Paget’s Disease of the Breast After Segmentectomy and Radiotherapy
Diana Carolina Vásconez Celis1,*, Paulina Gabriela Pacheco Buñay1, Josselyn Nicole Valarezo Sanchez1, Bianca Fantin de Souza1, Lucas Lazzari2 and Paulo Ricardo Martins Souza3
1Dermatology Resident, Department of Dermatology, Santa Casa de Misericórdia de Porto Alegre, Porto Alegre, Brazil
2Second-year Pathology Resident, Santa Casa de Misericórdia de Porto Alegre / Universidade Federal de Ciências da Saúde de Porto Alegre (UFCSPA)
3Dermatologist, Department of Dermatology, Santa Casa de Misericórdia de Porto Alegre
Received Date: 28/10/2025; Published Date: 01/12/2025
*Corresponding author: Diana Carolina Vasconez Celis, Department of Dermatology, Santa Casa de Misericórdia de Porto Alegre Hospital, Rua Professor Annes Dias, 295, Centro Histórico, Porto Alegre, RS, 90020-090, Brazil
Abstract
Paget’s Disease of the Breast (PDB) is a rare malignancy that often presents as a unilateral eczematous lesion of the nipple-areolar complex, mimicking benign dermatoses and leading to diagnostic delays. Skin biopsy is crucial to distinguish PDB from common conditions and ensure timely diagnosis. We report the case of a 52-year-old patient previously treated for HER2+ carcinoma who developed a persistent nipple ulcer initially misdiagnosed as radiodermatitis, later confirmed as PDB by biopsy.
Keywords: Paget’s disease of the breast; Dermatology; Differential diagnosis; Case report
Introduction
Paget’s disease of the breast (PDB), described by Sir James Paget in 1874, is a rare presentation of breast cancer, accounting for approximately 1–3% of cases and usually associated with an underlying ductal carcinoma in situ or invasive carcinoma [1,2].
PDB affects the nipple–areolar complex, clinically manifesting as a chronic eczematous, scaly, or ulcerated lesion with irregular borders, and sometimes with pigmentation. It may be limited to the nipple, extend to the areola, or even involve the adjacent skin. This nonspecific clinical pattern explains why the diagnosis is often delayed, especially in patients with a history of breast-conserving surgery and radiotherapy, in whom nipple changes are often initially attributed to benign postoperative alterations or secondary effects of radiation [3,4].
The differential diagnosis also includes other cutaneous neoplasms with intraepidermal pagetoid spread, reinforcing the need to perform a skin biopsy in persistent lesions in this region [5].
The present report describes a case of PDB in a patient with a history of HER2+ carcinoma treated with breast-conserving surgery and radiotherapy, initially interpreted as radiodermatitis.
Case Presentation
A 52-year-old female patient with a history of right breast invasive carcinoma (HER2+, cT4, cN0), diagnosed in 2022, was treated with neoadjuvant chemotherapy, segmentectomy with sentinel lymph node biopsy (ypTis, ypN0), trastuzumab, and adjuvant radiotherapy. After completing treatment, she remained free of signs of recurrence.
In January 2025, she presented to the dermatology service with persistent irritation of the right nipple, initially attributed to radiodermatitis. On physical examination, erythema, induration, and local friability were observed, in addition to superficial ulceration. The diagnostic hypotheses included radiodermatitis and Paget’s disease (Figure 1).
An incisional biopsy of the nipple revealed intraepithelial neoplasia with a pagetoid pattern, composed of clear vacuolated cells, consistent with Paget’s disease, associated with a focus of adjacent spongiotic dermatitis (Figure 2).
Immunohistochemistry showed positivity for CK7 and HER2 (2+), negativity for hormonal receptors and melanocytic markers, a profile consistent with Paget’s disease of the breast (Figure 3).
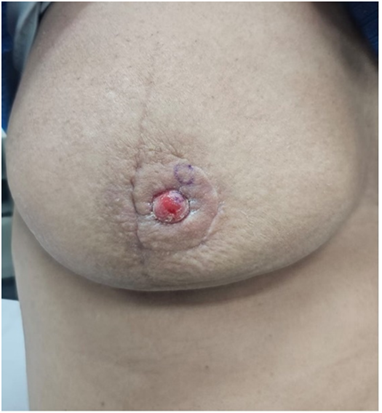
Figure 1: Nipple with erythema, hardened area, and ulceration.
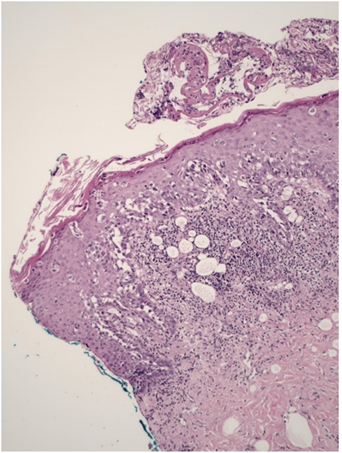
Figure 2: Anatomopathological examination (H&E, 100x): Intraepithelial proliferation of a pagetoid pattern consisting of large cells with clear cytoplasm, pleomorphic nucleus, and prominent nucleolus, compatible with paget's cells.
