The Symptom Masquerade: Narcolepsy or A Psychiatric Disorder?
An Mariman1,2,* and Lammers Gert Jan3,4
1Department of Psychiatry and Department of Physical Medicine and Rehabilitation, Ghent University Hospital, Corneel Heymanslaan 10, Ghent B-9000, Belgium
2Faculty of Medicine and Health Sciences, Ghent University, Corneel Heymanslaan 10, Ghent B-9000, Belgium
3Department of Neurology, Leiden University Medical Centre, Leiden, the Netherlands
4Sleep Wake Centre, Stichting Epilepsie Instellingen Nederland (SEIN), Heemstede, the Netherlands
Received Date: 25/08/2025; Published Date: 17/09/2025
*Corresponding author: An Mariman, Department of Psychiatry and Department of Physical Medicine and Rehabilitation, Ghent University Hospital, Corneel Heymanslaan 10, Ghent B-9000, Belgium; Faculty of Medicine and Health Sciences, Ghent University, Corneel Heymanslaan 10, Ghent B-9000, Belgium
Abstract
Narcolepsy is often misdiagnosed due to overlapping psychiatric symptoms and absence of cataplexy. A 24-year-old man presented with severe fatigue, daytime sleepiness, concentration problems and vivid, frightening dream-like experiences. Polysomnography and multiple sleep latency testing revealed short sleep latencies and SOREMs, leading to a probable diagnosis of Narcolepsy Type 2 (NT2). After treatment with classical stimulants failed, modafinil was initiated. Shortly thereafter, mood instability occurred, culminating in a manic-psychotic episode. Despite the resolution of psychosis, sleep-related complaints, anhedonia and fatigue persisted. Cerebrospinal fluid analysis later revealed a hypocretin-1 concentration ≤ 110 pg/ml, confirming Narcolepsy Type 1 (NT1). This case highlights diagnostic challenges posed by narcolepsy with psychiatric overlap. The presence of mood instability and psychotic features often leads to diagnostic uncertainty and repeated reassessments, especially when classic stimulants are ineffective. CSF hypocretin-1 analysis provided crucial neurochemical confirmation. A transdisciplinary approach improves recognition and leads to safe, individualized treatment.
Keywords: Narcolepsy; Excessive daytime sleepiness; Hypnagogic hallucinations; Modafinil-induced mania; Psychotic symptoms; Diagnostic uncertainty
Introduction
Narcolepsy is a chronic sleep-wake disorder characterised by excessive daytime sleepiness (EDS), hypnagogic/hypnopompic hallucinations, sleep paralysis, disturbed night-time sleep and the only specific symptom, cataplexy. The presence of cataplexy facilitates diagnosis, but some patients never develop cataplexy and suffer from so-called NT2. Hypocretin-1 deficiency is typically associated with the presence of cataplexy and defines the diagnosis of NT1. However, it also occurs in a minority of people with NT2. In these people, it usually predicts the future onset of cataplexy. This means that NT1 represents a homogeneous organic brain disorder. In contrast, NT2 may be a precursor to NT1, if hypocretin-1 deficiency is found, but this phenotype can also be caused by chronic sleep deprivation, shift work, severe disruption of the circadian rhythm and possibly mood disorders, among other unknown causes [1].
Despite the neurobiological basis of narcolepsy, particularly the deficiency of hypocretin-1, which distinguishes this condition from primary psychiatric disorders, its clinical presentation often overlaps with mood, anxiety, developmental, and psychotic disorders. This overlap often leads to misdiagnosis, delaying the recognition and treatment of narcolepsy or psychiatric disorders [2,3].
If present, cataplexy may be misinterpreted as a conversion or dissociative symptom, and hypnagogic hallucinations may be mistaken for perceptual disturbances associated with psychosis, and sleep paralysis may resemble panic-related somatic experiences [4, 5]. EDS is commonly attributed to depression or attentional disorders, prompting psychiatric pharmacotherapy trials that fail to address the underlying sleep pathology [2]. These diagnostic missteps contribute to prolonged clinical uncertainty and may compound psychiatric distress [3].
