Sudden Death Within 24 Hours Due to Severe Dengue Fever During a 2020 Outbreak in Mayotte : A Systemic Literature Review
Abdoulahy Diallo*
Service de Médecine, Centre Hospitalier de Mayotte, Pamandzi, Mayotte
Received Date: 29/12/2025; Published Date: 05/02/2026
*Corresponding author: Abdoulahy Diallo, Service de Médecine, Centre Hospitalier de Mayotte, Pamandzi, Mayotte
Abstract
Background: Dengue fever, also know as « tropical influenza », has a wide spectrum of clinical presentations, often with unpredictable clinical evolution and outcome.
Case presentation: Five deaths were recorded within 24 hours of admission to the hospital in Mayotte, including four cases diagnosed by PCR and one case by serological test. Among these patients, three were women and two men with ages between 32 and 54. The diagnosis at the time of clinical presentation was severe dengue. Two cases of dengue shock syndrome, one case of myocarditis, one case of myopericarditis and finally one case of dengue hemorrhagic fever were the causes of deaths.
Conclusion: Viral dengue infection is a multi-systemic disease, which can quickly become fatal if not diagnosed and managed from the outset, as demonstrated by the death of five patients in our study within 24 hours of their admission to hospital.
Keywords: Outbreak; Severe dengue; Death within 24 hours; Mayotte
Abbreviations: ALF - Acute Liver Failure; ARF - Acute Renal Failure; ALT - Alanine aminotransferase; AST - Aspartate aminotransferase; BNP - Brain natriuretic peptide; Bpm - Beat per minute; CSF - Cerebrospinal fluid; DHF - Dengue Haemorragic Fever; DSS - Dengue Shock Syndrome; DIC - Disseminated Intravascular Coagulation; DENV – Dengue; ECG – Electrocardiogram; TTE - Trans-Thoracic Echocardiography; LVEF - Left ventricular ejection fraction; F – Female; ICU - Intensive Care Unit; IgG - Immunoglobulin G; IgM - Immunoglobulin M; MOF - Multi-Organ Failure; Mo – Months; M – Male; ND - No data available; NSAID - Non-Steroidal Anti-Inflammatory Drug; OSAHS - Obstructive sleep apnea/hypopnea syndrome; PCR - Polymerase Chain Reaction
Introduction
Dengue is a re-emerging disease that is more common in tropical, subtropical and recently temperate climates. In Mayotte, dengue is now the main human arbovirus with a cumulative incidence of 16.1 cases per 1,000 inhabitants in 2020 due to population growth estimated at 321,000 (+ 3.8% per year on average) and urbanization. In the past, Mayotte reported two outbreaks of dengue that could be documented, 2010 with 108 cases (caused by DENV-3), and 2014 with 522 cases (caused by DENV-2). There was no death or severe form. But in 2020, the worst dengue epidemic occurred in Mayotte, 4. 491 cases confirmed biologically since March 2019 of which 4,305 cases in 2020 with 31 deaths registered including 21 at the Hospital Center of Mayotte. Only DENV-1 serotype circulated during this outbreak [1].
Dengue is one disease entity with different clinical presentations and often with unpredictable clinical evolution and outcome. While most patients recover from a non-severe, self-limiting clinical course, a small proportion progress to serious disease, characterized by plasma leakage with or without hemorrhage. The long-standing 1997 World Health Organization (WHO) dengue classification and management scheme was recently revised in 2009, replacing DF, Dengue Hemorrhagic Fever (DHF), and Dengue Shock Syndrome (DSS) with Dengue without Warning Signs, Dengue with Warning Signs (abdominal pain, persistent vomiting, fluid accumulation, mucosal bleeding, lethargy, liver enlargement > 2 cm , increasing hematocrit with decreasing platelets) and Severe Dengue (SD; dengue with severe plasma leakage, severe bleeding, or organ failure) [2]. The lethality of severe forms is on average 1 to 5% and can reach 20% in the absence of early and appropriate medical treatment [3]. Mortality in the dengue shock patient in the intensive care unit (ICU) is significantly associated with a decreased level of consciousness, the lowest platelet count, and the number of organs that have failed [4].
