Congenitally Corrected Transposition of the Great Arteries and Mesocar-dia in a Young Female: A Case Report
Nitansh Gajjar1,*, Gauri Mahajan2 and Neeraj Mahajan3
1Medical Student in NHLMMC College, Ahmedabad, Gujarat, India
2Medical Student, GMERS Medical College, Sola, Ahmedabad, Gujarat
3Associate Professor, Department of Physiology, NHLMMC College, Ahmedabad, Gujarat, India
Received Date: 13/08/2025; Published Date: 08/09/2025
*Corresponding author: Nitansh Gajjar, Medical Student in NHLMMC College, Ahmedabad, Gujarat, India
Abstract
Congenitally Corrected Transposition of the Great Arteries (CCTGA) is a rare congenital cardiac anomaly characterized by both atrioventricular and ventriculoarterial discordance, resulting in physiologically corrected but anatomically abnormal circulation. We report the case of a 24-year-old female, admitted in a tertiary care hospital presenting with exertional dyspnea, palpitations, and cyanosis, who was incidentally found to have CCTGA with mesocardia during evaluation for amenorrhea. Clinical examination revealed central cyanosis, clubbing, and an irregular pulse. Imaging and echocardiography confirmed the diagnosis of CCTGA with a large ventricular septal defect, severe pulmonary stenosis, and preserved biventricular function. This rare case highlights the need for careful evaluation, with treatment options including a double switch operation or VSD closure with pulmonary valvotomy.
Keywords: CCTGA; Mesocardia; Large Ventricular Septal Defect; Pulmonary Stenosis
Introduction
Transposition of the Great Vessels (TGV), also known as Transposition of the Great Arteries (TGA), is a rare and serious congenital heart defect where the aorta and pulmonary artery are attached to the opposite ventricles of the heart. Opposite to the normal anatomy, in TGA, the aorta is connected to the right ventricle and the pulmonary artery is connected to the left. The incidence is estimated at 1 in 3,500–5,000 live births, with a male-to-female ratio 1.5 to 3.2:1. In 50% of cases, the Ventriculoarterial (VA) discordance is an isolated finding.
The association with other cardiac malformations such as ventricular septal defect (VSD) and left ventricular outflow tract obstruction is frequent and dictates timing and clinical presentation, which consists of cyanosis with or without congestive heart failure.
In 10% of cases, TGA is also associated with noncardiac malformations [4].
The vast majority of cases of transposition of the great vessels can be diagnosed in the first few weeks of life with electrocardiogram, x-ray and fluoroscope [1].
This case is of Congenitally corrected transposition of the great arteries (ccTGA) and mesocardia. ccTGA is a rare defect representing approximately 0.5% of all congenital heart disease, with incidence 1:33,000 live births [5,10].
ccTGA is characterised by the combination of atrioventricular (AV) discordance and Ventriculo-Arterial (VA) discordance. The anatomy is described as congenitally ‘corrected’ because the flow of blood is normal with the deoxygenated systemic venous blood being pumped to the lungs and the well oxygenated pulmonary venous blood being pumped to the body. Nevertheless, the two wrongs of AV and VA discordance do not make a right, as the morphologic Left Ventricle (LV) and mitral valve supply the pulmonary circulation and the morphologic right ventricle (RV) and tricuspid valve supply the systemic circulation [2].
Anteroposterior thoracic X-rays may suggest the diagnosis, particularly when a narrow waist is present at the base of the heart, accompanied by the absence of a pulmonary-artery "knob" and the presence of an enlarged left atrium. Electrocardiographic features that should suggest corrected transposition are atrioventricular block (particularly 2:1 or complete heart block), abnormal P waves, absent or low R voltage in aVR, an initial Q wave in leads 3, aVR, aVF and V1, absence of a Q wave in lead V6, upright T waves across the precordium in children, and a clockwise spatial loop in the frontal plane. Cardiac catheterization may be diagnostic in this malformation when careful documentation is made of the location of the atrioventricular valves and their relation to the semilunar valves, together with the position of the great vessels in the anteroposterior and lateral views. Alteration of hemodynamics is secondary to associated malformations. Inability to enter the pulmonary artery during catheterization should arouse suspicion, and in these cases, particularly, angiocardiography can be diagnostic [3].
