The Effect of an Inspiratory Muscle Training Program on Functionality in Adolescents and Young Adults with Cerebral Palsy: A Randomized Controlled Trial
Afrodite Evangelodimou1,*, Emmanouil Skordilis1, Eirini Grammatopoulou2 and Konstantinos Karteroliotis1
1Department of Physical Education and Sports Science, National and Kapodistrian University of Athens, Dafni Athens, Greece
2Department of Physiotherapy, University of West Attica, Ag. Spyridonos str, Egaleo, Postal code 12243, Athens
Received Date: 24/09/2025; Published Date: 09/10/2025
*Corresponding author: Afrodite Evangelodimou, PhD candidate, Department of Physical Education and Sports Science, National and Kapodistrian University of Athens. 70, Sarantaporou str, Peristeri, 12131, Athens
Abstract
Inspiratory Muscle Training (IMT) may improve respiratory muscle strength, pulmonary function and functional exercise capacity and quality of life in children with Cerebral Palsy (CP). The present study was designed to evaluate the effect of an IMT on functional capacity in adolescents and young adults with CP. For this purpose, an 8- week controlled experimental trial was conducted. 42 adolescents and young adults with CP from a special education school and a special education center volunteered to the study and were randomly assigned in two groups (IMT and control). The study was completed by 37 participants: a) 20 participants followed an 8-week IMT, at 30% of maximal inspiratory pressure (MIP), four sessions per week, for 20 minutes per day and participated in the standardized physiotherapy program of the special education school or center, and b) 17 participants followed the standardized physiotherapy program. The main outcome measure was the 6-minute walking distance test (6MWT) and secondary outcome measures were: 1-minute walking distance test (1MWT), 5 repetitions sit-to- stand test (STS), 5-stair timed-up-and-down test (TUDS), Berg Balance Scale (BBS), World Health Organization-Disability Assessment Schedule 2.0 (WHODAS 2.0), respiratory muscle strength [MIP and maximal expiratory pressure (MEP)] and pulmonary function [forced expiratory volume in 1 second % predicted (FEV1%pred), forced vital capacity % predicted (FVC%pred) and peak expiratory flow % predicted (PEF%pred)]. The 2 × 3 repeated measures ANOVA revealed a significant interaction effect between intervention and time in 6MWT (p <0.001), 1MWT (p <0.001), STS (p<0.001), TUDS (p <0.001), WHODAS (p <0.001), MIP (p <0.001), MEP (p <0.001),
FEV1%pred (p <0.001), FVC%pred (p =0.003) and PEF%pred (p =0.023). In conclusion, IMT improved functionality, respiratory muscle strength, and pulmonary function in adolescents and young adults with CP, supporting the effectiveness of the treatment in this population.
Keywords: Inspiratory muscle training; Functionality; Cerebral palsy; Adolescents; Young adults
Introduction
Cerebral Palsy (CP) refers to a group of permanent disorders in the developing brain of the fetus or newborn, involving changes in the biomechanics of all parts of the human body with consequences on the development of posture and movement, resulting in significant limitations in functionality and quality of life [1,2]. The weakness in the respiratory muscles observed in CP causes changes in the biomechanics of the chest resulting in modification of the length-force relationship of the diaphragm [3]. The diaphragm has a dual function (ventilation and posture) with an essential role in the maintenance of lumbar spine stability, as it has a direct anatomical connection to the spine via its crural fiber [4].
Children with CP compared to typically developing peers have shown lower inspiratory muscle strength and aerobic capacity (six-minute walk test and the Shuttle test), essential characteristics to perform energy-efficient walking and functional activities [5-10]. Children and adolescents with CP are at risk for respiratory problems and parenchymal lung diseases [11-13], which often result in hospital admission or deaths [14]. Respiratory muscle strength and lung function in children with CP are positively correlated with their ability levels to perform daily self-care and social functions [9,15]. Respiratory function is declining as the levels of the Gross Motor Function Classification System (GMFCS) progress [16]. Inspiratory muscle training (IMT) seems to improve trunk control, respiratory muscle strength, daily living activities, functional exercise capacity and quality of life in children with CP [1] as well as pulmonary function such as forced expiratory volume in 1 second (FEV1), forced vital capacity (FVC), and peak expiratory flow (PEF) [17,18]. IMT also seems to improve FEV1 and PEF in adults with CP [11]. On the contrary, some studies have shown no IMT impact on mobility capacity, balance, or 6MWT in children and adolescents with CP [16,19] resulting in no significant changes after inspiratory and balance training program.
Based on the above conflicting findings, the primary objective of the study is to shed more light in the field and investigate the effect of an IMT on functionality in adolescents and young adults with cerebral palsy. Improvements are expected in the above variables as well as in maximal inspiratory pressure (MIP) and possibly in pulmonary function.
Methods
Study design
The study was a single blind randomized controlled clinical trial (RCT) with allocation concealment. The study protocol was approved by the Internal Research Ethics- Bioethics Committee (1377/20-04-2022) of School of Physical Education and Sports Science of National and Kapodistrian University of Athens and registered on ANZCTR (Australia New Zealand Clinical Trials Registry) with registration number ACTRN12625000149460, retrospectively. The present study followed the SPIRIT (Standard Protocol Items: Recommendations for International Trials) statement.
Participants
The participants were volunteers, recruited from a special education public school and a special education center in Athens, Greece. They were diagnosed with cerebral palsy by a qualified pediatric neurologist [20] and were able to understand and follow simple verbal commands in Greek. They were also at levels I to III according to the Gross Motor Function Classification System (GMFCS) (able to walk with or without assistance) [21]. Exclusion criteria: level IV to V (GMFCS), participation in another IMT program six (6) months before the study [17], participation in therapeutic procedures such as orthopedic surgeries or botox injections in the last six (6) months [17,19], cardiopulmonary diseases, acute medical illness, inability to understand and follow verbal instructions and concurrent involvement in interventional programs [1]. Participants did not receive any kind of economic support and provided informed consent for their inclusion in the study.
Power analysis
The calculation of the minimum sample size for detecting significant differences between groups was based on the effect size of 0.85 for the 6MWT in the study of Keles and colleagues (2018) and the corresponding tables of Whitley and Ball (2002) [22]. More specifically, with an effect size of 0.85, power size of 0.80, and α = 0.05, the minimum sample size was found to be 40 participants, corresponding to 20 individuals allocated in the experimental (IMT) group and 20 in the control group.
Randomization and blinding procedures
Initially, 42 adolescents and young adults with CP (level I to III, according to the GMFCS) volunteered to participate in the study, aged 15 to 27 years, who underwent baseline assessment (from October 2023). They were randomly assigned to experimental (8 women and 13 men) and control groups (9 women and 12 men) using a computer-generated method by the primary researcher. Only the primary researcher was aware of the allocation of the participants.
During the study, five (5) participants had to drop out, four (4) due to respiratory disease and one (1) due to musculoskeletal injury. The final sample consisted of 37 adolescents and young adults with CP (level I to III, according to the GMFCS), aged 15 to 27 years, as they were initially allocated to experimental (8 women and 12 men) and control groups (6 women and 11 men).
The study’s flowchart is presented in Figure 1, according to CONSORT 2025 Flow Diagram [23].
Research Tools
Participants were assessed by a pneumonologist and a physical therapist, blinded to the patients’ treatment allocation, on the following measures, administered in random order, at three points (0, 4, 8 weeks):
- A questionnaire regarding
- The 6-minute Walking Test (6MWT) [24].
- The five repetitions sit-to-stand test (STS) [25].
- Spirometry with the Spiro sense spirometry system (Burdick, Inc., Deerfield, WI, USA).
- Maximal Inspiratory Pressure (MIP), Maximal Expiratory Pressure (MEP) with a portable respiratory pressure meter (MD Diagnostics Ltd. Kent, UK).
- The 1-minute walking distance test (1MWT) [26, 27].
- The Timed up and down stairs test (TUDS) [28].
