Bowel Perforation Following Diagnostic Laparoscopy: A Two-Year Review from Two Referral Hospitals in North Central Nigeria
Solomon D Peter¹,*, Christopher O Egbodo², Kenneth N Ozoilo¹, Andrew H Shitta¹, Femi Ale¹, Mercy W Isichei¹ and Micheal A Misauno¹
¹Department of Surgery, Jos University Teaching Hospital, Jos, Nigeria
²Department of Obstetrics and Gynecology, Jos University Teaching Hospital, Jos, Nigeria
Received Date: 09/02/2026; Published Date: 13/04/2026
*Corresponding author: Solomon D Peter, Department of Surgery, Jos University Teaching Hospital, Jos, Nigeria
Abstract
Background: Diagnostic laparoscopy is increasingly being used for evaluating abdominal pain and fertility related complaints, with its attendant complications.
Method: A prospective study of patients who had diagnostic laparoscopy from January, 2024, to December, 2025 in two referral hospitals in Jos. Patients’ entries were entered into a database and analyzed using the IBM SPSS 25.
Result: All the patients are females with a mean age of 34.6±4.6. Nine patients (10.7%) had bowel perforation, out of a total of 84 diagnostic laparoscopies, ileum being the most perforated (55.6% of the perforations). Thirty-four (40.5%) patients had previous abdominal surgeries, appendectomy being the highest. Tachycardia is the most consistent clinical indicator of the perforations p val of 0.0001. All the perforations were repaired via laparotomy with 0 mortality.
Conclusion: Previous abdominal surgery markedly increases risk of bowel perforation during diagnostic laparoscopy, and tachycardia is the most consistent clinical feature of peritonitis following the perforation. A combined collaboration between Gynecologists and General Surgeons is important for timely and proper decisions to be made. Early recognition of bowel injury is crucial for a favorable clinical outcome. Laparotomy and two layered closure of the perforation is a safe and reliable treatment.
Keywords: Laparoscopy; Bowel perforation; Peritonitis; Laparotomy
Introduction
Diagnostic laparoscopy is a minimally invasive intervention essentially to look into the peritoneal cavity in an effort to identify a specific problem [1,2]. It is increasingly becoming a common armamentarium for evaluating abdominal pain and masses, and infertility especially in General surgery and Gynecological practices [3-5]. Despite its importance and relevance, the procedure carries inherent risk including bowel injury and perforation [6-9].
Bowel injury is a serious complication of gynecological laparoscopy and it is considered to be the most feared complication of laparoscopy generally, because of the resultant sepsis and mortality that may occur [10]. The incidence of the injury depends on the pathology being evaluated, and the type of procedure which may be diagnostic, the focus of this research; minor operative; or complex operative in nature [12,13].
In order to mitigate complications including perforation, certain conditions or situations are considered as contraindications to laparoscopy in general, including diagnostic. The patient limitations to laparoscopic surgery can be both anatomic and physiologic. Adverse anatomic considerations include difficult access to the abdomen, obliteration of the peritoneal space, organomegaly, intestinal distension, and the potential for dissemination or recurrence of cancer. The major physiologic obstacles to safe laparoscopy include pregnancy, increased intracranial pressure, abnormalities of cardiac output and gas exchange in the lung, and chronic liver disease and coagulopathy. While many of these conditions were formerly considered absolute contraindications to laparoscopy, they are now considered, by many surgeons, to be only relative contraindications [14]. Previous abdominal surgery is also considered as a relative contraindication for laparoscopy. However, increasing expertise and better equipment has progressively shrunken this relativity, hence a number of patients still undergo diagnostic laparoscopy safely, despite previous abdominal surgical procedures [14-16].
Against this back ground, we review the patients who had diagnostic laparoscopy, bowel perforation and eventual laparotomy in two referral hospitals in North Central Nigeria.
