A Pathological Fracture of the Humerus Revealing Rheumatoid Arthritis and Chondrosarcoma in A Diabetic Patient: A Very Rare Association
Ibrahima Amadou Dembélé1, Stéphane Loique Djeugoue1,4,*, Kaly Keïta1, Adama Sinayoko1, Mamadou Cissoko1, Sandra Guerra Puig2, Famakan Sangaré2, Diarra Check Mansour2, Romuald Nounga Nyanké1, Diallo Ousmane2, Oumar Diarra2, Mangane Sambou dit M'Pah2, Souleymane Sy Traoré2, Cissé Moctar Housseini2, Diarra Adama Kampogo2, Florent Mbakilayi Tshitenga5, Soumare Assitan1, Djeri-Alassani Oupidja1, Jordane Anaïs MK Fianyoh1, Samba Camara1, Landouré Sekou1, Aoua Diarra1, Yacouba Koné1, Oumou Dembélé1, Nouhoum Koné1, Moussa Sangaré1, Mamadou Mallé1, Amadou Koné3, Sy Djibril1,3, Djénébou Traoré1,3, Didier Mukeba Tshialala4, Soukho Assétou Kaya1,3, Dembélé Mamadou1,3 and Hamar Alassane Traore1,3
1Internal Medicine Department, University Hospital Center Point G, Bamako, Mali
2Polyclinique les Orangers, Banankoro, Mali
3Endocrinology and Metabolism Department of the Mali University Hospital, Bamako, Mali
4Faculty of Medicine and Odontostomatology, University of Sciences, Techniques and Technologies of Bamako, Mali
5Faculty of Medicine, Pharmacy and Public Health, University of Mbuji-Mayi, Democratic Republic of Congo
6Internal Medicine Department, Faculty of Medicine, Official University of Mbuji-Mayi, Democratic Republic of Congo
Received Date: 27/08/2025; Published Date: 18/09/2025
*Corresponding author: Stéphane Loique Djeugoué, Internal Medicine, University Hospital Center Point G, Bamako, Mali
Abstract
Background: Rheumatoid arthritis (RA) is a chronic autoimmune inflammatory disease whose etiology remains unknown. An inaugural association with cancers is often frequent, notably in this case a chodrosarcoma.
Clinical Case: This article describes the case of a 64-year-old diabetic patient in whom we diagnosed, through the etiological search for a pathological fracture of the left humerus, a rheumatoid arthritis in the state phase (ACR/EULAR 2010 criteria) associated with a central grade III chondrosacromy of the left humerus. It also reviews the existing literature on the various publications reporting this very rare association.
Conclusion: The limited links between autoimmunity and carcinogenesis are being dismantled, as these two events may correspond to facets of the same process. Occult cancer should always be sought in the presence of rheumatoid arthritis with pathological fracture.
Keywords: Rheumatoid arthritis; Chondrosarcoma; Autoimmunity; Cancer; Internal Medicine; Mali
Introduction
Rheumatoid Arthritis (RA) is a chronic autoimmune inflammatory disease whose etiology remains unknown [1]. It is characterized by inflammatory changes in joints, cartilage, and synovitis, with synovitis being a prominent feature of RA [1]. Clinically, RA presents as symmetrical, invasive joint inflammation affecting the small joints of the hands and feet, leading to pain, swelling, and joint stiffness. It predominantly affects women aged 30 to 50, the disease progresses rapidly after onset, resulting in irreversible physical dysfunction and joint deformities [1,2]. Additionally, RA patients may exhibit extra-articular manifestations involving various organs, including interstitial lung disease, pericarditis, pleural effusion, or bronchiectasis. Importantly, RA patients have a higher risk of serious infections, respiratory diseases, osteoporosis, cardiovascular diseases, cancer, and mortality compared to the general population [2].