- The Berg Balance Scale (BBS) [29].
- The World Health Organization-Disability Assessment Schedule (WHODAS 2.0) [30].
Primary outcome
The 6-minute Walking Test (6MWT) [24] has been used to evaluate the functional exercise capacity in children with CP [19,31,32]. In the present study, the 6MWT was performed according to the American Thoracic Society (ATS) recommendations (2002) [33]. The 6MWT has been shown to be a valid [34] and reliable test [32] for ambulatory children with CP.
Secondary outcomes
The 1-minute walking distance test (1MWT) [26] evaluates the walking ability of the participants for one minute in a 20-meter oval track. It has been used for rapid assessment in adolescents with CP levels I–III, both at school environment and during rehabilitation [27] showing high intraclass correlation coefficient. High intraclass coefficient has been reported in children with bilateral spastic CP as well [35].
The five repetitions sit-to-stand test (STS) [25] has been used to evaluate the functional strength in children with CP [36] and has shown high intraclass correlation coefficient (ICC) and inter-rater reliability for children and adolescents with CP [37].
The Timed up and down stairs test (TUDS) assesses functional mobility in children with CP [28]. It has demonstrated excellent test-retest reliability, intra-rater and inter-rater reliability [38].
The Berg Balance Scale (BBS) [29] evaluates functional balance [39] and has appeared to be a valid and highly reliable tool in adolescents with CP [40]. The BBS can be used for both clinical examinations and for distinguishing between levels of functional balance in adolescents with CP [40]. The BBS has been validated in a Greek sample with excellent reliability [41].
The World Health Organization-Disability Assessment Schedule (WHODAS 2.0) assesses disability, considering body deficiencies, activity limitations as well as restrictions in participation [30,42]. The WHODAS 2.0 has shown high internal consistency [42] and has been proved to be a reliable and valid instrument for the Greek population, demonstrating excellent internal consistency [43].
Maximal Inspiratory Pressure (MIP) and Maximal Expiratory Pressure (MEP) were measured according to the American Thoracic Society/ European respiratory Society criteria (2002) [44], using a respiratory pressure meter device (MD Diagnostics Ltd. Kent, UK). MIP has been used for assessing the strength of inspiratory muscles in children with CP [1,9,19].
The Pulmonary function test was performed with spirometry using a calibrated spirometer (Spiro sense spirometry system, Burdick, Inc. Deerfield, WI, USA) according to the guidelines of the American Thoracic Society (ATS) and European Respiratory Society (ERS) [45]. The maximal air volume exhaled in the first second of forced maximal exhalation (FEV1), the maximal air volume exhaled in forced exhalation (FVC) and the maximal flow during exhalation (PEF) were measured and recorded as percentages of the predicted values. Before the test, the participants were at rest for 10 minutes. The spirometry test was performed three times, and the best results, for the above-mentioned variables, were recorded [19].
Method of Comparison
Initial assessment
A pneumonologist performed lung function testing (FEV1, FVC, PEF) as well as MIP and MEP measurements for assessing respiratory muscle strength. A qualified physical therapist, with five years of experience in the assessment of neurologic patients, measured all functional tests (6MWT, 1MWT, STS, TUDS, BBS) and administered WHODAS 2.0 in all participants. The participants were at rest before each assessment, according to their heart rate and the rated perceived exertion (PRE) scale. The above research colleagues delivered the collected data from each measurement of the study (0, 4, 8 weeks) to the secretariat of the special education school and special education center, which in turn forwarded the data to the statistician and the primary researcher.
Interventions
Before the initial assessment, both groups attended a one-hour informative session, handled by the primary researcher. The session covered respiratory pump function and functional ability as well as physiotherapy management for individuals with CP. During the session, there was a demonstration of a) the pulmonary function tests and b) the MIP and MEP measurements by the pneumonologist, and c) the functional ability tests, and the WHODAS 2.0, by a physiotherapist (different from the one that participated in the initial assessment), who implemented the IMT intervention. Additionally, all participants followed the standardized physiotherapy program of the special education school and center, which included stretching exercises, range of motion exercises and techniques for facilitating normal movement patterns, all tailored to individual needs. The standardized physiotherapy program was implemented and supervised by the physiotherapist of the special education school and center.
Experimental group: A qualified physical therapist with five years of experience in the treatment of neurologic patients (different from the physiotherapist who conducted the assessments) managed and implemented the IMT intervention program to ensure the adherence and address any possible discomfort, such as dizziness, breathing difficulties, or fatigue. The physical therapist also kept a diary during the sessions, recording these findings as well as any other symptoms. Before intervention, the experimental group completed three familiarization sessions to become accustomed to the training device (Threshold IMT, Philips-Respironics, Pittsburgh, PA, USA) and to learn how to perform diaphragmatic breathing. In addition, the specific physiotherapist provided information regarding the eight-week duration of the intervention. Specifically, the experimental group received four (4) 20-minute inspiratory training sessions per week using the threshold respiratory device, which applied specific, constant resistance during inspiration, over the course of eight (8) weeks at the special education school and center. The resistance of the IMT started at 30% of the initial MIP and was adjusted every two weeks to correspond to 30% of the MIP at each period of the program. Participants were instructed to complete 10–15 breaths using the IMT device during each session. Then, they rested for 30 seconds while performing diaphragmatic breathing before continuing with the IMT. Participants were excluded from the study if they missed more than one treatment session or experienced symptoms of acute respiratory disease.
Control Group: This group participated in the standardized physiotherapy program provided by the special education school and center, which was customized to each participant’s needs, as presented above.
Data analysis
In the present study, data analyses were conducted with the Statistical Package for the Social Sciences (IBM Corp., SPSS, version 19, Armonk, NY, USA). The Shapiro-Wilk test was used initially to explore data normality for every dependent variable for primary (6MWT) and secondary outcome measures (1MWT, STS, TUDS, BBS, WHODAS 2.0, MIP, MEP, FEV1, FVC and PEF) [46]. The reliability of repeated measurements (test-retest reliability) was tested, with the intraclass correlation coefficient (ICC) [47], to examine the degree of association across the assessments (0, 4 and 8 weeks) for the entire sample.
A 2 × 3 repeated measures ANOVA with Bonferroni adjustment was conducted for the interaction effect between intervention (experimental and control group) and time (0, 4, and 8 weeks) for every dependent variable separately [48]. Levene’s test was used to assess the homogeneity of variance [49]. The statistical significance level (p) was set at 0.05.
Results
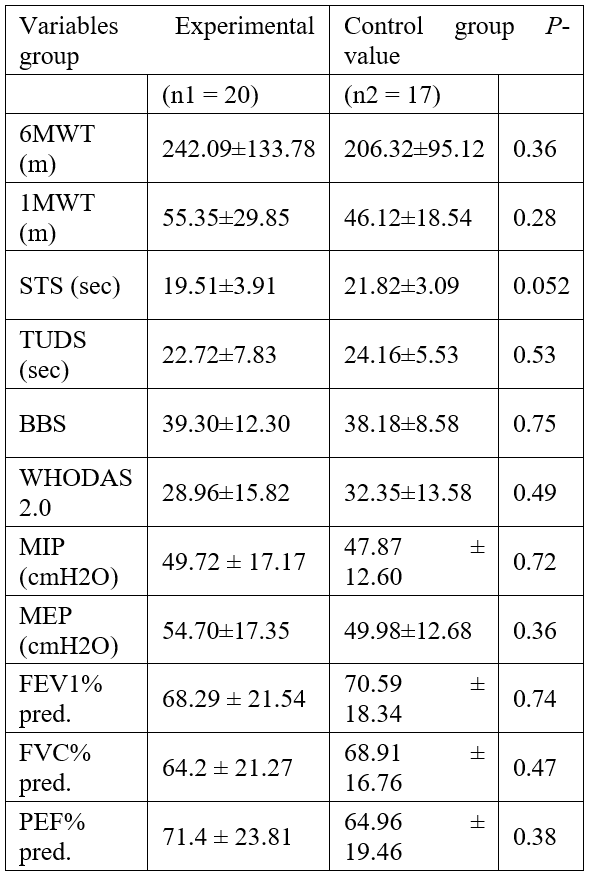
37 adolescents and young adults with CP, aged 15 to 27 years, participated in the study. The participants were randomized to experimental (8 women and 12 men) and control groups (6 women and 11 men). No baseline group differences were found in demographic characteristics (Table 1). The participants in the experimental group compared to those in the control group did not differ significantly in the baseline assessment of the research variables (p >0.05) (Table 2).