Dengue myocarditis/pericarditis is exceeding rare, with only a handful of cases reported in world literature. A review revealed myocarditis and pericarditis were present in 2.9% and 0.1% of cases, respectively [5]. The risk of atypical cardiac manifestations is more in patients with non-severe dengue with warning signs and severe dengue than in patients with non-severe dengue without warning signs [6] and these manifestations may present variable clinical signs, symptoms, etiologies and outcomes, including sudden death [7, 8].
Here, we describe the first series of five cases of severe dengue in adults who suddenly dead within 24 hours of admission during a 2020 outbreak in Mayotte and review the literature.
Case Report
Case 1: A 32-year woman was admitted on April 21, 2020 at about 06 :45 pm in the emergency room for a fall due to awkwardness, with pain in the left knee without any notion of fever. April 22, 2020 at about 02 :00 am, she suddenly had chest pain with dyspnea and restlessness progressing towards a first cardiac arrest. After several attempts of resuscitation, unfortunately the patient died at 03 :35 am. In view of the various clinical elements, the diagnosis of fulminant Myocarditis was confirmed. Biology finds Troponin I (cTnI) HS at 1.186 μg/L, dengue serology showed a presence of IgG and IgM anti-dengue virus.
Case 2: A 38-year-old woman consults on April 06, 2020 at 07 :00 am in the emergency room for abdominal pain and watery diarrhea without fever that began on April 05, 2020. She is receiving symptomatic treatment. April 06, 2020 At 12 :38 pm, she subsequently presented with hemodynamic failure with cold extremities, rapid pulse, tachycardia at 130 bpm with uncontrollable blood pressure, always apyretic. Gasometry finds a lactate 10 - ph 7.08 - HCO3- 13. ECG finds a under PQ and micro-voltage. The biology before transfer to ICU showed a BNP at 122 pg/mL, troponin 1.092 μg/L. A cardiac examination shows an TTE with a circumferential pericardial effusion 1 cm not compressive, LVEF 10%, subaortic VIT 4.5 cm at best, variation of the peak of systolic velocity therefore probable hypovolemia. The diagnosis of fulminant Myopericarditis was confirmed. At about 02 :00 pm the patient is transferred to ICU and dies at 04 :20 pm. Dengue PCR Type 1 on April 06, 2020 at 04 :50 pm was positive.
Case 3: A 38-year man had febrile syndrome with flu-like syndrome and vomiting for 4 days without his state motivates him to consult until the evening to March 12, 2020. His condition then quickly worsened, which led him to go to the emergency room. Upon admission, no biological analysis was carried out. On March 13, 2020, at 10 :08 AM, he was transferred to intensive care following a tonic-clonic crisis. The gasometry showed a pH of 6.94, Lactates >15, HC03- 9. Dengue PCR Type 1 was positive. The patient died at 02 :48 pm. The diagnosis of Dengue Shock Syndrome (DSS) was retained.
Case 4: A 54-year man with a history of high blood pressure, type 2 diabetes, obstructive sleep apnea syndrome, hypertensive cardiomyopathy. Arrival in the emergency on April 01, 2020 at about 09 :45 pm for a morning hematemesis of medium abundance associated with epigastric pain with parallel deterioration of his respiratory status. The clinical examination found arterial hypotension at 74/50 mmHg, heart rate at 123 bpm, SpO2 88% in ambient air, temperature at 36.7°C. The biology found white blood cells at 16.6 giga/L, hemoglobin at 11.6 g/dL, platelet at 62 giga/L, prothrombin index at 72%, ALT 259 IU/L, AST 114 UI/L. The venous gasometrics found a pH 7.35, lactate 6.5. Dengue PCR Type 1 was positive. On April 02, 2020, around 09 :40 am, she was transferred to resuscitation. The Oeso-gastroduodenal fibroscopy (FOGD) that found bright red blood in the stomach without ulcer or lesion visualized, presence of a large clot in the fundus, and no esophageal varice. The patient died on April 02, 2020 at 11 :55 pm. The diagnosis of dengue hemorrhagic fever (DHF) was confirmed.
