Intersecting Endocrine, Metabolic, and Dermatologic Complications in ESRD: A Case of Uremic Pruritus with Bleeding
Sai Prasad1, Shaily Agrawal2, Dr. Jay Nagda2,*, Dr. Darpan Kothia2, Dr. Deep Bavaria2, Deep Chahodiya3, Laxi Thaker3, Riti Aggarwal4 and Vidhi Parmar5
1S Nijalingappa Medical College, Nava Nagar, Bagalkot, Karnataka, India
2Shri M P Shah Government Medical College, Jamnagar, Gujarat, India
3Government Medical College, Surat, India
4Maulana Azad Medical College, Delhi, India
5D Y Patil Medical College, Navi Mumbai, India
Received Date: 30/10/2025; Published Date: 03/12/2025
*Corresponding author: Dr. Jay Nagda, Shri M P Shah Government Medical College, Jamnagar, Gujarat, India
Abstract
Chronic Kidney Disease-Associated Pruritus (CKD-aP), also known as uremic pruritus, is a distressing symptom observed in a significant proportion of patients with End-Stage Renal Disease (ESRD). Despite its high prevalence and substantial impact on quality of life, it remains underdiagnosed and inadequately treated. This case report presents a 75-year-old female with ESRD secondary to diabetic nephropathy, who developed severe generalised pruritus associated with bleeding from excoriated lesions, along with metabolic complications including anaemia, hypothyroidism, hypoalbuminemia, and peripheral oedema.
The patient had a longstanding history of hypertension and type 2 diabetes mellitus. Conservative CKD management had delayed dialysis initiation until worsening symptoms necessitated renal replacement therapy. She reported generalised itching over the limbs for one month, bleeding from scratched sites, and progressive lower limb swelling. Laboratory investigations revealed significant elevations in serum urea and creatinine, low haemoglobin and albumin, elevated TSH, and hypocalcemia. She was initiated on maintenance hemodialysis, gabapentin, antihistamines, topical emollients, corticosteroids, levothyroxine, and a renal-specific diet. These interventions led to improvement in her symptoms and functional status.
This case highlights the importance of early recognition of CKD-aP as a marker of worsening renal function. A multidisciplinary approach that incorporates dialysis optimisation, skin care, pharmacological management, and correction of hormonal and nutritional deficits is crucial. CKD-aP should be addressed proactively as part of comprehensive ESRD management to improve patient outcomes and quality of life.
Keywords: Chronic Kidney Disease–Associated Pruritus; End-Stage Renal Disease; Hemodialysis; Uremic Pruritus; Case Report
Introduction
Chronic Kidney Disease (CKD) affects over 10% of the global population and remains a Leading cause of morbidity and mortality, especially among the elderly. The progression of CKD to End-Stage Renal Disease (ESRD) is associated with a wide spectrum of complications involving cardiovascular, dermatological, and endocrine systems. One of the most distressing and underrecognized symptoms of ESRD is uremic pruritus, also known as CKD-Associated Pruritus (CKD-aP).
CKD-aP is estimated to affect approximately 40–50% of patients on maintenance hemodialysis, and its impact on quality of life is profound. It often leads to poor sleep, depression, impaired daily functioning, and in severe cases, skin trauma, secondary infections, and bleeding. Despite its high prevalence, the pathophysiology remains incompletely understood, with proposed mechanisms involving systemic inflammation, imbalance of opioidergic signalling, xerosis, and accumulation of uremic toxins [1,2].
This case report presents an elderly woman with ESRD secondary to diabetic nephropathy who experienced severe uremic pruritus with cutaneous bleeding. Her case underscores the need for early recognition and management of pruritus in CKD patients and highlights the therapeutic benefit of a comprehensive, multidisciplinary approach.
Presentation
A 75-year-old female presented with the following complaints:
- Severe generalised pruritus involving upper and lower limbs for 1 month
- Bleeding from scratching sites for 2 weeks
- Bilateral lower limb swelling for 1 week
- Difficulty walking due to pain, swelling, and weakness
The patient had a 10-year history of Stage 4 chronic kidney disease, secondary to diabetic nephropathy, managed initially with conservative therapy. Her medication regimen included Furosemide 80 mg once daily, Sevelamer 400 mg once daily, and intermittent darbepoetin injections (100 mcg/0.5 mL). She also had long-standing type 2 diabetes mellitus, initially treated with Metformin 850 mg and Glimepiride 1 mg once daily, later transitioned to Insulin Glargine at 0.2 units/kg subcutaneously once daily. Additionally, she had a history of hypertension, managed with a combination of Telmisartan and Hydrochlorothiazide 40 mg once daily.
