Intergenerational Communications and Relations in Medicine
Fatimah Lateef1,* and Jonathan Kim Yang Chan2
1Senior Consultant, Department of Emergency Medicine, Singapore General Hospital, Core Faculty, Emergency Medicine Residency, Sing Health, Professor, Duke NUS Graduate Medical School, Yong Loo Lin School of Medicine, National University of Singapore and Lee Kong Chian Medical School, Nanyang Technological University, Director, Sing Health Duke NUS Institute of Medical Simulation (SIMS), Faculty, Duke NUS Global Health Institute, Singapore
2Associate Consultant, Dept of Emergency Medicine, Singapore General Hospital, Singapore
Received Date: 04/07/2025; Published Date: 19/08/2025
*Corresponding author: Fatimah Lateef, FRCS (A&E), MBBS, FAMS (Em Med), Senior Consultant, Dept of Emergency Medicine, Singapore General Hospital, Core Faculty, Emergency Medicine Residency, Sing Health, Professor, Duke NUS Graduate Medical School, Yong Loo Lin School of Medicine, National University of Singapore and Lee Kong Chian Medical School, Nanyang Technological University, Director, Sing Health Duke NUS Institute of Medical Simulation (SIMS), Faculty, Duke NUS Global Health Institute, Singapore
Abstract
Generational diversity amongst physicians presents a unique dynamic in the workplace. Various outcomes are possible when groups of physicians from different generational cohorts collaborate. If they can engage well, collaborate efficiently, embrace open-mindedness, and show a willingness and a big heart to accept and learn from each other, positive outcomes can be multiplied and translated to superior patient care experiences and outcomes. However, the reality is that various hurdles do occur secondary to differences in expectations, perspectives, communication styles, work approach preferences, and the ability to negotiate information technology and Artificial Intelligence (AI) tools. These differences can escalate into friction and conflict, altering the work environment and climate into one of discomfort and disharmony.
The authors, from different generational cohorts, share their views and perspectives on the subject, which is not well covered in the literature, especially in the Asian context.
Keywords: Intergenerational relations; Generation X; Generation Y; Generation Z; Baby Boomers; Healthcare
Introduction
Communication is the life cord and keystone in the practice of all disciplines of Medicine. Progressing from the authoritative, one-way approaches of doctors from the early era, today’s medical field embraces a more collaborative and open communication method. With the emphasis on shared decision-making prevalent in our current practice, communication techniques, and capabilities have certainly evolved over the years [1,2]. The formal practice of modern Medicine started during the 18th century, with the introduction of professional societies and more structured medical education programmes. The 20th Century, particularly from the 1870s onwards, saw a greater professionalisation accorded to the practice [3]. Yet throughout these changes, one constant remains important i.e., the critical need for clear and effective communication between physician and patient as well as between physicians themselves. Since the early practice of medicine, various generations of healthcare providers have ventured into the discipline. Today, diverse cohorts of doctors engage in the practice of Medicine in tandem. These different generations offer a rich mix of experiences and perspectives to patient care, with some from the older generations still in practice whilst the younger generation are now working together, alongside the former [4-9].
Effective communication is crucial in doctor-doctor relationships, directly influencing patient care and team dynamics. However, challenges like communication barriers, time constraints, and cultural differences can impede the seamless flow of information, sharing, and collaboration. These challenges often lead to misinterpretations, errors, and even negative impacts on patient outcomes [10-14].
It is important to understand that people born and raised in different eras often develop distinct values and worldviews [4,5,15,16]. This may lead to difficulty and challenges in understanding each other. With globalisation, rapidly changing lifestyles and the influence of varying ideologies continue to widen the chasm of the generation gap. Thus, special efforts may be needed to uplift and bridge the understanding across groups [12,17]. The four commonest generational cohorts in medical practice today include the following groups [4,5, 18-22]:
The Baby Boomers (Table 1)
This generation is more traditional in work approaches and tends to hold more leadership roles currently. They are hardworking (with strong ethics and commitment to the organization), planners and schedulers, put in a lot of effort in preparation, and take pride in doing things/ tasks systematically. They are very organised and process-oriented. Highly respected due to their roles and seniority, and hierarchy is still relevant to them. Some in this generation still find it hard to adapt to change and the latest technology, but they will tend to do whatever it takes as they believe in the adage, "Live to work” [4,5,22,23].