In a retrospective analysis involving nine patients presenting with musculoskeletal pain as their initial symptom, subsequent diagnoses revealed various malignancies, including acute lymphoblastic leukemia, acute myeloid leukemia, lymphoma, neuroblastoma, and Ewing’s sarcoma [3]. Notably, RA was initially diagnosed in four of these cases [3]. Another comprehensive retrospective study spanning 14 years examined 29 pediatric patients with malignancies, encompassing lymphoma, Ewing’s sarcoma, and other malignancies. Surprisingly, initial diagnoses of rheumatoid arthritis were made in 12 of these cases [3]. It is worth noting that individuals with RA exhibit an elevated overall incidence of malignancies, with a 5–10% increased risk compared to the general population [3,4]. In a literature review,
Chondrosarcoma (CS) is the second most common primary malignant bone tumor in adults after osteosarcoma [13]. Its incidence is approximately 0.1/100,000 cases per year, with a peak between the ages of 30 and 60 years and a male to female ratio of 1 [13]. It is very rarely associated with non-organ-specific autoimmune diseases, particularly rheumatoid arthritis. Very few cases of this presentation have been reported in sub-Saharan Africa. Thus, we describe one of the rare cases of a diabetic patient with rheumatoid arthritis associated with chondrosarcoma revealed by a pathological fracture of the humerus.
Observation
We report the case of a 64-year-old Malian woman, a housewife. She was admitted on June 21, 2025, for pain in the left arm.
The onset of the symptoms dates back to one day, marked by the sudden onset of sharp pain in the left arm, without any notion of trauma, of high intensity estimated at 9/10 according to the visual analogue scale ; without triggering factors, non-radiating, aggravated by mobilization, calmed by taking tramadol + paracetamol and rest, associated with functional impotence of the homolateral upper limb. These symptoms were preceded more than a month ago by generalized joint and muscle pain, with a gradual onset, predominantly in the shoulders, elbows, wrists, hands (with difficulty carrying everyday objects during peak pain), and symmetrically in the knees. The pain was of variable intensity (between 5 and 8/10 on the global numerical scale), without radiation, triggered spontaneously or by movement, aggravated by movement, relieved by tramadol + paracetamol and rest, and without associated functional impairment. All of this occurs in a context of unquantified fever for over 3 months, with a gradual onset, intermittent, and without a specific schedule, without hyperhidrosis, or cough ; non selective anorexia, physical asthenia rated at 7/10 on the global numerical scale, and significant unquantified weight loss for over a year. As no therapeutic approach has been undertaken, she decides to consult us for treatment. In addition to her medical history, she has intermittent crampy epigastralgia of moderate intensity according to the simple verbal scale, without radiation, without associated ascending gastric reflux, triggered by hunger, relieved by meals or esomeprazole, occurring periodically throughout the year. She has a feeling of early satiety, moderate polyuria, predominantly nocturnal, associated with polydipsia, and palmoplantar tingling with a sensation of walking on a sponge when walking barefoot on the ground.
As background ; she has been diabetic for about 9 years in irregular care but currently on Mixtard 30, hypertensive for 4 years in regular care, a catarct of the left eye for 3 years ; undocumented ulcer syndrome and lumbar osteoarthritis and bilateral knee osteoarthritis for 7 years. From a diabetic and hypertensive father, a diabetic cousin, she is the 6th gesture, 6th parity, 6 livings children including 2 fetal macrosomia (4000kg for the 5th parity and 4150 kg for the 6th parity) ; married in a monogamous regime. She reportedly took tramadol + paracetamol (37.5/325mg) one tablet morning and evening, Mixtard 30, 12 IU morning and evening subcutaneously, amlodipine + perindopril (5/5mg) one tablet daily in the morning, esomeprazole (40mg) one capsule every morning, thirty minutes before breakfast, and chlordroitin sulfate (400mg) one capsule morning and evening. She drinks coffee and her diet consists mainly of cereals, fish, red meat (beef, sheep essentially), wheat flour, rice, peanuts, fruit, and a low-sodium diet.
