Management of Interhemispheric Subdural Hematoma with Hemispheric Subdural Hematoma
Achraf Moussa1,*, Adil Ounjar1, Hatim Belfquih1,2 and Ali Akhaddar1,3
1Department of Neurosurgery, Avicenne Military Hospital of Marrakech, Morocco
2Cadi Ayyad University in Marrakech, Morocco
3Mohammed V University in Rabat, Morocco
Received Date: 14/09/2025; Published Date: 29/09/2025
*Corresponding author: Achraf Moussa, Department of Neurosurgery, Avicenne Military Hospital, 40000, Marrakech, Morocco
Abstract
Interhemispheric Subdural Hematoma (IHSDH) is a rare but serious type of intracranial hemorrhage often linked to head trauma, coagulation disorders, and anticoagulant use. This report discusses the case of a 55-year-old woman on anticoagulant therapy who presented with altered consciousness and vomiting. Imaging identified a compressive left Hemispheric Subdural Hematoma (HSDH) with subfalcine herniation alongside an acute IHSDH. The patient underwent surgical evacuation of the left HSDH but unfortunately died from a pulmonary infection a week after surgery. IHSDH typically results from the rupture of bridging veins due to torsional forces or coagulation issues. While CT imaging plays a crucial role in diagnosis, the treatment approach should be tailored based on symptom severity and hematoma size, with conservative management being the primary strategy unless surgical intervention is warranted. This case illustrates the need for prompt recognition and comprehensive management in patients with IHSDH and highlights the importance of multidisciplinary care, especially in individuals receiving anticoagulant therapy. Continued research is essential to enhance treatment protocols for these complex cases.
Keywords: Interhemispheric subdural hematoma; Hemispheric subdural hematoma; Coagulation disorders; Surgical Evacuation
Introduction
IHSDH is a rare and complex type of brain hemorrhage that occurs between the cerebral hemispheres. Although it has been documented in the medical literature, ISDH remains poorly studied due to its low incidence. Its deep location within the brain and potential to cause serious neurological deficits make both diagnosis and treatment particularly challenging [1]. Management of these hematomas often requires a multidisciplinary approach that includes neurosurgical evaluation and supportive care. We report the case of a patient suffering from an IHSDH with a subacute HSDH and review the literature.
Case Report
We report a 55-years-old woman presented with consciousness disorder with vomiting for 2 days. Past history revealed a mitral replacement in 2008 and she had beeing using anticoagulant agent (Acenocoumarol). The neurologic examination revealed a disorder of consciousness was 07/15 assessed by the Glasgow Coma Scale (GCS), pupil in myosis, stiff neck. The biological check-up showed a platelet count was 219,000/mm3, and thrombo test was 55% and an International Normalized Ratio of 1.39. CT (computed tomography) scan of the head showed a left subacute subdural hemispheric hematoma compressive with subfalcoral engagement associated with an acute ISDH (Figure 1). Consequently, we proceeded with the surgical evacuation of the left subdural hematoma via two burr-hole fronto-parietal craniotomy then she was transferred to the intensive careunit. The anticoagulant agent was stopped. The patient is still intubated, the sedation was stopped 3 days postoperatively with no sign of awakening. A control CT scan was performed three days after, showing only the acute IHSDH (Figure 2).
The patient was subjected to thoracic scan following respiratory deterioration, which revealed nosocomial pneumopathy, Unfortunately, the patient died one week later in the intensive care unit of pulmonary infection.
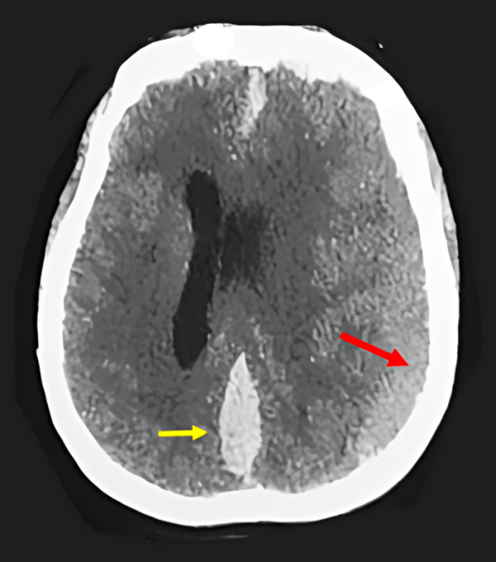
Figure 1: CT-scan of the head showed a left subacute HSDH (yellow arrow) compressive with subfalcoral engagement associated with an acute IHSDH (red arrow).
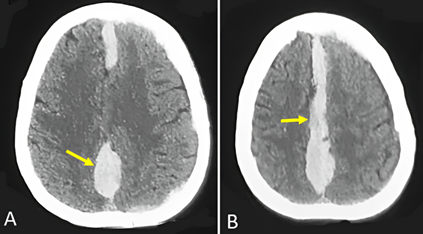
Figure 2: A and B: CT-scan of the head three days postoperatively showing only acute IHSDH without HSDH (arrow).
Discussion
ISDH is usually occur after trauma or in patients with coagulation disorders (e.g., use of anticoagulants). The clinical presentation of patients with ISDH can vary considerably, which can make diagnosis difficult, especially in the absence of risk factors [2].