Levene’s test was found greater than 0.05, indicating that the variances were not significantly different and the assumption of the homogeneity was met [49].
Table 1: Distribution of 37 study participants with cerebral palsy by socio- demographic characteristics, according to intervention category.
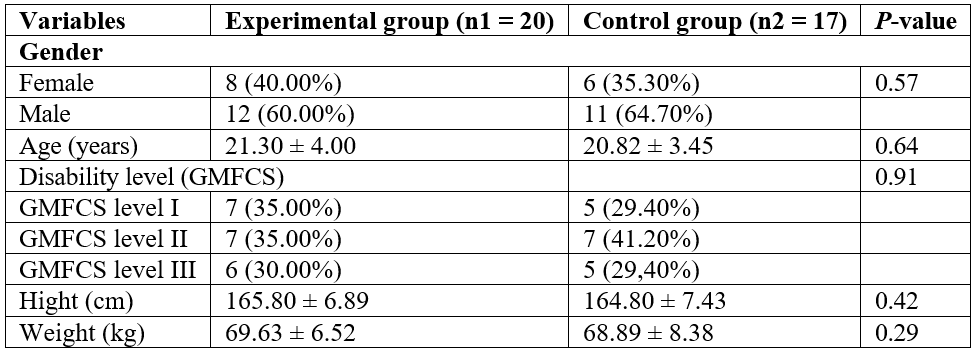
Table 2: Baseline comparisons between experimental and control groups in research variables.
Reliability
The test-retest reliability for all study variables, examined with the intraclass correlation coefficient (ICC), was excellent according to Koo and Li (2016) [47] for the total sample. Specifically, the ICC was found: 0.97 for FEV1, 0.97 for FVC, 0.97 for PEF, 0.91 for MIP, 0.95 for MEP, 0.95 for 1MWT, 0.87 for 6MWT, 0.94 for STS, 0.97 for TUDS, 0.96 for BBS and 0.93 for WHODAS 2.0.
Interaction effect between intervention and time
The factorial 2 × 3 ANOVA analysis showed significant interaction effect between intervention and time regarding:
a) 6MWT (F = 02, p < 0.001, η2 = 0.53) (Figure 2),
b) 1MWT (F = 99, p < 0.001, η2 = 0.62) (Figure 3),
c) STS (F =83.61, p < 001, η2 = 0.83) (Figure 4),
d) TUDS (F = 98, p < 0.001, η2 = 0.60) (Figure 5),
e) WHODAS 0 (F = 33.63, p < 0.001, η2 = 0.66) (Figure 6),
f) MIP (F = 15, p < 0.001, η2 = 0.91) (Figure 7),
g) MEP (F = 62.12, p < 0.001, η2 = 0.79) (Figure 8),
h) FEV1 % pred (F = 88, p < 0.001, η2 = 0.41) (Figure 9),
i) FVC % pred (F = 09, p = 0.003, η2 = 0.29) (Figure 10) and
j) PEF % pred (F = 23, p = 0.023, η2 = 0.20) (Figure 11).
Differences between experimental and control groups
Table 3 presents the mean values and standard deviations of the study variables for both experimental and control groups across time, as well as the t-test parameter estimates used to evaluate the group differences across time.
Table 3: Participants’ performance assessment across time.
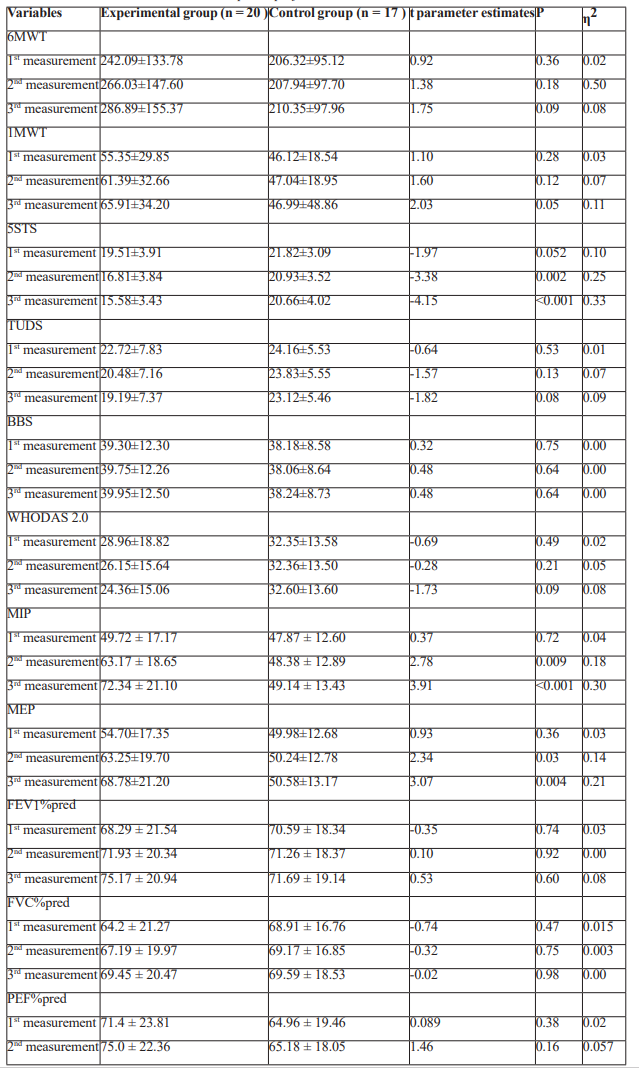
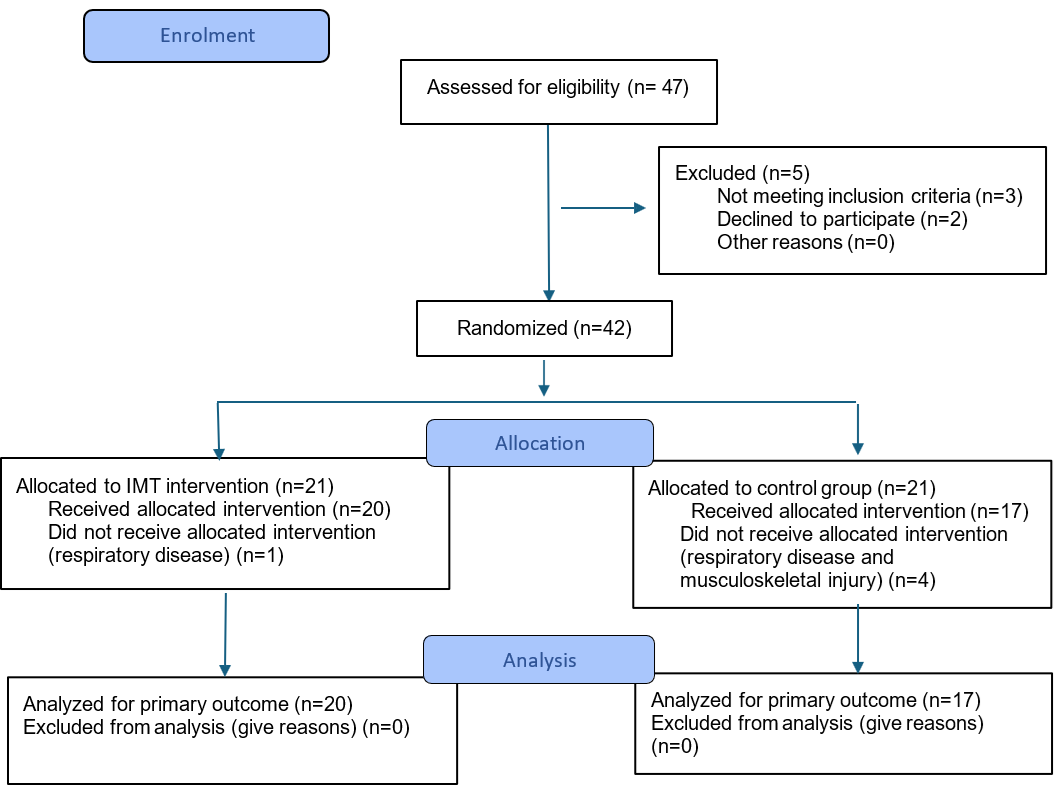
Figure 1: Flowchart of the study (CONSORT 2025).
