The Use of Ultrasound Guided Stellate Ganglion Nerve Block to Treat Refractory Ventricular Arrhythmias During Cardiac Arrest: A Case Series
Matthew Berger1,*, Matthew Tripod1, Mark Magee2 and Ryan Gibbons2
1Capital Health, Department of Emergency Medicine, Pennington, New Jersey, United States
2Lewis Katz School of Medicine at Temple University, Department of Emergency Medicine, Philadelphia, Pennsylvania, United States
Received Date: 07/10/2025; Published Date: 17/10/2025
*Corresponding author: Matthew Berger, M.D, Capital Health, Department of Emergency Medicine, Pennington, New Jersey, United States
Abstract
Electrical Storm (ES) refers to ventricular arrhythmia that occurs three or more times in a 24-hour period. Patients in cardiac arrest with ES that is refractory to defibrillation and typical medications used in resuscitation protocols present a challenge. Many interventions have been proposed to restore a normal cardiac rhythm in these situations. There is a paucity of quality evidence to clearly support any of them. The stellate ganglion nerve block is a procedure that has been shown to be effective in abating refractory ventricular rhythms, however, existing literature largely excludes patients in cardiac arrest. The procedure can be performed at the bedside by any physician proficient with point-of-care ultrasound and may be an important tool in treating Refractory Ventricular Arrhythmia (RVA) in cardiac arrest patients. We present three cases in which an ultrasound guided stellate ganglion nerve block performed at the bedside in the Emergency Department (ED) successfully terminated RVA in patients in cardiac arrest.
Keywords: Stellate Ganglion; Cardiac Arrest; POCUS; Ventricular Fibrillation
Introduction
Advanced Cardiac Life Support (ACLS) protocols provide a framework for physicians to approach and treat patients in cardiac arrest. Emergency physicians, however, need to be resuscitation experts, and be familiar with therapeutic options for unique circumstances that are not addressed by the basic algorithm. One such circumstance is Ventricular Fibrillation (VF) or pulseless Ventricular Tachycardia (VT) that does not respond to defibrillation attempts or antidysrhythmic medications. This situation is often termed “electrical storm” and is defined by three or more episodes of VT or VF in a 24-hour period [1]. It is thought that ES is due to unstable cardiac myocytes resulting from ischemia and myocyte damage and perpetuated by a surge of catecholamines [2].
Multiple interventions have been proposed to combat RVA, including double sequential defibrillation, beta blockers and early initiation of extracorporeal membrane oxygenation (ECMO) [3]. Recently, the stellate ganglion nerve block has emerged as a possible intervention for RVA in cardiac arrest. Here we present three cases of patients in cardiac arrest with RVA that were treated with an ultrasound guided stellate ganglion nerve block in the Emergency Department (ED).
Case Reports
Case 1:
A 53-year-old female was brought into the ED in cardiac arrest. The patient had reportedly been found in a car which had drifted off the road. There was no significant trauma. The patient apparently went into cardiac arrest while driving. She was found to be in VF on EMS arrival, and ACLS was initiated. Prehospital care included nine defibrillation attempts, six 1mg doses of epinephrine intravenous, 450mg total of amiodarone and supraglottic airway placement. ACLS was continued in the ED, and the patient received multiple additional defibrillations attempts as well as multiple doses of 1mg of epinephrine, magnesium sulfate, calcium chloride and sodium bicarbonate. The patient persisted in pulseless VF despite all interventions. Additional interventions were attempted including double sequential defibrillation as well as an esmolol bolus and continuous infusion, however they were ineffective at terminating VF. The resuscitation time totaled nearly one hour. The patient was deemed not to be a candidate for ECMO. An ultrasound guided left Stellate Ganglion Block (SGB) was performed using a lateral approach and approximately 5ml of 2% lidocaine was injected around the stellate ganglion. Shortly thereafter the patient achieved Return of Spontaneous Circulation (ROSC) with a stable blood pressure and was placed on an amiodarone continuous infusion. A 12 lead ECG showed ST segment elevation in a VR and ST depressions in multiple leads. The patient was taken emergently for cardiac catheterization on esmolol and amiodarone infusions.