Initiation of dialysis was deferred due to a preference for conservative management. In the days leading up to the presentation, she developed symptoms suggestive of hypothyroidism, including cold intolerance, lethargy, and dry skin.
Investigations:
Table 1: Vitals.
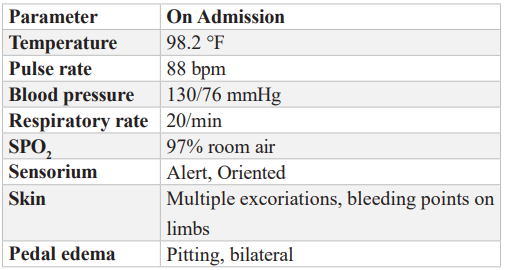
Table 2: Complete Blood Count.
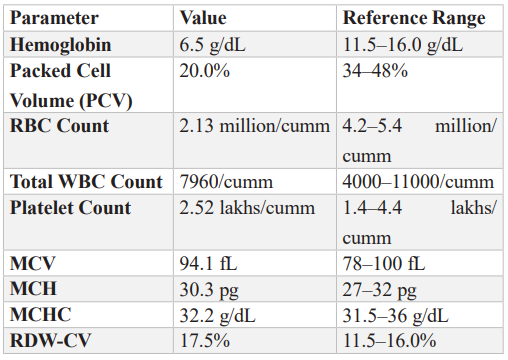
Table 3: Iron Profile.
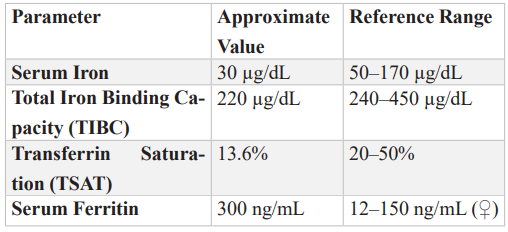
Table 4: Urinalysis Report.
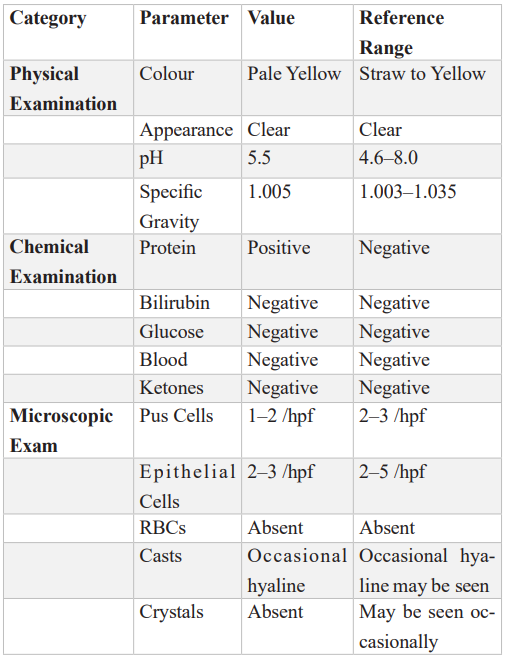
Table 5: Liver Profile.
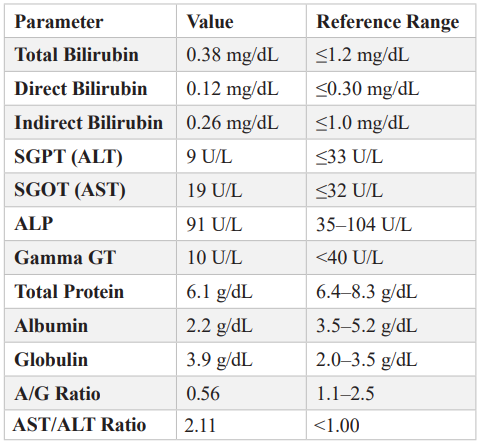
Table 6: Renal Profile.
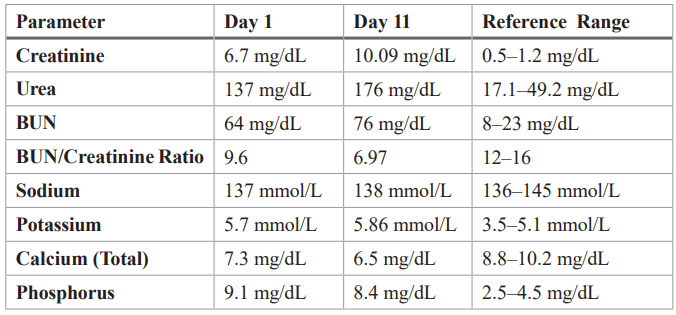
Table 7: ABG Analysis (Day 11).