Cranial trauma is accountable for the bulk of person instances of ISDH, eleven however cerebral aneurysm rupture might also purpose ISH. Intrinsic coagulopathy, anticoagulant therapy, and alcohol abuse were diagnosed as predisposing elements for ISDH. Thirteen Traumatic rupture of bridging veins among the cerebral cortex and the advanced sagittal sinus is the same old mechanism through which ISDH occur. Tearing of cerebral bridging veins has additionally been implicated because the putative mechanism of harm with inside the improvement of different kinds of subdural hematoma after dural puncture and decreased CSF pressure [3].
Computed tomography imaging is taken into consideration the gold preferred for the analysis of ISH and, as found in our patient, commonly demonstrates ISH as a hyperdense fluid series alongside the interhemispheric fissure. A cranial CT test without angiographic assessment can be unreliable seven to 21 days in spite of everything varieties of HSDH (such as ISDH) due to the fact the hematoma and surrounding mind tissue have comparable radiographic density. MRI or cerebral angiography is useful neuroimaging techniques to establish the diagnosis [3].
Spontaneous ISDH was generally associated with coagulopathy. According to multivariate logistic regression analysis, no factor influenced the poor outcome in patients with ISDH. Although surgery was performed to remove the combined lesions in 24% of cases [4].
Although some have recommended surgical treatment [5], the mortality rate of conservative management was lower than that of surgery (10.5% and 31.7%, respectively) [6]. In 50 cases of ISDH, the hematoma resolved within two weeks in 80% of cases [7].
However, surgery may be beneficial, if: 1) there is progression of clinical signs and symptoms, especially worsening weakness of the lower limbs; 2) paralysis of both lower limbs is present; 3) there is a persistent increase in ICP (>30 mmHg); and 4) the hematoma volume is >40 mL and/or the hematoma thickness is >15 mm. Otherwise, conservative treatment is generally preferred. Although the outcomes were poor in conservatively treated patients in this study, this does not mean that surgical treatment was better than conservative treatment [4].
These measures are critical for improving neurological outcomes in a condition associated with high morbidity and mortality.
Patients with ISH have superior outcomes thane patients with convexity SDH, with the latter requiring more intense surgical care and longer inpatient hospital stays, while the previous is mostly managed conservatively with superior outcomes. Takeuchi and colleagues reported factors correlated with poor outcomes in patients with ISH: GCS score, hypovolemic shock, skull fracture, convexity or posterior fossa SDH. Comparable prognostic factors have been reported to be associated with poor outcomes by Wang et al; low GCS at presentation, the source of the hematoma, and greater thickness of hematoma. These factors are in line with our findings of low GCS at presentation being associated with a poorer outcome [8].
In our case, the management consisted of a combined approach to treat an IHSDH associated with a HSDH. The surgical indication was exclusively for subacute HSDH, due to its size and compressive effect, while conservative treatment was chosen for ISDH. This strategy reflects the importance of rigorous clinical and radiological assessment in individualizing treatment decisions.
Conclusion
Interhemispheric subdural hematoma and hemispheric subdural hematoma are a rare type of intracranial hemorrhage associated with various causes, including head trauma and anticoagulant use. It occurs due to the rupture of bridging veins, resulting in blood accumulation, typically unilateral. Early diagnosis using CT scan is essential, as smaller hematomas can resolve on their own while larger ones may require surgical evacuation. Prognosis varies based on the cause and timing of treatment.
References
- Shankar A, Joseph M, Chandy MJ. Interhemispheric subdural hematoma: an uncommon sequel of trauma. Neurol India, 2003; 51(1): 63–64.
- Schilder JC, Weisfelt M. Ataxia associated with an interhemispheric subdural hematoma: a case report. Cases J, 2009; 2: 8876. doi: 10.4076/1757-1626-2-8876.
- Liang MY, Pagel PS. Bilateral interhemispheric subdural hematoma after inadvertent lumbar puncture in a parturient. Can J Anaesth, 2012; 59(4): 389-93. 710.1007/s12630-011-9664-6.
- Ahn JM, Lee KS, Shim JH, Oh JS, Shim JJ, Yoon SM. Clinical Features of Interhemispheric Subdural Hematomas. Korean J Neurotrauma, 2017; 13(2): 103-107. doi: 10.13004/kjnt.2017.13.2.103.
- Glista GG, Reichman OH, Brumlik J, Fine M. Interhemispheric subdural hematoma. Surg Neurol, 1978; 10(2): 119-122.
- Bartels RH, Verhagen WI, Prick MJ, Dalman JE. Interhemispheric subdural hematoma in adults: case reports and a review of the literature. Neurosurgery, 1995; 36: 1210–1214. doi: 10.1227/00006123-199506000-00026.
- Yoo JS, Hu C, Hong SK, Kim HJ, Han YP. Clinical analysis of interhemispheric subdural hemorrhage and tentorial hemorrhage. J Korean Neurosurg Soc, 1991; 20: 13–19.
- Kashif M, Nkrumah-Boateng PA, Hammad EM, Abdullahi HI, et al, The Clinical Presentation, Treatment Modalities, and Outcomes Associated with Interhemispheric Subdural Hematomas. Asian Journal of Neurosurgery, 2025. https://doi.org/10.1055/s-0044-1801770.