Patients, Materials and Method
This is a prospective hospital-based study carried out in Jos University Teaching Hospital, Jos, Plateau State, Nigeria, a 526-bed hospital offering tertiary health care, and Fertile Ground Specialist Hospital, a minimal access and fertility hospital that renders laparoscopic, general surgery and all gynecological services. These facilities receive patients from at least 6 neighboring states of Nasarawa, Kaduna, Taraba, Adamawa, Bauchi, Gombe and Plateau states, and the Federal Capital Territory. The patients present to these study locations because of availability and expertise equipment, and Specialist for laparoscopic, gynecological and general surgery services.
Both laparoscopy and laparotomy when needed were done by Consultant Gynecologist and General Surgeon respectively, and occasionally together. All the patients that met indication for laparoscopy had basic laboratory investigations including HIV and viral hepatitis screening. Single port laparoscopy was done through the umbilical cicatrix.
In performing the laparoscopy, 2 Allis forceps were applied on either sides of umbilical crease to evert the inferior crease of the umbilicus; via 2mm skin deep stab wound on the inferior crease ,a confirm to be patent and spring actionable veress needle is inserted pointing towards the pelvis while elevating the anterior abdominal wall; needle is removed, saline filled syringe is used to aspirate, irrigate and aspirate again before a hanging-drop test is done to confirm correct placement in the peritoneal cavity; an insufflator is connected and inflated initially to 200ml, 500ml and finally between 2-6 liters; close monitoring of both quadromanomatic and multi-parameter monitors were observed. Following adequate insufflations, skin incision is enlarged using a mosquito forceps up to rectus sheath; while elevating anterior abdominal wall, a 10mm trocar cannula is introduce, removed and a 10mm telescope is inserted; peritoneal cavity is explored for any pathology; dye is introduced through the cervical os while observing for spillage/patency of the Fallopian tubes.
All patients requiring laparotomy were resuscitated with intravenous Normal saline until they were making clear and adequate urine, and a pulse rate is noted to be within normal limit or returning to normal range. Laparotomy was performed via mid line route, irrespective of previous abdominal surgeries. Formal explorations were performed to identify perforation(s), and separate any offending adhesion. Identified gut perforations were repaired in two layers using vicryl 0 and 2/0. Abdominal cavity is copiously lavage with normal saline and peritoneal drains inserted. Rectus sheath is closed with Nylon 2, and skin apposed with interrupted Nylon 2/0. Patients that required secondary skin suturing had it with interrupted Nylon 2/0 after resolution of surgical site infection.
Diagnosis of bowel perforation was made based on intra-laparoscopic findings, features of peritonitis afterwards, and laparotomy findings of the perforations.
Information extracted from the patients’ medical records included age, sex, previous abdominal surgeries, vital signs, duration of peritonitis, gut perforated, complications, and outcome were transferred into Excel spread sheet and analyzed using SPSS version 25. Results are presented in tables, with frequencies and percentages, means and charts.
Ethical clearance was obtained for this study.
Results
The age distribution is as shown in Table 1, with mean age of 34.6±4.6 years, and 59.5% between the ages of 30-39 years, accounting for the highest proportion. All the patients are females.
The indications for the laparoscopy were either abdominal pain, or fertility related evaluation as shown in Figure 1. Nine (9) patients had bowel perforation, out of a total of 84 diagnostic laparoscopies over the 2-year period (Table 2). This indicates an average of 4.5 patients per year with traumatic bowel perforation from diagnostic laparoscopy, and a perforation rate of 10.7%. Forty-two patients representing 50% of the total had previous abdominal surgery as shown in Table 3, with appendectomy being the commonest surgery.
Table 4 shows difference in Mean of physiological variables (pulse rate, respiratory rate, temperature and systolic and diastolic blood pressures) between perforated and non-perforated patients, and duration of hospital stay. Patients with perforation had a markedly higher mean pulse rate (105.33 ± 20.98 beats/min) compared to non-perforated patients (75.47 ± 7.57 beats/min). This difference was statistically significant (t = 8.706, p = 0.0001). All the patients without complication stayed less than a day in the hospital as also shown in Figure 2. Table 5 shows the relationship between previous abdominal surgeries and development of complications.