The Generation X (Table 1)
This group is also hardworking and tends to be independent/self-sufficient, but they are more pragmatic and tend to be risk-takers. They hold some of the leadership roles and many are in the mid-level leadership roles. They are resilient, believe in change for the positive, and can adapt more readily than the former generations. They also tend to believe in preparedness but are comfortable with novel ideas, collaboration, and "thinking out of the box.” They are adaptable to modern technology and Information Technology (IT). Work-life balance is important to them [4,5,19,20].
Generation Y/ Millennials (Table 1)
This generation is comprised of the multi-taskers. They ask questions to generate solutions and are agents of change. They love the digital world of immediacy and are very technology-savvy. Generation Y is focused on goals and looks to execute work by way of processes. They hold on to work-life balance strongly and believe in “work whilst living.” They tend to appreciate feedback for improvement and are good coordinators [5,6].
Generation Z (Table 1)
They are the digital natives and represent a generation inherently Information Technology (IT) and Artificial Intelligence (AI) savvy. They do not know the world without technology and IT. There are many advocates and activists amongst them, for a variety of causes they strongly believe in. Generation Z tends to be very passionate, especially about what they believe in and care for. Generation Z are also very comfortable with social media and loves social networking. They represent a very portable, mobile, and flexible generation. They can learn and work anywhere, everywhere, and appreciate micro-learning [4,5,7,24].
Background
In healthcare institutions of today, there are at least 4 generations of staff working side by side. They are usually from the Baby Boomers to Generation Z. Whilst there may be some from the Traditionalist generation who are still working, the vast majority of the Alpha Generation are primarily still pursuing their studies and not yet out in the workforce in significant numbers. The focus on the interplay of the currently active cohorts is significant.
With the different upbringings, life experiences, socio-political exposure, circumstances as well as the developments during their prime years, there will be unique intergenerational characteristics. These will certainly have an impact on and shape their work ethics and preferences, communication styles as well as interaction approaches. (6, 8) These differences can be a tremendous asset if staff from different generations harness and utilise their strengths, accept differences, integrate well, and work together. However, these distinctions in approach to work can be a major source of dispute and misunderstanding. These would include factors such as the way the generations think and approach situations, their attitude, behaviour, and value system, their technical knowledge as well as many other factors [9,25].
Objectives
This paper aims to delegate into the intergenerational challenges prevalent in today’s practice of Medicine and healthcare institutions. We will explore these dynamics from the perspectives of a senior clinician, offering insights into the real-world complexities that are likely to be encountered when different generations work side-by-side. These challenges may be classified into several themes as shown in Table 2. These were then regrouped into five categories as discussed below:
1. Communications and Interactions
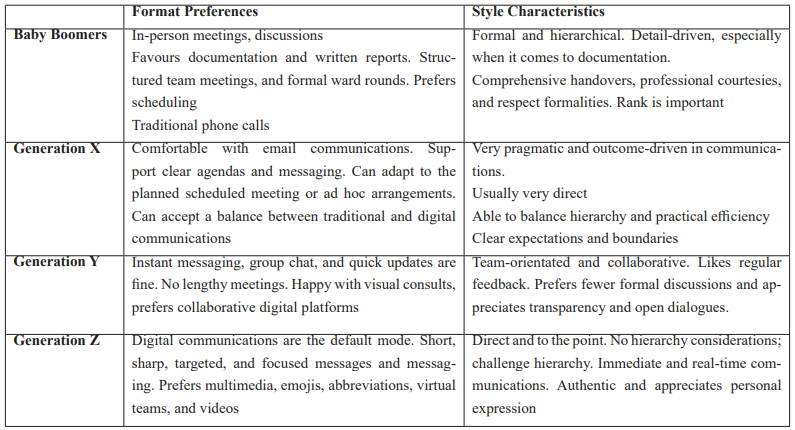
This category emerged as the most frequently cited challenge, and everyone had met with some form of communication conflict or challenge in intergenerational relations. This is not surprising given the significant role that communication occupies in the core of medical practice. It features in all interactions, instructions, and orders, mentoring, training, as well as many other daily activities. Communication can be in the form of verbal, nonverbal, telephonic, written, digital, and others. Cooperation, teamwork, and information flow all depend on good, positive communication and communication styles. These are all affected by the thinking process across the different generations and thus, will affect knowledge sharing and knowledge transfer [5]. The common preferences and styles of communication across the various generational groups are shared in Table 3.