The general examination revealed a conscious, bedridden, athletic patient with fever to touch ; her Karnofsky index was 80%. Her sitting blood pressure in the left arm was 136/74 mmHg ; her heart rate was 106 bpm ; her respiratory rate was 18 cycles per minute ; her left axillary temperature was 37.8°C ; and her random capillary blood glucose on admission was 2.47 g/L ; On the urine strip, glucosuria 2 crosses and ketonuria none. Her measurements on admission were as follows : weight 52 kg, height 163 cm, and a body mass index of 19.57 kg/m² ; SpO2 95% on room air.
On physical examination, the patient presented with a Dessault posture, with painful swelling in the left arm, reduced mobility of the left upper limb with functional impairment of the left arm, no local warmth, and crepitus. Mobility of all five fingers was preserved. The remainder of the physical examination revealed bilateral "wind-like" ulnar deformity of the fingers in both hands ; mallet deformity of the 2nd, 3rd, and 5th fingers of the right hand. Both thumbs were permanently abducted with discomfort in pronation-supination (Image 1). Symmetrical tenderness of the intercarpal, metacarpophalangeal, and proximal interphalangeal joints in both hands. Poor spinal straightness, the bell sign present in the L5 and S1 regions, and the Lazèque maneuver was positive in both lower limbs. A retraction of the left nipple. The other devices were carefully examined and did not present any abnormalities.
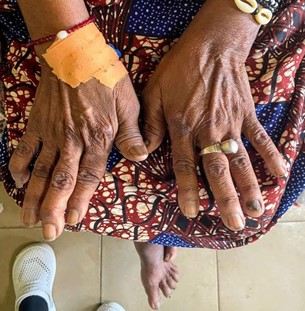
Picture 1: Pictures of the patient's hands showing deformations secondary to rheumatoid arthritis.
Biological examinations were carried out at the entrance:
- Mild, microcytic, normochromic anemia with a hemoglobin level of 12.1 g/dL, a mean corpuscular volume of 79.6 flL, and a mean corpuscular hemoglobin concentration of 32.8 g/dL. Platelets at 296,000/mm3.
- Inflammatory syndrome with a CRP of 31.16 mg/L, an ESR of 67 mm/h (1st hour) and 99 mm/h (2nd hour), and hyperferritinemia at 609.4 ng/mL. Leukocytosis at 12,470/mm³ with a predominance of polymorphonuclear neutrophils at 9,400/mm³.
- Serum creatinine at 73 µmol/L with a clearance of 107.99 mL/min. Serum azotemia at 3.9 mmol/L, serum uric acid at 3.7 mg/dL, and HbA1c at 8,34%. Total protein at 66.5 g/L, hypoalbuminemia at 35.01 g/L. CPK at 102 IU/L, prothrombin time at 91%. ALAT at 19 IU/L and ASAT at 28 IU/L ; plasma electrolytes normal, PTH normal at 21.55 pg/ml ; vitamin D at 31.08 ng/ml ;
- Serum protein electrophoresis normal with total protein at 6.59 g/dL and albumin (3.89 g/dL) ; albumin/globulin ratio at 1.44.
- Immunological assessment : antinuclear antibodies (ANA-Screen) at 0.50 (negative) ; anti-SSA antibodies not detected ; anti-SSB not performed, anti-Sm 1.20 iu/mL (negative), anti-CCP 36.21 iu/mL (positive), anti-native DNA 14.58 iu/mL (negative). Complement testing was requested but not performed, rheumatoid factor 8.3 iu/mL (positive threshold of approximately 20 iu/mL). ASLO negative, total anti-HBc antibodies positive, HIV1-2 and HCV serologies negative ; HBsAg negative. A cryoglobulin test was requested but not performed.