This case report illustrates such diagnostic ambiguity. The report emphasizes the importance of recognizing sleep-related phenomena within psychiatric contexts and advocates for an integrated diagnostic approach.
Case Report
A 24-year-old male patient was referred to the sleep clinic for evaluation of pronounced fatigue, exhaustion and irresistible episodes of daytime sleepiness and attention problems. His sleep history was notable for sleepwalking until the age of 14, accompanied by persistent somniloquy. There was a hetero anamnesis of “choking” during the night. Partly due to the presence of obesity, the initial suspicion focused on Obstructive Sleep Apnea (OSA).
A diagnostic polysomnography (PSG) revealed a normal total sleep time, a short sleep latency, presence of a sleep-onset REM period (SOREMP) (Figure 1), cyclical sleep architecture, frequent arousals and somniloquy without associated snoring, apnea, or hypopnea.
Multiple sleep latency testing (MSLT), following PSG, demonstrated sleep in all four nap opportunities with a mean sleep latency of 7 minutes and SOREMP in two naps, consistent with a central disorder of hypersomnolence.
The presence of SOREMP during the PSG session and the MSLT, combined with pronounced daytime sleepiness and the absence of cataplexy, indicated narcolepsy type 2, although the differential diagnosis also included chronic sleep deprivation, circadian rhythm disorders (e.g., shift work disorder) and a mood disorder.
Further Evaluation and Diagnostic Workup
Structured screening provided no information pointing to chronic sleep deprivation or shift-work disorder. However, there were indications for a mood disorder: anhedonia and symptoms of sadness and hopelessness over the prior two weeks [6]. The patient also described intermittent but vivid disturbances during the transition to sleep occurring once or twice monthly. He recounted:
“As I’m drifting off, I often see a black shadow looming over me. I’m in my own bedroom, and it looks like someone I know. I become terrified. Sometimes I hear moans or a scream—quiet but eerie, like a movie soundtrack. The shadow slowly grows and hovers above me. At times I feel I can’t breathe, as if it’s suffocating me. I want to scream but can’t, and I’m completely frozen. Only when I’m fully awake do I realize there was no ghost or person in my room. Yet it felt so real and so frightening.”
This experience was clinically interpreted as hypnagogic hallucinations, a recognized phenomenon in narcolepsy.
General physical examination and routine laboratory investigations were unremarkable.
The absence of CSF hypocretin-1 data and lack of cataplexy precluded confirmation of narcolepsy type 1. Instead, the clinical picture was consistent with narcolepsy type 2 according to ICSD-3 TR criteria [7].
Genetic testing demonstrated HLA-DR2/DQB1*0602 positivity, a finding frequently associated with narcolepsy, though not specific to type 2.
Treatment Course and Follow-Up
Central nervous system stimulants, including pemoline and methylphenidate, were initiated to manage EDS but proved ineffective, despite adequate dosing. Persistent fatigue, sleep attacks coincided with anhedonia and clinophilia, raising clinical suspicion of a comorbid mood disorder.
Given the limited efficacy of a trial with a selective serotonin reuptake inhibitor (SSRI) in targeting mood-related symptoms and EDS, modafinil (Provigil) was introduced. As a wake-promoting agent with a more targeted mechanism of action, modafinil resulted in improved daytime vigilance and a reduction in sleep attacks. The combination strategy also allowed for gradual tapering of amphetamine derivatives.
At follow-up, the patient reported a partial clinical response, particularly in cognitive alertness and daily functioning. Residual fatigue persisted but had become manageable, and the hypnagogic hallucinations were less frequent and less distressing. No side effects were reported.

Figure 1: hypnogram demonstrating a sleep-onset REM period.
Clinical Complications and Diagnostic Clarification
Following combined treatment with modafinil and prior psychostimulants, the patient developed symptoms of hypomania rapidly progressing into a full manic episode. Given modafinil's activity as a dopamine transporter inhibitor, its role in precipitating mood elevation and destabilization was considered a probable contributing factor. Psychostimulants are known to modulate dopaminergic transmission and carry a documented risk of inducing psychotic states, particularly in susceptible individuals [8].