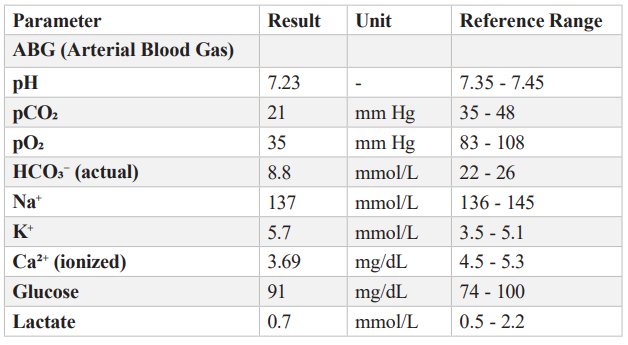
Table 8: Ultrasound Abdomen & Pelvis.
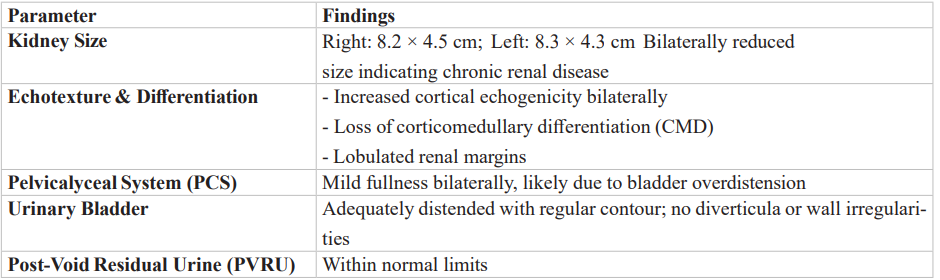
Impression:
Ultrasound findings are consistent with bilateral chronic renal parenchymal disease, corresponding to Stage 4 CKD. The post-void residual urine is within normal limits, indicating no significant lower urinary tract obstruction. Continued nephrology evaluation and monitoring are advised.
Table 9: Other Investigations.
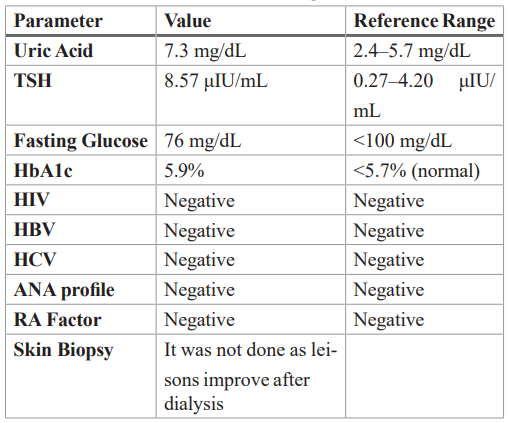
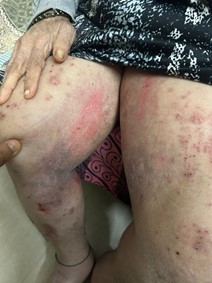
Figure 1: Bilateral thighs showing erythematous plaques with excoriations secondary to scratching in a patient with uremic pruritus. (Multiple excoriated lesions with erythematous plaques over thighs and shins).
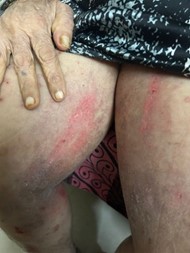
Figure 2: Close-up of inflamed plaques and linear scratch marks along the medial thighs. (Hyperpigmented and crusted papules from chronic scratching).
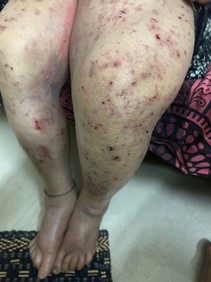
Figure 3: Both legs demonstrating hyperpigmented papules, crusting, and pitting pedal oedema—classic features of chronic CKD-associated pruritus. (Pitting pedal oedema is evident in the lower limbs).
Treatment And Follow-Up:
1. Dialysis Optimization
- The patient received maintenance haemodialysis sessions three times per week with close monitoring of fluid status, electrolytes, and anaemia parameters.
