Cytomegalovirus-Related Multisystem Disorder with Cardiac Tamponade and Monoclonal Gammopathy: A Rare Case Report
Payal Shukla1,2,*, Anil Regmi1 and Rakeshkumar Subramanian3
1Department of Internal Medicine, Parkview Health, Fort Wayne, Indiana
2Department of Anesthesiology, University of Iowa Hospitals and Clinics, Iowa City, Iowa
3Department of Pulmonology and Critical Care, Parkview Health, Fort Wayne, Indiana
Received Date: 23/12/2025; Published Date: 02/03/2026
*Corresponding author: Payal Shukla, Department of Internal Medicine, Parkview Health, Fort Wayne, Indiana; Department of Anesthesiology, University of Iowa Hospitals and Clinics, Iowa City, Iowa
Abstract
Cytomegalovirus (CMV) is a DNA virus and a member of the Herpesviridae family that can affect immunocompetent and immunocompromised individuals. In certain cases, CMV can cause multisystem involvement, which may trigger transient monoclonal gammopathy. The mechanism for this is complex and remains poorly understood. We report a rare case of CMV-related multisystem disorder in an immunocompetent patient with cardiac tamponade, pneumonia, pancytopenia, and diarrhea, who was later diagnosed with monoclonal gammopathy of undetermined significance (MGUS).
Keywords: Cytomegalovirus; Monoclonal gammopathy of undetermined significance; Immunology; Multisystem involvement; Viral immunology
Introduction
Cytomegalovirus (CMV) is a member of the Herpesviridae family, specifically classified as human herpesvirus 5 [4]. It is a double stranded DNA virus, and one of the largest viruses known to cause clinical disease. Other members of the herpes viruses include herpes simplex virus and varicella-zoster virus. CMV is primarily transmitted through direct contact with bodily fluids such saliva, tears, blood, and urine. Similar to other herpes viruses, after the resolution of the initial infection, CMV remains dormant within the host in the myeloid cells [4].
CMV infections often affect the salivary glands, leading to localized symptoms such as sore throat and cough [4]. However, most CMV infections are asymptomatic and do not require treatment, particularly in immunocompetent individuals. Treatment is typically reserved for severe or symptomatic infections in immunocompromised patients, such as those with HIV/AIDS, transplant recipients, or patients with congenital CMV. When indicated, the primary treatment includes Ganciclovir, a nucleoside analog whose antiviral activity involves phosphorylation by the CMV protein kinase, pUL97 [4].
CMV infections can cause multisystem involvement in immunocompromised individuals, but rarely affect immunocompetent patients. In such rare cases, CMV can present as a multisystem disorder with a wide range of clinical manifestations. These include CMV Hepatitis, CMV Esophagitis, Pneumonitis, Polyradiculopathy, Transverse Myelitis, and Subacute Encephalitis [4]. In non-immunocompromised patients, CMV is rarely fatal, however, immunocompromised patients, including those using corticosteroids, or undergoing chemotherapy can have significant morbidity and mortality.
CMV infections often trigger an immune response leading to production of immunoglobulins. There are few published case reports linking CMV infections with transient monoclonal gammopathies, including Monoclonal Gammopathy of Undetermined Significance (MGUS), particularly in immunocompetent patients. Further studies are necessary to explore the mechanisms underlying this probable relationship.
We present a rare case of CMV infection in an immunocompetent individual, manifesting as a multisystem disorder accompanied by MGUS.
Case Report
A 41-year-old female with no significant past medical history presented with shortness of breath, fever, fatigue, and diarrhea. Physical examination revealed elevated jugular venous pressure, distant heart sounds, and pulsus paradoxus—suggestive of pericardial tamponade.
