Large Retroperitoneal Liposarcoma: About a Case
Anas Tmiri*, Oussama Bjane, Mehdi Bennani, Yassine Daghdagh, Adil Kbirou, Amine Moataz, Mohamed Dakir, Adil Debbagh and Rachid Aboutaieb
Department of Urology, University hospital center Ibn Rochd, Casablanca, Morocco
Faculty of Medicine and Pharmacy, Hassan II University, Casablanca, Morocco
Received Date: 07/02/2026; Published Date: 02/04/2026
*Corresponding author: Anas Tmiri, Department of Urology, University hospital center Ibn Rochd, Casablanca, Morocco; Faculty of Medicine and Pharmacy, Hassan II University, Casablanca, Morocco
Abstract
Retroperitoneal liposarcomas are rare malignant tumors with insidious symptoms. Diagnosis rest essentially on tomodensitometry, with histological confirmation being necessary. The treatment of choice is wide surgical excision.
We report a case of a large retroperitoneal sarcoma operated via a thoraco-phreno-abdominal approach.
Keywords : Sarcoma; Retroperitoneal liposarcoma; Excision surgery; Retroperitoneal malignant tumor; Open surgery; Undifferentiated liposarcoma
Introduction
Retroperitoneal liposarcoma is a rare malignant soft tissue tumor that develops in the retroperitoneum. It is generally unique and consists of a single histological type. Tomodensitometry and abdominal magnetic resonance imaging allow for an accurate diagnosis. Surgical resection as wide as possible is the only therapeutic option [1,2].
We describe a case of a large retroperitoneal sarcoma in a 74-year-old woman operated by thoraco-phreno-abdominal laparotomy.
Case Report
A 74-year-old female patient being treated for hypertension with amlodipine, with the history of an incidental discovery of an abdominal mass by a general practitioner without abdominal pain or associated digestive disorder, without other accompanying signs, all evolving in a context of apyrexia and preservation of general condition.
The clinical examination noted a patient in good general condition with palpation of a large mass in the left flank, left hypochondrium and epigastric region, making contact with the left lumbar region, the rest of the clinical examination was unremarkable.
The abdominopelvic CT scan revealed a large left retroperitoneal mass measuring 16.4cm*25.8cm*29.5cm. Posteriorly, it comes into contact with the infrarenal abdominal aorta with a visible line of separation. It comes into contact with the left common iliac vessels inferiorly with loss of a visible line of separation. Superiorly, it comes into contact with the splenic artery with loss of a visible line of separation. It displaces the left kidney superiorly and anteriorly. Further superiorly, it comes into contact with the duodenal-jejunal junction and the proximal jejunal loops with persistence of a visible line of separation. Superiorly, it displaces the tail and body of the pancreas with loss of a visible line of separation. It comes into contact with the inferior pole of the spleen with loss of a visible line of separation. Anteriorly, it displaces the transverse colon (Figure 1).
A biopsy was performed which suggested a dedifferentiated liposarcoma.
The patient underwent surgery following the decision of the multidisciplinary consultation staff by open surgery via a thoraco-phreno-abdominal approach with simple post-op follow-up, the result of the anatomopathological examination was in favor of a dedifferentiated liposarcoma with clear margins (R0) (Figure 2).
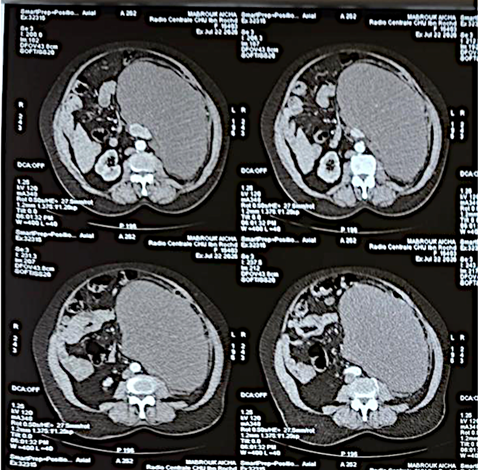
Figure 1: Abdomino-pelvic scan revealed a large left retroperitoneal mass measuring 16.4cm*25.8cm*29.5cm.
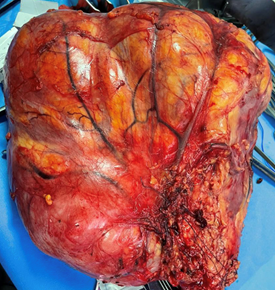
Figure 2: Surgical compartmental excision surgery of liposarcoma.
Discussion
Sarcomas are rare, primary mesenchymal tumors representing less than 1% of all malignant tumors. 10% to 15% are located in the retroperitoneum and are dominated by liposarcoma, which represents approximately 40 to 50% of retroperitoneal sarcomas [1,2].