Table 6 shows complications following laparotomy, with surgical site infection being the commonest, having 6 patients (7.1%). There was no mortality.
Table 1: Age Distribution.
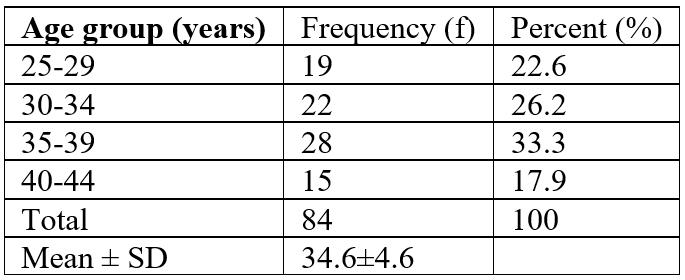
Table 2: Bowel perforated.
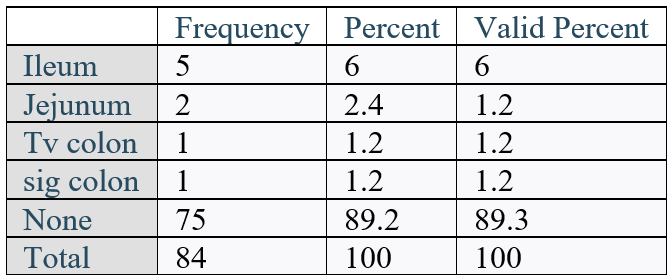
Table 3: Previous abdominal surgery.
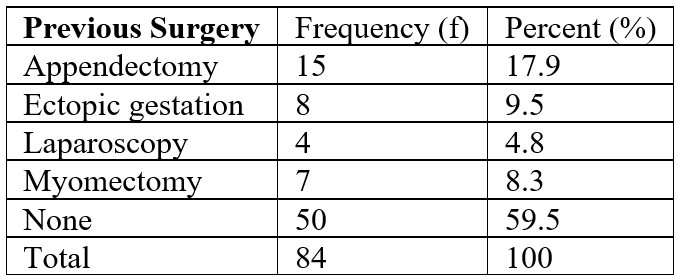

Table 4: Difference in Mean of physiological variables between perforated and Non-perforated, and duration of hospital stay.
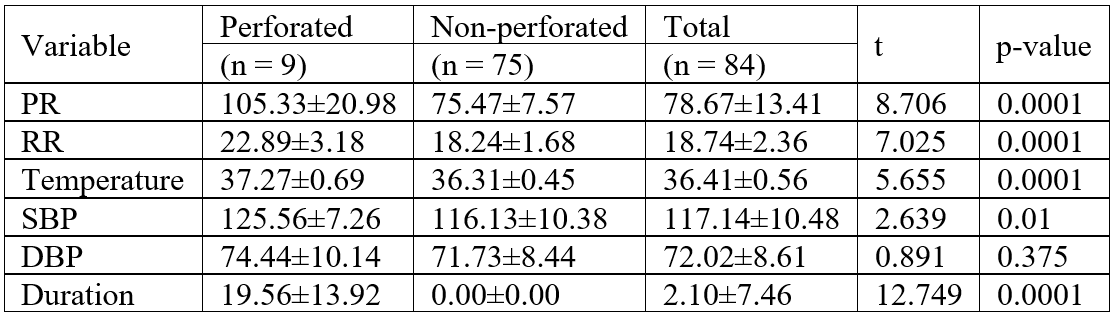
Table 5: Relationship between previous abdominal surgery and complication.