Upon resolution of the acute psychotic episode, the patient was re-evaluated at the sleep clinic for underlying narcolepsy. New clinical history revealed profound exhaustion, cognitive impairments, depressive and anxious symptoms, and intrusive dark thoughts, without suicidal ideation. Hypnagogic hallucinations persisted, occurring at sleep onset, while no features suggestive of cataplexy were reported.
At the time of psychiatric hospital admission, the patient met criteria for a psychotic disorder, with documented delusions, hallucinations, and manic affective symptoms. Upon reassessment at the sleep clinic, psychotic features had remitted. Nevertheless, the sleep-onset hallucinations, characteristic of narcolepsy and typically not requiring targeted intervention, remained present.
To clarify the diagnosis amidst ongoing mood symptoms and a complex treatment history, Cerebrospinal Fluid (CSF) analysis was performed, revealing a hypocretin-1 concentration of ≤ 110 pg/mL, confirming the suspected diagnosis of narcolepsy, despite the absence of cataplexy. This neurochemical finding provided definitive evidence supporting the initial clinical impression. At follow-up, psychotic features had resolved, though mood disturbances persisted and required ongoing monitoring.
Discussion
This case highlights the diagnostic complexity surrounding narcolepsy, particularly in the absence of cataplexy and when clinical features overlap with psychiatric syndromes. The patient's initial presentation, marked by irresistible daytime sleep attacks, sleep fragmentation, hypnagogic hallucinations, fatigue and impaired attention, reflected hallmark symptoms of narcolepsy, yet the absence of cataplexy and initial therapeutic response to stimulants delayed definitive recognition.
Misattribution of symptoms to mood disorders and adjustment reactions is common in narcolepsy, especially when presentations include fatigue, anhedonia, and clinophilia. Hypnagogic hallucinations may resemble psychotic perceptual disturbances (table 1), while sleep paralysis is often misconstrued as panic-related or dissociative. In this case, neuropsychiatric overlap led to treatment with antidepressants and stimulants, which ultimately exacerbated mood instability and precipitated a manic-psychotic episode.
The progression to hypomania and mania following modafinil administration illustrates the affective destabilization potential of wake-promoting agents, likely through dopaminergic pathways in vulnerable individuals.
Despite pharmacological complications, subsequent reevaluation of sleep-related symptoms and persistence of hypnagogic hallucinations prompted further investigation. The eventual detection of a low Cerebrospinal Fluid (CSF) hypocretin-1 concentration (≤ 110 pg/mL) provided neurochemical confirmation of narcolepsy, substantiating the prior clinical suspicion. Although cataplexy remained absent, the hypocretin deficiency supports a diagnosis of narcolepsy type 1, suggesting that cataplexy may emerge later or be overlooked due to subtle expression.
This case emphasizes the importance of maintaining a high index of suspicion for sleep disorders in psychiatric presentations, particularly where symptoms defy conventional diagnostic boundaries or show incomplete treatment response. Integration of sleep medicine into psychiatric evaluation, through tools such as PSG, MSLT, and when indicated, CSF hypocretin analysis, can improve diagnostic accuracy and patient outcomes. This is especially pertinent considering emerging therapeutic options, including hypocretin receptor agonists, which hold promise for causal treatment of narcolepsy [9]. In the context of current symptomatic therapies, particular stimulants and wake-promoting agents, clinicians must also remain vigilant for potential iatrogenic complications, particularly in patients with comorbid mood instability.
Ultimately, this patient’s trajectory illustrates the clinical utility of a transdisciplinary approach and the need for individualized treatment strategies grounded in neurophysiological evidence rather than symptom-based assumptions.
Table 1: Conditions that are (or may be) associated with hallucinations.