- Serum potassium levels were regularly assessed, and episodes of hyperkalemia were managed during dialysis as needed.
- Anaemia associated with chronic kidney disease was addressed with intermittent darbepoetin injections (100 mcg/0.5 mL) and transfusion of two units (600 mL) of packed red cells, administered as clinically indicated to improve haemoglobin levels and reduce fatigue.
2. Management of Uremic Pruritus and Skin Care
- Gabapentin 100 mg was administered orally at bedtime and titrated gradually up to 300 mg as tolerated for relief from pruritus.
- 10% urea with dexpanthenol cream was applied 3–4 times daily to restore skin hydration and barrier function.
- Hydroxyzine 25 mg was given at night to reduce itching and improve sleep
- 1% hydrocortisone cream was applied to lichenified and inflamed areas to reduce
- The patient was advised to keep their nails trimmed short and to use protective measures, such as gloves or mittens, at night to prevent trauma and bleeding.
3. Bleeding Control and Wound Care
- Gentle skin hygiene practices using mild cleansers were maintained to reduce the risk of infection.
- Excoriated and bleeding areas were covered with non-adherent sterile dressings to promote healing.
- NSAIDs were avoided due to the increased risk of
- The patient was closely monitored for signs of secondary infection, and prompt treatment was initiated when necessary.
4. Correction of Metabolic and Endocrine Abnormalities
- Levothyroxine 25 mcg was prescribed daily for hypothyroidism, with plans for gradual dose titration and TSH monitoring every 6–8 weeks.
- Calcitriol was given to manage secondary
- Hypocalcemia was corrected cautiously to avoid rapid calcium shifts that could precipitate vascular or soft tissue calcification.
5. Nutritional and Supportive Care
- The patient was advised on fluid and sodium restriction to aid fluid
- A renal-friendly diet low in potassium and phosphorus was
- Physiotherapy and gradual mobilisation were initiated once oedema and skin lesions
Patient Education and Follow-up
- The patient was educated on the importance of adherence to the dialysis schedule to prevent fluid overload and uremic complications.
- She was counselled on avoiding vigorous scratching and maintaining skin
- Regular follow-up visits were scheduled for clinical reassessment, laboratory monitoring, and adjustment of medications as required.
Discussion
Uremic pruritus, or CKD-Associated Pruritus (CKD-aP), is a distressing symptom seen in a significant proportion of patients with advanced chronic kidney disease, particularly those undergoing haemodialysis. While often overlooked in routine care, it poses a serious burden due to its effects on physical, psychological, and social well-being. The prevalence of CKD- aP ranges from 20% to 50%, yet it remains underdiagnosed, partly because many patients do not report it unless specifically asked. Its impact on the quality of life is profound, leading to sleep disturbances, depression, anxiety, and even increased mortality due to cardiovascular and infectious complications stemming from chronic inflammation and skin disruption [1,2].
The pathophysiology of uremic pruritus is complex and multifactorial. Contributing mechanisms include the accumulation of poorly cleared toxins, peripheral neuropathy, immune system dysregulation, xerosis (dry skin), secondary hyperparathyroidism, calcium- phosphate imbalance, mast cell activation, and altered expression of opioid receptors [3,4]. Notably, systemic inflammation and increased levels of interleukin-6 (IL-6) and C-Reactive Protein (CRP) are associated with greater itch severity, supporting the inflammatory basis of this condition [5].
Our case presents a 75-year-old woman with ESRD due to diabetic nephropathy who developed severe uremic pruritus with bleeding secondary to intense scratching. Pruritus with bleeding is a clinical marker of poor disease control, reflecting the severity and chronicity of her symptom burden. Her condition was further complicated by hypothyroidism, anaemia, and hypoalbuminemia, all of which contributed to fatigue, skin fragility, and impaired healing. Hypothyroidism can worsen pruritus. The delay in initiating dialysis likely worsened her symptom burden. Delayed dialysis worsens systemic complications. Her pruritus improved with a multifaceted approach—initiation of regular haemodialysis, administration of gabapentin (an alpha-2-delta ligand effective in neuropathic itch), antihistamines, and emollients. Gabapentin and skin care improve quality of life. This combination therapy reflects current best practices recommended in international nephrology guidelines [6,7].