Retroperitoneal liposarcoma affects both sexes equally. The average age at diagnosis is around the fifth decade, but the disease can affect all age groups. The slow increase in tumor volume and the compliance of the retroperitoneal space explain the tumor's long asymptomatic nature [1,2].
From an anatomopathological point of view, we rely on the AJCC classification based on size, grade, the depth of the tumor, and the presence or absence of lymphadenopathy or metastases. The clinical presentation is polymorphic and characterized by borrowed signs, depending on the region where the tumor develops and the stage of progression. Certain associated manifestations may be observed, such as multiple intramuscular or subcutaneous lipomas or scrotal liposarcoma.[3].
Laboratory tests do not contribute to the diagnosis; they sometimes reveal paraneoplastic hypercalcemia. Abdominal ultrasound shows a homogeneous hyperechoic mass displacing adjacent organs, allowing diagnosis in 30 to 50% of cases. Abdominopelvic tomodensitography is the key examination; it reveals a heterogeneous hypodense tumor, clarifies its relationship to adjacent organs, guides aspiration and biopsy, and allows for postoperative monitoring. Magnetic resonance imaging (MRI) can detect vascular invasion. Fine-needle aspiration cytology has been used by many authors; its limitations are the small amount of material and the experience of the pathologist. Percutaneous biopsy always carries the risk of seeding along the path of the biopsy needle [3,4,5].
The primary treatment is surgery. The excision must be complete and must extend into healthy tissue. A safety margin of two centimeters is considered optimal. If the patient underwent a preoperative biopsy, the excision will include the entry point of the biopsy trocar as well as the tract [3].
This surgery is often difficult due to the proximity of major blood vessels. Oncological imperatives sometimes necessitate organ sacrifice (kidney, spleen, tail of the pancreas) and vascular sacrifices (inferior vena cava, iliac artery or vein).
Sacrificing the infrarenal vena cava requires no additional procedures; however, arterial sacrifice necessitates reconstitution of the system Arterial [6,7].
In cases of metastases, adjuvant or neoadjuvant chemotherapy with doxorubicin is used. The course of the disease is characterized by very frequent local recurrences (40 to 90%), which justifies wide excisions and aggressive treatment.
A second resection is beneficial in cases of low-grade liposarcoma.
Poor prognostic factors include high grade, size greater than 5 cm, and age over 50 years. Myxoid liposarcoma has a better prognosis than other forms. Distant metastases can occur in the liver, pleura, and peritoneum. They are not common in liposarcoma, which has a higher tendency to recur. Very often, patients who undergo surgery for liposarcoma die from a recurrence [8,9].
Conclusion
Retroperitoneal liposarcoma is a rare malignant tumor, which often remains asymptomatic for a long time and is diagnosed late.
The treatment of retroperitoneal sarcomas requires a multidisciplinary approach and a center specializing in this rare clinical entity which will allow compartmental surgery with clear resection margins (R0) to improve the prognosis of these tumors.
References
- Antinori A, Antonacci V, Magistrelli P. Giant retroperitoneal liposarcoma. Am J Surg, 2002; 184(1): 56–57.
- Stoeckle E, Ciondre JM, Bonvalot S, Kantor G, Terrier P, Bonichon F, et al. Prognostic factors in retroperitoneal sarcoma: a multivariate analysis of a series of 165 patients of the French Cancer Center Federation Sarcoma Group. Cancer, 2001; 92(2): 359–368.
- Moley JF, Eberlein TJ. Soft-tissue sarcomas. Surg Clin North Am, 2000; 80.
- Jaques DP, Coint OG, Hajd SI. Management of primary and recurrent soft-tissue sarcoma of the retroperitoneum. Ann Surg, 1990; 212: 51-59.
- Ishida H, Naganuma H, Konno K, Sato M, Hamashima Y, Konno S, et al. Retroperitoneal liposarcoma: sonographic findings. Abdom Imaging, 2000; 2: 554-558.
- Zheng W, Song S, Liang F. Major blood vessel excision and reconstruction in the treatment of retroperitoneal neoplasms [abstract]. Chung Hua Chung Liu Tsa Chih, 1998; 20: 225-227.
- Barret A, Bossavy JP, Stouff S, Gouzi JL, Gedeon A. Retroperitoneal tumors and surgery of the great vessels. Chirurgie, 1997; 122: 25-30.
- Lewis JJ, Leung D, Woodruff JM, Brennan MF. Retroperitoneal soft-tissue sarcoma: analysis of 500 patients treated and followed at a single institution. Ann Surg, 1998; 228: 355-365.
- Karmouni T, El Fassi MJ, Ech-Cherif El Kettani N, El Khader K, Tazi K, Koutani A, et al. Liposarcome rétropéritonéal. À propos d’un cas. Ann Urol, 2001; 35: 273-275.