- Tumor markers : Alpha-fetal protein at 20 ng/mL ; CA 15-3 at 38.95 u/ml (Raised)
- Parasitology : a positive thick blood smear with 80 trophozoites/microliter of blood
The X-ray of the left upper limb (Image 2) revealed :
- a minimally displaced fracture of the upper third of the humeral shaft with an excluded fragment
- bone demineralization of the shoulder and humerus related to osteoporosis
- narrowing of the left glenohumeral and acromioclavicular joints with osteosclerosis of the articular surfaces related to left osteoarthritis
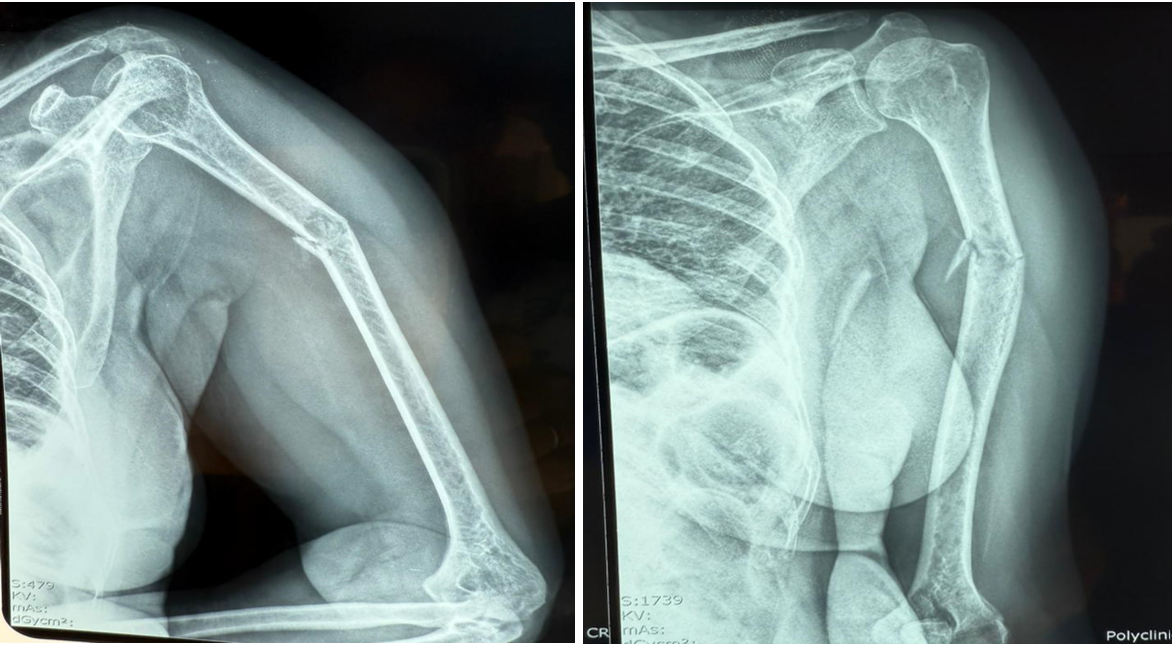
Picture 2: The X-ray of the left upper limb.
The anatomopathological examination of the bone biopsy (Image 3) revealed fragments of connective tissue, a tumor process made up of areas of atypical chondrocytes, and infiltration of the soft tissue related to the histological appearance of a grade III chondrosarcoma.
