Paracortical Necrosis with a Twist: Monocytosis Predominant Kikuchi-Fujimoto Disease
Adarsh Agarwal1,*, Mehshar Khan1, Manasi Mundada2, Arumugam P1 and Rajani G1
1Department of Internal Medicine & Critical Care, Basavatarakam Indo-American Cancer Hospital & Research Institute, Hyderabad, Telangana, India
2Department of Pathology, Basavatarakam Indo-American Cancer Hospital & Research Institute, Hyderabad, Telangana, India
Received Date: 23/12/2025; Published Date: 30/01/2026
*Corresponding author: Adarsh Agarwal, Department of Internal Medicine & Critical Care, Basavatarakam Indo-American Cancer Hospital & Research Institute, Hyderabad, Telangana, India
Abstract
Background: Kikuchi-Fujimoto Disease (KFD) diagnosis relies on characteristic histopathology— paracortical necrosis with karyorrhectic debris and specific immunohistochemical patterns. Associated hematologic findings typically include neutropenia and lymphopenia, while monocyte abnormalities remain underdescribed in published literature.
Case: A 27-year-old female presented with four-week fever and bilateral multiregional lymphadenopathy. Laboratory investigation revealed moderate leucopenia (WBC 2.92 × 10⁹/L) with a distinctive monocytosis (8%; normal 2-6%), an atypical hematologic pattern not routinely emphasized in KFD. 18F-FDG PET-CT imaging showed metabolically active bilateral cervical, axillary, mediastinal, and iliac lymph nodes with high-avidity uptake (SUV_max 12.2 in right axilla, 11.2 in right cervical level II). Excisional lymph node biopsy revealed characteristic paracortical necrosis with abundant karyorrhectic debris. Immunohistochemistry demonstrated CD3+ T-cell predominance with conspicuous CD20 negativity in affected regions, CD68+ histiocytes, and scattered CD30+ cells—diagnostic for KFD. GeneXpert MTB/RIF was negative.
Unique Finding: Monocytosis accompanying moderate leucopenia represents an underrecognized hematologic phenotype in KFD that directly correlates with the disease's CD68+ histiocytic infiltration.
Clinical Impact: Recognition of this "monocytosis predominant" variant may facilitate earlier diagnosis and prevent unnecessary malignancy-directed interventions.
Conclusion: This case expands the recognized hematologic spectrum of KFD and highlights monocyte patterns as potential disease-specific diagnostic clues.
Keywords: Kikuchi-Fujimoto disease; Monocytosis; Paracortical necrosis; Hematologic phenotypes; Histiocytic necrotizing lymphadenitis; Diagnostic markers
Introduction
Kikuchi-Fujimoto disease, first described in 1972, presents diagnostic challenges due to overlapping clinical, radiographic, and histologic features with lymphoproliferative malignancies and infectious lymphadenitis. While the histopathologic hallmark—paracortical necrosis with karyorrhectic debris—is well-established, the associated hematologic abnormalities receive less systematic investigation and characterization.
Current literature documents anemia, neutropenia, and lymphopenia as characteristic findings in KFD. However, monocyte parameters have not been systematically evaluated in large cohorts, resulting in incomplete understanding of the disease's hematologic phenotype. Given that KFD fundamentally involves infiltration of CD68+ activated histiocytes (tissue macrophages derived from circulating monocytes), abnormalities in peripheral monocyte counts may represent a specific, underrecognized manifestation.
This case presents a 27-year-old female with KFD characterized by an atypical "monocytosis predominant" hematologic pattern—moderate leucopenia accompanied by elevated monocyte
percentage (8% versus normal 2-6%)—a combination rarely highlighted in published reports. This finding likely reflects the disease's fundamental pathophysiology and may serve as a diagnostic clue.
Case Presentation
A 27-year-old female with no significant medical history presented with four weeks of continuous fever (peak 38.5-39.2°C), malaise, and progressive weight loss. Physical examination revealed fever (38.8°C), bilateral tender cervical (levels II-IV) and axillary lymphadenopathy; spleen was not clinically enlarged. No rash or articular manifestations noted.
Complete Blood Count - Distinctive Hematologic Pattern: Hemoglobin: 113 g/L (mildly low); WBC: 2.92 × 10⁹/L (moderate leucopenia); Neutrophils: 54% (relatively elevated);
Monocytes: 8% (notably elevated; reference 2-6%); Lymphocytes: 38% (relatively preserved); Platelets: 265 × 10⁹/L (normal).