Laboratory studies showed pancytopenia, elevated inflammatory markers, and a high CMV DNA viral load. Echocardiography and chest computed tomography revealed a large pericardial effusion consistent with cardiac tamponade and bilateral patchy pulmonary infiltrates. Bronchoscopy, Bronchoalveolar Lavage (BAL), and transbronchial biopsy showed a lymphocytic-predominant inflammatory response, though histopathological evaluation was non-diagnostic.
Fungal workup, including histoplasmosis, blastomycosis, cryptococcus, and aspergillus antigen testing were negative. Respiratory pathogen PCR and blood cultures were negative. Cardiac MRI findings consistent with subacute myopericarditis, and MRI of the abdomen/MRCP revealed hepatosplenomegaly. Further investigation, including protein electrophoresis, showed elevated serum kappa and lambda as well as elevated immunoglobulins. Bone marrow biopsy revealed clonal plasma cell proliferation consistent with IgM Monoclonal Gammopathy of Undetermined Significance (MGUS).
The patient underwent pericardiocentesis with drain placement, which provided temporary relief of her symptoms. As her condition continued to decline and with no alternative etiology was identified, she was diagnosed with severe CMV-associated illness and initiated on intravenous ganciclovir therapy. Her clinical status improved gradually following treatment. During admission, the patient experienced episodes of arrhythmia and hypotension, which were managed with intravenous albumin and amiodarone.
Follow-up CT chest showed significant improvement in the bilateral pneumonia. Repeat serum protein electrophoresis showed resolution of the monoclonal gammopathy, supporting a transient MGUS likely related to the acute CMV infection.
Table 1
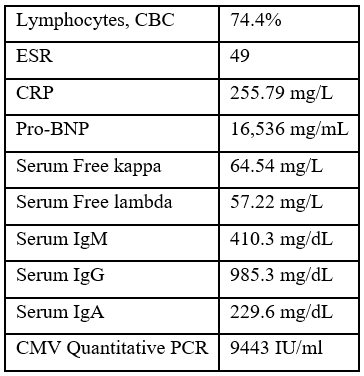
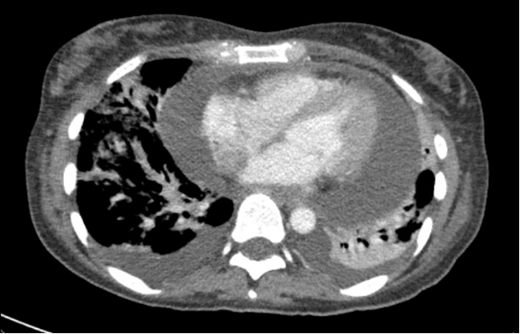
Figure 1: CT chest showing large pericardial effusion.
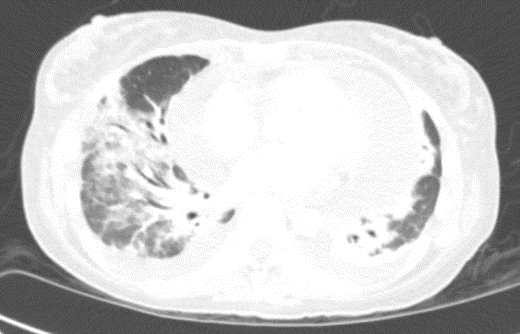
Figure 2: CT chest showing lung infiltrates.
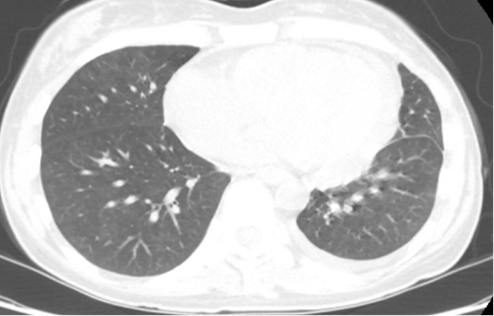
Figure 3: CT chest showing improved pericardial effusion and lung infiltrates.