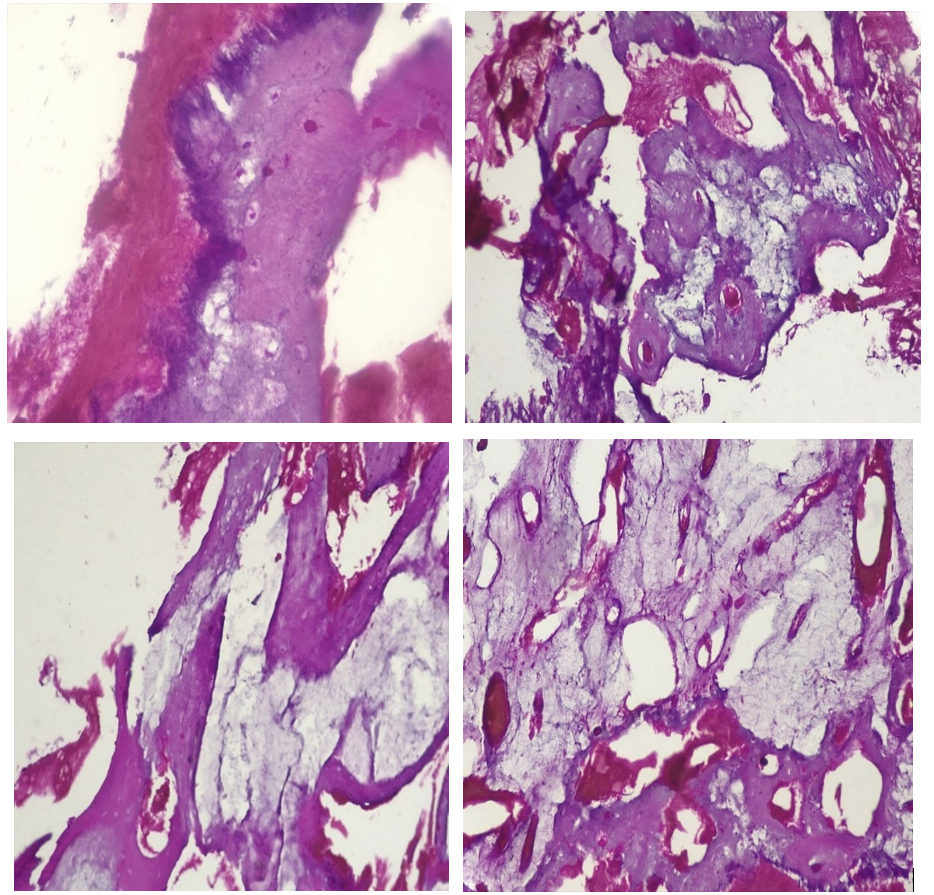
Picture 3: The anatomopathological examination of the bone biopsy.
On breast ultrasound : a bilateral BIRADS 1 breast ultrasound appearance associated with varicose dilation of the upper-outer quadrant of her right breast related to a varicose vein. The patient had a bone mineral density with a z-score of -3.4, indicating severe osteoporosis with a high risk of fracture. The thoraco-abdominopelvic CT scan at the entrance revealed no abdomino-pelvic lesions of the solid organs detectable today, a severe biconcave vertebral fracture (grade 3) staged with a suspicious appearance from L1 to L4.
We therefore retained the diagnosis of glycemic imbalance with the following contributing factors:
- rheumatoid arthritis in the state phase, with a score of 8/10 according to the ACR/EULAR 2010 classification criteria (excluding psoriatic arthritis, viral arthritis, gout, calcium pyrophosphate dehydrate rheumatism, and systemic lupus). The DAS 28-ESR score was 5.1, indicating high activity. The functional impact assessment using the HAQ index showed severe functional impact with an HAQ index of 2.8.
- Chondrosarcoma of the left humerus with probable vertebral infiltration
- uncomplicated malaria
The patient was hospitalized, put on MIXTARD ® 30 at a dose of 10 IU every 12 hours, injectable omeprazole 40 mg every 24 hours for the prevention of stress gastritis, enoxaparin 4,000 IU subcutaneously daily, 0.9% saline 500 ml every 8 hours. Injectable Tramadol 100 mg every 8 hours intramuscularly, Methotrexate 7.5 mg/week combined with folic acid 10 mg every week (48 hours after methotrexate) ; arthemether-lumefantrine (80/480) 1 tablet morning and evening (8 hours between the first and second doses, then every 12 hours) for 3 days, chondroitin sulfate 400 mg every 8 hours, and Alendronate 70 mg tablet, one tablet every tuesday at 9 a.m.weekly. She underwent osteosynthesis surgery with placement of an intramedullary fixator with a shoulder orthosis for support. She was put on Ciprofloxacine 500mg every 8 hours for 15 days and began oncological management. Daily supportive psychotherapy and therapeutic education for the patient and her family were provided.
