A Rare Case of Pediatric Pulmonary Mucoepidermoid Carcinoma Presenting with Hemoptysis: A Case Report and Literature Review
Nosyba Omer1,*, Fatima Majeed1, Zubair Khurshid1, Sara Hashim Hussein Yousif1, Mishraz shaikh1, Fazal Nouman Wahid2, Mohamed Shatari3, Essa Alrashidi4 and Abdelbasit Elsayed Ali5
1Associate Consultant, Department of Pediatric Surgery, King Saud Medical City, Riyadh, Saudi Arabia
2Consultant Pediatric Surgeon, King Saud, Medical City, Riyadh, Saudi Arabia
3PICU Consultant, King Saud Medical City, Riyadh, Saudi Arabia
4Consultant, Pediatric Pulmonology, King Saud Medical City, Saudi Arabia
5Consultant Pediatric Surgeon, King Saud, Medical City, Riyadh, Saudi Arabia
Received Date: 21/07/2025; Published Date: 28/08/2025
*Corresponding author: Nosyba Omer, MD (Paed Surg) Associate Consultant, Department of Pediatric Surgery, King Saud Medical City, 7790 Imam Abdulaziz bin Mohamed bin Saud, Ulayshah, 12746 Riyadh, KSA
Abstract
Mucoepidermoid carcinoma (MEC) of the lung is an exceedingly rare entity in children, arising from the submucosal glands of the tracheobronchial tree and accounting for less than 0.2% of all primary pulmonary malignancies. We present the case of a 12-year-old male initially misdiagnosed with upper gastrointestinal bleeding, who was ultimately found to have low-grade bronchial MEC. The patient underwent emergency thoracic surgery, with histopathology confirming the diagnosis. This report highlights the diagnostic and therapeutic challenges in pediatric pulmonary MEC, especially in the presence of atypical symptoms.
Keywords: Mucoepidermoid carcinoma; Pulmonary cancer; Children
Introduction
Mucoepidermoid Carcinoma (MEC) is a malignancy commonly arising in the salivary glands but can also develop in other sites such as the tracheobronchial tree. Pulmonary MEC (PMEC) is particularly rare in children, with fewer than 55 pediatric cases reported worldwide [1,2]. PMEC arises from submucosal glands of the bronchi and is composed of mucous, squamous, and intermediate epithelial cells. The low-grade variant, more prevalent in pediatric patients, generally carries a favorable prognosis [3] with complete surgical resection.
This report discusses a rare pediatric case of PMEC, highlighting diagnostic ambiguity, the role of multidisciplinary management, and the importance of early bronchoscopy in cases of unexplained hemoptysis.
Case Report
A previously healthy 12-year-old boy presented with multiple episodes of upper gastrointestinal bleeding over four days. He denied abdominal pain, melena, jaundice, fever, or urinary changes. Family and social history were unremarkable. Upper GI endoscopy revealed hyperemic gastric fundal spots without active bleeding. However, persistent bleeding was noted from the Endotracheal Tube (ETT) during the procedure.
Following stabilization, flexible bronchoscopy revealed inflamed airways with a large obstructive clot in the right intermediate bronchus. As depicted in the Chest CT (Figure 1) demonstrated right lower lobe collapse with a "tree-in-bud" appearance, suggesting possible infection or hemorrhage. A CT angiogram raised suspicion of right lower lobe pulmonary sequestration (Figure 2).
A multidisciplinary team—including pediatric surgery, thoracic surgery, pulmonology, PICU, and gastroenterology—determined the need for urgent bronchoscopy and possible lobectomy due to ongoing hemorrhage. Medical management, including transfusion of blood products, failed to stop the bleeding. Chest radiography showed complete right lung opacification, likely due to airway obstruction.
The thoracic team proceeded with rigid bronchoscopy, identifying and removing friable granulation tissue and fresh clots from the right lower lobe bronchus. Despite those measures, bleeding persisted, prompting immediate thoracotomy and right middle lobectomy. Intraoperatively, a mass was found at the upper part of the right lower lobe extending into the middle lobe, necessitating careful resection of the right lower lobe up to but preserving the right middle lobe and bronchus (Figure 3).
Intraoperatively, the patient experienced sudden desaturation due to a dislodged fatty tissue fragment obstructing the left main bronchus, which was successfully removed using Dormia basket. The patient stabilized and had an uneventful recovery in the PICU. He was discharged home in a stable condition on day 10 postoperatively.
Histopathological examination revealed low-grade bronchial mucoepidermoid carcinoma (Figure 4a,4b,4c). It showed a malignant epithelial neoplasm composed predominantly of invasive carcinoma with focal squamous differentiation and mucin-secreting cells, set within a background of cystic spaces and focal solid areas. A small high-grade component, comprising less than 10% of the overall tumor volume, demonstrated solid and nested architecture, cytological atypia, increased mitotic activity, necrosis, and hemorrhage (Figure 4).