Moreover, the patient’s hypothyroidism illustrates the overlap of metabolic and endocrine dysfunctions in ESRD. Hypothyroidism itself can exacerbate fatigue, cognitive dysfunction, and skin dryness. Her low albumin and protein levels indicated poor nutritional status, which required dietary intervention and monitoring. These overlapping morbidities in elderly CKD patients highlight the importance of a tailored, comprehensive approach [8].
Wound care was equally critical in this patient due to excoriations that risked superimposed bacterial infections. The use of non-adherent dressings, gentle skin cleansing, and corticosteroid creams minimised trauma and inflammation. Importantly, the patient was also educated on protective behaviours such as nail trimming and the use of gloves to prevent further skin damage during sleep. Biopsy was not done—while clinical improvement justified not doing a biopsy, histology could have clarified secondary dermatosis.
Multidisciplinary collaboration is indispensable in managing CKD-aP. Nephrologists must work in tandem with dermatologists, nutritionists, endocrinologists, mental health professionals, and physiotherapists. A patient-centric, integrative treatment plan is key not only to symptomatic control but also to improving dialysis adherence and overall prognosis [9].
This case reinforces that pruritus in CKD is not merely a benign dermatologic issue but a systemic, quality-of-life-altering condition. Proactive screening, patient education, and timely intervention are imperative. With an ageing global population and rising CKD prevalence, healthcare systems must prioritise the management of non-traditional CKD symptoms such as pruritus as part of comprehensive renal care [10].
Conclusion
This case highlights the clinical burden of uremic pruritus in elderly patients with ESRD and diabetes. Early recognition, dialysis initiation, and individualised treatment strategies are critical to alleviating symptoms and preventing complications such as infection, anaemia, and immobility.
Comprehensive management involving skin care, pharmacologic therapy, hormonal correction, and nutritional support can greatly enhance the quality of life for CKD patients.
Routine screening for pruritus and addressing it proactively in the treatment plan is essential to ensure patient-centred care in nephrology practice.
Data Availability: The data supporting the findings of this study are available from the corresponding author upon reasonable request.
Conflicts of Interest: The authors declare that there is no conflict of interest regarding the publication of this article.
Funding Statement: This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Acknowledgments: The authors would like to thank the medical and nursing staff who were involved in the patient’s care.
Ethical Approval and Consent to Publish: Written informed consent was obtained from the patient for publication of this case report and accompanying clinical images. All identifying information has been anonymised to protect the patient’s privacy. The study was conducted per the principles of the Declaration of Helsinki.
References
- Pisoni RL, Wikström B, Elder SJ, Akizawa T, Asano Y, Keen ML, et al. Pruritus in hemodialysis patients: International results from the Dialysis Outcomes and Practice Patterns Study (DOPPS). Nephrol Dial Transplant, 2006; 21(12): 3495–3503.
- Mettang T, Kremer Uremic pruritus. Kidney Int, 2015; 87(4): 685–691.
- Verduzco HA, Shirazian CKD-associated pruritus: new insights into diagnosis, pathogenesis, and management. Kidney Int Rep, 2020; 5(9): 1387–1402.
- Rayner HC, Larkina M, Wang M, Graham-Brown MPM, van der Veer SN, Robinson BM, et al. International comparisons of prevalence, awareness, and treatment of pruritus in people on hemodialysis. Clin J Am Soc Nephrol, 2017; 12(12): 2000–2007.
- Combs SA, Teixeira JP, Germain Pruritus in kidney disease. Semin Nephrol, 2015; 35(4): 383–391.
- Simonsen E, Komenda P, Lerner B, Askin N, Bohm C, Shaw J, et Treatment of uremic pruritus: a systematic review. Am J Kidney Dis, 2017; 70(5): 638–655.
- Mathur VS, Lindberg J, Germain M, Block G, Tumlin J, Smith A longitudinal study of uremic pruritus in hemodialysis patients. Clin J Am Soc Nephrol, 2010; 5(8): 1410–1419.
- Ramkumar N, Bhandari Managing endocrine complications in chronic kidney disease. Best Pract Res Clin Endocrinol Metab, 2019; 33(4): 101313.
- Shirazian S, Aina O, Park Y, Chowdhury N, Leger K, Hou L, et Chronic kidney disease-associated pruritus: impact on quality of life and current management challenges. Int J Nephrol Renovasc Dis, 2017; 10: 1126.
- Nistor I, Rees J, Sola H, Schmid H, Goldsmith D, Massy ZA, et al. Pruritus management in patients with CKD: a systematic review of randomised controlled trials. Am J Kidney Dis, 2016; 68(3): 353–363.