Catheterization showed an acute plaque rupture in the mid left anterior descending coronary artery. Blood flow was sufficient through the artery and no intervention was indicated. The patient began to have worsened cardiac output and an intra-aortic balloon pump was placed. She was admitted to the cardiac Intensive Care Unit (ICU). Over the subsequent days the patient had progressive loss of brain stem reflexes and multisystem organ failure. The patient’s family elected to withdraw care five days after admission.
Case 2:
A 66-year-old male with an extensive medical history including coronary artery disease requiring a three-vessel bypass, ischemic stroke, diabetes, sick sinus syndrome requiring a dual chamber pacemaker and end stage renal disease requiring dialysis presented to the ED from the dialysis unit in cardiac arrest. Per family, the patient had not been feeling well for a few days and had missed his previous dialysis session. The patient became unresponsive during his dialysis session, and a rapid response was called. Upon arrival of emergency staff, the patient was pulseless and receiving CPR. On first pulse check in the ED the patient was first noted to be asystolic. Calcium chloride 1g and sodium bicarbonate 50 mEq were given in addition to repeat doses of epinephrine 1mg. On subsequent pulse checks the patient was noted to be in VF. This persisted despite continued ACLS as well as repeated doses of epinephrine, calcium, sodium bicarbonate, magnesium, amiodarone and lidocaine. Esmolol was also added after more than 30 minutes of VF. After several defibrillation attempts and multiple double sequential defibrillations attempts the patient remained pulseless in VF. SGB was performed. Under ultrasound guidance in the left lateral approach, approximately 5ml of 2% lidocaine was injected around the stellate ganglion. ROSC was achieved within one minute of injection. The patient was hypotensive and had several brief repeat cardiac arrests, alternating between pulseless electrical activity and VF. He received continued repeat doses of calcium in addition to epinephrine and sodium bicarbonate and was placed on a continuous esmolol infusion. Sustained ROSC was achieved after approximately an hour and a half of resuscitation. Ultimately, the family decided to withdraw care and the patient was terminally extubated.
Case 3:
A 60-year-old male with a history of cocaine use presented to the ED by private vehicle in cardiac arrest. Reportedly, the patient had been riding in the passenger seat of the car when he suddenly had an episode of gasping breaths and became unresponsive. The patient was driven approximately 20 minutes to the hospital, during which time CPR was not performed. On arrival the patient was noted to be in VF. During the ensuing resuscitation the patient received multiple doses of epinephrine 1 mg as well as amiodarone totaling 450 mg, sodium bicarbonate 50 mEQ and calcium chloride 1g. The patient continued in VF at subsequent pulse checks and esmolol bolus was administered without effect. An ultrasound guided left SGB was performed using the lateral approach. At the next pulse check the patient was noted to have pulseless electrical activity (PEA) and ACLS protocol was continued. The patient was deemed to not be a candidate for ECMO. The patient remained in PEA and after a 34-minute resuscitation, efforts were terminated due to futility.
Discussion
The use of percutaneous stellate ganglion nerve block for the treatment of refractory cardiac arrhythmia was first described in the 1970s [4]. While not novel, the technique has only gained traction as a viable treatment option in the ED recently, which in part can be attributed to the widespread adoption of point-of-care ultrasound (POCUS) in the specialty. The STAR study (2024) and another study by Chouairi et al. (2024) are among several observational studies published recently that demonstrate significant reduction in ventricular arrhythmia in patients after the stellate ganglion block is performed [5,6]. Additionally, a 2024 meta-analysis by Motazedian et al. that included 15 observational studies also concluded that SGB was effective in reducing ventricular arrhythmia in patients with ES [7]. These studies, however, include very few patients in cardiac arrest and are focused on admitted patients rather than ED patients. Unfortunately, there are no published studies which look at the efficacy of SGB in cardiac arrest patients in the ED. The current literature is limited to case reports regarding this patient population.