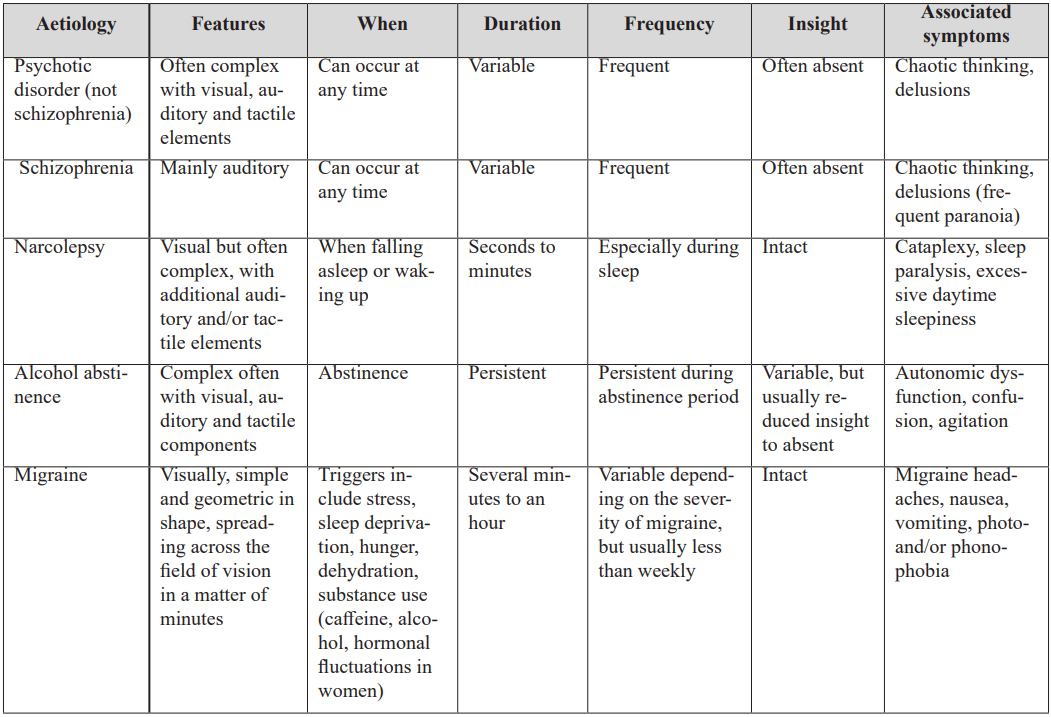
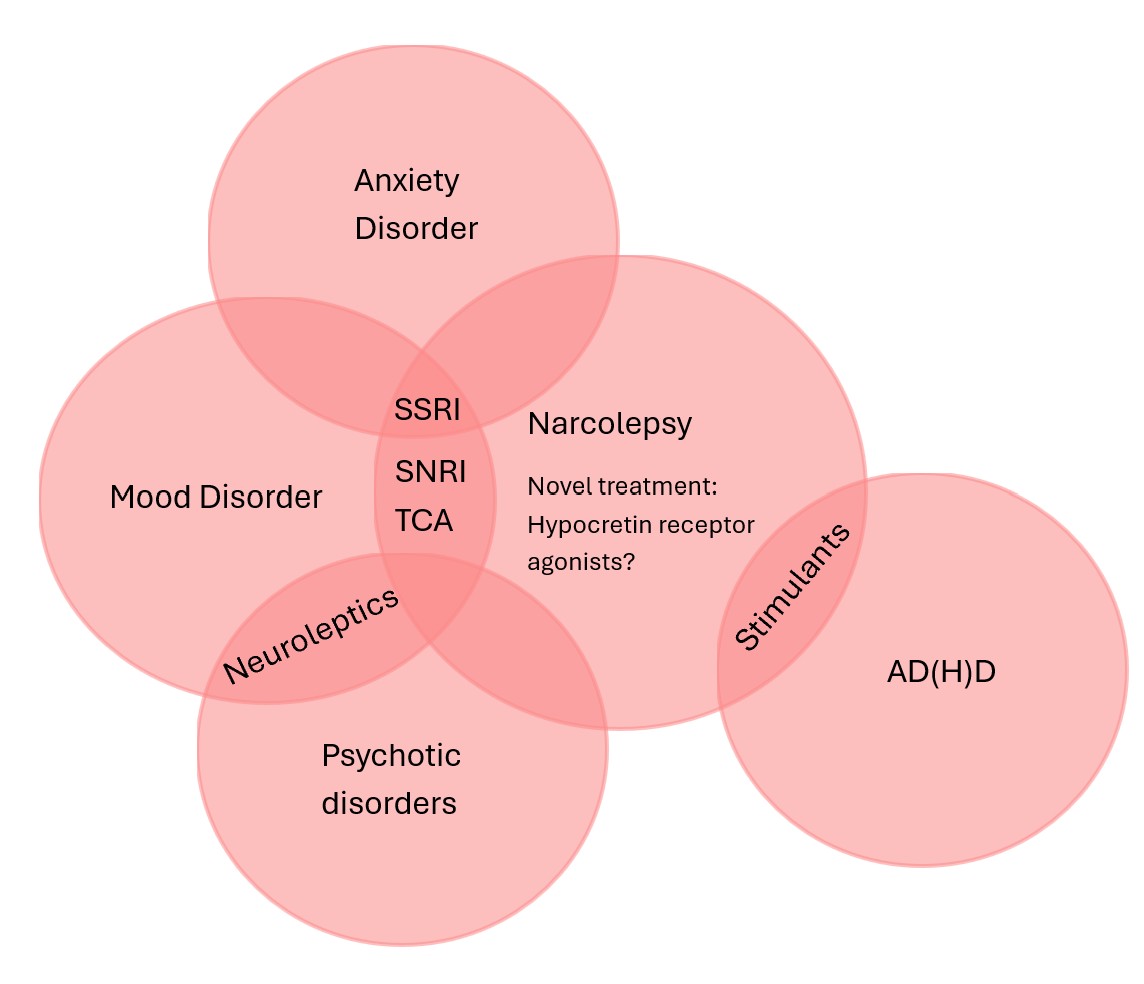
Figure 2: Overlap/relationship between various psychiatric disorders and narcolepsy.
Conclusion
This case highlights the diagnostic challenges associated with narcolepsy, particularly when symptoms resemble psychiatric disorders. Figure 1 illustrates the potential areas of overlap. The presence of mood instability as well as psychotic features, whether iatrogenic or not, often led to diagnostic uncertainty and repeated reassessments. Neurochemical confirmation via CSF hypocretin-1 was pivotal in clarifying the diagnosis. A transdisciplinary approach, combining sleep medicine and psychiatry, is essential to improve timely detection and guide safe, individualized therapy. Furthermore, patients with a confirmed diagnosis of narcolepsy may develop psychiatric disorders later in life, highlighting the need for continued vigilance and regular psychiatric assessment and support throughout the disease course.
References
- Vlasiadis K, Vlasiadis Z. Health Facility Management Strategies for Economic Development. Anna Clin Rev Cas Rep, 2024; 157. doi: 10.47991/2837-3642/ACRCR-136.