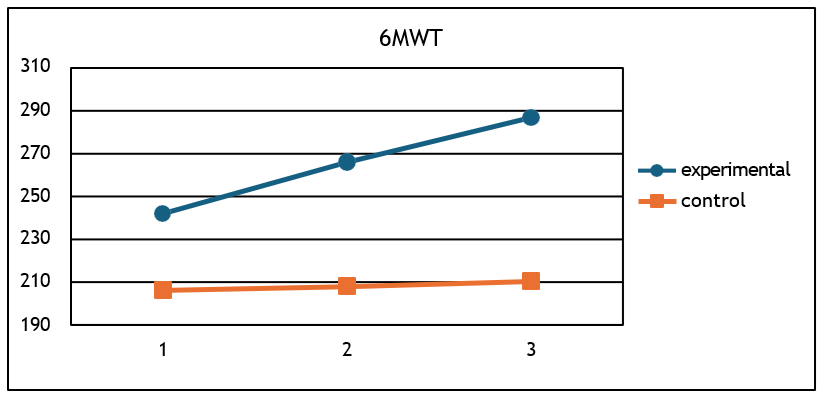
Figure 2: Mean 6MWT values for the two groups at the 3 measurements.
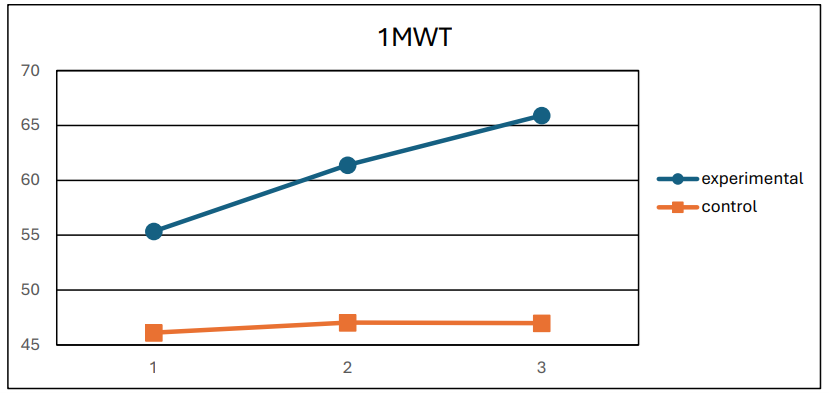
Figure 3: Mean 1MWT values for the two groups at the 3 measurements.
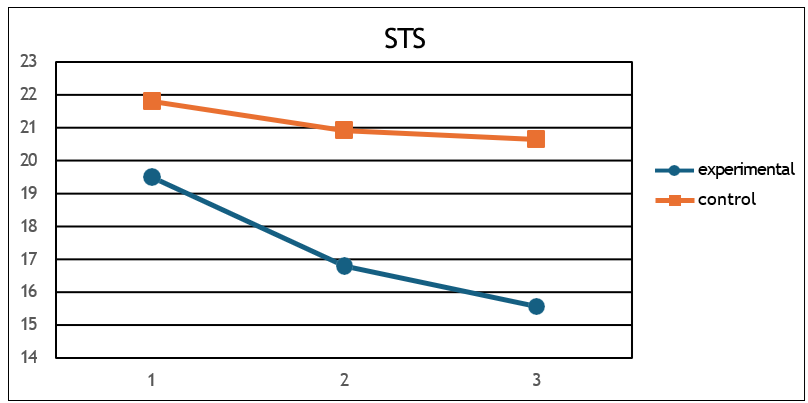
Figure 4: Mean STS values for the two groups at the 3 measurements.
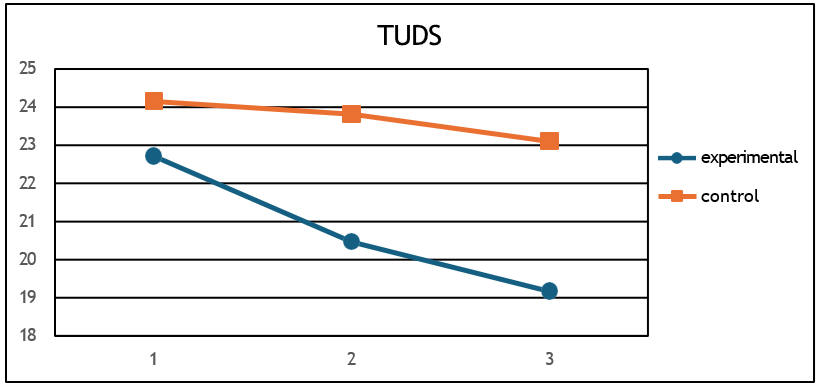
Figure 5: Mean TUDS values for the two groups at the 3 measurements.
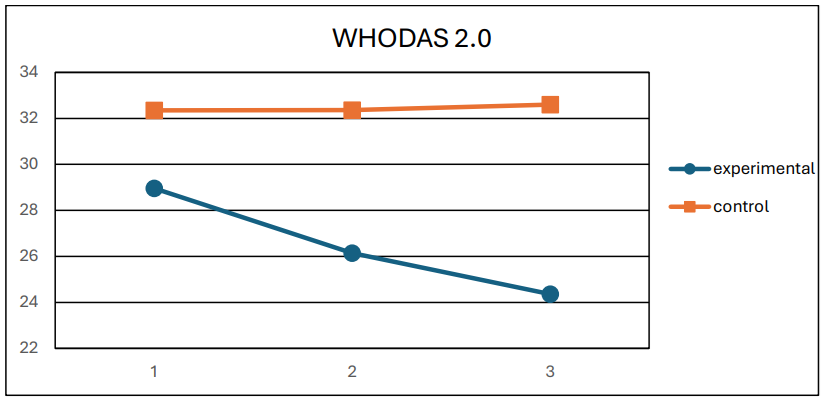
Figure 6: Mean WHODAS 2.0 values for the two groups at the 3 measurements.
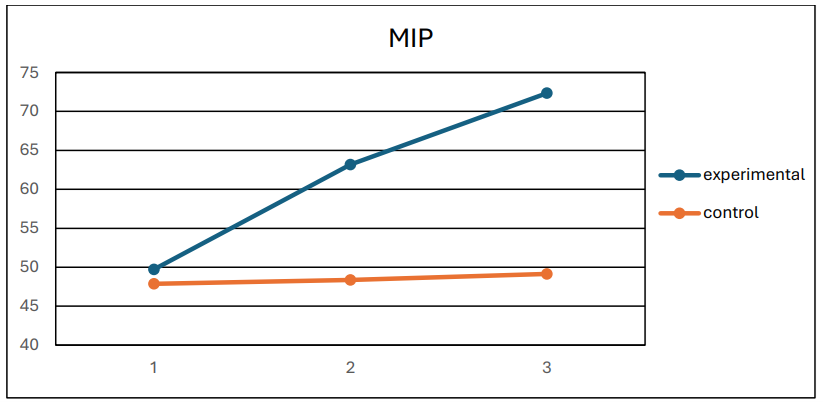
Figure 7: Mean MIP values for the two groups at the 3 measurements.
