Evaluation of Prescription Practices and WHO-Aligned Rational Drug Use Indicators in Outpatient Department Patients: A Cross-Sectional Audit Study
Ruhamah Arshad2, Saleha Sajjad2, Aqna Malik1,2,*, Rafia shoukat2, Rida Ahmed2, Sana Saeed2, Sara liaquat2 and Farwa Liaquat3
1Department of Pharmacy, The University of Lahore, Pakistan
2Department of Pharmacy, The University of Chenab, Gujrat, Pakistan
3Department of Physical Therapy, University of Lahore, Islamabad campus
Received Date: 21/01/2026; Published Date: 13/03/2026
*Corresponding author: Dr. Aqna Malik, Department of Pharmacy, University of Chenab, Gujrat; Department of Pharmacy, University of Lahore, Lahore, Pakistan
https://orcid.org/0000-0003-3875-9621
Abstract
Background: Prescription audits provide actionable insight into prescribing quality and rational drug use. This study evaluated outpatient prescriptions using structured WHO-aligned indicators captured in an Excel proforma.
Methods: A retrospective cross-sectional study designed to collect prescription data from OPDs of public and private tertiary care teaching hospitals in Sialkot and Kharian by PG students at The University of Chenab. 642 printed prescriptions were selected for audit study after random sampling and initial analysis. using HIS of concerned hospitals from August 2025 to January 2026. Prescription analysis was done via close assessment of demographic data, diagnosis, drug information, and prescription completeness, Generic prescribing, antibiotic prescribing rate, and drug classes included in current medications prescribed to patient visiting OPD Medicine ward,prescritions were assessed as per criteria of WHO prescribing guidelines and indicators for good prescribing. under supervision of Dr. AQNA MALIK, Department of Pharmacology, The University of Chenab, Gujrat,
Statistical analysis: Data was analyzed using descriptive statistics and One-way ANOVA in GraphPad 10.6.2.1.
Results: A total of 642 prescriptions were audited. The mean age of patients was 40.4±18.8 years (range 1–85). Most patients were Adult (18–59): 501.8 (78.16%), followed by elderly patients (≥60): 113.03 (17.6%) and Paediatric (<18): 27.13 (4.22%).
The mean number of current medications was 3.56± 1.72. Polypharmacy (≥5 current medications) occurred in 30 (21.12%). Antibiotics were prescribed in 37.23%.
Dose was mentioned in 528.9 (82.39%, dosage form in 533.5 (83.1%), directions appropriate in 515.4 (80.28%), and medications aligned with BP/weight in 334.6 52.1%).
Conclusion: Although technical prescription completeness was high, antibiotic exposure and medication burden exceeded WHO-recommended thresholds, supporting targeted quality-improvement interventions.
Keywords: Prescription audits; WHO prescribing indicators; Rational drug use
Introduction
Rational drug use is defined as the prescription of appropriate medications in doses that meet patient needs for an adequate period at the lowest cost. Rational Prescribing satisfies patient needs for an adequate period at the lowest cost is rational drug use.
Irrational prescribing increases morbidity, polypharmacy, adverse medication responses, and antimicrobial resistance in developing healthcare systems. Prescription audits objectively evaluate prescribing trends and treatment guidelines.
Current study used rational drug use indicators to assess outpatient prescription procedures and identify quality improvements. The WHO defines rational medication use as administering relevant medicines in right doses for an acceptable period at the lowest cost to patients and communities. Irrational prescribing causes adverse drug reactions, AMR, and unnecessary healthcare costs. To measure drug consumption and enhance quality, WHO advises routine monitoring using key prescription indicators. This study used WHO-aligned rational drug use indicators tailored to dataset factors to assess outpatient prescription patterns. The WHO defines rational medication use as administering relevant medicines in right doses for an acceptable period at the lowest cost to patients and communities. Irrational prescribing causes adverse drug reactions, antimicrobial resistance, and unnecessary healthcare costs. To measure drug consumption and enhance quality, WHO advises routine monitoring using key prescription indicators. This study used WHO- aligned rational drug use indicators tailored to dataset factors to assess outpatient prescription patterns. The prescription of relevant pharmaceuticals in levels that satisfy patient needs for an adequate period at the lowest cost is rational drug use.