The rationale for the use of SGB for RVA lies in decreasing sympathetic effects on the heart. The stellate ganglion is located lateral to the vertebral bodies of C6-7. It lies anterior to the longus colli muscle and in close proximity to the internal jugular vein and common carotid artery (Figure 1). The stellate ganglion provides the majority of the sympathetic input to the ventricles [7]. Cardiac arrest and shocks cause myocyte injury resulting in an endogenous catecholamine surge. This coupled with repeated doses of epinephrine increases the likelihood of repeated arrhythmia [2,6]. By interrupting impulses between the stellate ganglion and the heart, sympathetic tone and corresponding arrhythmic effects are decreased, providing a more favorable environment for sustained normal rhythm.
SGB is within the scope of any emergency physician proficient in the use of POCUS, however the blocks described here were performed by ultrasound fellows. Continuous visualization of the needle (Figure 2) is necessary especially during ongoing compressions in order to decrease the chance of complication. Multiple studies have shown ultrasound guidance for SGB improves efficiency and precision and allows for a smaller injection volume [8-10]. 5mL of 2% lidocaine was injected in each case presented here (Figure 3).
In all cases that we present, RVA was effectively terminated immediately after SGB was performed. In case three, ROSC was not achieved, however, the patient did convert from VF to PEA. While each case ultimately had an unfavorable outcome, all patients had extremely poor prognosis due to prolonged resuscitation efforts. This does not reflect the efficacy of SGB as a treatment for ES. The use of SGB earlier in the resuscitation as soon as ES is identified may result in more favorable outcomes. More research that focuses on ED patients in cardiac arrest with ES is needed to draw reliable conclusions.
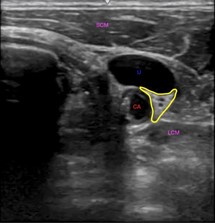
Figure 1: Transverse ultrasound image of the lateral neck showing the stellate ganglion outlined in yellow, the carotid artery (CA) labeled in red, the internal jugular vein (IJ), labeled in blue and the longus colli (LCM) and sternocleidomastoid (SCM) muscles labeled in purple.
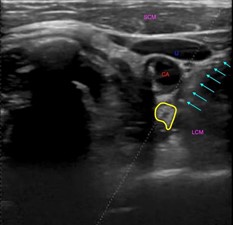
Figure 2: Transverse ultrasound image of the lateral neck showing a needle approaching the stellate ganglion in the long axis (teal arrows). Carotid artery (CA), internal jugular vein (IJ), longus colli muscle (LCM) and sternocleidomastoid muscle (SCM) again labeled. Stellate ganglion outlined in yellow.
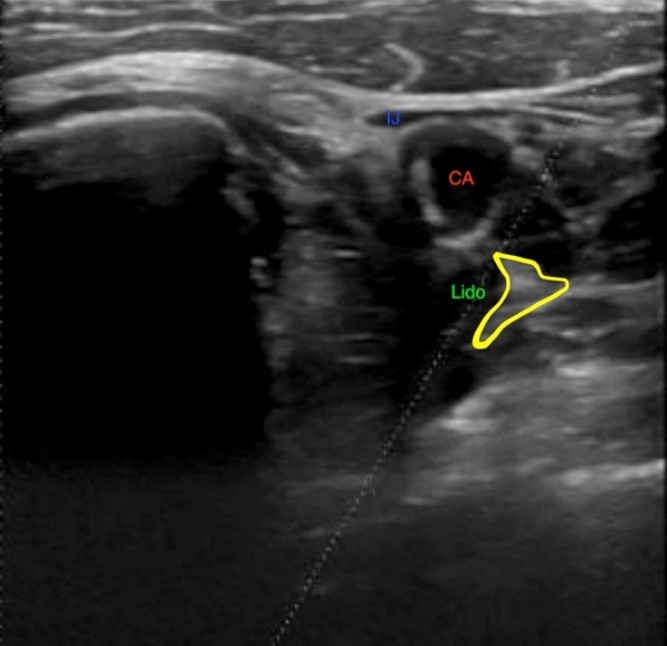
Figure 3: Transverse ultrasound image of the lateral neck showing hydrodissection of surrounding structures away from the stellate ganglion (outlined in yellow) after injection of lidocaine (Lido in green). Carotid artery (CA) and internal jugular vein (IJ) again labeled.