To summarise, some of the challenges of intergenerational communications encountered today arise due to [8,9,22]:
- Preference for different communication channels
- Varying levels of comfort with technology adoption
- Different perspectives on authority and hierarchy
- Different views on work-life balance and
- Diverse expectations on availability and response
2. Perspectives and Expectations
The differences in perspectives can create both challenges as well as opportunities in healthcare. Baby boomers value physical presence, often equating long hours at work to dedication. They emphasise traditional knowledge acquisition and the building up of clinical experience gradually, expecting similar commitments from younger physicians as well as medical students. In contrast, Generation X is more efficient and emphasises work-life balance. They tend to be strong proponents of in-depth decision-making and autonomy. They have clear guidelines, framework as well as protocols to support their pragmatic approach [5]. The millennials want work-life integration, continuous learning and are strong in professional development. They will seek meaning and purpose in the work they do, and they appreciate regular, constructive feedback and inputs. Generation Z’s focus is on wellbeing, especially mental health. They love working remotely and virtually but do realise that not all areas and disciplines of medical practice offer this. They favour flexibility and efficiency, thus demanding efficient work systems, technology, and AI (artificial intelligence). They tend to seek multiple career options and pathways and enjoy spin-offs such as entrepreneurial opportunities and innovation in healthcare. They are not at ease with the status quo and tend to be "hungry" for the acquisition of knowledge and skills in their areas of choice. In general, Generation Z ascribes to microlearning, which focuses on efficiency, flexibility, and knowledge retention in their medical practice [6,7,17].
3. Professional Values and Identity
In the context of Medicine, professional values represent the fundamental principles and behavioural standards of conduct that guide medical professionals in their interactions with patients, colleagues, and society. These values are crucial for ensuring ethical, safe, and effective healthcare. They help to define the expected behaviours and attitudes of healthcare providers, emphasising concepts like patient well-being, integrity, and commitment to excellence. The baby boomers interpret long hours at work and being physically present as proof of a dedication to their work. This is the standard they tend to impose on the younger generation and judge them by. They often feel this is in line with the necessary part of the younger generation “paying their dues” [5-7]. The younger physicians (Generation Y and Z) share a distinct perspective on values. To them, efficiency and the successful delivery of results may be sufficient indicators of dedication, rather than the sheer number of hours spent at work. Generation X often bridges these two viewpoints and tends to hold a more balanced outlook on work values, midway between the baby boomers and the younger physicians [13,16].
4. Leadership and Management Styles
The Baby Boomers often lean towards more hierarchical and authoritative leadership styles, valuing experience, and seniority. They appreciate formal decision-making processes and prefer a more detailed oversight of their juniors and subordinates, often adhering to a traditional apprenticeship model that emphasises loyalty and commitment. Generation X is typically more strategic, valuing competence over position. They are typically more strategic and pragmatic, and through efficiency and a result-oriented mindset, they prioritise performance as well as outcomes [14].
Generation Y and Z physician leaders advocate for a flatter organisation structure with participative and collaborative decision-making. Generation Y embraces innovation and fresh perspectives in their leadership approach. They will empower team members, share feedback and information, and have frequent check-ins, their mentorship model via peer learning, and close engagements. Generation Z leaders tend to be very well networked, especially digitally and are comfortable with virtual and hybrid work methodologies and lead with a more fluid and adaptive approach. When it comes to managing their teams, baby boomers like a clear, formal chain of command. They appreciate structured career progression for the people they work with. Face-to-face interaction is their strength, especially in supervision. Generation X prefers project-based and merits-based advancements based on the performance of their team members, whilst Generation Y and Z, focus on cross-functional teams and frequent feedback [26,27].
5. Technology Adoption
Digital literacy and attitudes towards technology and AI also vary significantly across generations in healthcare. This is reflected by the period of their growing up and their exposure to technological developments and advancements. These differences also affect their preferences and savviness in aspects of communications technology, use of IT and AI, as well as resource utilisation and adoption of digital resources in modern institutional practice [28]. Despite these generic observations, there are groups of individuals within each generation who are highly digitally literate and have developed their capabilities and share an open mindset to change and adoption of technology and modernisation. They may thus be more familiar than their counterparts and can be role models and even champions for their colleagues to bridge the generational digital divide [29]. In some institutions, the practice of reverse mentoring is employed whereby senior physicians are matched with junior physicians who are more tech-savvy and can share their expertise. The term “reverse mentoring” aptly describes this dynamic, as it flips the traditional mentorship model where senior physicians typically guide and share expertise with the juniors. This approach can be successful if embarked on with the correct mindset and open approach of working together and engaging each other through strength and capabilities, rather than solely focusing on seniority [30-35].