Irrational prescribing increases morbidity, polypharmacy, adverse medication responses, and antimicrobial resistance in developing healthcare systems. Healthcare providers in many clinical contexts must write prescriptions well. A well written prescription fits patients' therapeutic needs and reduces pharmaceutical errors during dispensing. Since prescriptions are legal documents, Registered Medical Practitioners must be careful while dispensing them. Medical regulators may discipline prescribers for medication errors, which can result in patient distrust, legal issues, and legal action. Medication mistakes cause roughly 41% of hospital admissions worldwide, causing significant societal and economic harm. Several research suggest that collaborative student-teacher sessions can assist students develop prescription writing skills. The medical curriculum includes P-drug exercises, problem based learning, and prescription-writing assignments. These educational methods teach students how to create a rational medication inventory, choose case-specific drugs, and improve patient adherence, reducing irrational and outdated clinical prescribing. Clear and legible prescriptions are as important as correct diagnosis and medicine selection for the patient's condition, which affects the prescription's quality and efficacy. Several studies have shown that doctors' illegible handwriting has serious economic and health consequences for the community. Therefore, it is crucial to link numerous elements to provide the best patient therapy. By assessing clinical management, a prescription audit improves patient care and treatment outcomes. To meet WHO core prescribing indicators, Outpatient and Inpatient Departments (OPD and IPD) must have regular prescription audits. Audits can identify, assess, and reduce prescription writing errors, increasing pharmaceutical quality and safety.
Objective of Study: The objective of this study was to audit the drug prescriptions from the OPD of Medicine in a tertiary care teaching hospitals in Public and Private hospitals of Sialkot and Kharian to investigate and identify the recurring low-scoring parameters, and to incorporate corrective actions to help the prescribers improve the overall quality of prescriptions in OPD.
Methods
This retrospective observational cross-sectional study was carried out in public and private tertiary care teaching hospitals of Sialkot and Kharian to collect prescription data from OPD patients,
Sample size and sampling
Using the formula n = Z2 * P * (1 - P)/d 2, the sample size was calculated to be a minimum of 642 at a 95% confidence level with a prevalence of 56.4%. Convenient sampling was used as a sampling technique. A total of 642 printed prescriptions was randomly sampled and analysed using the hospital information system (HIS), The study data for prescription auditing was collected for a period of 6 months, i.e., August 2025-January 2026.
Data collection and analysis
The prescriptions from the public and private tertiary care teaching hospitals of Sialkot and Kharian to collect prescription data from OPD patients, were accessed by logging in to the HIS, and relevant information like demographic data, diagnosis, drug information, and prescription completeness was collected on a preset prescription audit form manually. Data collection was done by M. Phil students from University of Chenab, who, interned in tertiary care Hospitals. The collected data were screened, analysed, and evaluated for appropriateness and rationality using the WHO core prescription indicators by Dr AQNA MALIK, Department of Pharmacology, The University of Chenab, Gujrat. Self structured Excel Performa was used as Data collection tool. Manual entry of appropriate data into Microsoft Excel spreadsheets (Microsoft Corp., Redmond, WA, US) was performed on a day-to-day basis. Descriptive statistics were used to summarize the findings. The analysis of the OPD prescriptions encompassed three main categories: patient and prescriber information, drug-related information, and WHO core prescribing indicators. Prescribing indicators and patient data were retrieved from prescriptions. First, demographic information was collected on each patient, including MR number on OPD prescription, age, gender, and age groups. Clinical factors such PMH, current diagnosis (where recorded) were noted. Among prescribing indicators number of drugs per prescription, previous medications, newly prescribed medications. To check rationality of prescription indicators like dose appropriateness, exact duration of dose mentioned, compliance with body weight and BP, prescription indicators related to antibiotic prescribed (Yes/No), relevance of antibiotic therapy, culture sensitivity basis (Performed or not). Safety indicators like drug interactions, contraindications were assessed and prescriptions were assessed for documentation of monitoring parameters. The average number of medications per contact, antibiotic prescribing rate, polypharmacy rate, dose documentation, dosage form, directions, and blood pressure and body weight-based therapy were WHO-aligned prescribing metrics. Previous and current drugs were used to calculate medication counts and polypharmacy.