Mesocardia is a rare anatomical congenital disorder in which heart is centrally located with longitudinal axis aligned with thoracic mid sagittal plane [9].
This case study is of a 24-year-old female patient with CCTGA and mesocardia with various different symptoms stated in the case presentation section.
Case Presentation
A 24-year-old female presented to the gynecology ward with a 2-month history of amenorrhea, with complaints of dyspnea on exertion corresponding to NYHA (New York Heart Association) grade 2, palpitations, and perspiration on walking.
At presentation, physical examination revealed an uncomfortable young female, poorly built, with clubbing and central cyanosis, normal rate (96 beats/min), irregular rhythm, variable volume, normotensive (100/60 mm Hg), she was afebrile, not tachypnoeic (19 cycles/min), oxygen saturation on room air was 82%.


Figure 1, 2: photograph showing clubbing of the patient’s fingers (Grade 3).
Echocardiography revealed visceroatrial situs solitus with mesocardia. The systemic and pulmonary venous returns were normal. There was evidence of atrioventricular (AV) and ventriculoarterial (VA) discordance, consistent with congenitally corrected transposition of the great arteries (CCTGA). The aorta was positioned anterior and to the left of the pulmonary artery.
A large inlet ventricular septal defect (VSD) with muscular extension and a bidirectional shunt was noted. Additionally, there was severe valvular pulmonary stenosis with a peak gradient of 65.48 mmHg. Right and left ventricular systolic functions were preserved. No coarctation of the aorta was observed, and the aortic arch appeared normal X-ray.
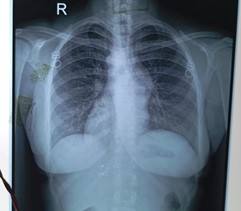
Figure 3
The frontal chest radiograph (Figure 3) demonstrates mesocardia, with a midline cardiac apex, and mild cardiomegaly suggestive of volume overload, likely secondary to a large ventricular septal defect. Pulmonary vascularity is reduced bilaterally, consistent with diminished pulmonary blood flow due to severe valvular pulmonary stenosis. There are no radiographic features of pulmonary venous congestion, interstitial edema, or pleural effusion.
Electrocardiogram
The electrocardiogram (Figure 4) showed left axis deviation, absence of lateral Q waves, and presence of Q waves in V1, consistent with ventricular inversion as seen in CCTGA. A prolonged PR interval suggests first-degree AV block, and features of right ventricular hypertrophy are also present, correlating with the patient’s severe pulmonary stenosis.