Immunohistochemical analysis showed the tumor cells were positive for Pan-Cytokeratin (Pan-CK), Cytokeratin 7 (CK7), and focally positive for CK5/6 and p63 [5]. The tumor cells were negative for TTF-1, Napsin A, Synaptophysin, Chromogranin, CD56, CD10, GATA-3, p16, Melan-A, S100, and Progesterone Receptor (PR). Mucicarmine stain highlighted the mucin-secreting component. The Ki-67 proliferation index was approximately 4%. The histomorphological features, together with the immunohistochemical profile, support a diagnosis of low-grade mucoepidermoid carcinoma, likely originating from bronchial submucosal glands, with a focal high-grade component (<10%). Hilar lymph node biopsy showed no evidence of LN involvement.
Accordingly, the Pathologic Stage Classification (pTNM, AJCC 8th Edition) was pT1b pN0.
Post-surgical imaging revealed residual heterogeneously enhancing soft tissue at the bronchus intermedius and enlarged paratracheal nodes. The patient was referred for oncology center for PET scan, chemotherapy and close follow-up. Fortunately, after PET scan the patient needed no further treatment.
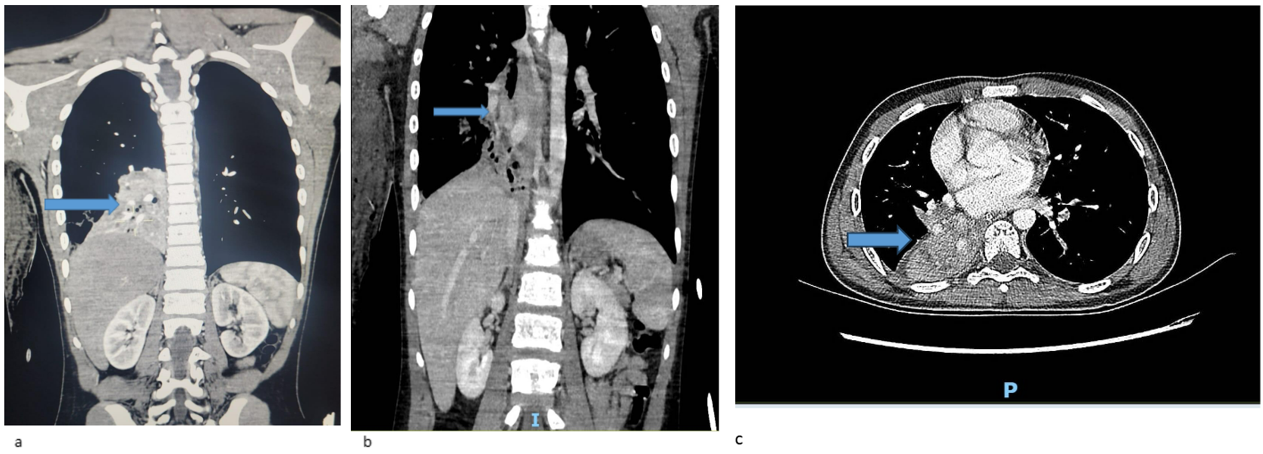
Figure 1: Chest CT with contrast showing heterogeneous mass lesion in Right lower lobe of the lung, (a,b coronal views, c axial view).
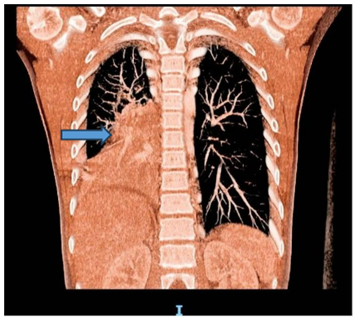
Figure 2: CT angiography showing a doubtful right pulmonary lower lobe sequestration.
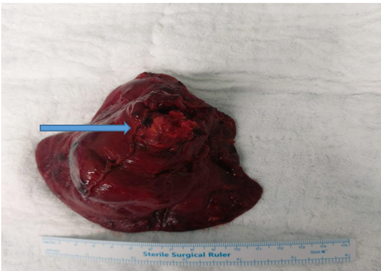
Figure 3: Resected specimen Right lower lobe with tumor infiltrating the Right lower lobe bronchus.