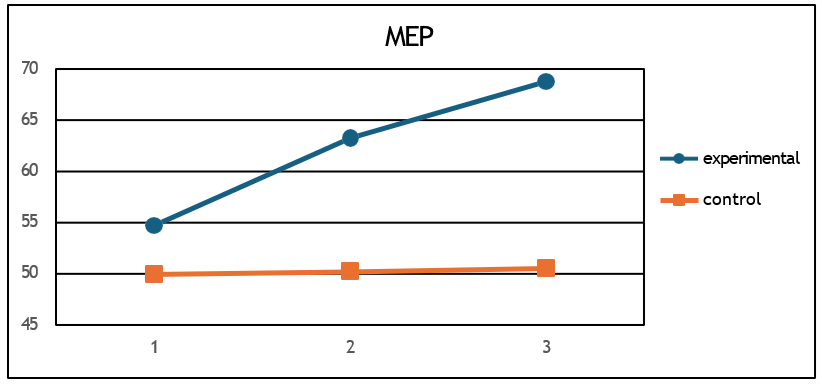
Figure 8: Mean MEP values for the two groups at the 3 measurements.
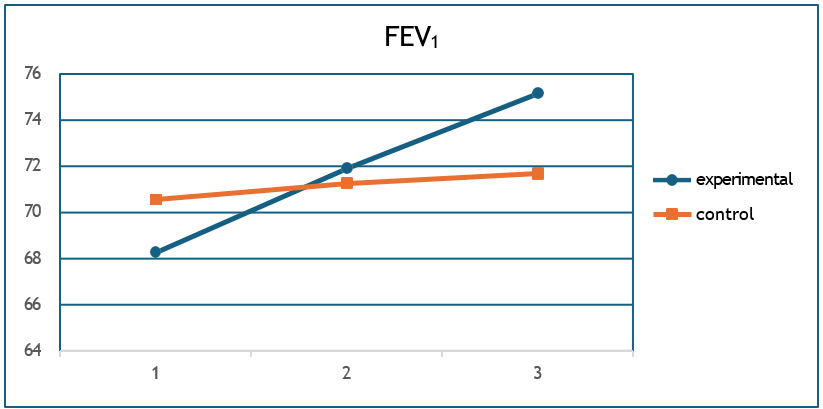
Figure 9: Mean FEV1%pred values for the two groups at the 3 measurements.
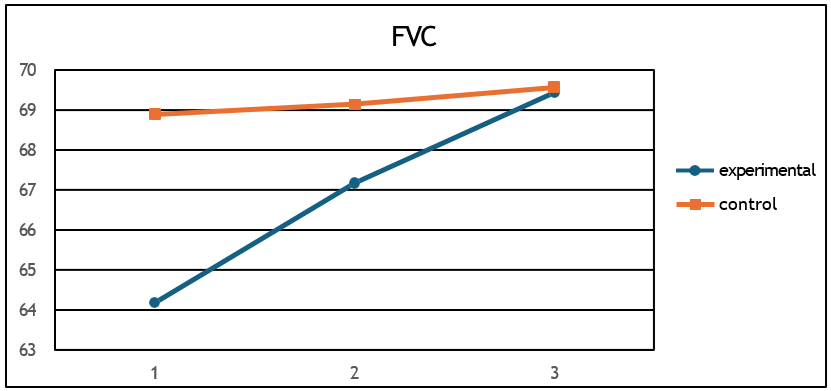
Figure 10: Mean FVC%pred values for the two groups at the 3 measurements.
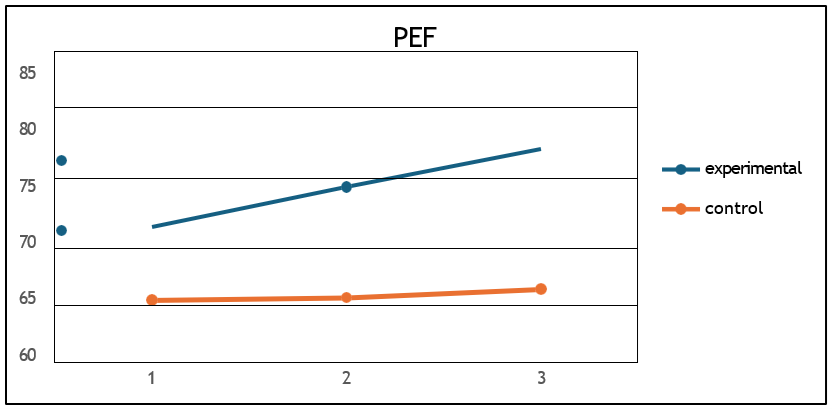
Figure 11: Mean PEF%pred values for the two groups at the 3 measurements.
Discussion
The present study was the first known RCT to examine the effectiveness of IMT on functional ability in adolescents and young adults with CP. The above clinical population has been investigated only to a limited extent, despite the increasing mobility restrictions associated with aging. The IMT intervention therefore improved functional ability (6MWT, 1MWT, STS and TUDS), perceived disability (WHODAS 2.0), respiratory muscle strength (MIP and MEP), as well as pulmonary function (FEV1%pred, FVC% pred, PEF% pred) in adolescents and young adults in an eight- week period.
The interaction effect in the outcome variables was associated with no group differences across time, except in STS, MIP and MEP. According to Leppink, O’Sullivan and Winston (2017) [50], the interaction effect may occur when the extent of group differences are changing or shifting across time with respect to the outcome variables. In the present study, the interaction was due to the changing size of group differences across time, besides FEV1, where a shifting of differences between groups was observed [51].
The significant improvement in functional ability tests following IMT suggests that respiratory training may have positive effects on peripheral muscles. This effect on peripheral muscles may be attributed to the attenuation of inspiratory muscle metaboreflex, which enhances oxygenation and blood flow to peripheral muscles, resulting in improvements in physical performance and exercise tolerance [52,53]. According to Vilaça et al (2019) [54], during exercise, the sympathetic nervous system intervenes through the inspiratory muscle metaboreflex, causing a decrease in blood flow to active peripheral muscles, reducing performance. IMT seems to attenuate the inspiratory muscle metaboreflex, enhancing physical performance and delaying fatigue, as shown by the increase in 6MWT in the present study. In addition, aerobic capacity of inspiratory muscles may be promoted with IMT, resulting in increased minute ventilation during exercise and improving exercise tolerance [55]. The improvement of STS and TUDS due to IMT may include involvement of the diaphragm [19] and show the need to control the trunk and lower extremity movements in adolescents and young adults with CP. IMT increases inspiratory muscle strength and possibly improves their function, including the contribution of diaphragm to the regulation of intra-abdominal pressure, participating in this way to postural control through enhanced core stability in dynamic movement conditions [1]. These findings may also be attributed to the increase in MEP value, because of IMT implementation. In a study including children with cystic fibrosis, MEP was determined as a predictor for dynamic postural stability, as it reflects abdominal muscle strength [56]. The recruitment of abdominal muscles for stabilizing the trunk is essential in extremity movements, reflecting the ability of dynamic postural stability [56]. During STS and TUDS tests, the improvement in dynamic postural stability, resulting from better diaphragmatic function and abdominal muscle activation, may have resulted in more efficient movement patterns and thus in decreasing the time to complete the tests. There are no studies performed in CP populations examining STS and TUDS test results pre and post IMT. The findings of the present study may contribute as an initial indicator to including IMT in rehabilitation programs for adolescents and young adults with CP to improve their functional ability and exercise capacity.