Discussion
This observation reports a very rare case of association between a non-organ-specific autoimmune disease and a solid cancer in a patient with diabetes mellitus ; notably an association of rheumatoid arthritis (RA) in the state phase and a chondrosarcoma. Prior research has revealed a heightened prevalence of neoplasms in individuals diagnosed with rheumatoid arthritis [3]. Simon et al.'s 2015 meta-analysis studied the incidence of cancer in the population of patients with rheumatoid arthritis compared to the general population [4], the risk of developing cancer was increased by 10%, for all cancers combined [4]. In subgroup analyses, there was a significant increase in incidence for lymphomas, lung cancers, and non-melanoma skin cancers. The main risk factor was rheumatic disease activity [4]. For other cancers, the incidence rate did not appear to be increased, except for skin cancers, where there may be an increased risk [4]. For hematological diseases, the overall risk was multiplied by 2.46 [2.05-2.96] for lymphoma, by 3.21 [2.42–4.27] for Hodgkin's disease and by 2.26 [1.82-2.81] for non-Hodgkin's lymphoma [4]. Baecklund et al, showed that high RA activity was a risk factor for developing lymphoma [4].
Patients with RA have a 1.64-fold [1.51–1.79] increased risk of developing lung cancer compared to the general population [4]. Tobacco is a risk factor for developing lung cancer and RA in predisposed populations, by inducing the production of anti-CCP antibodies [4]. Furthermore, chronic pulmonary inflammation due to rheumatism may explain this increase in lung cancer. Choi, reported in thier study that Overall, malignancies occurred in 170 (5.5%) and 662 (5.4%) participants in the RA group (n = 3070) and without the RA group (n = 12,280), respectively [8]. In the RA group, the five most commoncancers were lung, thyroid, gastric, colorectal, and hepatic cancer (1.77, 1.64, 1.59, 1.26, and 0.65 incidence rate per 1000 person-years, respectively) [8]. Thus, chondrosarcoma is classically very rarely reported as a solid cancer associated with rheumatoid arthritis (Figure 1). Hence the interest in presenting our observation.
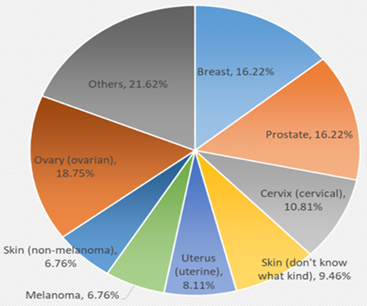
Figure 1: Type of cancers for patients with rheumatoid arthritis [9].
Yang and his team objectified in their study that, the results from the Mendelian randomization (MR) analysis revealed that there was no significant genetic association between RA and benign neoplasm of bone and articular cartilage (BNBAC) (p = 0.427, odds ratio [OR] 95% confidence interval [CI] = 0.971 [0.904–1.044]) [3]. However, a positive genetic association was observed between RA and malignant neoplasm of bone and articular cartilage (MNBAC) (p = 0.001, OR 95% CI = 1.413 [1.144–1.745]) [3]. The findings of this study demonstrate that RA constitutes a significant risk factor for MNBAC. In the context of clinical application, it is advisable to conduct MNBAC screening in RA patients and remain vigilant regarding its potential manifestation.
Pfitzenmeyer et al. reported 12 cases of polyarthritis, the paraneoplastic nature of which was likely given a parallel course of the disease with the cancer ; the average age of the patients was 61 years, and the joint manifestations preceded the cancer diagnosis [5]. The clinical features are the frequent presence of a marked alteration in the general condition, a high fever, and an explosive onset of joint involvement ; the polyarthritis is seropositive in 1 out of 2 cases, and the usual presentation is that of classic rheumatoid arthritis with bilateral and symmetrical distal involvement but without joint erosion [5].
The immune system plays a pivotal role in the pathogenesis of tumors, exerting multifaceted and intricate influences [8]. Certains types of tumors exhibit a heightened incidence of chronic inflammation and infection, establishing a clear connection between tumor development and these immunological factors [8]. RA, an autoimmune disease characterized by abnormal lymphocyte activity and the generation of autoantibodies against self-antigens, is associated with suppressed immune function [10]. Consequently, dysfunctional immune surveillance and immunosuppression are recognized as risk factors for various types of cancer [10]. The main hypothesis is that chronic immunological stimulation would increase the malignant transformation of immune system cells and reduce the number of suppressor T lymphocytes, thus increasing rates of lymphoma malignancy in patients with RA [8,11]. Moreover, the utilization of immunosuppressants is linked to an increased susceptibility to tumors. The etiology of tumor risk in RA patients may involve genetic predisposition and gene-environment interactions [10]. Furthermore, the usage of antirheumatic medications is associated with the tumor risk in RA patients [10].