Case 5: A 40-year-old woman with a history of high blood pressure who presented on May 24, 2020, with a fever, chills, myalgia, and headache. The next day confusion appeared with repeated vomiting and watery diarrhea with abdominal pain. She consulted at the emergency room on May 28, 2020 at 9 :52 am. At admission, she had correct hemodynamic parameters and a neurological examination without any particularity. On May 28, 2020 at 1 :00 pm, patient transferred to dechocage in front of an obnubilation accompanied by a generalized tonic-clonic convulsion associated with desaturation. Neurological examination found a glasgow at 7. Both the brain scan and lumbar puncture were normal. Dengue PCR Type 1 was positive. Around 5 :27 pm, she was transferred to intensive care with an intubation on arrival. In view of the aggravating metabolic acidosis and the frank oliguria and despite intensive resuscitation, patient will die at 1 :00 pm on May 29, 2020. The diagnosis of dengue shock syndrome (DSS) was confirmed.
Literature Review
We searched the PubMed and Google database to identify articles published in the literature. The terms « Severe dengue », « Death within 24 hours » were crossed during the search, completed by a secondary manual search.
A total of 21 relevant articles involving 39 patients were found through the research [9-29]. The information collected includes the year of publication, demographic data, medical history, the length of time between symptom onset and emergency room admission, as well as the time span between admission and development of complications, then between the occurrence of complications and death. We also collected data on the biological analysis technique, dengue serotype, and the precise cause of death. This information is summarized in Table 1.
Fatal outcomes as in our case have also been reported in these different articles namely Dengue Haemorrhagic Fever (DHF)/Dengue Shock Syndrome (DSS), Myocarditis, Pericarditis, Encephalitis, Cerebral haemorrhagic, Pulmonary haemorrhagic.
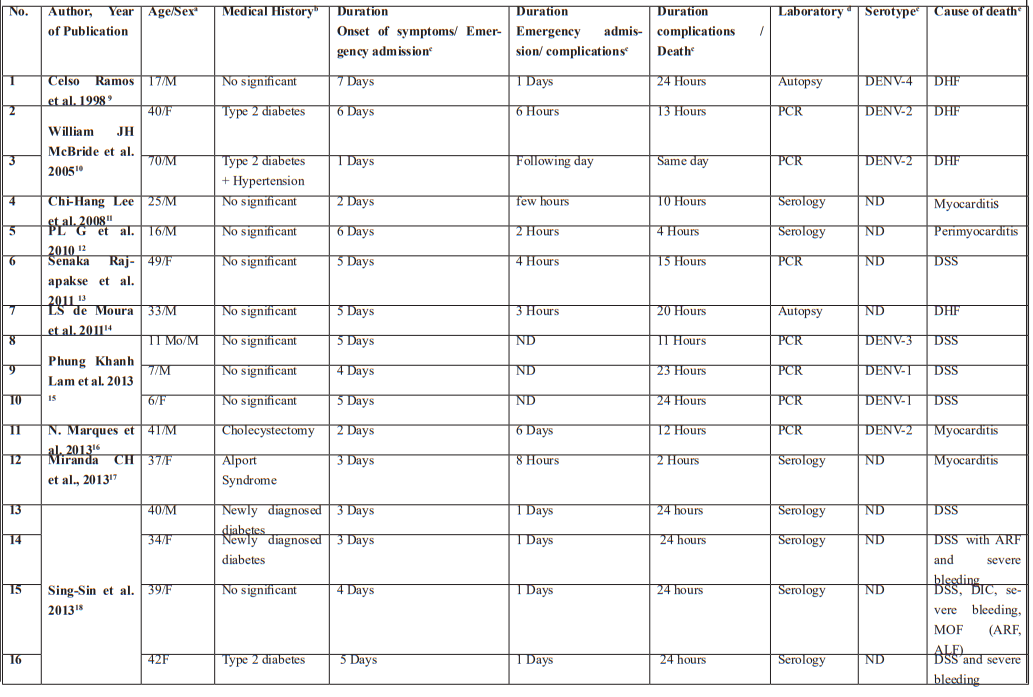
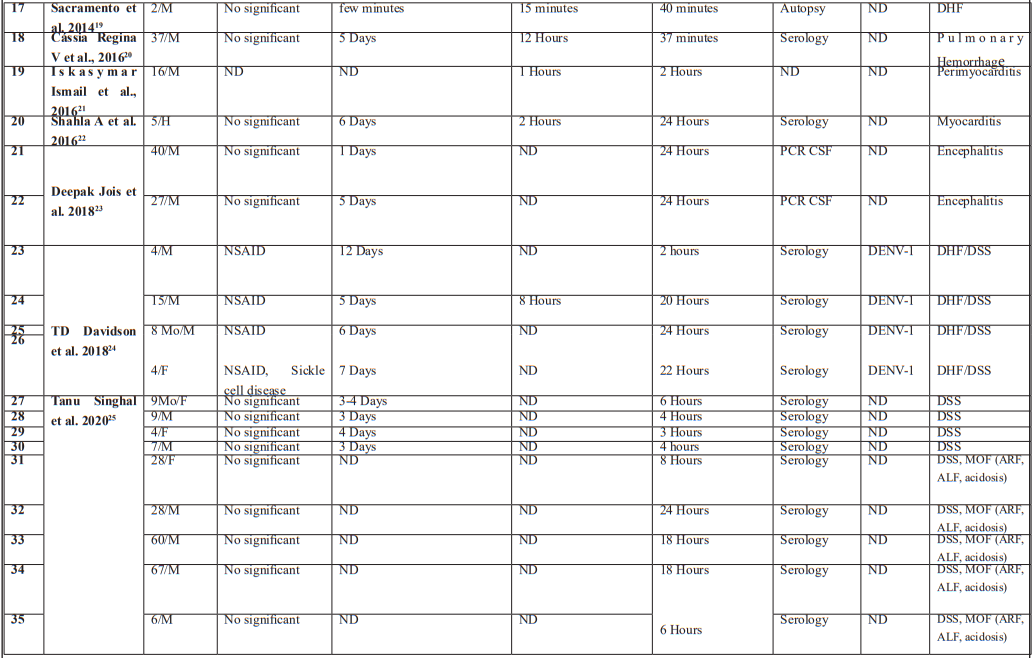
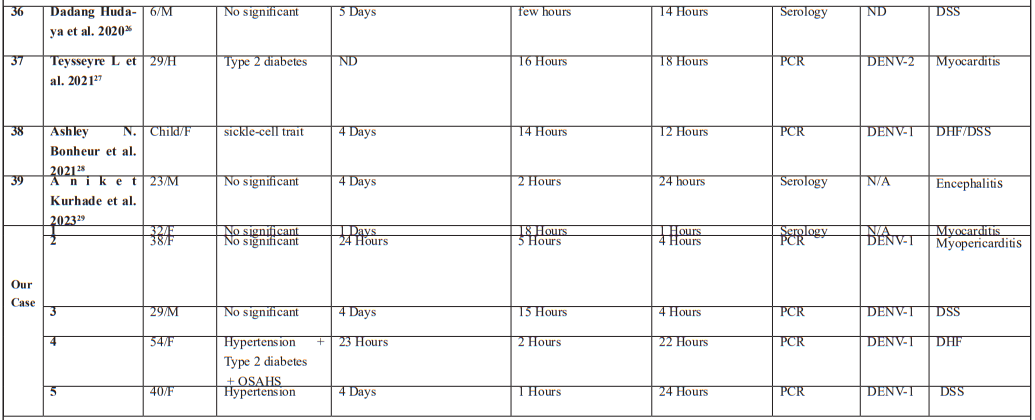
aAge/ Sex-- Months (Mo)/ Female (F); Male (M).