- Bhati D, Deogade MS, Kanyal D. Improving patient outcomes through effective hospital administration: a comprehensive review. Cureus, 2023; 15(10): e47731. https://doi.org/10.7759/cureus.47731.
- Herrera J, De Las Heras-Rosas C, Veiga PM. Editorial: healthcare management: challenges for improving performance and quality of patient services. Front Psychol, 2023; 14: 1272083.
- Lucifora C. Management practices in hospitals: A public-private comparison. PloS One, 2023; 18(2); e0282313.
- Bayot ML, Varacallo M. Management Skills. Treasure Island, FL: StatPearls Publishing, 2024.
- Vlasiadis K, Maisi E, Patelarou E, Patelarou, A. Strategies to enhance financial performance in hospitals. Int J Nurs Health Care Res, 2022; 5: 1299. doi: 10.29011/2688-101299.
- Bastani P, Mohammadpour M, Bahmaei J, Ravangard R, Mehralian G. Hospital management by health services management graduates: the change paradigm in Iran. Heliyon, 2021; 7(11): e08414.
- Doshmangir L, Khabiri R, Jabbari H, Arab-Zozani M, Kakemam E, Gordeev VS. Strategies for utilisation management of hospital services: a systematic review of interventions. Global Health, 2022; 18(1): 53.
- Ndayishimiye C, Dubas-Jakóbczyk K, Holubenko A, Domagała A. Competencies of hospital managers - A systematic scoping review. Front Public Health, 2023; 11: 1130136.