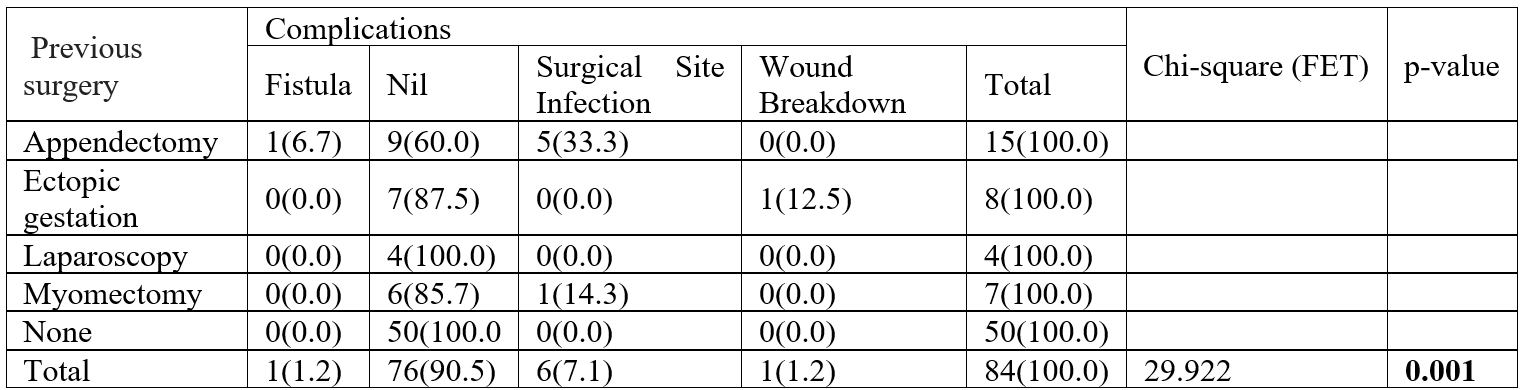
FET = Fisher’s Exact Test
NB: Relationship is statistically significant at p < 0.05
Table 6: Complications post laparotomy.
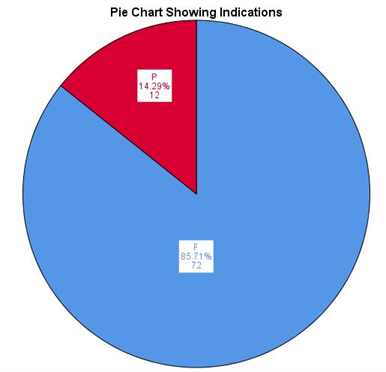
Figure 1: Chart showing indication for laparoscopy.
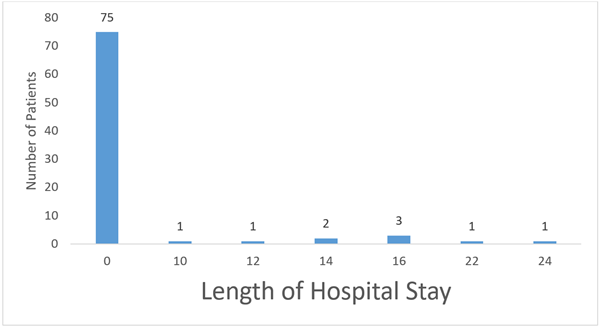
Figure 2: Duration of Hospital Stay.
Discussion
As seen in Table 1, the Mean age of patients in this study is 34.6± 4.6 years. This is not unexpected as the most common indication for diagnostic laparoscopy in this study is fertility related as shown in Figure 1. All the patients in the study are females because diagnostic laparoscopy has become an important tool in evaluating infertility in women [4-6].
The perforation rate in this study was 10.7%, significantly much higher than the average perforation rate of 0.39% to 2.4% in general laparoscopy [8,11,18,19]. This can be explained by the fact that all the patients that had the perforations had previous abdominal surgery as shown in Table 3. Previous abdominal surgeries significantly increase chances of adhesion formation and therefore risk of bowel injuries during laparoscopy [7,8]. This was confirmed by findings of the adhesion at both laparoscopy and during laparotomy in those that eventually had laparotomy. Adhesion was seen in all the patients that had laparotomy, irrespective of the previous surgery they had as shown in Table3. Previous abdominal surgeries should therefore be a stronger or more stringent contraindication to laparoscopy, rather than being a relative one.