bMedical History— Non-Steroidal Anti-Inflammatory Drug (NSAID), Obstructive sleep apnea/hypopnea syndrome (OSAHS).
cDuration/Serotype-- No data available - (ND).
dLaboratory-- Polymerase Chain Reaction- (PCR), Cerebrospinal fluid (CSF).
eCause of death- Acute Liver Failure (ALF) ; Acute Renal Failure (ARF) ; Dengue Haemorragic Fever (DHF) ; Dengue Shock Syndrome (DSS) ; Disseminated Intravascular Coagulation (DIC) ; Multi-Organ Failure (MOF).
Discussion
Fatal outcomes, similar to those of our study, have been reported in several research works. Nwe Ni Linn and colleagues studied 304 patients, 81 (26.6%) of whom died within 24 hours of admission [30]. Nguyen Thi Kim Tien and his collaborators found that in 2000, half of the deaths also occurred within the first 24 hours after hospitalization [31]. Jose G and colleagues reported that 30% of patients (seven people) died within 24 hours of being admitted to the hospital [32]. Yuan Liang Woon and his team reported that, among 322 fatal cases of dengue (94 in 2013 and 228 in 2014), the average age of patients was 40.7 19.3 years. Approximately 8.4% of these patients experienced rapid deterioration, resulting in death within 24 hours of admission [33]. Finally, Somia Iqtadar and his colleagues observed that the majority of admissions took place on the second day of the illness. Some critically ill patients have seen their condition worsen rapidly, leading to four deaths within 24 hours of arrival at the hospital [34].
A study published in 2019 by Pulak Mutsuddy’s team, involving 14,121 cases between 2013 and 2017, concluded that 28 deaths were recorded, of which more than 70% occurred within 24 hours of hospital admission [35]. For his part, Mohammad Nayeem Hasan and his collaborators reported that from 1,705 deaths in 2023, 67.4% (or 1,015 cases) died within one day of their admission to the hospital [36].
To date, no early and reliable marker allowing to predict the evolution towards a dengue shock has been identified, nor specific treatment for this complication. Consequently, the management of dengue shock syndrome (DSS) remains essentially symptomatic, relying on the restoration of blood volume by infusion of hyperosmotic solutions. The nature, infusion rate and quantity of fluids administered must be adapted according to the patient’s clinical condition and weight, with rigorous monitoring to ensure optimal management [37, 38, 39]. Although these treatments are not specific, their early implementation reduces mortality from 40% to less than 1% [40].
Ahmed Mubarak Daakeek and his collaborators demonstrated, by comparing early deaths (occurring within 24 hours of presentation) and late deaths (occurring after 24 hours), that cases of early deaths were significantly similar in terms of age, of gender, comorbidities and other parameters. They also observed that there were no significant differences between patients who died within 24 hours and those who died later [41]. These results suggest that prolonged hospitalization does not necessarily influence the mortality rate related to dengue, contrary to what other studies report [42, 43].
Conclusion
Viral dengue infection is a multi-systemic disease, which can quickly become fatal if not diagnosed and managed from the outset, as demonstrated by the death of five patients in our study within 24 hours of their admission to hospital.
The clinical evolution of dengue towards fatal complications, the most common being dengue shock syndrome is undoubtedly the result of many factors, imperfectly identified, which make it difficult to understand the disease and consequently, the establishment of early diagnosis and appropriate treatment.
A better understanding of the mechanisms involved in endothelial dysfunction responsible for plasma leakage could allow to highlight specific biomarkers or even predictive of evolution towards shock, as well as mechanisms or molecules likely to constitute therapeutic targets [50].