Table 1: The Four Commonest Generational Cohorts in Medicine Today.
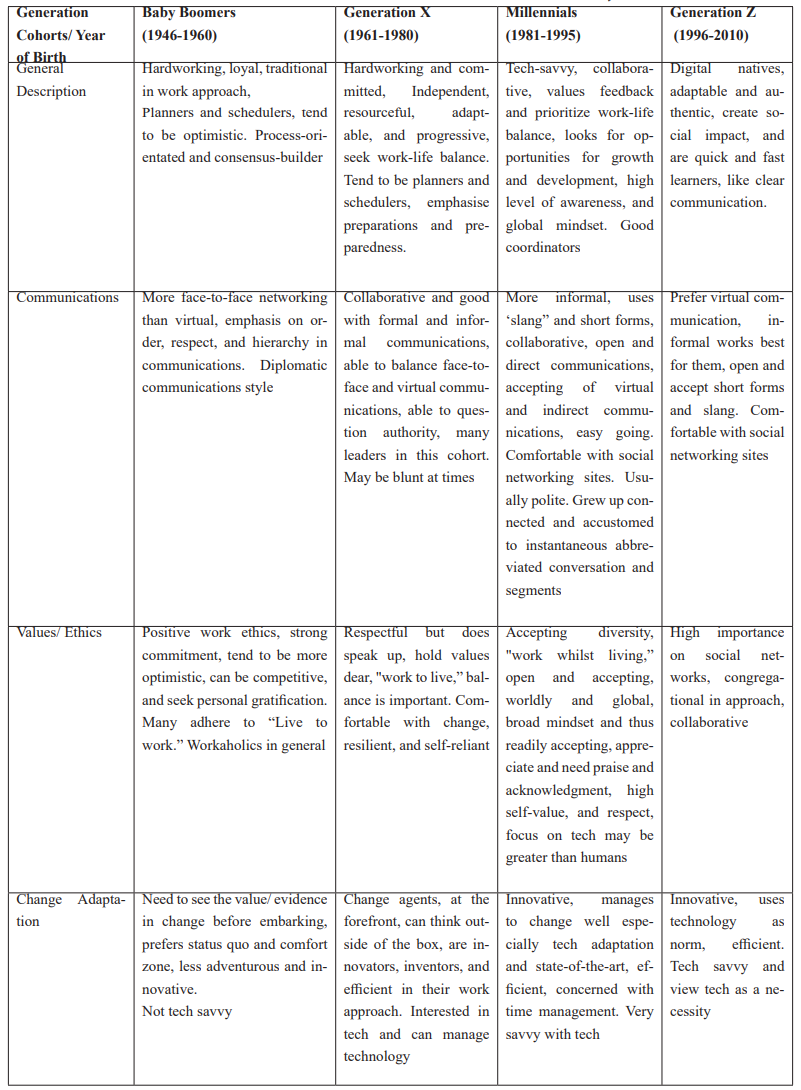
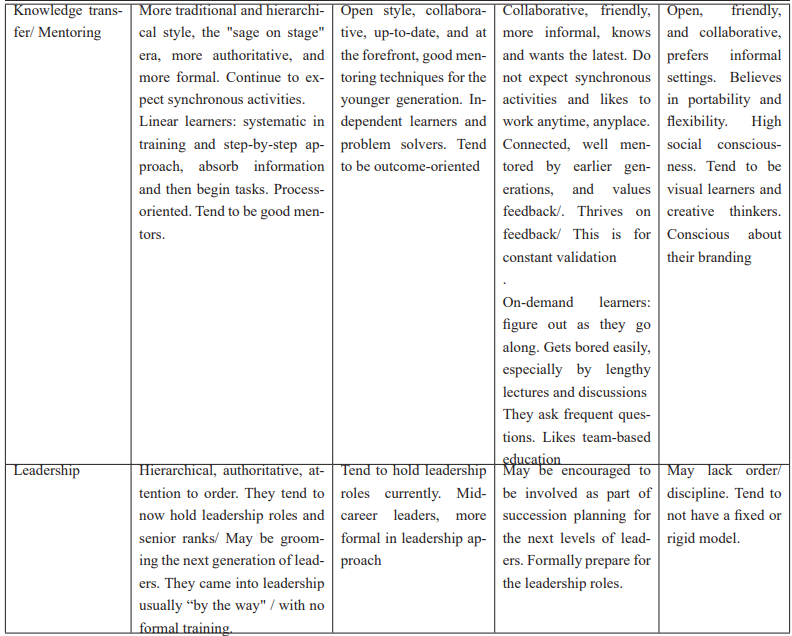
Table 2: Intergenerational Challenges Themes.