Infectious Workup: Blood cultures negative. Dengue, malaria, brucella, and scrub typhus serologies are all negative.
18F-FDG PET-CT Imaging: Metabolically active bilateral cervical nodes (right level II: 18 × 10 mm, SUV_max 11.2), bilateral axillary nodes (right: 21 × 10 mm, SUV_max 12.2—highest metabolic activity), mediastinal nodes (right paratracheal: 14 × 10 mm, SUV_max 4.1), and bilateral external iliac nodes (16 × 7 mm, SUV_max 6.2). No hepatosplenomegaly or pulmonary involvement.
Lymph Node Excisional Biopsy (Right Axilla): Fibrofatty tissue 3.0 × 1.3 × 1.0 cm, largest nodule 2.0 × 1.3 × 0.6 cm.
Histopathology (H&E Staining): Lymph node with effaced architecture. Atypical cells arranged in sheets displaying: Moderate eosinophilic cytoplasm, large nuclei with convoluted nuclear membranes (histiocytic morphology), Multiple foci of karyorrhectic debris (hallmark finding), Prominent areas of hyalinization, Remnant B-cell follicles partially preserved. Impression: Atypical lymphohistiocytic proliferation; recommend IHC.
Immunohistochemistry (Medium Panel)—Diagnostic Pattern:
CD3 (Clone MRQ-39): Diffuse positive staining, predominantly in interfollicular and paracortical regions
CD20 (Clone L26): Highlights remnant follicles only; negative in necrotic areas
CD30 (Clone BER-H2): Scattered positive cells (not extensive)
Myeloperoxidase (MPO): Scattered positive in histiocytes, reflecting myeloid origin
Diagnosis: Features favor Kikuchi-Fujimoto disease. The CD3+/CD20- pattern with paracortical necrosis, karyorrhectic debris, and MPO+ histiocytes established diagnosis. Differential considerations of autoimmune disease-associated lymphadenitis were excluded.
GeneXpert MTB/RIF Assay (on lymph node tissue): Mycobacterium tuberculosis NOT DETECTED. The patient was treated conservatively with anti-pyretics and NSAIDS and was discharged home with stable hemodynamics.
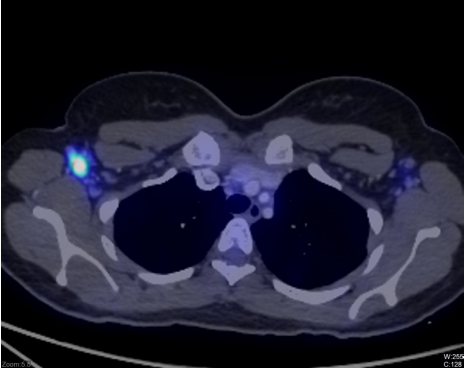
Figure 1: 18F-FDG PET CT scan showing right axillary lymph node.
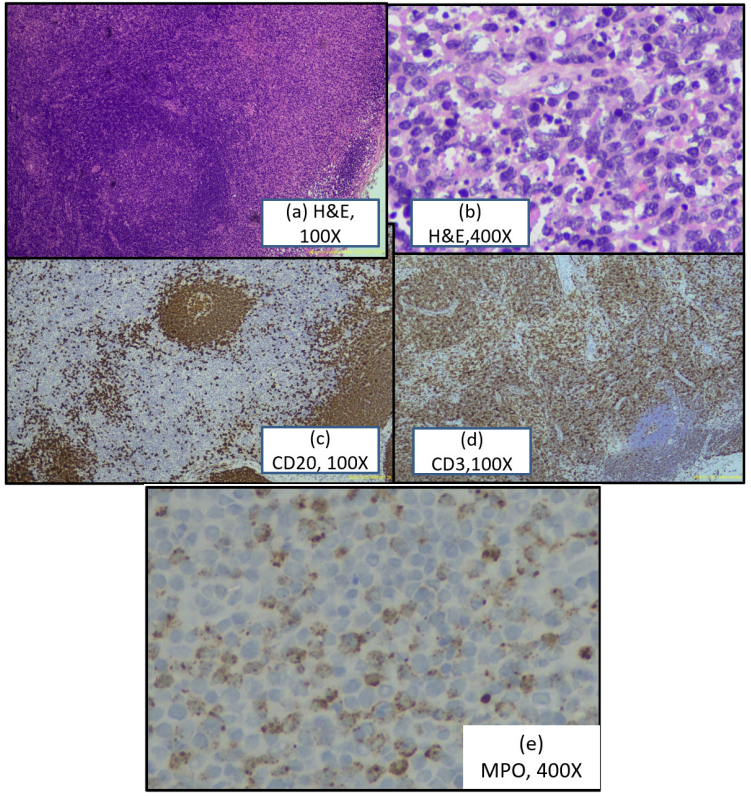
Figure 2:
(a): H&E microphotograph showing effaced lymph node architecture with preserved follicles and prominence of histiocytes.