Conflict of interest: The authors declare that they have no conflict of interest.
Ethical approval: The authors certify that they comply with the Principles of Ethical Publishing.
References
- Surveillance sanitaire de la dengue à Mayotte. Point épidémiologique, 2020.
- World Health Organization. Dengue guidelines for diagnosis, treatment, prevention and control : new edition, 2009: 1–160.
- Huy NT, Van GT, Thuy DHD, Kikuchi M, Hien TT, et al. Factors associated with dengue shock syndrome: a systematic review and meta-analysis. PLoS Negl Trop Dis, 2013; 7: e2412.
- Chen C-M, Chan K-S, Yu W-L, Cheng K-C, Chao H-C, Yeh C-Y, et al. The outcomes of patients with severe dengue admitted to intensive care units. Medicine, 2016; 95.
- Malik J, Iltaf Satti D. Cardiovascular manifestations of dengue. Heart, 2022; 108: A58. 1136/heartjnl-2022-BCS.78
- Adams CD, Syro D, Llano JF, Betancur JF. Myocarditis: an uncommon manifestation of dengue fever infection. BMJ Case Rep, 2021; 14: e241569. 1136/bcr-2021-241569
- Sagar S, Liu PP, Cooper LT, Jr. Myocarditis. Lancet, 2012; 379: 738-747. doi: 10.1016/s0140 6736(11)60648-x.
- Cooper LT, Jr. Myocarditis. N Engl J Med, 2009; 360: 1526-1538. doi: 1056/NEJMra0800028.
- Celso Ramos, Gilma SBnchez, Rogelio Hernandez Pando, Javier Baquera, Dalia Hernandez, Javier Motal, et al. Dengue virus in the brain of a fatal case of hemorrhagic dengue fever. Journal of NeuroVirology, 1998; 4: 465-468.
- William JH McBride. Deaths associated with dengue haemorrhagic fever : the first in Australia in over a century. MJA, 2005; 183: 35-37.
- Chi-Hang Lee, Clarence Teo, Adrian F. Low. Fulminant dengue myocarditis masquerading as acute myocardial infarction. International Journal of Cardiology, 2009; 136; e69–e71. Doi :1016/j.ijcard.2008.05.023
- PL Goh. Dengue perimyocarditis : a case report. Hong Kong j.emerg.med, 2010; 17: 58-60.
- Senaka Rajapakse. Dengue shock. J Emerg Trauma Shock, 2011; 4: 120-127. DOI :4103/0974-2700.76835.
- Luƒá sa Salles de Moura Mendonça et al. Splenic Rupture in Dengue Hemorrhagic Fever Report of a Case and Review. Jpn. J. Infect. Dis., 2011; 64: 330-332.
- Phung Khanh Lam, et al. Clinical Characteristics of Dengue Shock Syndrome in Vietnamese Children : A 10-Year Prospective Study in a Single Hospital. Clinical Infectious Diseases, 2013; 57(11): 1577–1586.
- Marques N, Gan VC, Leo Y-S. Dengue myocarditis in Singapore : two case reports. Infection, 2013; 41: 709–714. DOI: 1007/s15010-012-0392-9.
- Carlos Henrique Miranda, et al. A case presentation of a fatal dengue myocarditis showing evidence for dengue virus-induced lesion. European Heart Journal : Acute Cardiovascular Care, 2013; 2(2): 127–130. DOI : 10.1177/2048872613475889
- Sing-Sin Sam et al. Review of Dengue Hemorrhagic Fever Fatal Cases Seen Among Adults : A Retrospective Study. PLoS Negl Trop Dis, 2013; 7(5): e2194. Doi :1371/journal.pntd.0002194
- Rafael Henrique Machado Sacramento et al. Death by dengue fever in a Brazilian child : a case report. BMC Research Notes, 2014; 7: 855.