All perforations seemed to have occurred during initial trocar placement. This is similar to findings from most other results [8,9]. Hence there is need for greater caution when performing laparoscopy with both the open technique and using the Veress needle.
Only one of the nine bowel perforations was recognized during the laparoscopy, representing 11.1% of the perforations. This is in keeping with most other findings [21,23]. In this instance, the procedure was converted to laparotomy because of noticed adhesion and the perforation.
As expected, patient that had bowel perforation from the laparoscopy developed clinical features of peritonitis, including generalize abdominal pain, ileus and abdominal distension, and fever. However, the most consistent clinical feature of peritonitis in our study is tachycardia as shown in Table 4. Patients with perforation had a markedly higher mean pulse rate (105.33 ± 20.98 beats/min) compared to non-perforated patients (75.47 ± 7.57 beats/min). This difference was statistically significant (t = 8.706, p = 0.0001). As such we recommend that any patient with tachycardia during or immediately after laparoscopy should be promptly evaluated for bowel perforation.
Commonest complication noted following laparotomy was surgical site infection as shown in Table 6. This is not unexpected, as bowel perforation changes a diagnostic laparoscopic procedure classed as clean, to a dirty wound, with a higher infection rate [24].
Patients that sustained perforations and therefore laparotomy, had longer duration of hospital stay, an average of 16 days as shown in Figure 2. A patient that developed fistula stayed for 24 days. The longer duration of stay reaffirms some of the advantages of laparoscopy over open surgeries or laparotomy, and complications increase morbidity [25,26].
There was no mortality from our study despite the fact that bowel perforation is usually fraught with a high mortality [28,29]. This is mainly because of the relatively early recognition of the perforation in this study, prompt and adequate resuscitation where necessary, and effective repair of the perforation.
Conclusion
Previous abdominal surgery markedly increases risk of perforation during diagnostic laparoscopy, and tachycardia is the most consistent clinical feature of peritonitis following the perforation. A combined collaboration between Gynecologists and General Surgeons is important for timely and proper decisions to be made. Early recognition of bowel perforation is crucial for a favorable clinical outcome. Laparotomy and two layered closure of the perforation is a safe and reliable treatment.
Conflict of interest: None
Grant support: None
This work was carried out in collaboration between all authors.
References
- Monnet E, Twedt DC. Laparoscopy. Veterinary Clinics: Small Animal Practice, 2003; 33(5): 1147-1163.
- Nagy AG, James D. Diagnostic laparoscopy. The American journal of surgery, 1989; 157(5): 490-493.
- Weickert U, Jakobs R, Riemann JF. Diagnostic laparoscopy. Endoscopy, 2005; 37(1): 33-37.
- Bosteels J, Van Herendael B, Weyers S, D'Hooghe T. The position of diagnostic laparoscopy in current fertility practice. Human reproduction update, 2007; 13(5): 477-485.
- Rau B, Hünerbein M. Diagnostic laparoscopy: indications and benefits. Langenbeck's Archives of Surgery, 2005; 390(3): 187-196.
- Togni R, Benetti-Pinto CL, Yela DA. The role of diagnostic laparoscopy in gynecology. Sao Paulo Medical Journal, 2015; 134(1): 70-73.
- Loffer FD, Pent D. Indications, contraindications and complications of laparoscopy. Obstetrical & gynecological survey, 1975; 30(7): 407-427.
- van der Voort M, Heijnsdijk EA, Gouma DJ. Bowel injury as a complication of laparoscopy. Journal of British Surgery, 2004; 91(10): 1253-1258.
- Llarena NC, Shah AB, Milad MP. Bowel injury in gynecologic laparoscopy: a systematic review. Obstetrics & Gynecology, 2015; 125(6): 1407-1417.