(b): H&E microphotograph showing foci of karyorrhectic debri.
(c):Immunohistochemistry showing CD20 positive follicles
(d): Immunohistochemistry showing CD3 positive in interfollicular region.
(e): Immunohistochemistry showing MPO expression in histiocytes
Discussion
This case highlights an atypical hematologic phenotype in KFD: monocytosis accompanying moderate leucopenia. While the absolute WBC count decreased to 2.92 × 10⁹/L (moderate leucopenia), the monocyte percentage increased to 8%—a distinctive pattern rarely emphasized in KFD literature.
The pathophysiologic explanation is compelling: KFD involves CD68+ histiocytic infiltration of lymph nodes. Histiocytes are tissue-resident macrophages derived from circulating monocytes. Elevated peripheral blood monocytes in this patient likely represent either [1] compensatory release of monocyte precursors from marrow to replenish tissue histiocyte populations, or [2] systemic monocytic mobilization in response to inflammatory cytokine signaling orchestrating KFD immunopathology.
In contrast to published literature emphasizing neutropenia (11%) and lymphopenia (17%) in large KFD cohorts (Yu et al., 282 patients), monocyte abnormalities were not systematically characterized. This represents a literature gap. Recognition of monocytosis as an associated finding could represent a disease-specific hematologic phenotype.
The characteristic histology—paracortical necrosis with abundant karyorrhectic debris—directly correlates with the disease's fundamental pathophysiology: apoptosis of infiltrating lymphocytes. The immunohistochemical pattern (CD3+/CD20-) indicates T-cell-mediated disease with sparing of B-cell follicles, consistent with current understanding of KFD as a CD8+ T-cell-driven condition.
The high metabolic burden (SUV_max 12.2) exceeded typical KFD ranges (mean 4.2 ± 2.2) but aligns with severity criteria (Seong et al., 2021: SUV_max >9.27 indicates severe disease). This patient's presentation thus represents severe KFD with multisite involvement and heightened inflammatory response, potentially explaining the prominence of monocytosis.
Conclusion
This case expands the recognized hematologic spectrum of Kikuchi-Fujimoto disease by documenting a monocytosis-predominant variant characterized by moderate leucopenia with elevated monocyte percentage. This atypical hematologic phenotype likely reflects the disease's CD68+ histiocytic infiltration pathophysiology and warrants systematic investigation in future KFD cohorts. Recognition of monocytosis as a diagnostic clue, combined with characteristic histopathology and immunohistochemistry, facilitates accurate diagnosis and prevents unnecessary chemotherapy in this
benign, self-limiting condition. The monocytosis-predominant presentation described herein should be incorporated into clinician awareness as a potential disease-specific hematologic marker in KFD.
References
- Kikuchi M. Lymphadenitis showing focal reticulum cell hyperplasia with nuclear debris. Jpn J Lymphol, 1972; 5: 282-286.
- Fujimoto Y, Kojima Y, Yamaguchi K. Cervical subacute necrotizing lymphadenitis: A new clinicopathologic entity. Jpn J Clin Oncol, 1972; 2(1): 55-63.
- Mahajan VK, Sharma NL. Kikuchi-Fujimoto disease: Comprehensive review. Dermatol Pract Concept, 2023; 13(2): e2023077.
- Seong H, Song MH, Kyung YS, et al. Splenic uptake on FDG PET/CT correlates with Kikuchi disease severity. Radiology, 2021; 298(2): E65-E75.
- Yu SC, Lo KW, Tse HF, et al. Blood cell and marrow changes in patients with Kikuchi disease. Br J Haematol, 2022; 197(3): 334-345.
- Zhang J, Yao Z, Cheng L, et al. 18F-FDG PET/CT in Kikuchi disease patients. Int J Clin Exp Med, 2015; 8(11): 21034-21043.
- Diagnostic challenges in kikuchi-fujimoto disease: case report and review. Cureus, 2025; 17(1): e50842.