- Cássia Regina Vancini-Campanharo et al. Dengue Infection Could Provoke Cardiac Arrest and Death. Int Arch Nurs Health Care, 2016; 2: 030.
- Iskasymar Ismail, Tengku Suriani Tengku Ismail, Norzian Ismail. Dengue Perimyocarditis ; hypovolemic vs cardiogenic shock? 1st EMAS MEETING 2016. M-JEM Supplementary.
- Shahla Abrar, Mohammed Junaid Ansari. Acute fulminant myocarditis in a case of dengue fever : A case report. Asian Pac J Trop Dis, 2016; 6(4): 328-329. Doi : 1016/S2222-1808(15)61039-8.
- Jois D, Moorchung N, Gupta S, Mutreja D, Patil S. Autopsy in dengue encephalitis : An analysis of three cases. Neurol India, 2018; 66: 1721-1725. DOI : 10.4103/0028-3886.246276
- TD Davidson, I Vickers, CDC Christie. Outcome of Dengue in Hospitalized Jamaican Children. WIMJ Open, 2018; 5(1): 25. DOI: 10.7727/wimjopen.2016.525.
- Tanu Singhal and Vatsal Kothari. Clinical and Laboratory Profile of Fatal Dengue Cases at a Tertiary Care Private Hospital in Mumbai, India. Am. J. Trop. Med. Hyg., 2020; 103(3): pp. 1223–1227. Doi :10.4269/ajtmh.19-0425.
- Dadang Hudaya Somasetia et al. A fatal course of multiple inflammatory syndrome in children coinfection with dengue. A case report from Indonesia. IDCases, 2020; 22: e01002. http://dx.doi.org/10.1016/j.idcr.2020.e01002.
- Laura Teysseyre, et al. Case Report: Refractory Shock due to Fulminant Dengue Myocarditis Treated with Venoarterial Extracorporeal Membrane Oxygenation : A Report of Four Cases. Am. J. Trop. Med. Hyg., 2021; 104(2): pp. 552–556. Doi :10.4269/ajtmh.20-0372.
- Ashley N Bonheur, et al. A fatal case report of antibody‑dependent enhancement of dengue virus type 1 following remote Zika virus infection. Bonheur et al. BMC Infect Dis, 2021; 21: 749. https://doi.org/10.1186/s12879-021-06482-0.
- Aniket Kurhade. Death due to Dengue Encephalitis : A Rare Case Report. Journal of Clinical and Diagnostic Research, 2023; 17(10): OD10-OD12. DOI : 10.7860/JCDR/2023/63767.18563.
- Linn NN, Kyaw KWY, Shewade HD, et al. Notified dengue deaths in Myanmar (2017-18) : profile and diagnosis delays F1000 Research, 2020; 9: 579. https://doi.org/10.12688/f1000research.23699.1.
- Nguyen Thi Kim Tien, Nguyen Ngoc Anh Tuan, Khau Minh Tuan, Nguyen Trong, et al. Epidemiological Analysis of Deaths Associated with Dengue Haemorrhagic Fever in Southern Viet Nam in 1999- 2000. Dengue Bulletin, 2001; 25.
- Jose´ G, Rigau-Pe´ rez, Miriam K. Laufer. Dengue-Related Deaths in Puerto Rico, 1992–1996. Diagnosis and Clinical Alarm Signals. Clinical Infectious Diseases, 2006; 42: 1241–1246.
- Woon YL, Hor CP, Hussin N, Zakaria A, Goh PP, Cheah WK. A Two-Year Review on Epidemiology and Clinical Characteristics of Dengue Deaths in Malaysia, 2013-2014. PLoS Negl Trop Dis, 2016; 10(5): e0004575. doi: 10.1371/journal.pntd.0004575.
