A Rare Case of Coexisting Duodenal Atresia and Apple Peel Jejunoileal Atresia: A Case Report and Literature Review
Sara Hashim Yousif*, Ahmed Alolyet, Abdelbasit Elsayed Hamid, Abeer Seadan A Alrashedi and Tarek Talaat Harb Elkadi
Department of Pediatric Surgery, King Saud Medical City, Riyadh, KSA
Received Date: 06/11/2025; Published Date: 17/12/2025
*Corresponding author: Sara Hashim Yousif, Department of Pediatric Surgery, King Saud Medical City, Riyadh, KSA
Abstract
Coexistence of duodenal atresia and apple-peel jejunoileal atresia (type III B) is extremely rare and represents unique clinical challenges. To our knowledge, only 13 patients were reported in English literature, with 9 survivors. We report a 37-week baby girl with duodenal atresia associated with apple peel jejunoileal atresia. An end-to-end duodenojejunal anastomosis with tapering of the dilated duodenum was performed. This rare combination requires individualized surgical planning and multidisciplinary postoperative care to optimize the outcome. Reporting such cases enriches the literature and guides the management of future patients.
Keywords: Jejunoileal Atresia, Apple Peel, Duodenal Atresia, KSMC
Introduction
Duodenal atresia is one of the most common causes of intestinal obstruction in newborns. It has been linked to failure of recanalization of the duodenal lumen in early gestation. On the other hand, apple peel deformity is a rare variant of jejunoileal atresia that has been considered as a result of intrauterine vascular insult at later gestational stages [1]. The coexistence of duodenal atresia with apple peel jejunoileal atresia is exceptionally rare, with fewer cases documented in the literature.
This association of duodenal atresia and apple peel jejunoileal atresia queries the current embryology of duodenal atresia and poses significant surgical challenges.
Case Presentation
A 2.5 kg baby girl, born to a 26-year-old mother, at 37 weeks of gestation via cesarean section, was referred from another hospital to our neonatal intensive care unit (NICU) for evaluation of bilious vomiting since birth. The antenatal history was notable for polyhydramnios but no documented antenatal diagnosis of duodenal atresia or other form of obstruction.
At the referring hospital, the neonate underwent an upper gastrointestinal contrast study, which demonstrated duodenal obstruction.
The baby was active, in stable condition without respiratory distress, and had no obvious external dysmorphic features. There was upper abdominal fullness, and a bilious aspirate via nasogastric tube.
External genitalia and anal opening were normal. The baby has passed only pale mucus per rectum. Plain abdominal X-ray demonstrated the classic “double bubble” sign with absence of distal bowel gas (Figure 1).
Echocardiography revealed a small atrial septal defect (ASD), mild tricuspid regurgitation, and mild pulmonary regurgitation. No other congenital anomalies were detected.
On day 3 of life, an exploratory laparotomy was performed. Operative findings showed duodenal atresia with marked dilation of the proximal duodenum up to the second part below the duodenal papilla, ending blindly (Figure 2), associated with apple-peel (type IIIb) jejunoileal atresia (Figure 3). End-to-end duodenojejunal anastomosis was done along with tapering of the grossly dilated proximal duodenum using a GIA stapler (Figure 4).
Postoperatively, the baby was maintained on TPN while kept NPO. Nasogastric feeding was commenced on postoperative day 7 and advanced gradually to full feeds by postoperative day 11. The patient was discharged home on postoperative day 13 in good condition, with regular outpatient follow-up.
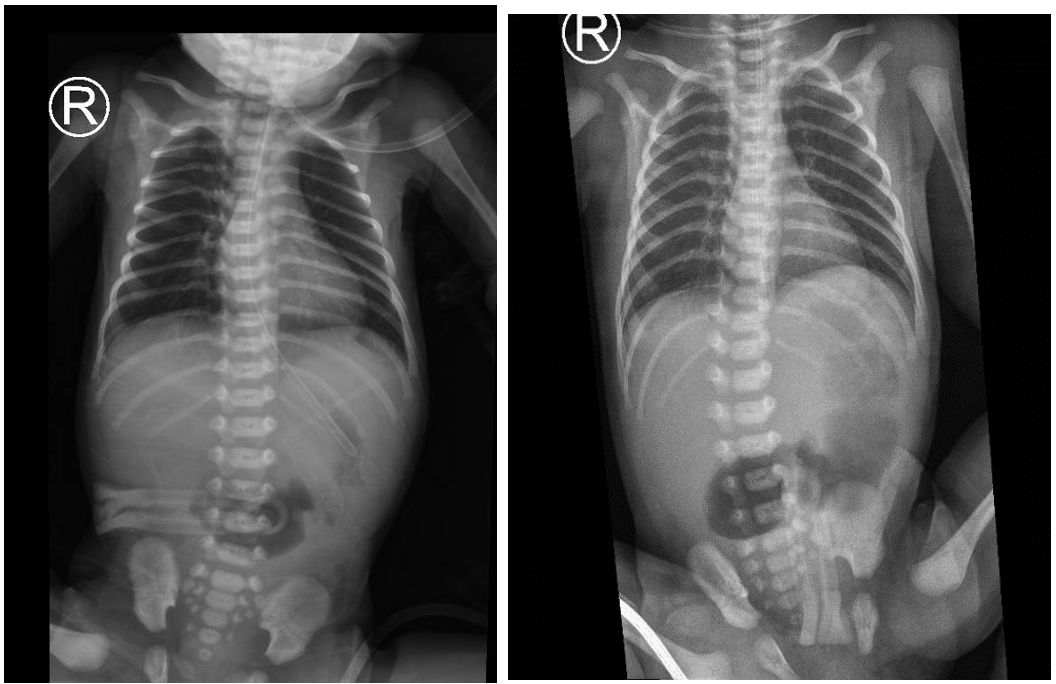
Figure 1: Plain abdominal x-ray showing double-bubble sign with no gas distally.
