Pulmonary Vein Thrombosis: A Rare and Underdiagnosed Condition
Dehayni Fariss*, Yassine Kassab Alia, Neftah Ismail, Messaoud Ola, Iraqi Houssaini Zaynab, Jroundi Laila, El Aoufir Omar
Department of Emergency Radiology, Ibn Sina Hospital, Faculty of Medicine and Pharmacy of Rabat, Morocco
Received Date: 22/09/2025; Published Date: 24/10/2025
*Corresponding author: Dehayni Fariss, Faculty of Medicine and Pharmacy of Rabat, Morocco
Case Description
A 74-year-old woman was admitted in shock. Past medical history includes end-stage renal disease on chronic hemodialysis and atrial fibrillation on acenocoumarol (Sintrom). She presented with failed hemodialysis due to hemodynamic instability, hypotension (80/40 mmHg), tachycardia (120 bpm), prolonged bed rest, and chest pain. Echocardiography revealed right ventricular dilatation with paradoxical septal motion.
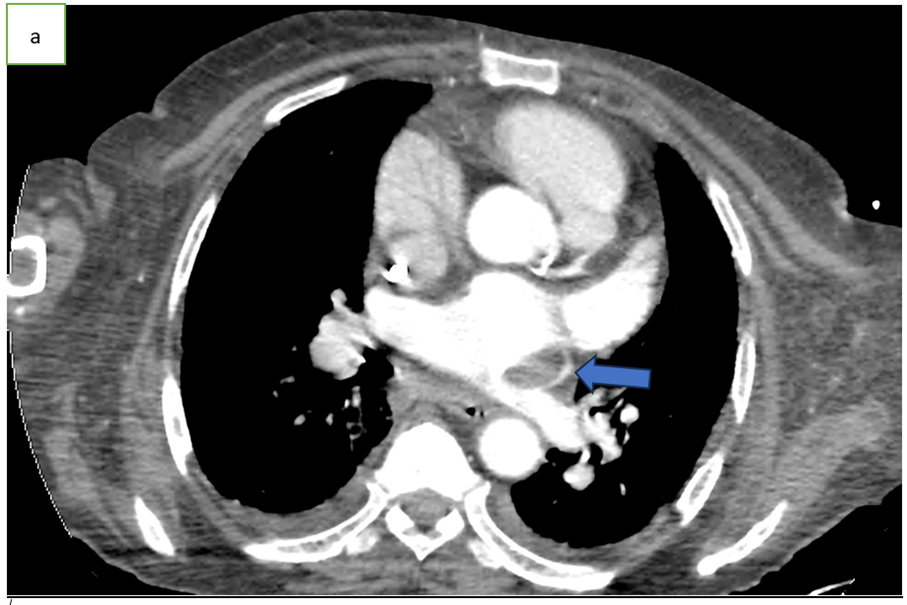
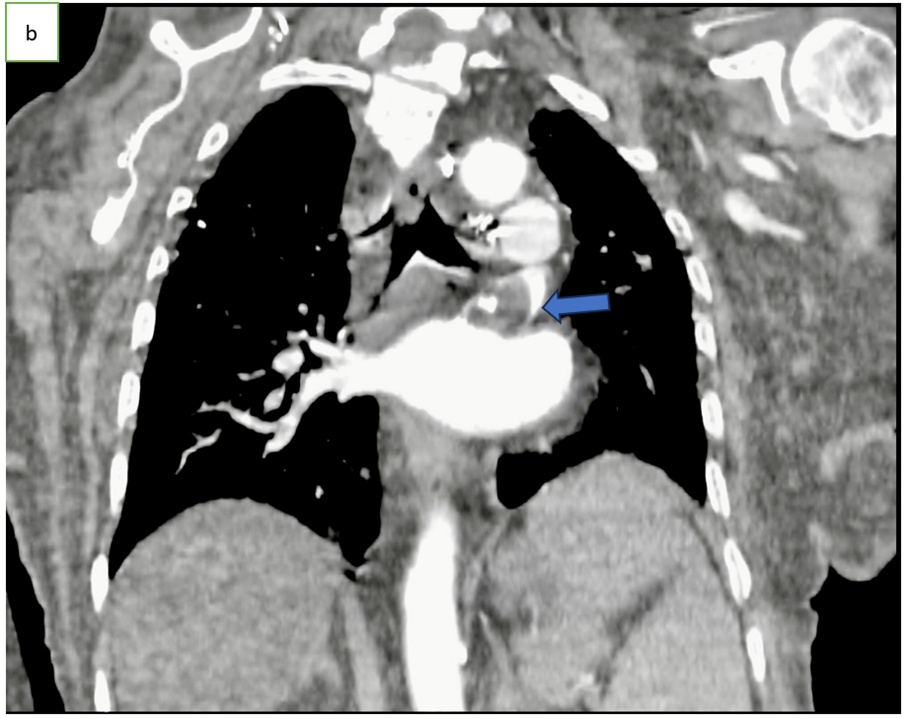
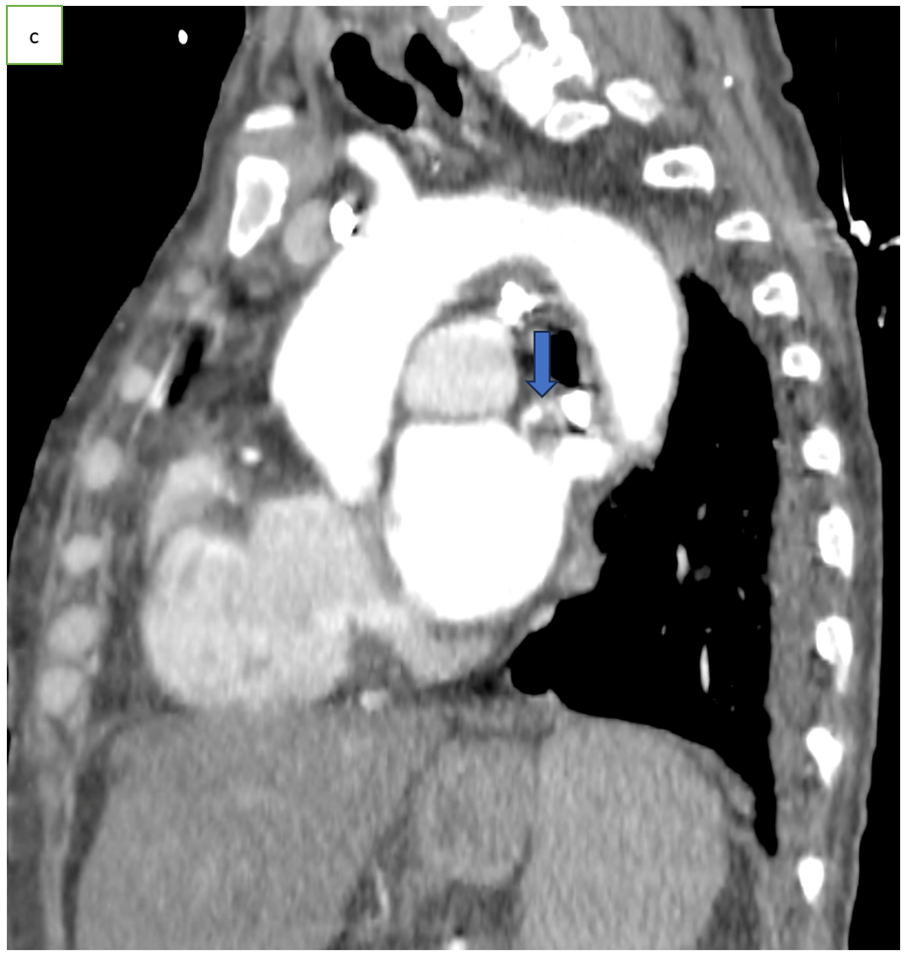
Figure 1: Axial CT scan angiography (a), coronal (b) and sagittal (c) reconstruction, showing an endoluminal thrombi in the pulmonary vein (arrow).
Discussion
Pulmonary Vein Thrombosis (PVT) is rare, often underdiagnosed, yet potentially life-threatening [1].
Its causes can be divided into postoperative factors—such as lobectomy, lung transplantation, radiofrequency catheter ablation, and arteriovenous malformation—and non-postoperative factors, including primary or secondary lung cancer, metastases, chest trauma, hiatal hernia, pulmonary aspergillosis, and omalizumab therapy [2,3]. Some cases remain idiopathic, often in the context of hemoglobinopathies [1-3].
Pathophysiology
After surgery, PVT may develop due to turbulent blood flow or stasis in the residual vein stump [2]. In cancer-related cases, the mechanism is less clear but may involve tumor extension into the vein, endothelial injury from tumor invasion, or a hypercoagulable state [1]. Increased pulmonary venous pressure can lead to compensatory pulmonary arterial vasoconstriction, raising pulmonary artery pressure and causing right ventricular expansion [3].
Clinical presentation