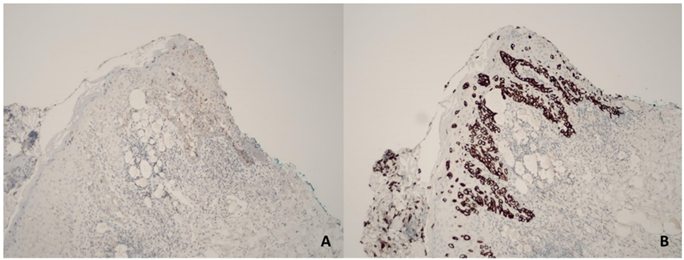
Figure 3: Immunohistochemistry: A) HER-2 positive (2+). B) CK7 positive.
Discussion
Paget’s Disease of the Breast (PDB) is a rare condition that accounts for 0.7% to 4.3% of all breast cancers and is strongly associated with underlying ductal carcinoma in situ or invasive carcinoma [6].
Clinically, PDB is characterized by an erythematous, scaly, or ulcerated plaque of the nipple–areolar complex, usually unilateral, and may present with crusting, erosions, or irregular pigmentation. However, this pattern mimics several benign dermatoses such as contact eczema and psoriasis, as well as cutaneous neoplasms such as squamous cell carcinoma or melanoma in cases with pigmentation [6–8].
The presence of intraepidermal Paget cells with clear cytoplasm and pleomorphic nuclei is the characteristic histopathological finding. Immunohistochemistry is essential to differentiate PDB from other pagetoid entities such as malignant melanoma or squamous cell carcinoma in situ. Markers such as CK7, EMA, CEA, GCDFP-15, and HER2 are typically positive in Paget cells [7].
Skin biopsy of persistent dermatoses in the nipple region is the main diagnostic method, as imaging studies such as mammography or ultrasonography may be normal in up to half of patients with PDB.
Conclusion
In summary, PDB remains a diagnostic challenge due to its ability to mimic common benign conditions. This case highlights the importance of a multidisciplinary approach but especially underscores the crucial role of dermatology in raising suspicion and confirming the diagnosis, thereby avoiding delays that may compromise the prognosis.
Author Contributions: All authors made substantial contributions to the conception and design of the study, data acquisition, analysis, and interpretation. Each author participated in drafting the article and/or critically revising it for important intellectual content, and all approved the final version of the manuscript prior to submission.
Conflicts of Interest: The authors declare that they have no conflicts of interest related to the publication of this manuscript.
Grant Information: The authors received no specific funding for this work
Acknowledgements: The authors express their sincere gratitude to the staff of the Dermatology and Pathology Departments at Santa Casa de Misericórdia de Porto Alegre Hospital for their valuable guidance, academic support, and collaboration in the preparation of this case report.
References
- Plastaras JP, Harris EE, Solin LJ. Paget’s disease of the nipple as local recurrence after breast-conservation treatment for early-stage breast cancer. Clin Breast Cancer, 2005; 6(4): 349–53. http://dx.doi.org/10.3816/CBC.2005.n.039
- Grewal IS, Rajagopal T. Studying the Presentation of Paget Disease of the Breast. Cureus, 2023; 15(6): 2–5.
- Kar H, Cin N, Tavusbay C, Yemez K, Peker Y, Sarı AA, et al. Paget’s disease of the breast presenting as a local recurrence following breast-conserving surgery. Erciyes Tip Derg, 2016; 38(1): 29–31.
- Pu Q, Zhao Q, Gao D. Local recurrence of mammary Paget’s disease after nipple-sparing mastectomy and implant breast reconstruction: a case report and literature review. World J Surg Oncol, 2022; 20(1): 1–7. https://doi.org/10.1186/s12957-022-02746-4
- Karakas C. Paget′s disease of the breast. J Carcinog, 2011; 10(1): 31.
- Kanitakis J. Mammary and extramammary Paget’s disease. J Eur Acad Dermatology Venereol, 2007; 21(5): 581–590.
- Zengin HB, Tan PH, Liu R, Smoller BR. ‘Eczematous’ dermatitis of the nipple: clinical and histopathological differential diagnosis of Paget disease. Pathology, 2024; 56(3): 300–312.
- Scott-Emuakpor R, Reza-Soltani S, Altaf S, NR K, Kołodziej F, Sil-Zavaleta S, et al. Mammary Paget’s Disease Mimicking Benign and Malignant Dermatological Conditions: Clinical Challenges and Diagnostic Considerations. Cureus, 2024; 16(7): 1–16.