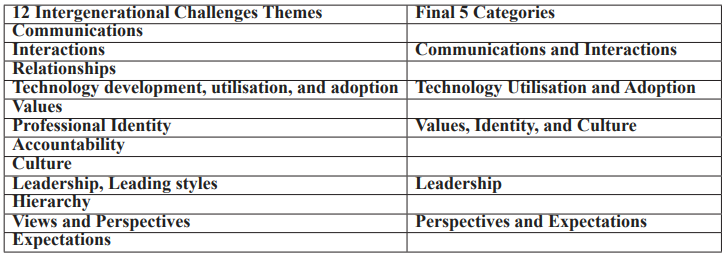
Table 3: Communications Across the Generations: Format and Style Preferences.
Challenges to Human Resource (HR)
With the varied characteristics and personalities peculiar to each group of physicians, HR in healthcare institutions today will certainly have to undergo a significant shift, to adapt and practice flexibility in their policies and approaches. HR practices must evolve and progress with time. There may be challenges in getting senior physicians from the Traditionalist and Baby Boomer generations on board with current practices, but it is possible. They may benefit from more time to adapt, “reverse mentoring” from their tech-savvy younger colleagues, and step-by-step guidance to keep abreast with recent developments and to remain current. HR must consider these factors to get buy-in and must be aware and practice flexibility in their processes such as recruitment, employment offers, performance evaluation, developing physicians’ motivation, payment system and structure as well as career management tracks.
Healthcare institutions often have a long history of culture and tradition. At times, it may be challenging to change and evolve already established work systems. Today, newer, and previously not explored work systems are already in place in other institutions. To keep up-to-date, other institutions should review these practices and customise contemporary work settings as appropriate. There are now satellite workplaces, “hot desking” concepts, open spaces as offices (with no doors), breakout and socialising spaces, mobile centres, green HR, activity-based work, and strong partnership models. These may be very new for senior physicians who are used to having rooms with doors inscribed with their names; where such spaces are private and not shared. Whilst these measures can represent a significant departure from the traditional norms, successful integration of these new models can be achieved with careful planning, transparent communication, and a greater focus on how these changes can benefit all generations within each institution.
Discussion
Intergenerational differences contribute to some of the misunderstandings and conflicts in the workplace. However, this is not a topic that has been scrutinised and studied in great depth. It is also an extremely sensitive topic. For harmony at the workplace, physicians from the various generations should inculcate an understanding of each group’s characteristics, peculiarities, working styles, preferences, strengths, and weaknesses.
The authors would like to suggest the following initiatives to be considered for implementation to help address the issues:
- Creation of awareness and open discussions on the issues. If possible, it could be the subject of an address at the healthcare institution town hall, a CEO (Chief Executive Officer) engagement session, or a Family Meeting agenda. These sessions are often attended by a substantial number of healthcare professionals (whether physically or virtually) across different generations and age groups. This would reflect leadership and management’s buy-in into the issues and would be easier for Heads of Department and Specialties Departments to take on this subject with their staff.
- Use of narratives and stories to share the messages as intended. Role models can also be highlighted. The latter can function as resource persons for others to consult, in case they encounter challenges along the way when sharing the topic with their departments.
- Following Point 2 above, the appointment of “Intergenerational champions" can be useful, just as healthcare institutions appoint "Patient Safety Ambassadors” or “Inter-professional Collaboration Champion”. This action can emphasize the weightage and importance of intergenerational relations within the institution.