The IMT has been shown to have positive effects on exercise capacity, activities of daily living and quality of life in children with CP [1] whereas other studies concluded that IMT showed no significant difference in balance [19] and in 6MWT [16,19]. The 6MWT findings of the present study are consistent with the findings of Keles et al (2018) [1], indicating that IMT improves exercise capacity in adolescents and young adults with CP, although the study of Keles et al (2018) [1] included participants aged 7-14 years old, with GMFCS levels I and II. In the study of Kepenek-Varol et al (2021) [19], in hemiplegic children with CP (GMFCS levels I and II), no significant difference in 6MWT was evident between groups (experimental-IMT and control), but there was a significant increase in 6MWT pre and post intervention in both groups separately. In the same study though, the IMT was implemented for 15 minutes twice every day, seven days per week for eight weeks, but only one session per week was supervised by a physiotherapist. Another study showed no impact of IMT on 6MWT in children and adolescents with CP (GMFCS levels I-III), as IMT was implemented only for 15 minutes, in 3 sessions per week for six weeks, probably not imposing an adequate load to induce adaptations to inspiratory muscles and thus significant changes in 6MWT [16].
The present study recorded no significant changes in BBS score after the IMT, in accordance with the findings of Kepenek-Varol et al (2021) [19], despite the differences in the IMT protocol employed in the present study. Postural control and balance are impaired in children with CP, leading to restrictions in daily activities [19]. In contrast, Keles et al (2018) [1], demonstrated significant improvement in balance, assessed with the Trunk Control Measurement Scale-TCMS, after a 6-week IMT. In the present study, balance was assessed with the BBS, with 14 different tasks, some of them involving whole body postural control [29], while TCMS used by Keles et al (2018) [1] focuses on trunk control measurements, assessing balance parameters affected by separate body compartments. Furthermore, TCMS may detect changes after IMT because of the location of respiratory muscles and their role in trunk stability, as mentioned above.
Children with CP endure lifelong restrictions that affect their quality of life [1]. In addition, a study of Maanum et al (2010) [57] revealed that 39% of their participants experienced a decline in functionality, as they had deteriorated by one GMFCS level from the adolescence to the adulthood. It has also been reported that there is a correlation between quality of life and functionality in children with CP [58]. The findings of the presents study demonstrated a significant change in WHODAS 2.0 scores, indicating reduced perceived disability among participants as a result of enhanced functionality. The present finding is in accordance with the study of Keles et al (2018) [1], who reported improvements in well-being, acceptance and functionality, as measured by the Cerebral Palsy Quality of Life Questionnaire for Children (CPQOL- Child), following IMT.
Prior to IMT, all participants in the present study exhibited inspiratory muscle weakness, with MIP values lower than 80cmH2O [44]. Previous studies have also observed respiratory muscle weakness in adults [11] and children with CP [1,59]. The present study showed significant improvements in respiratory muscle strength, as indicated by increases in MIP and MEP values in adolescents and young adults with CP. The observed improvement in inspiratory muscle strength could likely be attributed to IMT, as this intervention is specifically designed to apply resistive load to the inspiratory muscles [60]. Inspiratory muscles respond to IMT load like other skeletal muscles respond to external resistance, resulting in increasing endurance and strength [61]. IMT produces its effect by causing the inspiratory muscles to adjust in order to overcome the imposed resistance [60]. In the present study, MEP also showed improvement, indicating adaptations in the expiratory muscles after IMT. The recorded improvements in respiratory muscle strength may also be attributed to the learning effect, after repetitive exposure to training load, which enables more efficient neuromuscular recruitment patterns [11]. The findings of the present study are in line with those of Martin-Sanchez et al (2024) [11], who investigated the effect of IMT on institutionalized adults with CP, applying low-intensity IMT (20% of MIP) vs high- intensity IMT (40% of MIP) and resulted in MIP and MEP increment. In addition, our findings are aligned with previous similar studies in children with CP [1], and with hemiplegic cerebral palsy [19]. On the contrary, Aanand and Karthikbadu (2021) [16] in children and adolescents with CP, showed no effect on MIP. This inconsistency may result from the differences in the imposed load in IMT.
The significant improvement in pulmonary function (FEV1%pred, FVC%pred, and PEF%pred) during the present study may be explained by the increased MIP and MEP. Adults with CP exhibit reduced lung volumes due to restricted lung expansion, attributed to weakness in trunk muscles [62] and trunk control that is related to expiratory muscle strength [63]. Children with CP also exhibit reduced vital capacity due to inspiratory and expiratory muscle weakness [9]. The observed increase in PEF may have resulted from the augmented lung expansion, ensuing from the inspiration against resistance in IMT. This enlarged lung expansion may have led to greater flow rates during expiration and thus in increased PEF [16]. The findings of the present study may be supported by those of Fry et al (2007) [64], who implemented IMT in patients with multiple sclerosis and led to improvement in deep breathing, which in turn improved FEV1 and FEF25-75%. Similar findings (FEV1, PEF) were also observed in the study of a) Martin-Sanchez et al (2024) [11] conducted in institutionalized adults with CP (GMFCS levels I-V), b) Gkaraveli et al. (2019) [65] examining the effect of IMT on pulmonary function (FEV1, FVC) in preschool children with spastic CP and c) Lee at al. (2014) [18] who examined the effect of feedback respiratory training on pulmonary function (FEV1, FVC) in children with CP. On the contrary, a) Anand and Kartikbadu (2021) [16] reported significant difference only in PEF%pred, and not in FEV1%pred and FVC%pred in children and adolescents with CP, possibly due to the differences in the duration of the program as well as to the fewer repetitions of the IMT sessions per week (three sessions per week) compared to the present study. Also, b) Kepenek-Varol et al. (2021) [19] implementing IMT in hemiplegic children with CP found a significant increase only in PEF%pred, and not in FEV1%pred and FVC%pred, possibly due to the different delivery methods of IMT (home training program) and c) Keles et al. (2018) [1] applying IMT in children with CP (GMFCS levels I and II) reported not significant differences in pulmonary function, probably due to the different age groups, the GMFCS levels as well as the differences in the IMT protocols.
The strength of the present study lies in: a) no baseline differences between groups,
b) the internal validity, assured by randomization, concealed allocation and blinding of the examiners, the use of valid and reliable tools (1MWT, 6MWT, STS, TUDS, BBS, WHODAS), homogeneity of the sample, no participation of volunteers in other training programs and c) the physiological assessments (FEV1%pred, FVC%pred, and PEF%pred) used.
The present single-blind study has certain potential limitations. The total sample was recruited from a specific special education school and a respective center, which may limit the external validity of the results. Further, although the initial pool consisted of 42 participants, there was a drop out of five individuals (two adolescents and three young adults), that led to a decrement in the required sample size. Despite the sample size limitation, the effect size (η2) for functionality, respiratory muscle strength and pulmonary function was found to be moderate to high, supporting therefore the power analysis conducted in the present study [66].
Future research should investigate the effect of IMT on functional capacity and daily activities over a longer period, as well as the long-term effects of such training on adults with CP. Furthermore, other psychosocial variables should be evaluated, such as changes in occupation, participation and income following IMT. Alternative methods of implementing the program may also be explored in the future, such as home-based IMT after self-training or integrating IMT into a tele-rehabilitation program. In addition, future studies should aim to include all GMFCS levels and potentially develop and establish standardized program guidelines for each level.
Clinical Implementation
Although current scientific evidence supports the use of IMT in individuals with CP, clinical trials in adolescents and young adults with CP are limited, and no standardized IMT program has been established for this population. Respiratory problems and functional limitations observed in adults with CP represent a significant challenge for respiratory physiotherapy today. The present study is the first RCT to examine the effectiveness of IMT on functional ability in adolescents and young adults with CP. Its clinical implications arise from the magnitude of the effect on functional ability, respiratory muscle strength, and pulmonary function. The protocol of the present study may be used for designing and implementing integrated CP strategies in the future,
potentially facilitating the expansion of IMT implementation in adolescents and adults with CP.
Conclusion
The present study provided evidence for the effectiveness of an IMT program on functional ability, respiratory muscle strength, and pulmonary function in adolescents and young adults with CP. The IMT program had a moderate to high effect on each outcome variable, which is unlikely to be attributed to other confounding factors not assessed in the experimental procedure. The procedure followed in the present study may be suggested as a cornerstone of an integrated CP rehabilitation program for adolescents and young adults.