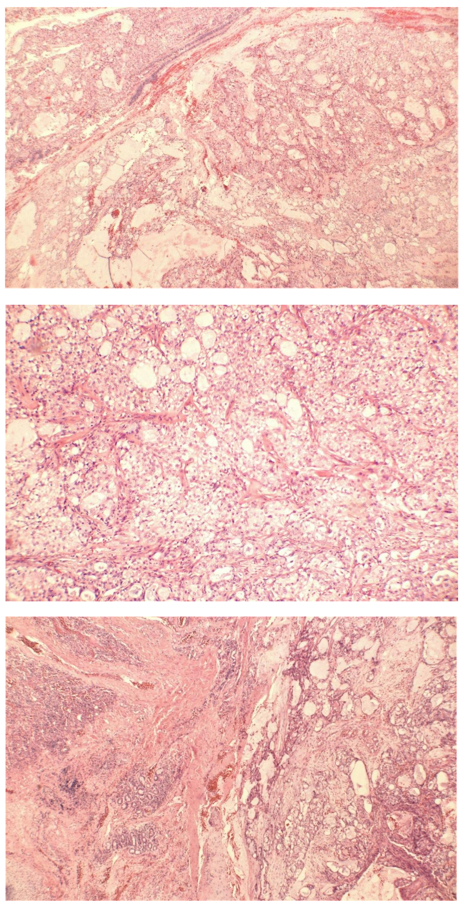
Figure 4: Hematoxylin and Eosin stain histopathology showing:
(a) mucous filled glands adjacent to respiratory epithelium (left) (X10)
(b) mucus secreting cells, squamoid cells without significant keratinization, and intermediate type cells (X40)
(c) mucous filled glands adjacent to lung parenchyma (X10)
Discussion
Pulmonary MECs are rare neoplasms representing less than 1% of lung cancers, with even fewer cases documented in children. They commonly arise centrally, leading to airway obstruction, and may present with nonspecific symptoms such as cough, wheezing, or recurrent pneumonia [2,4,5]. Hemoptysis, though more frequent in adults, can be an alarming sign in pediatric cases and should prompt early airway imaging and bronchoscopy.
Our patient’s initial presentation mimicked upper GI bleeding, delaying definitive diagnosis. Only upon persistent bleeding from the ETT was bronchoscopy pursued, revealing an endobronchial mass.
Histologically, PMECs are classified as low- or high-grade based on features such as mitotic rate and cellular atypia. Low-grade tumors, like in this case, tend to behave indolently and respond well to complete resection [1,6,7]. Immunohistochemical markers such as CK5/6, CK7, p63 [5], and MUC5AC are typically positive, and the CRTC1-MAML2fusion gene—associated with better outcomes—is often present in low-grade MEC.
In the largest pediatric case series to date, complete surgical excision has been curative especially with low grade tumors [1], with no need for adjuvant therapy. In our patient, no further treatment or adjuvant therapy was needed 4-months post-surgical resection.
Conclusion
This case highlights the importance of considering pulmonary etiologies in children presenting with hemoptysis or unexplained airway bleeding. Early bronchoscopy and imaging are essential for timely diagnosis. Surgical resection remains the cornerstone of treatment for low-grade PMEC, with excellent outcomes. Continued surveillance is crucial due to the potential for recurrence or residual disease.
References
- Alsidawi S, Morris JC, Wikenheiser-Brokamp KA, Starnes SL, Karim NA. Mucoepidermoid carcinoma of the lung: a case report and literature review. Case Rep. Oncol. Med, 2013; 1–5. doi: 10.1155/2013/625243.
- Huang Y, Fu Y, Sun J, Xu B, Wu L, Tang LF. Pulmonary mucoepidermoid carcinoma in children: two case reports and a review of the literature. Front Pediatr, 2023; 11: 1232185. doi: 10.3389/fped.2023.1232185.
- Fois AG, Diana G, Arcadu A, Marras V, Crivelli P, et al. Bronchial mucoepidermoid carcinoma: A case report. International Journal of Surgery Case Reports, 2017; 31: 159–162.
- Dardouri T, Ezzine A, Ben Fredj M, Boudriga H, Mensi S, Ayadi A, et al. Pulmonary mucoepidermoid carcinoma in children: a rare diagnosis not to be overlooked - case report. Ann Med Surg (Lond), 2023; 85(4): 1092-1095. doi: 10.1097/MS9.0000000000000331.
- Vu LT, Duc NM, My TT, Bang LV, My LT, Thuy LTP, et al. Pulmonary mucoepidermoid lung carcinoma in pediatric confused with asthma,Respiratory Medicine Case Reports, 2021; 33.
- Wang YQ, Mo YX, Li S, Luo RZ, Mao SY, Shen JX. Low-Grade and High-Grade Mucoepidermoid Carcinoma of the Lung: CT Findings and Clinical Features of 17 Cases. AJR Am J Roentgenol, 2015; 205(6): 1160-1166. doi: 10.2214/AJR.14.14153.
- Limaiem F, Lekkala MR, Sharma S. Mucoepidermoid Lung Tumor. In: StatPearls: Treasure Island (FL): StatPearls Publishing, 2025.