Statistical analysis
Data was analysed using descriptive statistics and One-way ANOVA in GraphPad 10.6.2.1.
Results
Demographic Characteristics
A total of 642 prescriptions were audited. The mean age of patients was 40.4±18.8 years (range 1–85). Most patients were Adult (18–59): 501.8 (78.16%), followed by elderly patients (≥60): 113.03 (17.6%) and Paediatric (<18): 27.13 (4.22%).
Prescriptions comply with WHO-Aligned Prescribing Indicators:
Table 1: Prescriptions comply with WHO-Aligned Prescribing Indicators.
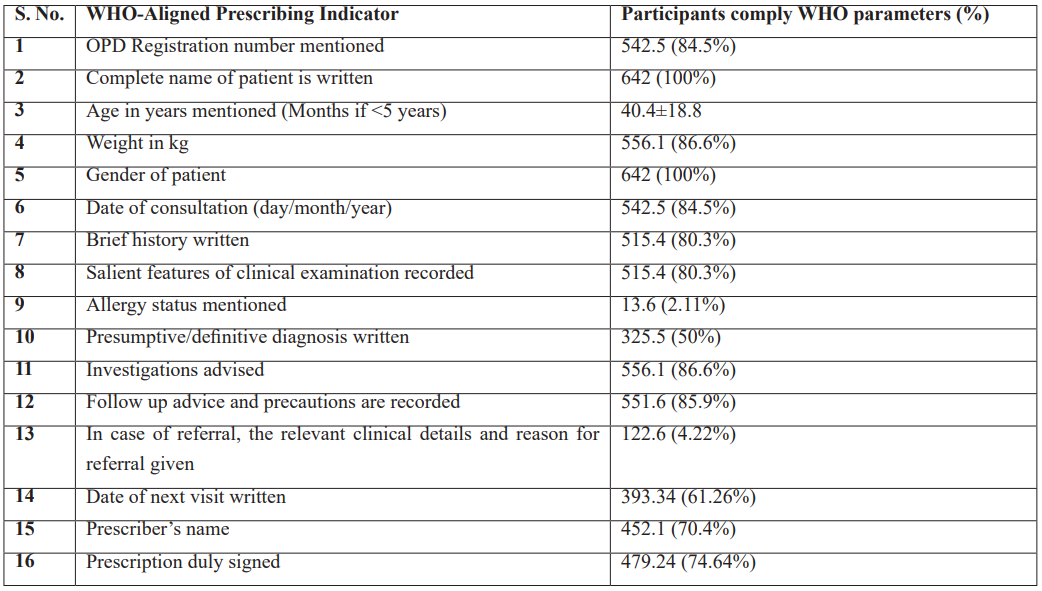
WHO Core Prescribing Indicators
WHO Core Prescribing Indicators including mean number of current medications per prescription, Polypharmacy (≥5 current medications), while polypharmacy based on total medications (previous plus current) was also observed.
Core Prescribing Indicators
Core Prescribing Indicators as per WHO Guidelines were also noted and calculated like Mean drugs per encounter as per current&Previous medications prescribed, Polypharmacy rate, Antibiotic prescribing rate and Individualized therapy
Table 2: WHO Core Prescribing Indicators.