- Organisation of more dialogues and open conversations to discuss this topic. It can take the style of a Balint Group approach [36,37]. Publicity of these sessions is important and the messaging used must be sensitive enough in addressing the topic [38,39].
- Consider introducing this topic early for discussion at the medical school level/ other healthcare schools as well.
- Establish clear communication channels so that no matter what the age group of the staff, issues can be discussed objectively.
- Have standardised protocols for a variety of issues but incorporate flexibility to accommodate unique styles and approaches. Hybrid options can be utilised where possible.
- The greater offering of training courses about the topic with carefully curated curriculum and practical activities, which may utilise Standardised Patients (SPs) embedded in simulation scenarios. The best way to learn and feel the experience is when one is in the "hot seat" during these training sessions.
Whilst some healthcare staff involved in intergenerational conflicts may tend to tolerate, suffer in silence, or act with 'avoidance" of such situations, the better way to handle these will be to create awareness, for leadership to take some institution stand and make this a more central topic, as appropriate. Having an open mindset to help build bridges and manage egos is a constructive approach as well.
Conclusion
To have a harmonious work environment in healthcare today, there must be knowledge and understanding about intergenerational differences and preferences; each has its expectations and behaviour. Therefore, some aspects of professional development should be focused on building their strengths and supporting them in integration. (40) Policies in healthcare must account for work-life balance and accord some flexibility for each generation to negotiate so that they can adapt more readily. Open dialogue to enhance communications, as well as training as relevant, should also be planned, promoting the exchange of ideas, knowledge, and work experiences to help each generation achieve its full potential.
References
- Widder J. The origins of medical evidence: communication and experimentation. Med Health Care Philos, 2004; 7(1): 99-104. doi: 10.1023/b:mhep.0000021679.52642.25.
- Howell LP, Joad JP, Callahan E, et al. Generational forecasting in academic medicine: a unique method of planning for success in the next two decades. Acad Med, 2009; 84(8): 985-993.
- Albini Adriana. Evolution of the doctor-patient relationship: from ancient times to the personalised medicine era. Available at: Evolution of the doctor-patient relationship: from ancient times to the personalised medicine era | Cancerworld Magazine.
- Guptill M, Reibling E, Phan T, et al. Working in fours: generational communications in the ED. Int Journal of Emerg Med, 2023; 16: 58. https://doi.org/10.1186/s12245-023-00536-7.
- Weingarten RM. Four generations, one workplace: a Generation X-Y staff nurse’s view of team building in the ED. J Emerg Med, 2009; 35(1): 27-30.
- Bencsik A, Horrath-Csikos G, Juhasz T. Y and Z Generations at workplaces. J of Competitiveness 2016; 8(3): 90-106.
- Elenga M, Krishnaswamy G. A new generation of physicians: The Generation Z. Are you ready to deal with it? Frontier in Public health, 2023; 10: 1015584. Doi: 10.3389/fph.2022.1015584.
- Mehra P, Niderson C. Organizational communications and job satisfaction: what role do the generational differences play? Int J of Org Analysis, 2018; 27(30): 524-547.
- Myers KK, Sadaghiani K. Millennials in the workplace: a community perspective on millennials: organizational relationships and performance. J of Bus and Psychology, 2010; 25(2): 225-238.
- Smith LG. Medical professionalism and the generation gap. Am J Of Med, 2005; 118: 439-442.
- Umberson D, Montez JK. Social relationships and health: a flashpoint for health policy. J Health Soc Behav, 2010; 51(Suppl): S54-66. doi: 10.1177/0022146510383501.
- Fatimah Lateef. Transition from Junior to Senior Residency in Emergency Medicine: Requirements, Challenges and Recommendations. Curr Tr Clin & Med Sci, 2021; 2: 3. DOI: 10.33552/CTCMS.2021.02.000537.
- Berger E. This sentence would easily fit on twitter: EPs are learning to “tweet”. Ann Emerg Med, 2009; 54(2): A23-A25.
- Lateef F, Kiat KT, Yunus M, Rahman MA, Galwankar S, Al Thani H, et al. BRAVE: A point of care adaptive leadership approach to providing patient‑centric care in the emergency department. J Emerg Trauma Shock, 2022; 15: 47-52.
- Washburn ER. Are you ready for Generation X? Physician Exec, 2000; 26(1): 51-57.