- Zhu D, Wang S, Li Y. Strategic management and risk control of emergency hospital construction: SWOT and STPA framework from a system thinking perspective. PloS One, 2023; 18(11): e0295125.
- Alim DS, Wening N. SWOT analysis is the most popular management strategy tool in the health care sector, why? A literature reviews. Psychology & Education, 2021; 58(5): 303-307.
- Ghanem M, Schnoor J, Heyde CE, Kuwatsch S, Bohn M, Josten C. Management strategies in hospitals: scenario planning. GMS Interdiscip Plast Reconstr Surg DGPW, 2015; 4: Doc06. https://doi.org/10.3205/iprs000065.
- Parand A, Dopson S, Renz A, Vincent C. The role of hospital managers in quality and patient safety: a systematic review. BMJ Open, 2014; 4: e005055.
- Siddiqui A. SWOT analysis (or SWOT Matrix) tool as a strategic planning and management technique in the health care industry and its advantages. Biomed J Sci Tech Res, 2021; 40(2): 32035-32042.
- Grailey K, Leon-Villapalos C, Murray E, Brett SJ. Exploring the working environment of hospital managers: a mixed methods study investigating stress, stereotypes, psychological safety and individual resilience. BMC Health Serv Res, 2022; 22(1): 1371.
- Seelbach CL, Brannan GD. Quality Management. Treasure Island, FL: StatPearls Publishing 2024.
- Moradi F, Toghroli R, Abbas J, Ziapour A, Lebni JY, Aghili A, et al. Hospital managers' skills required and onward challenges: A qualitative study. J Educ Health Promot, 2020; 9: 228.
- van de Riet MCP, Berghout MA, Buljac-Samardžić M, van Exel J, Hilders CGJM. What makes an ideal hospital-based medical leader? Three views of healthcare professionals and managers: A case study. PloS One, 2019; 14(6): e0218095.
- Humphreys P, Spratt B, Tariverdi M, Burdett RL, Cook D, Yarlagadda PKDV, et al. An overview of hospital capacity planning and optimisation. Healthcare (Basel), 2022; 10(5): 826.
- Mistri IU, Badge A, Shahu S. Enhancing patient safety culture in hospitals. Cureus, 2023; 15(12): e51159.
- Stubbe DE. Practicing cultural competence and cultural humility in the care of diverse patients. Focus (Am Psychiatr Publ), 2020; 18(1): 49-51.
- Varnosfaderani SM, Forouzanfar M. The role of AI in hospitals and clinics: transforming healthcare in the 21st century. Bioengineering (Basel), 2024; 11(4): 337. https://doi.org/10.3390/bioengi-neering11040337.
- Vlasiadis K, Vlasiadis Z, Kliagkona K. Public Relations and Communication in Healthcare Facilities: Strategies to Enhance Reputation and Public Trust. Int J Clin Studies Med Case Rep, 2025. DOI: 10.46998/IJCMCR.2025.54.001332.
- Alowais SA, Alghamdi SS, Alsuhebany N, Alqahtani T, Alshaya AI, Almohareb SN, et al. Revolutionizing healthcare: the role of artificial intelligence in clinical practice. BMC Med Educ, 2023; 23(1): 689. https://doi.org/10.1186/s12909-023-04698-z
- Bhagat SV, Kanyal D. Navigating the future: the transformative impact of artificial intelligence on hospital management- a comprehensive review. Cureus, 2024; 16(2): e54518. https://doi.org/10.7759/cureus.54518.
- Franczukowska AA, Krczal E, Knapp C, Baumgartner M. Examining ethical leadership in health care organizations and its impacts on employee work attitudes: an empirical analysis from Austria. Leadersh Health Serv (Bradf Engl), 2021; (ahead-of-print): 229-47. https://doi.org/1-0.1108/LHS-06-2020-0034.
- Qin X, Wang BL, Zhao J, Wu P, Liu T. Learn from the best hospitals: a comparison of the mission, vision and values. BMC Health Serv Res, 2023; 23(1): 792. https://doi.org/10.1186/s12913-023-09699-8.