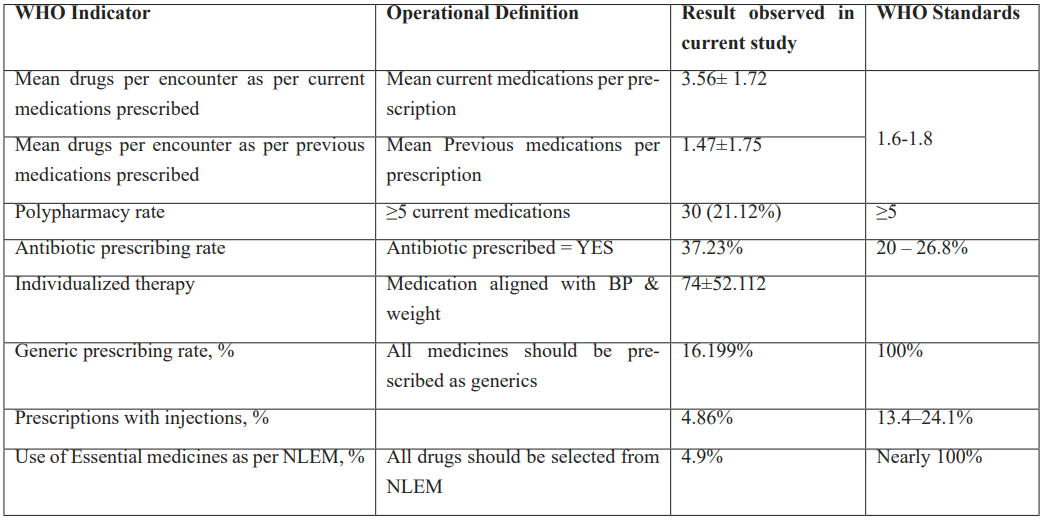
Prescription Completeness and Safety Indicators as per WHO guidelines
Among total 642 prescriptions both from public and private sector hospitals observations related to indicators like Dose & Dosage form mentioned, appropriateness of dosage and directions like how and when to take medications etc. as per WHO guidelines were recorded.
Table 3: WHO Prescription Completeness and Safety Indicators.
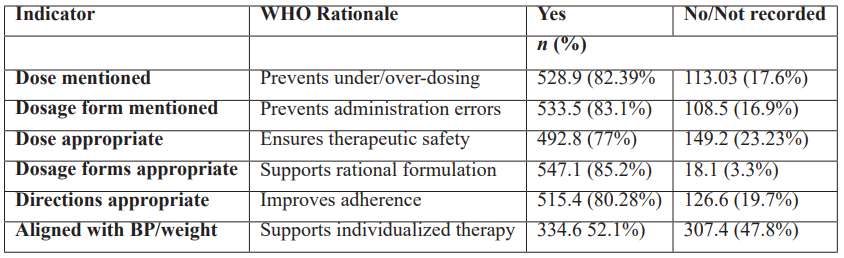
Antibiotics Prescribing:
Antibiotic prescribing was evaluated in Table.7, according to the core metric, which is the percentage of patient encounters with at least one antibiotic prescribed.
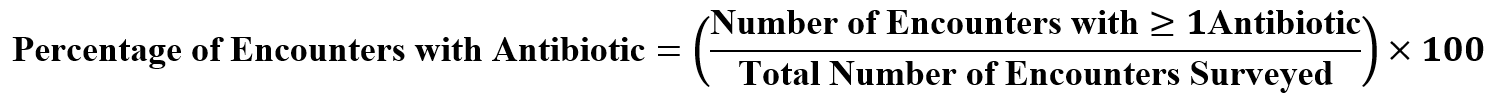
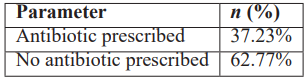
Table 4: WHO Stewardship-Oriented Antibiotic Indicator.

Drug Class wise Prescription Analysis:
Table 5: Distribution of Drug Classes Prescribed.
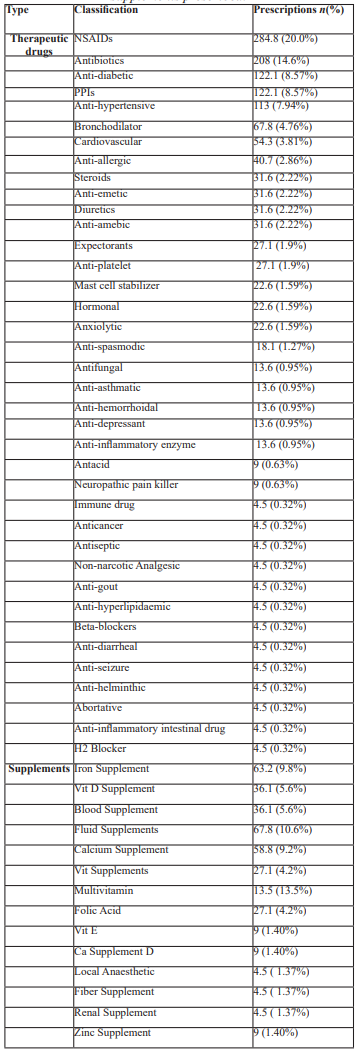
Table 6: Fixed-Dose Combination Prescribing.