- Iqtadar S, Akbar N, Mehmood M, Abaidullah S. Clinical Audit of Dengue related deaths in 2011 at Mayo Hospital Lahore Pakistan. Pak J Med Sci, 2017; 33(5):1070-1073. Doi : https://doi.org/10.12669/pjms.335.13051
- Pulak Mutsuddy, Sanya Tahmina Jhora, Abul Khair Mohammad Shamsuzzaman, Golam Kaisar SM, Md Nasir Ahmed Khan. Dengue Situation in Bangladesh : An Epidemiological Shift in terms of Morbidity and Mortality. Canadian Journal of Infectious Diseases and Medical Microbiology, 2019; Article ID 3516284: 12 pages. https://doi.org/10.1155/2019/3516284.
- Hasan MN, Rahman M, Uddin M, Ashrafi SAA, Rahman KM, Paul KK, et al. The 2023 fatal dengue outbreak in Bangladesh highlights a paradigm shift of geographical distribution of cases. Epidemiology and Infection, 2025; 153(e3): 1–9. https://doi.org/10.1017/S0950268824001791.
- World Health Organization. Dengue haemorrhagic fever : diagnosis, treatment, prevention and control. 2nd edition. World Health Organization ed, Geneva, 1997.
- Wills BA, Nguyen MD, Ha TL, Dong TH, Tran TN, Le TT, et al. Comparison of three fluid solutions for resuscitation in dengue shock syndrome. N Engl J Med, 2005; 353: 877-889.
- Smart K, Safitri I. Evidence behind the WHO guidelines : hospital care for children : what treatments are effective for the management of shock in severe dengue ? J Trop Pediatr, 2009; 55: 145-148.
- Kalayanarooj S. Standardized Clinical Management : Evidence of Reduction of Dengue Haemorrhagic Fever Case-Fatality Rate in Thailand. Dengue Bulletin, 1999; 23: 10-17.
- Dakeek AM, Alghasali HS, Bahashwan AA. Dengue Related Deaths at Ibn-Sina Hospital- Al-Mukalla : Causes and Alarming Signals. J Infec Dis Treat, 2017; 3(2): 10.
- Assir MZK, Ahmad HI, Masood MA, Kamran U, Yusuf NW. Deaths due to dengue fever at a tertiary care hospital in Lahore, Pakistan. Scand. J. Infect. Dis, 2014; 46(4): 303–309.
- Leo Y-S, Thein TL, Fisher DA, Low JG, Oh HM, et al. Confirmed adult dengue deaths in Singapore : 5-year multi-center retrospective study. BMC Infect. Dis, 2011; 11(1): 1.
- Moraes GH, de Fatima Duarte E, Duarte EC. “Determinants of mortality from severe dengue in Brazil: a population-based case-control study,” ,e American Journal of Tropical Medicine and Hygiene, 2013; 88(4): pp. 670–676.
- Guzman MG, Alvarez M, Rodriguez R, et al. “Fatal dengue hemorrhagic fever in Cuba, 1997,” International Journal of Infectious Diseases, 1999; 3(3): pp. 130–135.
- Ooi EE, Goh KT, Wang DNC. “Effect of increasing age on the trend of dengue and dengue hemorrhagic fever in Singapore,” International Journal of Infectious Diseases, 2003; 7(3): pp. 231-232.
- Morrison AC, Zielinski-Gutierrez E, Scott TW, Rosenberg R. “Defining challenges and proposing solutions for control of the virus vector Aedes aegypti,” PLoS Medicine, 2008; 5(3): p. e68.
- Karunakaran A, Ilyas WM, Sheen SF, Jose NK, Nujum ZT. “Risk factors of mortality among dengue patients admitted to a tertiary care setting in Kerala, India,” Journal of Infection and Public Health, 2014; 7(2): pp. 114–120.
- Kalayanarooj S. “Standardized clinical management : evidence of reduction of dengue haemorrhagic fever case fatality rate in &ailand,” Dengue Bulletin, 1999; 23: pp. 10–17.
- Devignot S, Tolou H, Couissinier-Paris P. Le syndrome de choc de dengue : vers un décryptage de la physiopathologie. Med Trop, 2010; 70: 288-301.