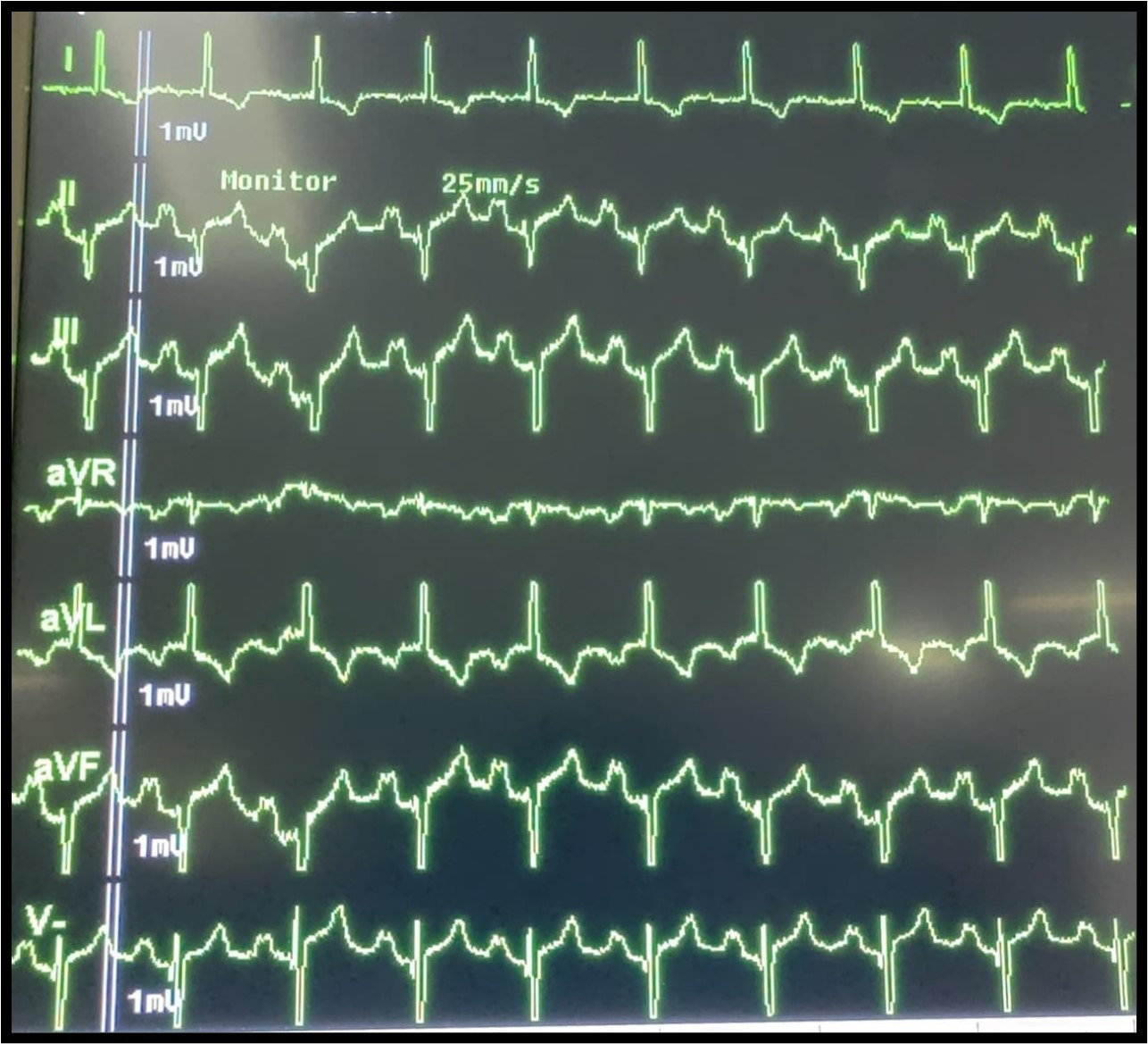
Figure 4
Discussion
This case presents a complex cardiac anomaly in a young female who was incidentally diagnosed during evaluation for gynecological issues. The patient's clinical presentation with cyanosis, clubbing, and dyspnea prompted a comprehensive cardiac evaluation, revealing CCTGA with mesocardia, VSD, and pulmonary stenosis.
A thorough understanding of the pathophysiology is essential for this case. In CCTGA, blood flows in a physiologically correct sequence despite the anatomical abnormalities. However, the addition of a large VSD and significant pulmonary stenosis drastically alters this physiology. The severe pulmonary stenosis (peak gradient 65.48 mmHg) restricts pulmonary blood flow and creates right ventricular pressure overload. Simultaneously, the large VSD allows right-to-left shunting of deoxygenated blood, explaining the patient's cyanosis, reduced oxygen saturation, and compensatory polycythemia.