Discussion
CMV-related multisystem disorder is a rare clinical entity that can present with a wide range of clinical manifestations. This case highlights the potential for CMV infection to cause severe multisystem involvement, including life-threatening cardiac tamponade, pneumonia, and pancytopenia, even in immunocompetent individuals without underlying hematological disorders.
The pathophysiology underlying CMV-induced multisystem involvement in immunocompetent individuals is not fully understood. CMV infection progresses through distinct phases: an initial systemic replication phase that activates the innate immune system, followed by a persistent phase with tissue-localized replication, and finally a latency phase with restricted viral gene expression. During the systemic phase, widespread viral replication can lead to significant tissue damage and inflammation, potentially resulting in multisystem involvement.
CMV has also been associated with hematologic abnormalities, including cytopenias. The virus can infect hematopoietic progenitor cells and disrupt normal hematopoiesis, leading to conditions such as anemia, leukopenia, and thrombocytopenia. It is unclear whether the severe CMV infection contributed to the patient's MGUS. However, the patient did undergo follow-up serum testing, which showed resolution of the elevation of immunoglobulins.
Multiple Myeloma and MGUS are plasma cell dyscrasias that are characterized by the monoclonal proliferation of pathological plasma cells and uncontrolled production of immunoglobulins [4].
MGUS is characterized by the presence of a monoclonal protein (M-protein) in the without clinical features of malignant plasma cell disorders [4]. Chronic antigenic stimulation, including viral infections, may contribute to the development and persistence of MGUS [4]. Studies have reported a high prevalence of monoclonal gammopathy among immunocompetent patients with primary CMV infection, suggesting a potential causal relationship; however, further studies are needed to confirm causality between CMV infection and MGUS.
Conclusion
In the diagnosis of CMV-related multisystem disorder, it is important to rule out other infectious and non-infectious causes of the patient's clinical presentation, such as other viral infections, connective tissue disorders, and malignancies. Elevated CMV DNA levels, along with a high index of suspicion, can help in establishing the diagnosis.
To date, only one other published case report links CMV with systemic involvement and monoclonal gammopathy. This study involves a 62-year-old immunocompetent patient, similar to this case, presenting with splenic vein thrombosis and pulmonary embolism, in addition to MGUS [1]. Further studies are needed to better understand the pathogenesis and clinical course of this rare manifestation of CMV infection in immunocompetent individuals.
In conclusion, early diagnosis and appropriate management are essential to improving clinical outcomes in this rare manifestation of CMV infection in immunocompetent patients.
Provenance and peer review: Not commissioned, externally peer-reviewed.
Ethical approval and consideration: According to the local ethical guidelines, ethical approval is unnecessary to write a case report. We obtained written informed consent from the patient to include the clinical details.
Sources of funding: No funding was obtained for this case report.
Author contributions: Payal Shukla, Anil Regmi, and Rakeshkumar Subramanian.
Rakeshkumar Subramanian was involved in direct patient care including establishing the diagnosis, coordinating the patient's management with different specialties, and treating the patient.
References
- de Rooij E, Verheul R, de Vreede M, de Jong Y. Cytomegalovirus infection with pulmonary embolism, splenic vein thrombosis and monoclonal gammopathy of undetermined significance: a case and systematic review. BMJ Case Rep, 2019; 12(3): e226448. doi: 10.1136/bcr-2018-226448.
- Giordano L, Cacciola R, Barone P, et al. Autoimmune Diseases and Plasma Cells Dyscrasias: Pathogenetic, Molecular and Prognostic Correlations. Diagnostics (Basel), 2024; 14(11): 1135. doi:10.3390/diagnostics14111135.
- Gonsalves WI, Rajkumar SV. Monoclonal Gammopathy of Undetermined Significance. Ann Intern Med, 2023; 176(2): 288. doi: 10.7326/AITC202212200.
- Gupta M, Shorman M. Cytomegalovirus. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing, 2025.
- Grzelak et al., J Immunol, 2018.