Authorship criteria:
1. Concept and design of study: Afrodite Evangelodimou, Emmanouil Skordilis, Eirini Grammatopoulou, acquisition of data: Afrodite Evangelodimou, analysis and interpretation of data: Afrodite Evangelodimou, Emmanouil Skordilis, Eirini Grammatopoulou
2. Drafting the article or revising it critically for important intellectual content: Konstantinos Karteroliotis
3. Final approval of the version to be published: Emmanouil Skordilis - guarantor
Conflicts of Interest: The authors declare no conflicts of interest.
Funding: This research received no external funding.
Acknowledgments: I would like to express my gratitude to the non-profit organization Cerebral Palsy Greece/Open Door for their assistance and especially to Mrs Aikaterini Spyridaki and Mrs Georgia Spai.
References
- Keles MN, Elbasan B, Apaydin U, Aribas Z, Bakirtas A, Kokturk N. Effects of inspiratory muscle training in children with cerebral palsy: a randomized controlled trial. Braz J Phys Ther, 2018; 22: 493-501.
- González-Matilla R, Abuín-Porras V, Mínguez-Esteban I, Heredia-Rizo AM. Biomechanical and clinical differences in muscle tone, stiffness, range of motion, and pain perception in children with cerebral palsy: a cross-sectional study. Front Physiol, 2025; 16: 1588084.
- Bennett S, Siritaratiwat W, Tanrangka N, Bennett MJ, Kanpittaya J. Diaphragmatic mobility in children with spastic cerebral palsy and differing motor performance levels. Respir Physiol Neurobiol, 2019; 266: 163-170.
- Kocjan J, Gzik-Zroska B, Nowakowska K, Burkacki M, Suchoń S, Michnik R, et al. Impact of diaphragm function parameters on balance maintenance. PLoS One, 2018; 13: e0208697.
- Garcia CC, Alcocer-Gamboa A, Ruiz MP, Caballero IM, Faigenbaum AD, Esteve-Lanao J, et al. Metabolic, cardiorespiratory, and neuromuscular fitness performance in children with cerebral palsy: A comparison with healthy J Exerc Rehabil, 2016; 12: 124- 131.
- Eken MM, Houdijk H, Doorenbosch CA, Kiezebrink FE, van Bennekom CA, Harlaar J, et al. Relations between muscle endurance and subjectively reported fatigue, walking capacity, and participation in mildly affected adolescents with cerebral Dev Med Child Neurol, 2016; 58: 814-821.
- Balemans AC, Van Wely L, De Heer SJ, Van den Brink J, De Koning JJ, Becher JG, et al. Maximal Aerobic and Anaerobic Exercise. Med Sci Sports Exerc, 2013; 45: 561-568.
- Carlon SL, Taylor NF, Dodd KJ, Shields N. Differences in habitual physical activity levels of young people with cerebral palsy and their typically developing peers: a systematic review. Disabil Rehabil, 2013; 35: 647-655.
- Kwon YH, Lee HY. Differences of the truncal expansion and respiratory function between children with Spastic Diplegic and Hemiplegic Cerebral Palsy. J Phys Ther Sci, 2013; 25: 1633-1635.
- Verschuren O, Takken T. Aerobic capacity in children and adolescents with cerebral palsy. Res Dev Disabil, 2010; 31: 1352-1357.
- Martin-Sanchez C, Barbero-Iglesias FJ, Amor-Esteban V, Martin-Sanchez M, Martin-Nogueras AM. Benefits of inspiratorymuscle training therapy in institutionalized adult peoplewith cerebral palsy: A double-blind randomized controlled trial. Brain Behav, 2024; 14: e70044.
- Fitzgerald DA, Follett J, Van Asperen PP. Assessing and managing lung disease and sleep disordered breathing in children with cerebral Paediatr Respir Rev, 2009; 10: 18-24.
- Seddon PC, Khan Y. Respiratory problems in children with neurological impairment. Arch Dis Child, 2003; 88: 75–78.
- Young NL, McCormick AM, Gilbert T, Ayling-Campos A, Burke T, Fehlings D, et al. Reasons for hospital admissions among youth and young adults with cerebral palsy. Arch Phys Med Rehabil, 2011; 92: 46-50.
- Wang HY, Chen CC, Hsiao SF. Relationships between respiratory muscle strength and daily living function in children with cerebral palsy. Res Dev Disabil, 2012; 33(4): 1176-1182.
- Anand B, Karthikbabu S. Effects of additional inspiratory muscle training on mobility capacity and respiratory strength for school-children and adolescents with cerebral palsy: a randomized controlled trial. Braz J Phys Ther, 2021; 25: 891-899.
- Choi JY, Rha DW, Park Change in pulmonary function after incentive spirometer exercise in children with spastic cerebral palsy: A randomized controlled study. Yonsei Med J, 2016; 57: 769-775.
- Lee HY, Cha YJ, Kim K. The effect of feedback respiratory training on pulmonary function of children with cerebral palsy: a randomized controlled preliminary report. Clin Rehabil, 2014; 28: 965-971.
- Kepenek-Varol B, Gürses HN, İçağasıoğlu DF. Effects of Inspiratory Muscle and Balance Training in Children with Hemiplegic Cerebral Palsy: A Randomized Controlled Trial. Dev Neurorehabil, 2022; 25: 1-9.
- Jones MW, Morgan E, Shelton JE, Thorogood C. Cerebral palsy: introduction and diagnosis (part I). J Pediatr Health Care, 2007; 21: 146-152.
- Palisano R, Rosenbaum P, Walter S, Russell D, Wood E, Galuppi B. Development and reliability of a system to classify gross motor function in children with cerebral palsy. Dev Med Child Neurology, 1997; 39: 214–223.
- Whitley E, Ball Statistics review 4: sample size calculations. Crit Care, 2002; 6: 335-341.
- Hopewell S, Chan AW, Collins GS, Hróbjartsson A, Moher D, Schulz KF, et CONSORT 2025 Statement: updated guideline for reporting randomised trials. BMJ, 2025; 388: e081123.
- Solway S, Brooks D, Lacasse Y, Thomas S. A qualitative systematic overview of the measurement properties of functional walk tests used in the cardiorespiratory domain. Chest, 2001; 119: 256-270.
- Medina-Mirapeix F, Vivo-Fernández I, López-Cañizares J, García-Vidal JA, Benítez-Martínez JC, Del Baño-Aledo Five times sit-to-stand test in subjects with total knee replacement: Reliability and relationship with functional mobility tests. Gait Posture, 2018; 59: 258-260.
- McDowell BC, Kerr C, Parkes J, Cosgrove Validity of a 1-minute walk test for children with cerebral palsy. Dev Med Child Neurol, 2005; 47: 744-748.
- Chrysagis N, Skordilis EK, Koutsouki D. Validity and clinical utility of functional assessments in children with cerebral Arch Phys Med Rehabil, 2014; 95: 369-374.
- Zaino CA, Marchese VG, Westcott SL. Timed up and down stairs test: preliminary reliability and validity of a new measure of functional mobility. Pediatr Phys Ther, 2004; 16: 90-98.
- Berg KO, Wood-Dauphinee SL, Williams JI, Maki Measuring balance in the elderly: validation of an instrument. Can J Public Health, 1992; 83: S7- S11.
- World Health Organization. Measuring Health and Disability: Manual for WHO Disability Assessment Schedule WHODAS 2.0. World Health Organization, 2010.
- Fitzgerald D, Hickey C, Delahunt E, Walsh M, OʼBrien T. Six-Minute Walk Test in Children with Spastic Cerebral Palsy and Children Developing Typically. Pediatr Phys Ther, 2016; 28: 192-199.
- Maher CA, Williams MT, Olds The six-minute walk test for children with cerebral palsy. Int J Rehab, 2008; 31: 185-188.