- Elbiss HM, Abu-Zidan FM. Bowel injury following gynecological laparoscopic surgery. African Health Sciences, 2017; 17(4): 1237-1245.
- Shirk GJ, Johns A, Redwine DB. Complications of laparoscopic surgery: how to avoid them and how to repair them. Journal of Minimally Invasive Gynecology, 2006; 13(4): 352-359.
- Chapron C, Querleu D, Bruhat MA, Madelenat P, Fernandez H, Pierre F, et al. Surgical complications of diagnostic and operative gynaecological laparoscopy: a series of 29,966 cases. Human reproduction (Oxford, England), 1998; 13(4): 867-872.
- Miranda CS, Carvajal AR. Complications of operative gynecological laparoscopy. JSLS: Journal of the Society of Laparoendoscopic Surgeons, 2003; 7(1): 53.
- Bowers SP, Hunter JG. Contraindications to laparoscopy. In the SAGES manual: perioperative care in minimally invasive surgery. New York, NY: Springer New York.jh, 2006; pp. 25-32.
- Grace L, Soliemannjad R. Bowel injury in gynecologic laparoscopy: a systematic review. Obstetrics & Gynecology, 2015; 126(6): 1306.
- Van Goethem B, Katic N. Laparoscopic Contraindications, Complications, and Conversion. Small Animal Laparoscopy and Thoracoscopy, 2022: 106-122.
- Buote NJ, McClaran JK. Laparoscopic contraindications, complications, and conversion. Small animal laparoscopy and thoracoscopy, 2015; 93-102.
- Onders RP, Mittendorf EA. Utility of laparoscopy in chronic abdominal pain. Surgery, 2003; 134(4): 549-552.
- Pitt T, Brethauer S, Sherman V, Udomsawaengsup S, Metz M, Chikunguwo S, et al. Diagnostic laparoscopy for chronic abdominal pain after gastric bypass. Surgery for Obesity and Related Diseases, 2008; 4(3): 394-398.
- De Groen PC, Rakela J, Christopher Moore S, McGill DB, Burton DD, Ott BJ, et al. Diagnostic laparoscopy in gastroenterology: a 14-year experience. Digestive diseases and sciences, 1987; 32(7): 677-681.
- Schrenk P, Rieger R, Shamiyeh A, Wayand W. Diagnostic laparoscopy through the right lower abdominal incision following open appendectomy. Surgical endoscopy, 1999; 13(2): 133-135.
- Grant HW, Parker MC, Wilson MS, Menzies D, Sunderland G, Thompson JN, et al. Adhesions after abdominal surgery in children. Journal of pediatric surgery, 2008; 43(1): 152-157.
- Bishoff JT, Allaf ME, Kirkels WI, Moore RG, Kavoussi LR, Schroder F. Laparoscopic bowel injury: incidence and clinical presentation. The Journal of urology, 1999; 161(3): 887-890.
- Mohil R. Classification of wounds. Principles and practice of wound care, 2012; 1: 42-52.
- Devaney L, Rowell KS. Improving surgical wound classification—why it matters. AORN journal, 2004; 80(2): 208-223.
- Garry R. Laparoscopic surgery. Best Practice & Research Clinical Obstetrics & Gynaecology, 2006; 20(1): 89-104.
- Milingos S, Kallipolitis G, Loutradis D, Liapi A, Mavrommatis K, Drakakis P, et al. Adhesions: laparoscopic surgery versus laparotomy. Annals of the New York Academy of Sciences, 2000; 900(1): 272-285.
- Ahuja A, Pal R. Prognostic scoring indicator in evaluation of clinical outcome in intestinal perforations. Journal of Clinical and Diagnostic Research: JCDR, 2013; 7(9): 1953.
- Onken F, Senne M, Königsrainer A, Wichmann D. Classification and treatment algorithm of small bowel perforations based on a ten-year retrospective analysis. Journal of Clinical Medicine, 2022; 11(19): 5748.