Conclusion
ED patients in cardiac arrest with RVA present significant challenges to physicians. In this case series, the ultrasound guided SGB effectively terminated RVA in each instance. Further studies are needed in this patient population to determine the efficacy of SGB and how to incorporate it into cardiac arrest resuscitation.
Author Contributions:
Matthew Berger: Manuscript draft
Matthew Tripod: Manuscript revision
Mark Magee: Manuscript revision
Ryan Gibbons: Manuscript revision
Conflicts of Interest: All authors report no conflicts of interest
Grants: No financial support
References
- Callipari C, Stone M, John D, Keceli M, Giles RA. Intra-Cardiac Arrest Use of Stellate Ganglion Block for Refractory Ventricular Tachycardia. J Emerg Med, 2023; 64(5): 628-634. doi: 10.1016/j.jemermed.2023.03.051.
- Nair A, Bhoi S, Choudhary Y. Cease the storm - Successful stellate ganglion block in terminating refractory electrical storm. Am J Emerg Med, 2024; 81: 160.e3-160.e7. doi: 10.1016/j.ajem.2024.03.003.
- Bell SM, Lam DH, Kearney K, Hira RS. Management of Refractory Ventricular Fibrillation (Prehospital and Emergency Department). Cardiol Clin, 2018; 36(3): 395-408. doi: 10.1016/j.ccl.2018.03.007.
- Grossman MA. Cardiac arrhythmias in acute central nervous system disease. Successful management with stellate ganglion block. Arch Intern Med, 1976; 136(2): 203-207.
- Savastano S, Baldi E, Compagnoni S, et al. Electrical storm treatment by percutaneous stellate ganglion block: the STAR study. Eur Heart J, 2024; 45(10): 823-833. doi: 10.1093/eurheartj/ehae021.
- Chouairi F, Rajkumar K, Benak A, Qadri Y, Piccini JP, Mathew J, et al. A Multicenter Study of Stellate Ganglion Block as a Temporizing Treatment for Refractory Ventricular Arrhythmias. JACC Clin Electrophysiol, 2024; 10(4): 750-758. doi: 10.1016/j.jacep.2023.12.012.
- Mohd Y, Kumar A, Sheikh I, Fatima A, Bhoi S, Jamshed N, et al. Calming the storm - Stellate ganglion block in refractory ventricular arrhythmia in the emergency department. Am J Emerg Med, 2021; 45: 685.e5-685.e8. doi: 10.1016/j.ajem.2020.12.063.
- Narouze S. Ultrasound-guided stellate ganglion block: safety and efficacy. Current Pain Headache Reports, 2014; 18: 424.
- Ghai A, Kaushik T, Kundu ZS, Wadhera S, Wadhera R. Evaluation of new approach to ultrasound guided stellate ganglion block. Saudi J Anaesth, 2016; 10(2): 161-167. doi: 10.4103/1658-354X.168815.
- Kapral S, Krafft P, Gosch M, Fleischmann D, Weinstabl C. Ultrasound imaging for stellate ganglion block: direct visualization of puncture site and local anesthetic spread. A pilot study. Reg Anesth, 1995; 20(4): 323-328.