- ATS Statement: Guidelines for the Six-Minute Walk Am J Respir Crit Care Med, 2002; 166: 111–117.
- Nsenga Leunkeu A, Shephard RJ, Ahmaidi S. Six-minute walk test in children with cerebral palsy gross motor function classification system levels I and II: reproducibility, validity, and training effects. Arch Phys Med Rehabil, 2012; 93: 2333-2339.
- McDowell BC, Humphreys L, Kerr C, Stevenson Test- retest reliability of a 1-min walk test in children with bilateral spastic cerebral palsy (BSCP). Gait Posture, 2009; 29: 267-269.
- Chaovalit, S.; Dodd, K.J.; Taylor, N.F. Sit-to-stand training for self-care and mobility in children with cerebral palsy: a randomized controlled Dev Med Child Neurol 2021, 63, 1476-1482.
- Kumban W, Amatachaya S, Emasithi A, Siritaratiwat Five-times-sit-to- stand test in children with cerebral palsy: reliability and concurrent validity. NeuroRehabilitation, 2013; 32: 9-15.
- Ayed AE, Hanna S, Abdelazeim FH. Reliability of the TUDS test for children with cerebral palsy. Bull Fac Phys Ther, 2022; 27: 46.
- Hayes KW, Johnson ME. Measures of adult general performance tests: The Berg Balance Scale, Dynamic Gait Index (DGI), Gait Velocity, Physical Performance Test (PPT), Timed Chair Stand Test, Timed Up and Go, and Tinetti Performance-Oriented Mobility Assessment (POMA). Arthritis Care Res, 2003; 49: s28-s42.
- Jantakat C, Ramrit S, Emasithi A, Siritaratiwat Capacity of adolescents with cerebral palsy on paediatric balance scale and Berg balance scale. Res Dev Disabil, 2015; 36C: 72-77.
- Lampropoulou SI, Gizeli A, Kalivioti C, Billis E, Gedikoglou IA, Nowicky A. Cross Cultural Adaptation of Berg Balance Scale in Greek for Various Balance Impairments. J Phys Med Rehabil Disabil, 2016; 2: 011.
- Díaz-Castro L, Arroyo-Belmonte M, Suárez-Brito P, Márquez-Caraveo ME, Garcia-Andrade C. Validation of the World Health Organization's Disability Assessment Schedule 2.0 for children with mental disorders in specialized health-care services. Front Psychiatry, 2024; 15: 1415133.
- Theotokatos G, Escorpizo R, Angelopoulos TJ, Chrysagis NK, Bickenbach J, Venieri A, et al. Psychometric Properties of the 12-Item World Health Organization Disability Assessment Schedule (WHODAS 2.0), Greek Version: A Cross-Sectional Study on Applicants of Welfare Benefits. Cureus, 2023; 15: e48588.
- American Thoracic Society/European Respiratory Society. ATS/ERS Statement on Respiratory Muscle Testing. Am J Respir Crit Care Med, 2002; 166: 518–
- Miller MR, Hankinson J, Brusasco V, Burgos F, Casaburi R, Coates A, et al. ATS/ERS Task Standardisation of spirometry. Eur Respir J, 2005; 26: 319-338.
- Thomas J, Silverman S, Nelson Research Methods in Physical Activity, 7th ed.; Human Kinetics: Champaign, Illinois, USA, 2015; pp. 189-195.
- Koo TK, Li MY. A Guideline of Selecting and Reporting Intraclass Correlation Coefficients for Reliability J Chiropr Med, 2016; 15: 155- 163.
- Tabachnick B, Fidell L. Using multivariate statistics, 6th ed.; Pearson: Boston, USA, 2013.
- Levene H. Robust Tests for Equality of Variances. In Contributions to Probability and Statistics; Olkin, I., Ed.; Stanford University Press: Palo Alto, USA, 1960.
- Leppink J, O'Sullivan P, Winston K. Are differences between groups different at different occasions? Perspect Med Educ, 2017; 6: 413-417.
- Pedhazur EJ, Pedhazur-Schmelkin L. Multiple Categorical Independent Variables: Factorial Designs. In Measurement, Design, and Analysis: An Integrated Approach; L. Erlbaum Associates: Hillsdale, NJ, USA, 1991.
- Tran D, Munoz P, Lau EMT, Alison JA, Brown M, Zheng Y, et al. Inspiratory Muscle Training Improves Inspiratory Muscle Strength and Functional Exercise Capacity in Pulmonary Arterial Hypertension and Chronic Thromboembolic Pulmonary Hypertension: A Pilot Randomised Controlled Study. Heart Lung Circ, 2021; 30: 388-395.
- Cavalcante Silva RL, Hall E, Maior AS. Inspiratory muscle training improves performance of a repeated sprints ability test in professional soccer players. J Bodyw Mov Ther, 2019; 23: 452-455.
- Vilaça AF, Pedrosa BCS, Amaral TCN, Andrade MA, Castro CMMB, França The effect of inspiratory muscle training on the quality of life, immune response, inspiratory and lower limb muscle strength of older adults: a randomized controlled trial. Rev bras geriatr gerontol, 2019; 22: e190157.
- Gomes-Neto M, Saquetto MB, Silva CM, Carvalho VO, Ribeiro N, Conceição CS. Effects of respiratory muscle training on respiratory function, respiratory muscle strength, and exercise tolerance in patients poststroke: A Systematic Review with Meta-Analysis. Arch Phys Med Rehabil, 2016; 97: 1994-2001.
- Zeren M, Cakir E, Gurses HN. Effects of inspiratory muscle training on postural stability, pulmonary function and functional capacity in children with cystic fibrosis: A randomised controlled trial. Respir Med, 2019; 148: 24-30.
- Maanum G, Jahnsen R, Frøslie KF, Larsen KL, Keller Walking ability and predictors of performance on the 6-minute walk test in adults with spastic cerebral palsy. Dev Med Child Neurol, 2010; 52: e126-132.
- Park Relationship between activity limitation and health-related quality of life in school-aged children with cerebral palsy: a cross-sectional study. Health Qual Life Outcomes, 2017; 15: 87.
- Kwon YH, Lee HY. Differences in respiratory pressure and pulmonary function among children with spastic diplegic and hemiplegic cerebral palsy in comparison with normal controls. J Phys Ther Sci, 2015; 27: 401-403.
- Chung Y, Huang TY, Liao YH, Kuo YC. 12-Week Inspiratory Muscle Training Improves Respiratory Muscle Strength in Adult Patients with Stable Asthma: A Randomized Controlled Int J Environ Res Public Health, 2021; 18: 3267.
- Dsouza FV, Amaravadi SK, Samuel SR, Raghavan H, Ravishankar N. Effectiveness of inspiratory muscle training on respiratory muscle strength in patients undergoing cardiac surgeries: A Systematic Review with Meta- Analysis. Ann Rehabil Med, 2021; 45: 264-273.
- Lampe R, Blumenstein T, Turova V, Alves-Pinto Lung vital capacity and oxygen saturation in adults with cerebral palsy. Patient Prefer Adherence, 2014; 8: 1691-1697.
- Jandt S, Caballero RM, Junior LA, Dias Correlation between trunk control, respiratory muscle strength and spirometry in patients with stroke: an observational study. Physiother Res Int, 2011; 16: 218-224.
- Fry DK, Pfalzer LA, Chokshi AR, Wagner MT, Jackson ES. Randomized control trial of effects of a 10-week inspiratory muscle training program on measures of pulmonary function in persons with multiple J Neurol Phys Ther, 2007; 31: 162-172.
- Gkaraveli M, Skordilis E, Grammatopoulou E, Karteroliotis K, Dania A, Morfis P, et al. The Effect of Inspiratory Muscle Training on Respiratory Pressure, Pulmonary Function and Walking Ability in Preschool Children with Cerebral Palsy. Ann Physiother Clin, 2019; 2: 1010.
- Cohen J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Erlbaum Associates: Hillsdale, NJ, USA, 1988.