Chondrosarcoma (CS) is the second most common primary malignant bone tumor in adults after osteosarcoma [12]. Chondrosarcomas account for 20% of all bone sarcomas, and the peak incidence occurs between the ages of 30 and 60 [6]. The long bones of the hand are involved in 40 to 65% of cases, followed by the major long bones (femur, humerus, and tibia), which account for approximately 25% of cases, and the small bones of the foot (7%) [12,13]. These tumors, with an estimated incidence of 1 in 200,000 per year, are characterized by the production of a cartilaginous matrix by tumor cells, poor vascularization, and a low percentage of dividing cells [12]. Chondrosarcoma is a heterogeneous group of tumor ; as a consequence many chondrosarcoma subtypes are described [12]. More than 90% of chondrosarcoma are conventional chondrosarcoma [12]. Among these, 90% are low grade to intermediate grade tumors; the remaining 5-10% are grade 3 lesions with high metastatic potential [12]. Conventional chondrosarcoma are sub-classified as central when they arise within the medullary cavity or as peripheral when they arise from the surface of the bone [12].
- Central CSs can be primary (85% of cases), or secondary to a solitary chondroma, or as part of Ollier disease or Maffucci syndrome [13]. They develop within the medullary cavity and are most commonly found in the proximal femur, pelvis, and proximal humerus [13].
- Peripheral CSs develop from the cartilaginous cap of an osteochondroma and are mainly located in the pelvis or shoulder girdle [13].
In addition to the morphologic classification, chondrosarcomas can be classified into 3 histologic grades, depending on findings of cellularity, atypia, and pleomorphism [12] : Grade I (low grade) cytologically similar to enchondroma (lesions rarely metastasize) ; Grade II (intermediate grade) characterized by a definite and increased cellularity ; Grade III (high grade) characterized by high cellularity, prominent nuclear atypia, and the presence of mitosis. In our case, it was a grade III central chondrosarcoma.
Survival of chondrosarcoma varies considerably across the large number of subtypes and histologic grades of these tumors [12]. Patients with adequately resected low-grade chondrosarcomas have an excellent survival rate. In general the survival of patients with high-grade tumors varies depending on the location, subtype, effectiveness of surgical treatment, size and stage of the tumor [12]. Due to their low mitotic activity and vascularization, SCs are usually refractory to chemotherapy and radiotherapy [12]. Surgical treatment is therefore the only therapeutic option. For intermediate- and high-grade lesions, en bloc resection with margins > 4 mm is the preferred option [13].
Conclusion
It appears from our observation that there are limited links between autoimmunity and carcinogenesis are being dismantled, as these two events could correspond to facets of the same process. However, the mechanisms of autoimmunity in solid cancers are more obscure. These autoimmune pathologies do not necessarily behave like a true paraneoplastic syndrome ; their progression may be different from that of the tumor pathology. As a general rule, occult cancer should be suspected in the presence of polyarthritis. The current challenge is the identification of reliable predictive markers to identify occult cancers in the presence of an autoimmune manifestation linked to the existence of cancer.
Additionnal Information
Declaration of patient consent: Written informed consent was obtained from the patient’s family to publish this report in accordance with patient consent policies. In this report, the patient has consented to the publication of his images and other clinical information in the journal.
Competing Interests: The authors declare no conflict of interest.
Authors’ Contributions: All authors participated in the evaluation and follow-up of the patient, in the writing and correction of the case report. All the authors of the manuscript have read and agreed to its content.