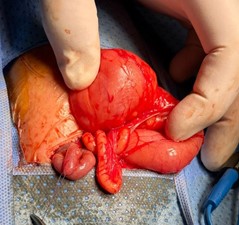
Figure 2: Image shows duodenal atresia.
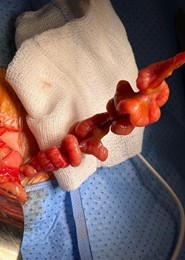
Figure 3: Image shows apple peel jejunoileal atresia.
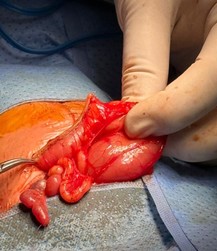
Figure 4: Image shows tapering of proximal dilated duodenum to perform end to end anastomosis.
Discussion
Duodenal atresia is one of the causes of neonatal intestinal obstruction with an incidence of about 1 in 5,000–10,000 live births. It is believed to be the result of the failure of recanalization of the duodenal lumen in early gestation.1 In contrast, apple peel deformity is a rare variant of jejunoileal atresia, characterized by the absence of the superior mesenteric artery and a spiral configuration of the small bowel supplied in a retrograde fashion by a single blood vessel from the ileocolic or right colic artery. It has been attributed to intrauterine vascular insult in the later weeks of gestation [2]. The simultaneous occurrence of duodenal atresia with apple- peel jejunoileal atresia is exceedingly rare, with fewer cases documented in the literature. Several hypotheses suggest that a vascular insult to the SMA during embryonic development may contribute to both lesions, either as a single event causing multi-level atresias or as separate insults occurring in close sequence [3,4]. Genetic factors have also been explored, although findings remain inconclusive [5].
Clinically, neonates typically present with bilious vomiting soon after birth and antenatal polyhydramnios [6], consistent with our patient’s presentation. Radiologically, the “double bubble” sign is suggestive of duodenal atresia, but distal bowel pathology such as apple-peel atresia is diagnosed intraoperatively.
Duodenal atresia is frequently associated with other congenital anomalies, most notably cardiac defects and down syndrome [7]. Cardiac defects, as seen in our case, are frequently reported and necessitate thorough evaluation.
This combination presents unique diagnostic and surgical challenges, as it involves both proximal intestinal obstruction and compromised distal bowel viability. Surgical management focuses on restoring intestinal continuity, while preservation of the fragile blood supply to the apple-peel segment is crucial. Tapering of the dilated duodenum and performing a duodenojejunal anastomosis, as done in this case, helps to overcome size discrepancies and maintain bowel function [8].
The outcomes depend on the length of preserved bowel, the presence of associated anomalies, and the quality of neonatal intensive care [9]. Recent studies report improving survival rates with advances in surgical and nutritional support. Our patient’s favorable postoperative course reflects these improvements.
Conclusion
Duodenal atresia associated with apple-peel jejunoileal atresia is an exceptionally rare condition that poses significant diagnostic and surgical challenges. Careful intraoperative assessment and tailored surgical techniques—such as tapering of the dilated duodenum and primary anastomosis—are crucial to preserve bowel length and function. Multidisciplinary postoperative management, including appropriate nutritional support, neonatal intensive care, contributes significantly to favorable outcomes. Reporting such cases enhances understanding and guides clinicians in managing this complex dual pathology.
References
- Molino Gahete JA, López Fernández S, Oliver B, et Duodenal atresia with apple peel associated with congenital diaphragmatic hernia: an exceptional case and a literature review. Cir Pediatr, 2022; 35(1): 31-35.
- Wong T, Volpe FAP, Tazima MF de FGS, Canesin WC, Sbragia Duodenal atresia with apple peel jejunoileal syndrome. J Pediatr Surg Case Rep, 2021; 64: 1–4.
- Sasa RV, Ranko L, Snezana C, Lidija B, Djordje S. Duodenal atresia with apple‑peel configuration of the ileum and absent superior mesenteric artery. BMC Pediatr, 2016; 16(1).
- Chinya A, Ratan SK, Aggarwal Duodeno jejunal Atresia with Apple-peel Appearance of the Remaining Ileum: A Rare Association. MAMC J Med Sci, 2015; 1: 34-36.
- Tatekawa Y, Kanehiro H, Nakajima Y. Duodenal atresia associated with "apple peel" small bowel without deletion of fibroblast growth factor-10 or fibroblast growth factor receptor 2IIIb: report of a case. Surg Today, 2007; 37: 430–433.
- Pathak M, Narula D. A case of duodenal atresia with apple‑peel appearance: challenging the current embryology. J Clin Neonatol, 2014; 3: 112–114.
- Alnosair AA, Naga MI, Abdulla MR, et Congenital duodenal atresia with ‘apple‑peel configuration’ of the small intestines and absent superior mesenteric artery: a case report and review of literature. J Pediatr Surg Case Rep, 2014; 2: 215–218.
- Zhu H, Gao R, Alganabi M, et al. Long‑term surgical outcomes of apple‑peel atresia. J Pediatr Surg, 2019; 54(12): 2503–2508.
- InsKirtane JM, Bhange SA, Nabi F, Shah V. Duodenal atresia with familial apple‑peel syndrome: case study with review of literature. BMJ Case Rep, 2019; 12(8): e230160.