Symptoms are non-specific—dyspnea, cough, and hemoptysis—often mimicking pulmonary embolism [1,3]. Hemodynamic signs are also non-specific, and the condition may be asymptomatic, especially in older patients [1,2].
Diagnosis
Chest CT angiography is the preferred imaging method, typically showing a well-defined, hypodense endoluminal thrombus in a pulmonary vein [1,3], outlined by contrast but not enhancing after injection [1].
Transthoracic or transesophageal echocardiography can visualize atrial thrombi [3] and is particularly useful for postoperative follow-up [3].
MRI helps distinguish bland from tumor thrombi: bland thrombi show high T1/T2 signal in the acute phase and low T2 (“flow void”) in chronic stages, without enhancement. Tumor thrombi may show vessel wall invasion, restricted diffusion, and post-contrast enhancement [1].
Complications
Delayed diagnosis or treatment can lead to severe outcomes: pulmonary hypertension with shock, pulmonary infarction, edema, fibrosis, massive hemoptysis, renal infarction, or ischemic stroke from embolization [1, 3].
Management
There is no clear consensus on treatment [1, 3]. In most cases, anticoagulation is given unless bleeding is present.
For postoperative thrombi, antibiotics plus anticoagulation are recommended, with thrombectomy in severe cases; spontaneous resolution is possible.
For tumor thrombi, anticoagulation is combined with tumor-specific therapy, and surgical resection may be considered if the tumor is operable [1].
References
- Chaaya G, Vishnubhotla P. Pulmonary Vein Thrombosis: A Recent Systematic Review. Cureus, 2017; 9(1): e993. doi: 10.7759/cureus.993.
- Paul D Stein, James E Denier, Lawrence R Goodman, Fadi Matta, Mary J. Hughes, Pulmonary vein thrombosis in patients with medical risk factors, Radiology Case Reports, 2018; 13(6): Pages 1170-1173. https://doi.org/10.1016/j.radcr.2018.07.031.
- Muhammad Asim Rana, Nicholas Tilbury, Yashwant Kumar, Habib Ahmad, Kamal Naser, Ahmed F Mady, et al. Idiopathic Pulmonary Vein Thrombus Extending into Left Atrium: A Case Report and Review of the Literature, 2016. https://doi.org/10.1155/2016/3528393.