The ECG findings in this patient are characteristic of CCTGA. Left axis deviation reflects the inverted position of the ventricles. The absence of lateral Q waves and presence of Q waves in V1 result from the ventricular inversion, as the septal activation sequence is reversed. The first-degree AV block (prolonged PR interval) is common in CCTGA due to the elongated and abnormal course of the conduction system through the heart. Studies show that approximately 2% of CCTGA patients develop progressive conduction disorders annually, with many eventually requiring permanent pacemaker implantation [6].
Reproductive Considerations
The gynaecological aspects of this case are particularly significant. Pregnancy in women with CCTGA and associated lesions carries increased risks, including heart failure, arrhythmias, and thromboembolic events. The physiological cardiovascular changes of pregnancy—including increased blood volume (50%), increased cardiac output (30-50%), and decreased systemic vascular resistance, procoagulant state—place additional strain on an already compromised cardiovascular system.
Suggestive Management
Two suggestive surgical management are possible in this patient.
1. DSO (Double Switch operation)
It is a surgical procedure which aims for to restore the normal anatomical connections of the heart leading anatomically correct blood flow [7].
2. VSD closure + pulmonary valvotomy
This procedure is usually performed in patient with VSD (Ventricular Septal Defect) and pulmonary stenosis [8].
Conclusion
This case report is of a 24-year-old female patient having transposition of great vessels which is congenitally corrected and mesocardia. This patient was presented to the gynaecology ward with a 2-month history of amenorrhea, with complains of dyspnoea on exertion corresponding to NYHA grade 2, palpitations, and perspiration on walking. Various tests and scans were done which helped doctors to diagnose this case, the tests and scans with relevant results and images are stated in the case presentation section. Suggestive management for this case was double switch operation (DSO) and VSD closure + Pulmonary valvotomy. This case is different from a standard TGV case as the patient is having TGA which is congenitally corrected and has mesocardia.
Conflict of Interest: None
References
- Keith JD, Neill CA, Vlad P, Rowe RD, Chute AL. Transposition of the great vessels. Circulation, 1953; 7(6): 830-838.
- Hornung TS, Calder L. Congenitally corrected transposition of the great arteries. Heart, 2010; 96(14): 1154-1161.
- Schiebler GL, Edwards JE, Burchell HB, DuShane JW, Ongley PA, Wood EH. Congenital corrected transposition of the great vessels: a study of 33 cases. Pediatrics, 1961; 27(5): 851-888.
- Martins P, Castela E. Transposition of the great arteries. Orphanet Journal of Rare Diseases, 2008; 3: 1-10.
- Wallis GA, Debich-Spicer D, Anderson RH. Congenitally corrected transposition. Orphanet journal of rare diseases, 2011; 6: 1-2.
- Moore JP, Gallotti R, Shannon KM, Pilcher T, Vinocur JM, Cano Ó, et al. Permanent conduction system pacing for congenitally corrected transposition of the great arteries: a Pediatric and Congenital Electrophysiology Society (PACES)/International Society for Adult Congenital Heart Disease (ISACHD) Collaborative Study. Heart rhythm, 2020; 17(6): 991-997.
- Ly M, Belli E, Leobon B, Kortas C, Grollmüss OE, Piot D, et al. Results of the double switch operation for congenitally corrected transposition of the great arteries. European journal of cardio-thoracic surgery, 2009; 35(5): 879-884.
- Singhi AK, Kothandam S. Lessons learnt from a series of hemodynamic and interventional complications during pulmonary valvotomy and device closure of ventricular septal defect. Annals of Pediatric Cardiology, 2015; 8(1): 59-63.
- Lev M, Liberthson RR, Golden JG, Eckner FA, Arcilla R. The pathologic anatomy of mesocardia. The American journal of cardiology, 1971; 28(4): 428-435.
- Amaral F, Valente AM, Manso PH, Gali LG, Braggion-Santos MF, Rocha JM, et al. Congenitally Corrected Transposition of the Great Arteries in the Adult. Brazilian journal of cardiovascular surgery, 2022; 37(4): 534–545. https://doi.org/10.21470/1678-9741-2021-0528.