Competing interests: None declared
Funding: No funding was required in the preparation of this manuscript
References
- Thomas B, Pascal R, Philippe D, Huguette L, Philippe O, Frédéric L. Manifestations systémiques de la polyarthrite rhumatoïde. Dans : Loïc Guillevin, Olivier Meyer, Éric Hachulla, Jean Sibilia, eds. Traité des Maladies et Syndromes Systémiques. 6e édition, Paris : Lavoisier, 2015; 434-489.
- Bardin T, Bouchaud-Chabot A. Manifestations systémiques de la polyarthrite rhumatoïde. Dans : Marcel-Francis Kahn, André Paul Peltier, Olivier Meyer, Jean-Charles Piette, eds. Maladies et syndromes systémiques. Paris : Flammarion Médecine-Sciences, 2000; 397- 432.
- Mingyi Yang, Yani Su, Ke Xu, Jiale Xie, Pengfei Wen, Lin Liu, et al. Rheumatoid arthritis increases the risk of malignant neoplasm of bone and articular cartilage : a two-sample bidirectional mendelian randomization study. Arthritis Research & Therapy, 2023; 25: 219.
- Amélie W. Risque de cancer chez les patients atteints de polyarthrite rhumatoïde traités par tocilizumab : données extraites du registre national REGATE. Thèse : Med : Université de Montpellier, 2021; p182.
- Pasquet F, et al. Maladies auto-immunes et cancers. Deuxième partie : maladies auto-immunes au cours des cancers et de leur traitement. Rev Med Interne, 2014. http://dx.doi.org/10.1016/j.revmed.2014.04.004.
- Choi HG, Kang HS, Lim H, Kim J-H, Kim JH, Cho S-J, et al. Potential Cancer Risk in Patients with Rheumatoid Arthritis: A Longitudinal Korean Population-Based Analysis. J. Pers. Med, 2022; 12: 965. https://doi.org/10.3390/jpm12060965.
- Bhandari B, Basyal B, Sarao MS, et al. Prevalence of Cancer in Rheumatoid Arthritis : Epidemiological Study Based on the National Health and Nutrition Examination Survey (NHANES). Cureus, 2020; 12(4): e7870. DOI: 10.7759/cureus.7870.
- Shuai Yuan, Jie Chen, Xixian Ruan, Mathew Vithayathil, Siddhartha Kar, Xue Li, et al. Rheumatoid arthritis and risk of site-specific cancers : Mendelian randomization study in European and East Asian populations. Arthritis Research & Therapy. https://doi.org/10.1186/s13075-022-02970-z.
- Tai Patricia, Yu Edward, Joseph Kurian, Miale Thomas. "A Review of Autoimmune Diseases Associated with Cancer" Oncology Publications, 2010; 70. https://ir.lib.uwo.ca/oncpub/70.
- Teresa A Simon, Adam Thompson, Kunal K Gandhi, Marc C Hochberg, Samy Suissa. Incidence of malignancy in adult patients with rheumatoid arthritis : a meta-analysis. Arthritis Research & Therapy, 2015; 17: 212. DOI: 10.1186/s13075-015-0728-9.
- Soldin I, Pereira N. Autoimmunity and Cancer : Two Stations on the Same Continuum. Cureus, 2024; 16(2): e54317. DOI: 10.7759/cureus.54317.
- François S. Implication of immune system in chondrosarcoma progression and therapeutic response. Could immunotherapy play a role in chondrosarcoma treatment ? Thèse : Doctorat : Université Claude Bernard Lyon 1, 2016; 2016 LYSE 1073: p197.
- Hadrien S, Thierry RF, Sana B, Didier H. Tumeurs cartilagineuses. Rev Med Suisse, 2018; 14: 2259-2263.
- Stevenson JD, Laitinen MK, Parry MC, et al. The role of surgical margins in chondrosarcoma. Eur J Surg Oncol, 2018; 44: 1412-1418.
- De Andrea CE, San-Julian M, Bovee J. Integrating morphology and genetics in the diagnosis of cartilage Tumors. Surg Pathol Clin, 2017; 10: 537-552.