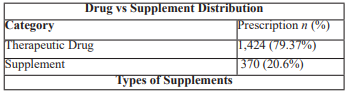
Table 6: Fixed-Dose Combination Prescribing.
Discussion
This audit demonstrates that while prescribers generally select appropriate therapeutic agents, critical gaps exist in prescription completeness and safety documentation. Polypharmacy was common, especially among elderly patients, consistent with international prescribing trends in chronic disease populations.
The omission of treatment duration is a well-recognized contributor to poor compliance and antibiotic misuse. Furthermore, limited documentation of monitoring parameters increases the risk of adverse drug events, particularly in patients receiving diuretics, antiplatelets, and antihypertensives.
Antibiotic prescribing was relatively restrained. Overall, these findings underscore the need for system-level interventions such as standardized prescription formats, antimicrobial stewardship programs, and clinical pharmacist participation in OPDs.
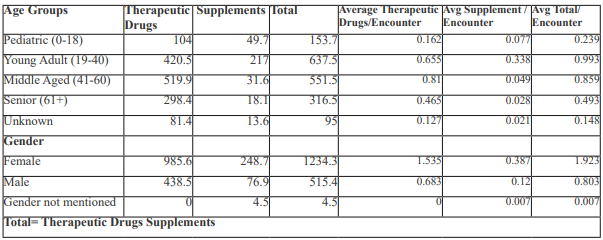
Despite high compliance with technical prescription components, WHO-recommended thresholds for medication burden and antibiotic exposure were exceeded. The average number of drugs per encounter was higher than WHO’s optimal range, and more than two-fifths of patients received antibiotics, raising antimicrobial stewardship concerns.
Individualized therapy based on blood pressure and weight was not documented in over one-quarter of prescriptions, indicating suboptimal patient-centered prescribing. Polypharmacy was particularly notable when prior medications were considered, suggesting cumulative medication burden and potential drug–drug interaction risks.
Implementation of standardized prescription templates, antimicrobial stewardship programs, and routine pharmacist-led audits could improve rational drug use.
Summary
Results drawn from calculations from prescription data summarise that Total therapeutic drug classes prescribed were 1,424, while total supplements prescribed were 370.Overall, 1794 drugs were prescribed in total, and the average number of drugs/Prescription was 2.218, and the average number of supplements/Prescription was 0.514.
Conclusion
The prescription audit revealed acceptable therapeutic selection but suboptimal documentation practices and limited safety monitoring. Strengthening rational prescribing through institutional protocols and continuous medical education is essential to enhance patient safety and treatment effectiveness.
Strengths
- Real-world outpatient data
- Broad assessment of rational drug use indicators
- Inclusion of antibiotic stewardship parameters
- Suitable for quality improvement initiatives
Limitations
- Single centre design
- No clinical outcome correlation
- Lack of laboratory and diagnostic integration
- Descriptive analysis only
- Reliance on prescription data without physician interviews
References
- Tariq RA, Vashisht R, Sinha A, et al. Medication Dispensing Errors and Prevention. In. StatPearls, Treasure Island (FL): StatPearls Publishing,
- Jadav S.Comparative study of patient-based versus case-based teaching in prescription writing skills of second year MBBS students. International Journal of Basic & Clinical Pharmacology, 2020. doi: 18203/2319-2003.IJBCP20200178.
- Singh T, Banerjee B, Garg S, Sharma S.A prescription audit using the World Health Organization-recommended core drug use indicators in a rural hospital of Delhi. J Educ Health Promot, 2019; 15: doi: 10.4103/jehp.jehp_90_18.
- World Health Organization (WHO). How to Investigate Drug Use in Health Facilities,
- Sharma M, Payal N, Devi LS, et al. Study on Prescription Audit from a Rural Tertiary Care Hospital in North India. J Pure Appl Microbiol, 2021; 15: 1931-1939. doi: 22207/JPAM.15.4.14.