- Wieck KL. Instilling an intergenerational workforce: scenario for success. Orthopaedic Nurs, 2007; 26(6): 366-371.
- Davey L. The key to preventing generational tensions is remembering that everyone wants to feel valued. Harv Bus Rev, 2018.
- Busari JO. The discourse of generational segmentation and the implications for postgraduate medical education. Perspect Med Edu, 2013; 2(5-6): 340-348.
- Erikson T. The four biggest reasons for intergenerational conflicts in teams. Harv Bus Rev, 2009.
- Eckleberry-Hunt J, Lick D, Hunt R. Is medical education ready for Generation Z? Journal of Grad Med Edu, 2018; 10: 378-381.
- Mohr NM, Moreno-Walton L, Mill AM, et al. Generational influences in academic medicine: teaching and learning, mentoring and technology (Part 1). Acad Emerg Med, 2011; 18(2): 190-199.
- Twenge JM, Campbell SM, Hoffman BJ, et al. General differences in work values: Leisure and extrinsic values increase whilst intrinsic values decrease. Journal of Manag, 2010; 36: 1117-1142.
- Boysen PG, Daste L, Norturm T. Multi generational challenges and the future of graduate medical education. Ochsner Journal, 2016; 16: 101-107.
- Kiecolt K Jill, Hughes Michael, Keith Verna M. Race, Social Relationships, and Mental Health. Personal Relationships, 2008; 15: 229–245.
- Suberry A, Bodner E. Intergenerational synchrony and its effect on boarding and group closeness amongst youth and older adults. Behv Sci, 2024; 14: 607. https://doi.org/10.3390/bs1`4070607.
- Blumenthal DM, Bernard K, Bohren J, et al. Addressing the leadership gap in medicine: residents need for leadership development training. Acad Med, 2012; 87(4): 690-704.
- Kessler EM, Staudinger UM. Intergenerational potential: effects of social interaction between older adults and adolescents. Psychology and Aging, 2007; 22(4): 513-522.
- Fatimah Lateef. Culture of Psychological Safety in the Emergency Department: Don’t Forget the Hidden Curriculum. Archives of Emergency Medicine and Intensive Care, 2021; 4(1): 18-26. DOI: https://doi.org/10.22259/2638-5007.0401004.
- Fatimah Lateef. The Paradox of Psychological Safety: How Far Should We Take It? Biomed J Sci & Tech Res, 2025; 60(4): 2025.
- Murphy WM. Reverse mentoring at work: fostering cross generational learning and developing millennial leaders. Human Resource Manag, 2012; 51: 549-573.
- Lateef F. Tying in Situational Awareness, Clinical Reasoning and Clinical Judgment through Cross-Training Using Case-Based Discussions in Emergency Medicine. Curr Res Emerg Med, 2022; 2: 1024.
- Lateef F. Informal and Non-Formal Faculty Development in Emergency Medicine: What Does It Take to Uplift Recognition. J Case Rep Rev Med, 2025; 1(1); 1-7.
- Gadomska-Lila K. Effectiveness of reverse mentoring in creating intergenerational relationships. J Organ Change Manag, 2020; 33.
- Gerards R, deGrip A, Weustink A. Do new ways of working increase informal learning at work. Pers Rev, 2020; 50: 1200-1215.
- Fatimah Lateef. “High Technology, High Touch: Implementing Virtual Reality Education and Ensuring the Elements of Humanism are Not Forgotten.” MAR Case Reports, 2023; 6(5): 1-16.
- Roberts M. Balint groups: a tool for personal and professional resilience. Can Fam Physician, 2012; 58(3): 245-247.
- McCray LW, Cronholm PF, Bogner HR, et al. Resident physician burnout: is there hope? Fam Med, 2008; 40(9): 626–632.
- Kjeldmand D, Holmström I, Rosenqvist U. Balint training makes GPs thrive better in their job. Patient Educ Couns, 2004; 55(2): 230–235. doi: 10.1016/j.pec.2003.09.009.
- Adams J, Schmidt T, Sander A, et al. Professionalism in Emergency Medicine. SAEM Ethics Committee. SAEM. Acad Emerg Med, 1998; 5: 1193-1199.
- Kuo YL, Lee JT, Yeh MY. Intergenerational learning to bridge the generation gap in humanistic care. Nursing Edu Healthcare, 2021; 9: 1291.

