean age of our patients was 40 years, with a range from 15 to 79 years. The male-to-female sex ratio was 1.66.
Seven patients (19.4%) had acute myeloid leukemia, six patients (16.67%) had acute lymphoblastic leukemia, five patients (13.89%) had non-Hodgkin lymphoma, five patients (13.89%) had multiple myeloma, two patients (5.56%) had myelodysplasia, one patient (2.78%) had primary central nervous system lymphoma, one patient (2.78%) had Hodgkin lymphoma, and one patient (2.78%) had Burkitt lymphoma. Eight patients (22.22%) were in bone marrow aplasia.
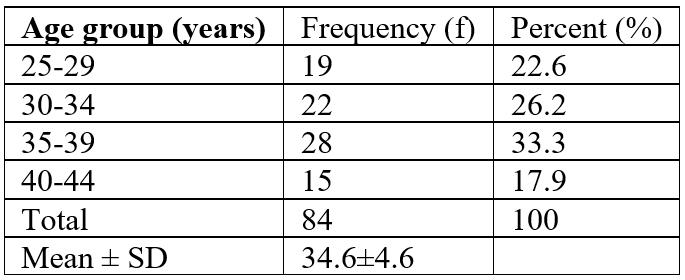
58% of the patients were receiving chemotherapy, including 14 patients in the induction phase and 3 in the consolidation phase.
The reasons for hospital admission were distributed as follows:
14 patients (38.89%) were admitted for afebrile impaired consciousness, 14 patients (38.89%) for febrile impaired consciousness, 5 patients (13.89%) presented with status epilepticus, and 3 patients (8.33%) presented with hemiplegia.
Brain CT performed at admission after patient stabilization revealed the following abnormalities:
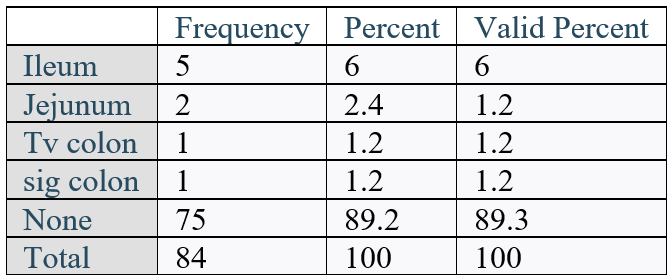
Note: The total percentage exceeds 100% because each patient may have presented with more than one abnormality simultaneously.
Patient outcomes:
Mortality was estimated at 86%, with 31 patients dying. Septic shock was the leading cause of death, accounting for 43% of cases. The mean length of hospital stay was 4.5 days, with a range from 1 to 13 days.
The prognostic factors identified in the multivariate analysis were: male sex (p = 0.036), status epilepticus (p = 0.0001), impaired consciousness (p = 0.003), bone marrow aplasia (p = 0.008), acute myeloid leukemia (p = 0.001), multiple myeloma (p = 0.001), hyperleukocytosis (p = 0.0001), renal failure (p = 0.029), and coma (p = 0.001).
Discussion
Mortality among hematology patients has markedly decreased over the past decade. In a recent multicenter prospective study, mortality was 27% in these patients [2]. However, when septic shock is involved, the mortality rate is higher, reaching nearly 65% [3]. In our study, mortality was also high, mainly due to septic shock as the primary cause.
A large number of clinical and biological factors are recognized for their prognostic value in malignant hematological diseases [4]. The accumulation of these factors increases mortality.
Subarachnoid and intraparenchymal hemorrhages have a poorer prognosis than subdural hematomas. Patients over 60 years of age had a better prognosis, partly explained by the higher frequency of subdural hematomas in this group [5].
Central nervous system relapse of leukemia is associated with a poor prognosis [6]. Several factors increase the risk of death in leukemia, particularly acute lymphoblastic leukemia, including age, which remains the most important factor. Patients over 60 years of age have a lower chance of survival [7]. In contrast, patient sex has no influence on prognosis in most studies [8]. Hyperleukocytosis is not only a risk factor for CNS involvement but also a determinant of patient prognosis [9].
Predictors of mortality in recent studies were mainly related to the severity of organ failure, as reflected by the need for mechanical ventilation and vasopressors.
An article published by E. Azoulay et al. in 2015 reported that factors previously associated with mortality in hematology patients after ICU admission are no longer relevant, including neutropenia, stem cell transplantation, type of hematological malignancy, disease stage, and the need for transfusion [10]. Nevertheless, early initiation of treatment remains a key prognostic factor [11].
Conclusion
Neurological involvement in hematology patients is an increasingly frequent complication and often requires admission to an intensive care unit. The aggressiveness and toxicity of treatments, as well as improved survival among patients followed in hematology, contribute to this trend. Prognosis in the ICU mainly depends on the presence of multiple organ failures and their association with sepsis. Consequently, early admission of these patients before the onset of multiorgan failure appears to be associated with a better prognosis.
References
- Complications neurologiques centrales dans les hémopathies malignes ; Revue Neurologique, 2019; 175(Supplement 1): Page S156.
- Saillard C, Sannini A, Chow-Chine L, et al. Prise en charge de la neutropénie fébrile chez le patient d’onco-hématologie admis en réanimation ; Bulletin du Caner, 2015; 102(4): Pages 349-359.
- Vargas F, Gruson D. Prise en charge du choc septique chez les patients d’onco-hématologie, 2007.
- Kaid Salim K. Thèse intitulée: Leucémie aigue Lymphoblastique de l’adulte avec envahissement du système nerveux central, 2011.
- Chen CY, Tai CH, Tsay W, Chen PY, Tien HF. Prediction of fatal intracranial hemorrhage in patients with acute myeloide leukemia. Ann Oncol, 2009; 20(6): 1100-1104.
- Azarm T, Jahani M, Amini A Gh, Saghfi MR. Central Nervous System Relapse in Acute Lymphoblastic Leukemia (Study on 160 cases), 2004.
- Rowe JM, Buck G, Burnett AK, et al. induction therapy for adults with acute lymphoblastic leukemia: results of more than 1500 patients from the international ALL trial: MRC UKALLXII/ECOG E2993. Blood, 2005; 106(12): 3760-3767.
- Plasschaert S, Kamps W, Vellenga E, et al. Prognosis in childhood and adult acute lymphoblastic leukaemia: a question of maturation? Cancer treatment reviews, 2004; 30: 37-51.
- Gokbuget N, Hoelzer D. Treatment of Adult Acute Lymphoblastic Leukemia. Hematology, 2006: 133-141.
- Azoulay E, Pène F, Darmon M, et al. Managing critically ill hematology patients: Time to think differently, Blood Reviews, 2015; 29(6): Pages 359-367.
- Tattevin P, Revest M, Lavoué A. Méningites et méningoencéphalites aseptiques. Division of infectious Diseases, San Francisco General Hospital, university of California, 2008.

