Unveiling Pulmonary Sequestration: The Role of Advanced Imaging in Diagnosis
Kaouthar Sfar*, Fatima Chait, Nourrelhouda Bahlouli, Nazik Allali, Siham El Haddad and Latifa Chat
Mother and Child Imaging Department, HER – Ibn Sina Hospital, Mohammed V University in Rabat, Rabat, Morocco
Received Date: 05/07/2025; Published Date: 22/08/2025
*Corresponding author: Kaouthar Sfar, Mother and Child Imaging Department, HER – Ibn Sina Hospital, Mohammed V University in Rabat, Rabat, Morocco
Pulmonary sequestration, also known as accessory lung, is a rare congenital anomaly involving a cystic or solid mass of nonfunctioning lung tissue that is disconnected from the tracheobronchial tree and receives blood supply from an anomalous systemic artery [1,2,4]. Classified as a bronchopulmonary foregut malformation, its incidence ranges from 0.1% to 6.4% [1]. There are two main types: Intralobar Sequestration (ILS), which shares the visceral pleura with the normal lung and drains into the pulmonary veins, and Extra-Lobar Sequestration (ELS), which has its own pleura and drains into systemic veins, forming an accessory lobe known as a "Rokitansky lobe" [1,2,6]. A variant known as pseudo-pulmonary sequestration, or Pryce’s type 1 sequestration, features systemic arterial supply to the lung but maintains communication with the tracheobronchial tree, distinguishing it from true sequestration [3,4]. To address the complexity of these broncho-vascular anomalies, Sade and colleagues introduced the concept of a "sequestration spectrum," while Clements and Warner expanded this with the notion of a "pulmonary malinosculation spectrum." Furthermore, Takahashi and associates proposed terms like “arterial sequestration” and “broncho-arterial sequestration” to differentiate between isolated systemic arterialization and classic sequestered lung tissue [4].
Intralobar sequestration is often asymptomatic and frequently diagnosed in adulthood, typically during chest CT scans performed for other reasons. When symptomatic, it most commonly presents as recurrent pneumonia in the same lung segment, though patients may also experience exertional shortness of breath, persistent cough with back pain or hemoptysis. In most cases, patients with pseudo-sequestration are asymptomatic [2,4]. When symptoms are present, they typically include hemoptysis, exertional shortness of breath, or congestive heart failure caused by left-to-left shunts. In severe cases, patients may experience respiratory distress and pulmonary hypertension.
The diagnosis of this congenital anomaly is typically established through CT (Figure) or MR angiography, which defines the anatomy, detects the anomalous systemic arterial supply, reveals the venous drainage and rule out other potential thoracic pathologies [2,5].
The treatment is surgical, involving lobectomy, basal segmentectomy, or anastomosis of the aberrant artery to the pulmonary artery. Alternatively, endovascular approaches such as ligation of the anomalous artery or coil embolization of the systemic vessel may be used [1,4].
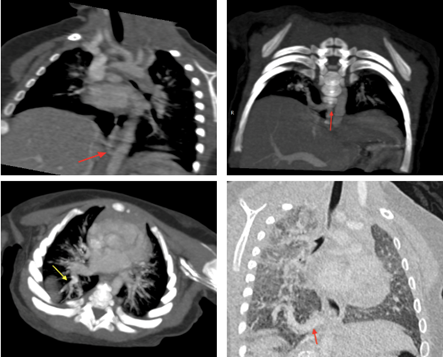
Figure: CT scan illustrating a systemic artery (red arrow) originating from the abdominal aorta at the level of the diaphragm, prior to the emergence of the celiac trunk. Venous drainage is directed toward a dilated right inferior pulmonary vein (yellow arrow). These findings are consistent with a Pryce type I pulmonary sequestration.
References
- Wani SA, Mufti GN, Bhat NA, Baba AA. Pulmonary Sequestration: Early Diagnosis and Management. Case Rep Pediatr, 2015; 2015: 454860. doi: 10.1155/2015/454860.
- Chakraborty RK, Modi P, Sharma S. Pulmonary Sequestration. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024.
- Qatomah WY, Ali RM, Qatomah AY, Arabi M. Successful coil embolization of pseudo pulmonary sequestration: A report of two cases. J Clin Imaging Sci, 2022; 12: 36. doi: 10.25259/JCIS_42_2022.
- Singh AS, Subbain SK, Subramanian KG, Agarwal R, Dave DJ, Kulkarni S, et al. Pseudosequestration of the left lung. Tex Heart Inst J, 2007; 34(2): 195-198.
- Ko SF, Ng SH, Lee TY, Wan YL, Lee CM, Hsieh MJ, et al. Anomalous systemic arterialization to normal basal segments of the left lower lobe: helical CT and CTA findings. J Comput Assist Tomogr, 2000; 24(6): 971-976. doi: 10.1097/00004728-200011000-00026.
- Gabelloni M, Faggioni L, Accogli S, Aringhieri G, Neri E. Pulmonary sequestration: What the radiologist should know. Clin Imaging, 2021; 73: 61-72. doi: 10.1016/j.clinimag.2020.11.040.