- Prasad K, Ranasinghe B.Pattern of private sector drug prescription in Galle: A descriptive crosssectional study. Gall Med J, 2006; 4: 64-6
- Haque M.Essential medicine utilization and situation in selected ten developing countries: A compendious audit. J Int Soc Prevent Communit Dent, 2017; 7: 147-1 doi: 10.4103/jispcd.JISPCD_224_17.
- Atal S, Jhaj R, Mathur A, Rai N, Misra S, Sadasivam B.Outpatient prescribing trends, rational use of medicine and impact of prescription audit with feedback at a tertiary care centre in India. The International Journal of Health Planning and Management, 2021; 36: 738-7 doi: 10.1002/hpm.3116.
- Chatterjee M, Datta S, Mandal P.Prescription Audit using WHO Core Drug Use Indicators in a Tertiary Care Centre in Eastern India: Clinical Pharmacology Block 1 Elective for MBBS Students. SSR Inst Int J Life Sci, 2025; 11: 7354-7360.
- Pagani S, Lombardi N, Crescioli G.On Behalf Of the MEREAFaPS Study Group. Drug-Related Hypersensitivity Reactions Leading to Emergency Department: Original Data and Systematic Review. J Clin Med, 2022; 16: doi: 10.21276/SSR-IIJLS.2025.11.3.7.
- Margolis KL, Ray RM, Van Horn L. Women's Health Initiative Investigators: Effect of calcium and vitamin D supplementation on blood pressure: the Women's Health Initiative Randomized Trial. Hypertension, 2008; 52: 847-8doi: 10.1161/HYPERTENSIONAHA.108.11499.
- Banerjee I, Bhadury T, Agarwal M.Prescribing pattern in orthopedics outpatient department of a medical college in India. Int J Basic Clin Pharmacol, 2017; 4: 1175-117
- Margolis KL, Ray RM, Van Horn L.Women's Health Initiative Investigators. Effect of calcium and vitamin D supplementation on blood pressure: the Women's Health Initiative Randomized Trial. Hypertension, 2008; 52: 847-8doi: 10.1161/HYPERTENSIONAHA.108.114991.
- Sohail R, Mathew M, Patel KK.Effects of Non-steroidal Anti-inflammatory Drugs (NSAIDs) and Gastroprotective NSAIDs on the Gastrointestinal Tract: A Narrative Review. Cureus, 2023; 15: doi: 10.7759/cureus.37080.
- Nagla A, Wadagbalkar P, Raipurkar S, Patel P. Prescription pattern study of drugs in orthopedics outpatient department (OPD) of a rural medical college hospital & research centre in. MP Indian J Orthop Surg, 2016; 2: 367-3
- Mehta SR, Kashyap AS, Das S.Diabetes Mellitus in India: The Modern Scourge. Med J Armed Forces India, 2009; 65: 50-5 doi: 10.1016/S0377-1237(09)80056-7.
- Hypertension control rate in India: systematic review and meta-analysis of population-level non-interventional studies, 2001-2022 Koya. Shaffi Fazaludeen et al.The Lancet Regional Health - Southeast Asia, 9:doi: 10.1016/j.lansea.2022.100113.
- Cazzola M, Matera MG. Fixed-dose combination inhalers. Handb. Exp. Pharmacol, 2017; 237: 117-129. doi: 1007/164_2016_66.
- Revikumar KG, Veena R.Fixed dose combinations in indian medicine market-a SWOT analysis. MOJ Bioequiv Availab, 2017; 4: 276-280.
- Singh A, Dhaneria S, Gupta D.Physician's knowledge, attitude and practice of fixed drug combinations: Can we recognize the lacunae?. J Family Med Prim Care, 2022; 11: 2019-2025. doi: 4103/jfmpc.jfmpc_1788_21.
- Saha D, Patel J, Buckingham D, et al. Urine culture follow-up and antimicrobial stewardship in a pediatric urgent care network. Pediatrics, 2017; 139: 20162103. doi: 10.1542/peds.2016-2103.

